 Back
BackBlood: Structure, Function, and Clinical Relevance in Human Anatomy & Physiology
Study Guide - Smart Notes

Blood: Structure and Function
Functions of Blood
Blood is a specialized connective tissue that plays a vital role in maintaining homeostasis and supporting the functions of various organ systems. Its functions include transport, regulation, protection, and clot formation.
Transport: Blood carries oxygen, nutrients, hormones, and waste products throughout the body.
Regulation: Blood helps regulate pH, water concentration, temperature, and osmotic function.
Protection: Blood provides immunological functions and prevents infection.
Clot Formation: Blood forms clots to prevent excessive blood loss.

Composition of Blood
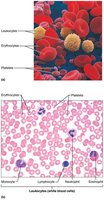
Blood consists of plasma (the liquid matrix) and formed elements (cells and cell fragments). The plasma is a colloid containing water, proteins, ions, nutrients, waste products, gases, and regulatory substances. The formed elements include erythrocytes (RBCs), leukocytes (WBCs), and platelets.
Plasma: 91% water, 9% solutes (proteins, ions, nutrients, waste, gases, regulatory substances).
Formed Elements: Erythrocytes (~45%), leukocytes and platelets (<1%), plasma (~55%).
Plasma and Plasma Proteins
Major Plasma Proteins
Plasma proteins are essential for blood function and homeostasis.
Albumins: Maintain viscosity, osmotic pressure, act as buffers, and transport fatty acids, bilirubin, and hormones.
Globulins: Transport lipids, carbohydrates, hormones, ions, and function as antibodies and complement proteins.
Fibrinogen: Key protein in blood clotting.
Other Plasma Components
Ions: Important for osmosis, membrane potentials, and acid-base balance.
Nutrients: Glucose, amino acids, triglycerides, cholesterol, vitamins.
Waste Products: Urea, uric acid, creatinine, ammonia, bilirubin, lactic acid.
Gases: Oxygen, carbon dioxide, nitrogen.
Regulatory Substances: Hormones, enzymes.
Formed Elements of Blood
Red Blood Cells (Erythrocytes)
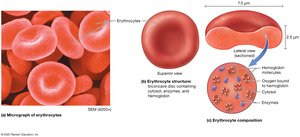
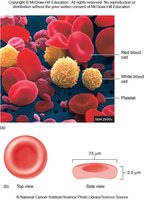
Red blood cells are biconcave, anucleate cells specialized for gas transport. They contain hemoglobin, which binds oxygen and carbon dioxide.
Structure: Biconcave shape increases surface area for gas exchange; no nucleus or mitochondria.
Function: Transport oxygen (98.5% bound to hemoglobin, 1.5% dissolved) and carbon dioxide (70% as bicarbonate, 23% bound to hemoglobin, 7% dissolved).
Hemoglobin: Each molecule can carry four O2; composed of four globin proteins and four heme groups (each with an iron atom).
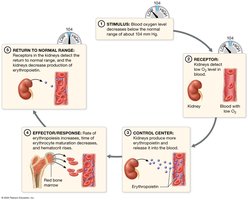
Erythropoiesis
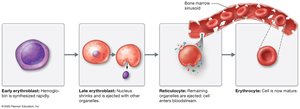
Erythropoiesis is the process of red blood cell production, regulated by erythropoietin (EPO) from the kidneys in response to low blood oxygen levels. RBCs mature from stem cells through several stages and last about 120 days in circulation.
Stages: Stem cell → proerythroblast → erythroblast → reticulocyte → erythrocyte.
Regulation: EPO stimulates production; balance maintained by hormonal controls and dietary requirements.
Eryptosis
Eryptosis is the programmed death of aging red blood cells. Macrophages recognize and phagocytose old RBCs, recycling their contents. Hemoglobin is broken down into heme (converted to bilirubin) and globin (reused as amino acids). Iron is transported by transferrin for storage or reuse.
White Blood Cells (Leukocytes)
Leukocytes are less than 1% of blood volume and are crucial for immune defense. They can leave capillaries (diapedesis), move through tissues (amoeboid motion), and respond to chemical signals (chemotaxis).
Granulocytes: Neutrophils, eosinophils, basophils (contain granules, lobed nuclei).
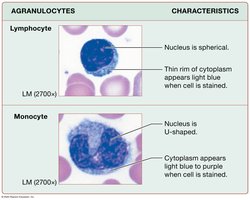
Agranulocytes: Lymphocytes, monocytes (lack prominent granules, non-lobed nuclei).
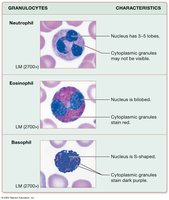
Neutrophils
Most numerous WBC (50–70%). Multi-lobed nucleus, phagocytic, "bacteria slayers."
Kill microbes: Respiratory burst produces oxidizing substances; defensins pierce microbe membranes.
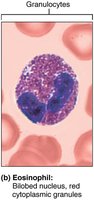
Eosinophils
2–4% of WBCs. Bilobed nucleus, granules contain digestive enzymes.
Function: Attack parasitic worms, modulate allergic responses, destroy inflammatory chemicals.
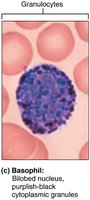
Basophils
Rarest WBC (0.5–1%). Granules contain histamine (vasodilator, attracts WBCs).
Function: Inflammatory response, allergic reactions; similar to mast cells.
Lymphocytes
20–40% of WBCs. Large, round nucleus; includes T cells, B cells, and Natural Killer cells.
Function: Adaptive immunity (helper T, cytotoxic T, B cells for antibody production, NK cells for innate immunity).
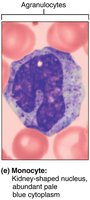
Monocytes
3–8% of WBCs. U-shaped nucleus; differentiate into macrophages in tissues.
Function: Phagocytosis, antigen presentation, defense against chronic infections.
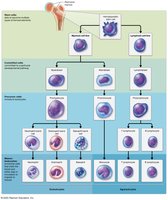
Leukopoiesis
Leukopoiesis is the formation of white blood cells, regulated by interleukins and colony-stimulating factors (CSFs). All WBCs originate from hemocytoblasts, which differentiate into lymphoid (lymphocytes) and myeloid (other WBCs) lineages.
Platelets (Thrombocytes)
Platelets are cell fragments derived from megakaryocytes. They form temporary plugs and release chemicals necessary for blood clotting. Platelet formation (thrombopoiesis) is regulated by thrombopoietin.
Normal count: 150,000–400,000 platelets/ml.
Life span: About 10 days.
Hemostasis: Prevention of Blood Loss
Hemostasis Overview
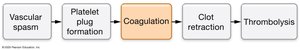
Hemostasis is the process that prevents excessive blood loss following injury. It involves several interdependent steps:
Vascular spasm: Vasoconstriction of damaged vessels.
Platelet plug formation: Platelets adhere to exposed vessel surfaces and aggregate.
Coagulation: Formation of a fibrin mesh that stabilizes the plug.
Clot retraction: Platelets contract to bring wound edges together.
Thrombolysis: Dissolution of the clot after healing.

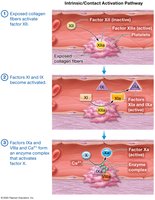
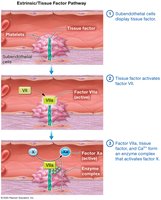
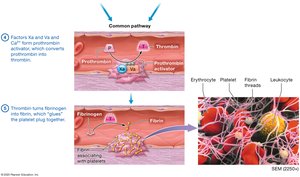
Coagulation Pathways
Coagulation involves intrinsic and extrinsic pathways, both leading to the activation of factor Xa and the conversion of prothrombin to thrombin, which then forms fibrin from fibrinogen.
Blood Types and Transfusion
ABO and Rh Blood Group Systems
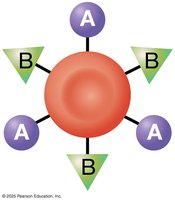
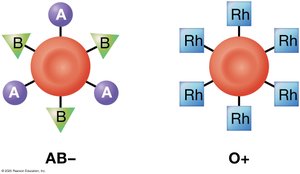
Blood types are determined by antigens (agglutinogens) on the surface of RBCs. The ABO system includes types A, B, AB, and O, while the Rh system is based on the presence or absence of the Rh antigen.
Antibodies (agglutinins): Bind to RBC antigens, causing agglutination or hemolysis if incompatible blood is transfused.
Transfusion: Must match donor and recipient blood types to avoid immune reactions.

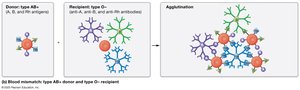
Blood Transfusion Reactions
Transfusion reactions occur when incompatible blood is introduced, leading to agglutination and hemolysis. Proper crossmatching and blood typing are essential for safe transfusions.
Diagnostic Blood Tests
Common Blood Tests
Type and Crossmatch: Determines ABO and Rh blood types.
Complete Blood Count (CBC): Measures RBC, WBC, and platelet counts.
Hemoglobin Measurement: Grams of hemoglobin per 100 mL of blood.
Hematocrit Measurement: Percentage of blood volume that is RBCs.
White Blood Cell Count: 5,000–10,000/µL of blood.
Broader Connections and Clinical Relevance
Blood Disorders and Systemic Connections
Understanding blood is essential for diagnosing and managing disorders such as hemophilia, sickle cell anemia, leukemia, and infections like osteomyelitis. Blood supports the respiratory, endocrine, and other systems, making its study crucial for clinical practice.
Osteomyelitis: Bone marrow infection can disrupt blood cell production.
Leukemia: Overproduction of WBCs leads to bruising and slow healing due to impaired clotting and immune function.
Additional info: Blood is central to homeostasis, immunity, and tissue repair, and its disorders can have widespread effects on health.
