 Back
BackBlood: Structure, Function, and Disorders – Study Notes for Anatomy & Physiology
Study Guide - Smart Notes

Overview of Blood
Major Components and Functions
Blood is a specialized connective tissue that plays a vital role in transport, protection, and regulation within the human body. It consists of plasma and formed elements, each with distinct functions.
Transport: Blood carries oxygen, carbon dioxide, nutrients, metabolic wastes, hormones, and stem cells throughout the body.
Protection: Blood performs immune functions, limits infection spread, and seals damaged vessels via clotting.
Regulation: Blood stabilizes blood pressure, fluid distribution, acid-base balance, and body temperature.
Composition of Blood
Plasma and Formed Elements
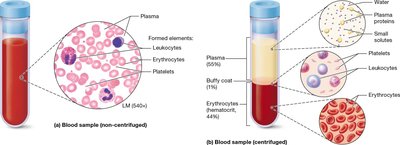
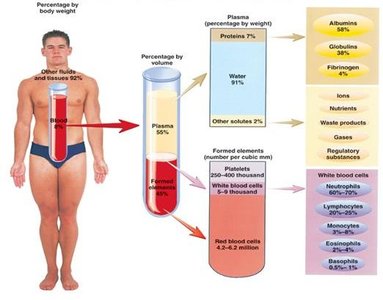
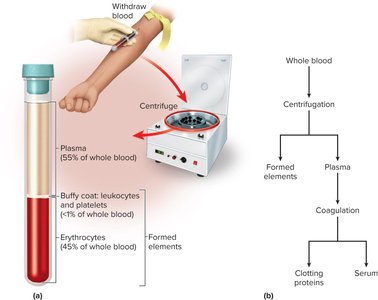
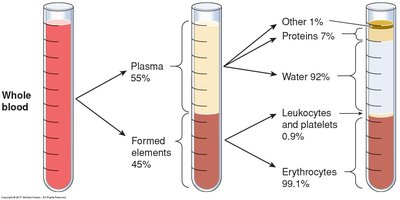
Blood is composed of plasma (the liquid matrix) and formed elements (cells and cell fragments).
Plasma: Makes up about 55% of blood volume; contains water, proteins, ions, nutrients, wastes, and gases.
Formed Elements: Includes erythrocytes (red blood cells), leukocytes (white blood cells), and platelets.
Plasma Components and Functions
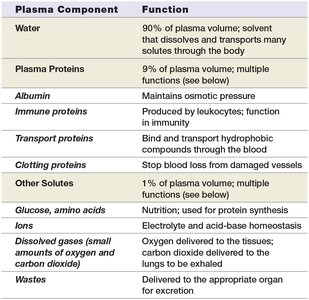
Plasma contains several key components, each with specific functions.
Plasma Component | Function |
|---|---|
Water | Solvent for transport; 90% of plasma volume |
Plasma Proteins | Multiple functions; 9% of plasma volume |
Albumin | Maintains osmotic pressure |
Immune proteins | Produced by leukocytes; immunity |
Transport proteins | Bind and transport hydrophobic compounds |
Clotting proteins | Stop blood loss from damaged vessels |
Other solutes | Electrolyte and acid-base homeostasis |
Glucose, amino acids | Nutrition; protein synthesis |
Ions | Electrolyte and acid-base homeostasis |
Dissolved gases | Oxygen and carbon dioxide transport |
Wastes | Excretion |
Major Plasma Proteins
Plasma proteins are essential for maintaining blood viscosity, osmotic pressure, and immune defense.
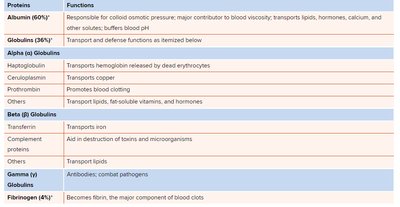
Protein | Functions |
|---|---|
Albumin (60%) | Colloid osmotic pressure, blood viscosity, transport, pH buffering |
Globulins (36%) | Transport and defense |
Alpha Globulins | Transport hemoglobin, copper, promote clotting |
Beta Globulins | Transport iron, aid in toxin destruction, transport lipids |
Gamma Globulins | Antibodies; combat pathogens |
Fibrinogen (4%) | Becomes fibrin, main component of blood clots |
Blood Viscosity and Osmolarity
Definitions and Importance
Viscosity: Resistance of blood to flow; whole blood is 4.5–5.5 times as viscous as water.
Osmolarity: Total concentration of solute particles; affects fluid transfer between capillaries and tissues.
Colloid osmotic pressure: Contribution of plasma proteins to blood osmolarity.
Fluid Sequestration and Edema
Types and Causes
Fluid sequestration refers to the accumulation of excess fluid in specific locations, often resulting in edema or effusion.
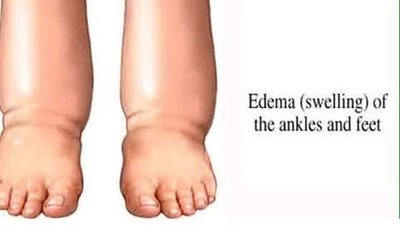
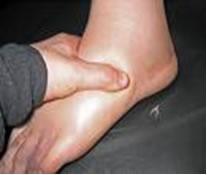
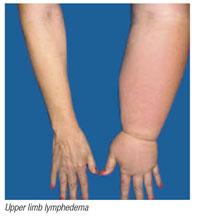
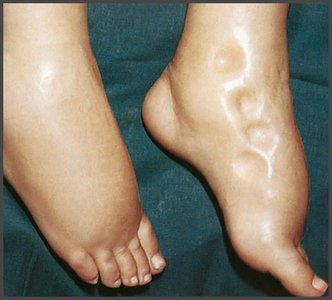
Edema: Accumulation of interstitial fluid, commonly in the extremities.
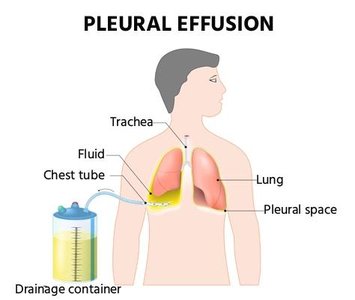
Effusion: Fluid collection within a body space, such as pleural effusion.
Hemorrhage: Pooling of blood outside circulation.
Edema: Pathophysiology
Edema can result from increased capillary filtration, reduced capillary absorption, or obstructed lymphatic drainage.
Increased capillary filtration: Kidney failure, histamine release, poor venous return.
Reduced capillary absorption: Hypoproteinemia, liver disease, dietary protein deficiency.
Obstructed lymphatic drainage: Surgical removal of lymph nodes.
Erythrocytes and Oxygen Transport
Structure and Function of Erythrocytes
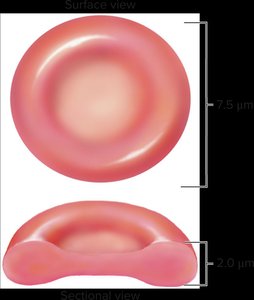
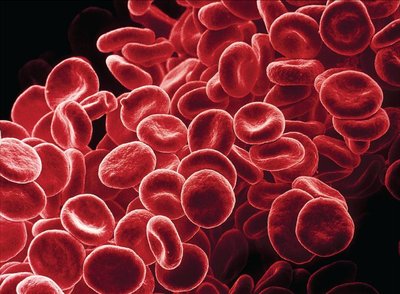
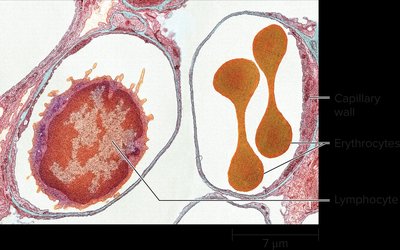
Erythrocytes (red blood cells) are specialized for oxygen transport due to their biconcave shape and high hemoglobin content.
Biconcave shape: Increases surface area for gas exchange.
No nucleus: Maximizes space for hemoglobin.
Flexible membrane: Allows passage through capillaries.
Hemoglobin: Structure and Types
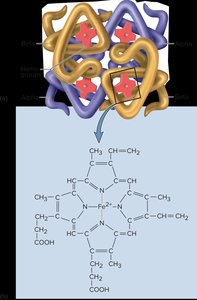
Hemoglobin is a protein with four globin chains, each binding a heme group for oxygen transport.
Embryonic hemoglobin: Present in early development.
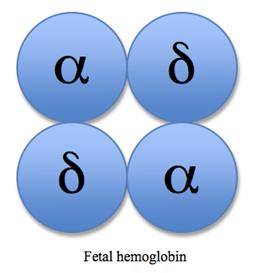
Fetal hemoglobin: Contains alpha and gamma globins; higher oxygen affinity.
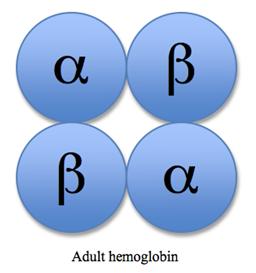
Adult hemoglobin: Contains alpha and beta globins.
Hemoglobin Forms and Terminology
Oxyhemoglobin: Hemoglobin bound to oxygen.
Deoxyhemoglobin: Hemoglobin without oxygen.
Carbaminohemoglobin: Hemoglobin bound to carbon dioxide.
Carboxyhemoglobin: Hemoglobin bound to carbon monoxide; prevents oxygen transport.
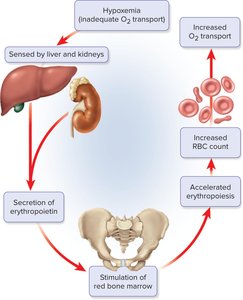
Erythropoiesis: Production of RBCs
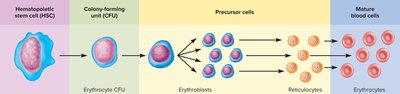
Erythropoiesis is the process of red blood cell formation, regulated by erythropoietin.
Stem cells differentiate into proerythroblasts, then erythroblasts, reticulocytes, and mature erythrocytes.
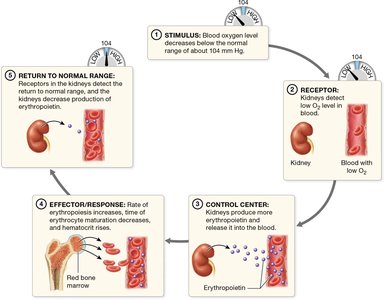
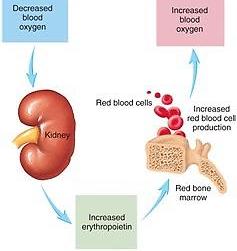
Erythropoietin: Hormone produced by kidneys in response to low blood oxygen.
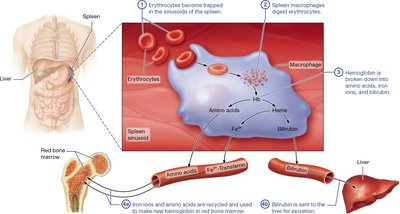
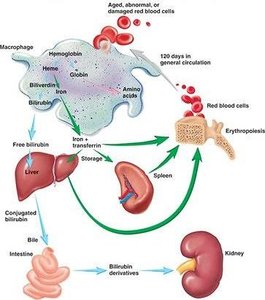
Life Cycle and Death of RBCs
RBCs circulate for about 120 days before being broken down in the liver and spleen. Hemoglobin is degraded into amino acids, iron, and bilirubin. 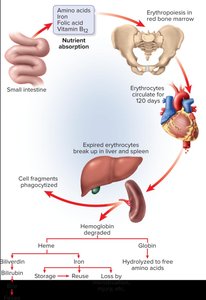
Quantities of Erythrocytes and Hemoglobin
RBC count: 4.6–6.2 million/μL
Hemoglobin: 14–18 g/100 mL (male), 12–16 g/100 mL (female)
Hematocrit: 42–52% (men), 37–48% (women)
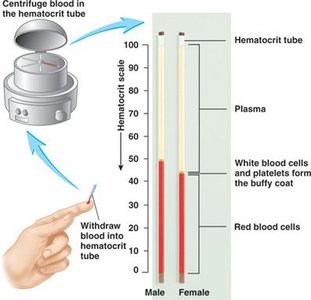
Hematocrit and Diagnosis
Hematocrit is used to diagnose anemia or polycythemia.
Formula:
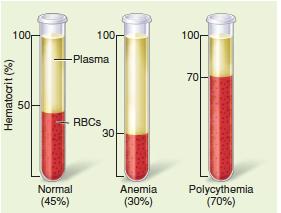
Erythrocyte Disorders
Polycythemia and Anemia
Polycythemia: Excessive RBCs; may result from bone marrow cancer or secondary causes.
Anemia: Deficiency of RBCs; can be caused by inadequate erythropoiesis, blood loss, or RBC destruction.
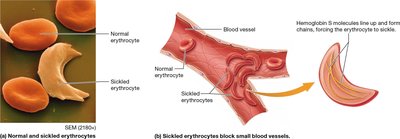
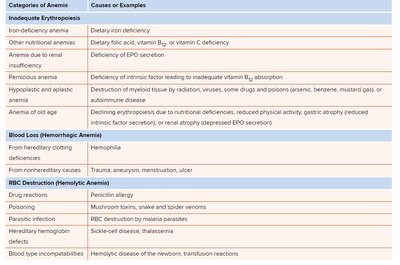
Leukocytes and Immune Function
Types and Functions of Leukocytes
Leukocytes (white blood cells) are essential for immune defense and removal of debris. There are five major types:
Neutrophils: Phagocytize bacteria.
Eosinophils: Combat parasites and allergens.
Basophils: Release histamine and heparin.
Lymphocytes: Produce antibodies and regulate immunity.
Monocytes: Phagocytize pathogens and debris.
Leukopoiesis
Granulocytes circulate for 4–8 hours, then migrate to tissues for 4–5 days.
Leukocyte Disorders
Leukopenia: Deficiency of WBCs; caused by radiation, infection, or poisoning.
Leukocytosis: Elevated WBC count; usually indicates infection.
Leukemia: Cancer of WBCs; abnormal blood smear.
Platelets and Hemostasis
Structure and Function of Platelets
Platelets are cell fragments from megakaryocytes, essential for clotting and vessel repair.
Functions: Vasoconstriction, platelet plug formation, procoagulant secretion, clot dissolution, chemotaxis, growth factor secretion.
Platelet Production
Platelets are formed from megakaryocytes in the bone marrow.
Hemostasis and Coagulation
Hemostasis is the process of stopping blood loss, involving vascular spasm, platelet plug formation, and coagulation.
Coagulation: Formation of fibrin mesh to stabilize the clot.
Clotting factors: Proteins required for coagulation; calcium ions and vitamin K are essential.
Fibrinolysis: Dissolution of clot after tissue repair.
Danger of Unwanted Clot Formation
Thrombus: Stationary clot in vessel.
Embolus: Mobile clot or obstruction.
Anticoagulant and Antiplatelet Control
Anticoagulants: Prevent clot formation (e.g., antithrombin, heparin, warfarin).
Antiplatelet agents: Inhibit platelet activation (e.g., aspirin, ADP inhibitors, GP IIb/IIIa inhibitors).
Blood Typing and Matching
ABO and Rh Blood Groups
Blood types are determined by surface antigens on erythrocytes.
ABO group: Type A, B, AB, O; based on presence of A and B antigens.
Rh group: Rh+ (D antigen present), Rh- (D antigen absent).
Agglutination and Transfusion Reactions
Agglutination: Clumping of RBCs when exposed to specific antibodies.
Transfusion reaction: Occurs when mismatched blood is transfused; can cause hemolysis, fever, renal failure.
Universal donor: Type O-
Universal recipient: Type AB+
Maternal-Fetal Mismatches
Hemolytic disease of the newborn (HDN) can occur when an Rh- mother has an Rh+ baby.
Prevention: Rh immune globulin (RhoGAM) given to Rh- mothers.
Blood Chemistry and Coagulation Labs
Blood Chemistry
Blood chemistry assesses the composition of plasma and is used to evaluate body system function.
Coagulation Labs
Platelet count: 250,000–400,000/μL
Prothrombin time: 9–12 seconds
Bleeding time: Measured after incision
Summary Table: Blood Components and Functions
Component | Main Function |
|---|---|
Plasma | Transport, regulation, protection |
Erythrocytes | Oxygen and carbon dioxide transport |
Leukocytes | Immune defense |
Platelets | Clotting and vessel repair |
Key Equations
Hematocrit:
Additional info:
Expanded explanations of plasma proteins and their functions were added for academic completeness.
Tables were recreated and expanded for clarity and study usefulness.
