 Back
BackBlood, Heart, Blood Vessels, Lymphatic, and Respiratory Systems: Structured Study Notes
Study Guide - Smart Notes

Blood and Blood Vessels
Components and Formed Elements of Blood
Blood is a specialized connective tissue with multiple components, each serving distinct physiological roles.
Plasma: The fluid matrix of blood, comprising about 55% of total blood volume. Contains water, electrolytes, nutrients, hormones, and plasma proteins (e.g., albumin, globulins, fibrinogen).
Formed Elements:
Red Blood Cells (Erythrocytes): Biconcave cells specialized for oxygen transport via hemoglobin.
White Blood Cells (Leukocytes): Immune cells divided into:
Granular Leukocytes: Neutrophils, Basophils, Eosinophils
Agranular Leukocytes: Lymphocytes, Monocytes
Platelets (Thrombocytes): Cell fragments derived from megakaryocytes, essential for blood clotting.
Functions of Red Blood Cells and Hemoglobin
Red Blood Cells: Transport oxygen from lungs to tissues and carbon dioxide from tissues to lungs.
Hemoglobin: Iron-containing protein in RBCs that binds oxygen; each molecule can carry four O2 molecules.
ABO Blood Types and Rh Factor
Blood typing is crucial for safe transfusions and organ transplants.
ABO System: Determined by presence of A and/or B antigens on RBCs.
Rh Factor: Presence (+) or absence (−) of D antigen; important in pregnancy and transfusion compatibility.
Blood Compatibility: Mismatched transfusions can cause agglutination and hemolysis.
Hemostasis
Hemostasis is the physiological process that stops bleeding at the site of injury.
Three Phases:
Vascular phase: Vasoconstriction reduces blood flow.
Platelet phase: Platelets adhere to exposed collagen and aggregate.
Coagulation phase: Cascade of clotting factors forms a stable fibrin clot.
Pulmonary vs. Systemic Circulation
Pulmonary Circulation: Right side of heart pumps deoxygenated blood to lungs for gas exchange.
Systemic Circulation: Left side of heart pumps oxygenated blood to body tissues.
Functional Anatomy of Blood Vessels
Arteries: Carry blood away from the heart; thick-walled and elastic.
Arterioles: Small branches of arteries leading to capillaries.
Capillaries: Microscopic vessels where exchange of gases, nutrients, and wastes occurs.
Veins: Carry blood toward the heart; thinner walls, often with valves to prevent backflow.
The Heart and Cardiovascular Function
Flow of Blood Through the Heart
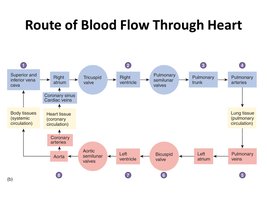
The heart is a dual pump that propels blood through pulmonary and systemic circuits in a specific sequence.
Blood enters the right atrium from the superior and inferior vena cava.
Passes through the right ventricle, then to the pulmonary trunk and arteries to the lungs.
Oxygenated blood returns via pulmonary veins to the left atrium, then left ventricle, and is pumped into the aorta for systemic distribution.
Cardiac Cycle and Conducting System
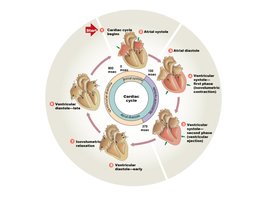
The cardiac cycle describes the sequence of events in one heartbeat, including contraction (systole) and relaxation (diastole) of atria and ventricles.
Atrial Systole: Atria contract, pushing blood into ventricles.
Ventricular Systole: Ventricles contract, ejecting blood into pulmonary and systemic circuits.
Diastole: Chambers relax and fill with blood.
Conducting System: SA node (pacemaker) initiates impulse → AV node → AV bundle → bundle branches → Purkinje fibers.
Autonomic Control and ECG
Parasympathetic (Vagus Nerve): Slows heart rate.
Sympathetic (Cardiac Nerves): Increases heart rate and contractility.
Electrocardiogram (ECG): Records electrical activity of the heart.
P wave: Atrial depolarization
QRS complex: Ventricular depolarization
T wave: Ventricular repolarization
Cardiac Output and Influencing Factors
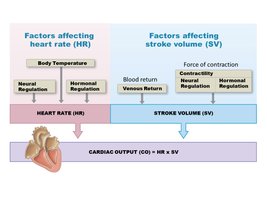
Cardiac output (CO) is the volume of blood pumped by each ventricle per minute.
Formula:
Heart Rate (HR): Beats per minute; influenced by neural, hormonal, and temperature factors.
Stroke Volume (SV): Volume of blood ejected per beat; influenced by venous return, contractility, and hormonal regulation.
The Lymphatic System and Immunity
Components and Functions of the Lymphatic System
The lymphatic system maintains fluid balance, absorbs dietary fats, and provides immune defense.
Lymphocytes: Key immune cells (T cells, B cells, NK cells).
T Cells: Cell-mediated immunity (cytotoxic, helper, suppressor types).
B Cells: Antibody-mediated immunity; differentiate into plasma cells to produce antibodies.
NK Cells: Innate immunity; destroy abnormal cells via immunological surveillance.
Innate vs. Adaptive Immunity
Innate (Nonspecific) Immunity: General defenses present at birth; includes barriers, phagocytes, inflammation, and fever.
Adaptive (Specific) Immunity: Targeted response to specific antigens; involves lymphocytes, memory, and specificity.
T-Cell and B-Cell Mediated Immunity
T-Cell Mediated Immunity: Cytotoxic T cells destroy infected cells; helper T cells activate other immune cells; suppressor T cells regulate response.
B-Cell Mediated Immunity: B cells differentiate into plasma cells that secrete antibodies targeting specific antigens.
The Respiratory System
Ventilation and Respiration
Ventilation: Movement of air into and out of the lungs.
External Respiration: Gas exchange between alveoli and blood.
Internal Respiration: Gas exchange between blood and tissues.
Functions of the Respiratory System
Voice production, olfaction, protection (against dehydration, temperature changes, pathogens), and regulation of blood pH.
Anatomy of the Respiratory System
Upper Respiratory Tract: Nasal cavity, pharynx, larynx; warms, filters, humidifies air.
Lower Respiratory Tract: Trachea, bronchi, bronchioles, lungs; site of gas exchange.
Epithelium: Pseudostratified ciliated columnar in most of tract; stratified squamous in oropharynx/laryngopharynx.
Larynx: Sound production; contains epiglottis and arytenoid cartilages.
Trachea and Bronchi: C-shaped cartilage rings keep airway open.
Bronchioles: Smallest airways; bronchodilation (sympathetic), bronchoconstriction (parasympathetic).
Lungs: Right lung (3 lobes), left lung (2 lobes); pleurae surround lungs (parietal and visceral layers).
Alveoli: Site of external respiration; surfactant-secreting cells reduce surface tension; macrophages engulf debris.
Respiratory Membrane: Thin barrier for gas exchange; consists of alveolar epithelium, fused basement membranes, and capillary endothelium.
Mechanics of Pulmonary Ventilation
Inspiration: Diaphragm and external intercostals contract, increasing thoracic volume and decreasing pressure, drawing air in.
Expiration: Usually passive at rest; active expiration uses accessory muscles.
Pleural fluid and pressure changes facilitate lung expansion and recoil.
Gas Transport in Blood
Oxygen: Mostly transported bound to hemoglobin:
Carbon Dioxide: Transported dissolved in plasma, bound to hemoglobin, or as bicarbonate ions:
Neural Control of Respiration
Respiratory centers in the pons and medulla oblongata regulate breathing rate and rhythm.
Dorsal respiratory group (DRG): Controls inspiration.
Ventral respiratory group (VRG): Controls forced breathing.
CO2 levels are the primary driver of respiratory rate adjustments.
