Back
BackPsychological Disorders: Core Concepts and Major Categories
Study Guide - Smart Notes

Psychological Disorders
Defining Psychological Disorders
Psychological disorders, also known as mental disorders, are patterns of thoughts, feelings, or behaviors that are deviant, distressful, dangerous, or dysfunctional. These patterns are not simply unusual behaviors but are characterized by a collection of symptoms that tend to occur together and significantly impact an individual's daily functioning and well-being.
Deviance: Behavior that differs from societal or cultural norms.
Distress: Symptoms cause significant stress or frustration, often because they are uncontrollable.
Dysfunction: Symptoms interfere with daily life, work, or relationships.
Danger: There is a risk of harm to oneself or others (less common than often assumed).
Abnormal psychology is the scientific study of these disorders, focusing on what has happened to a person rather than labeling them as "insane" or "crazy." The term "insane" is a legal term, not a clinical one.

Anxiety Disorders
General Features of Anxiety Disorders
Anxiety disorders are characterized by excessive and inappropriate feelings of apprehension, tension, or fear that are detached from actual danger. While anxiety can be adaptive, energizing us to cope with threats, it becomes a disorder when it is chronic, overwhelming, and interferes with daily life.
Panic Attack: Sudden episodes of intense dread, physical symptoms (chest pain, choking, numbness), and a strong urge to escape.
Panic Disorder: Recurrent, unexpected panic attacks and persistent concern about having more attacks, often leading to behavioral changes to avoid them.
Phobias: Irrational, intense fears of specific objects, situations, or activities (e.g., arachnophobia—fear of spiders; agoraphobia—fear of being away from a safe place, often triggered by panic attacks).

Trauma- and Stressor-Related Disorders
Posttraumatic Stress Disorder (PTSD)
PTSD is a disorder that develops after exposure to a traumatic or life-threatening event. Symptoms include reliving the trauma (flashbacks, nightmares), psychic numbing, social withdrawal, heightened anxiety, and insomnia. These symptoms persist for more than four weeks after the event.
Not everyone exposed to trauma develops PTSD; risk factors include genetic predisposition, prior psychological problems, poor emotional adjustment, and catastrophizing.



Obsessive-Compulsive and Related Disorders
Obsessive-Compulsive Disorder (OCD)
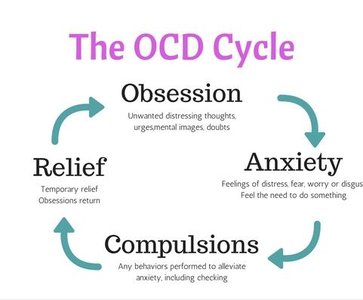
OCD is marked by persistent, unwanted thoughts (obsessions) and repetitive behaviors or mental acts (compulsions) that the individual feels driven to perform. These behaviors are time-consuming (at least one hour per day) and cause significant distress or impairment.
Obsessions: Intrusive, distressing thoughts, urges, or images.
Compulsions: Repetitive actions or mental rituals performed to reduce anxiety caused by obsessions.
OCD is considered a disorder when it causes distress, dysfunction, or deviates significantly from typical behavior.



Mood Disorders
Major Depressive Disorder and Bipolar Disorder
Mood disorders involve significant disturbances in mood that affect cognition, emotion, and behavior. Over 20% of North Americans experience a mood disorder in their lifetime.
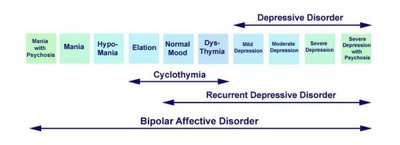
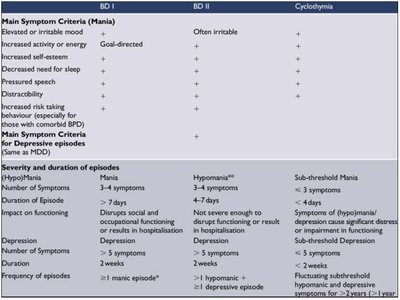
Major Depressive Disorder (MDD): Persistent depressed mood or loss of interest/pleasure in activities, plus other symptoms (e.g., appetite/sleep changes, fatigue, feelings of worthlessness, concentration problems, suicidal thoughts) for at least two weeks.
Bipolar Disorder: Alternating episodes of depression and mania (periods of elevated, expansive, or irritable mood, increased energy, impulsivity, and reduced need for sleep). Formerly called "manic-depressive disorder." Mania is more than just a "good mood"—it is a pathological state.
Contrasting Symptoms:
Depression: Pessimism, social withdrawal, lack of pleasure, inactivity, fatigue, excessive sleep.
Mania: Exaggerated optimism, hypersociality, impulsivity, racing thoughts, little need for sleep.

Biological Basis of Mood Disorders
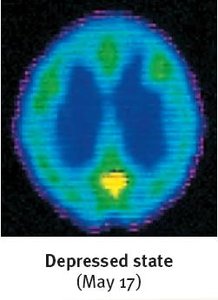
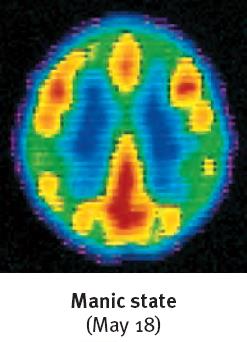
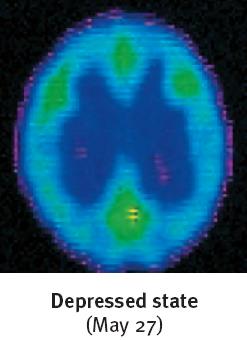
Brain imaging studies show that brain activity is diminished in depression and increased in mania. Structural differences include smaller frontal lobes in depression and fewer axons in bipolar disorder. Neurotransmitter imbalances are also implicated: reduced serotonin in depression and increased norepinephrine in mania.
Dissociative Identity Disorder
Features and Controversies
Dissociative Identity Disorder (DID), formerly known as Multiple Personality Disorder, is characterized by the presence of two or more distinct identities or personality states within a single individual. These identities may have their own names, traits, and memories, and are not present in consciousness at the same time. Some psychologists question the validity of DID, noting that treatment can sometimes increase the number of reported identities.

Schizophrenia Spectrum Disorder
Core Symptoms and Types
Schizophrenia is a severe psychotic disorder marked by distorted perceptions of reality, irrational behavior, and significant cognitive impairments. It is not the same as DID or bipolar disorder.
Positive symptoms: Presence of problematic behaviors (hallucinations, delusions, disorganized speech, bizarre behaviors).
Negative symptoms: Absence of healthy behaviors (flat affect, reduced social interaction, anhedonia, avolition, alogia, catatonia).

Summary Table: Key Points about Major Disorders
Disorder | Key Feature |
|---|---|
Depression | More than being sad |
Anxiety | More than worrying |
OCD | More than being tidy |
PTSD | More than just flashbacks |
Bipolar | More than mood swings |
Schizophrenia | More than seeing things |
EDs (Eating Disorders) | More than being underweight |
Borderline | More than instability |
Addiction | Not just "a choice" |

Psychological Disorders: The Importance of Understanding
Understanding psychological disorders requires a nuanced approach that goes beyond stereotypes and misconceptions. Effective diagnosis and treatment depend on recognizing the complexity of symptoms and the individual experiences of those affected.