 Back
BackBlood: Structure, Function, and Disorders – Study Guide for Anatomy & Physiology
Study Guide - Smart Notes

Blood: Structure, Function, and Disorders
Overview of Blood
Blood is a life-sustaining transport vehicle of the cardiovascular system, crucial for maintaining homeostasis and supporting metabolic processes. It is the only fluid tissue in the body and is classified as a connective tissue, consisting of a nonliving matrix (plasma) and living cells (formed elements).
Transport: Delivers oxygen and nutrients to cells, removes metabolic wastes, and transports hormones.
Regulation: Maintains body temperature, pH balance, and fluid volume.
Protection: Prevents blood loss and carries immune agents.
Composition of Blood
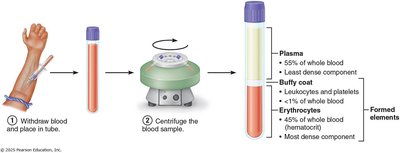
Blood consists of plasma and formed elements. When centrifuged, blood separates into three layers: erythrocytes (RBCs) at the bottom, a buffy coat (WBCs and platelets) in the middle, and plasma at the top.
Plasma: 55% of whole blood; least dense component.
Buffy coat: <1% of whole blood; contains leukocytes and platelets.
Erythrocytes: 45% of whole blood; most dense component.
Physical Characteristics and Volume
Blood is a sticky, opaque fluid with a metallic taste. Its color varies with oxygen content: scarlet red when oxygen-rich, dark red when oxygen-poor.
pH: 7.35–7.45
Body weight: ~8%
Average volume: Males: 5–6 L; Females: 4–5 L
Blood Plasma
Plasma is a straw-colored, sticky fluid, making up about 90% water and containing over 100 dissolved solutes, including nutrients, gases, hormones, wastes, proteins, and inorganic ions. Plasma proteins are the most abundant solutes, produced mostly by the liver.
Albumin: 60% of plasma proteins; functions as a carrier, blood buffer, and contributes to osmotic pressure.
Other proteins: Globulins (transport and immune functions), fibrinogen (clotting).

Formed Elements
The formed elements include erythrocytes (RBCs), leukocytes (WBCs), and platelets. Only WBCs are complete cells; RBCs lack nuclei and organelles, and platelets are cell fragments. Most formed elements originate in bone marrow and do not divide. 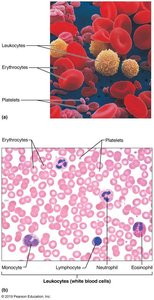
Erythrocytes (Red Blood Cells)
Structure and Function
Erythrocytes are small, biconcave, anucleate cells specialized for gas transport. Their shape provides a large surface area for gas exchange, and they are filled with hemoglobin (Hb), which binds oxygen. RBCs lack mitochondria, so ATP production is anaerobic, ensuring they do not consume the oxygen they transport. 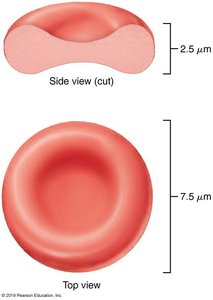
Hemoglobin Structure and Function
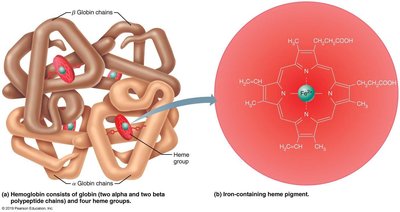
Hemoglobin is a protein composed of four polypeptide chains (two alpha, two beta) and four heme groups. Each heme contains an iron atom that binds one oxygen molecule.
Oxygen loading: In lungs, produces oxyhemoglobin (ruby red).
Oxygen unloading: In tissues, produces deoxyhemoglobin (dark red).
CO2 loading: 20% of CO2 binds to Hb, forming carbaminohemoglobin.
Erythrocyte Disorders
Anemia
Anemia is a condition where blood has an abnormally low oxygen-carrying capacity, insufficient to support normal metabolism. It is a symptom of underlying problems and is classified by cause:
Blood loss: Hemorrhagic anemia (rapid loss), chronic hemorrhagic anemia (persistent loss).
Not enough RBCs produced: Iron-deficiency anemia (microcytes), pernicious anemia (macrocytes, B12 deficiency), renal anemia (lack of EPO), aplastic anemia (bone marrow destruction).
Too many RBCs destroyed: Hemolytic anemias (incompatible transfusions, infections, genetic disorders like thalassemias and sickle-cell anemia).
Sickle-Cell Anemia
Sickle-cell anemia is caused by a mutation in the hemoglobin beta chain, resulting in crescent-shaped RBCs under low oxygen conditions. These cells rupture easily and block small vessels, leading to poor oxygen delivery and pain. 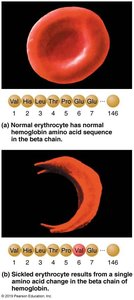
Polycythemia
Polycythemia is an abnormal excess of RBCs, increasing blood viscosity and causing sluggish flow. It can be caused by bone marrow cancer (polycythemia vera), low oxygen levels (secondary polycythemia), or blood doping in athletes.
Leukocytes (White Blood Cells)
Structure and Function
Leukocytes are the only complete cells among formed elements, making up less than 1% of blood volume. They defend against disease, can leave capillaries (diapedesis), and move through tissues by amoeboid motion and chemotaxis.
Leukocytosis: WBC count over 11,000/μl, a normal response to infection.
Categories: Granulocytes (neutrophils, eosinophils, basophils) and agranulocytes (lymphocytes, monocytes).
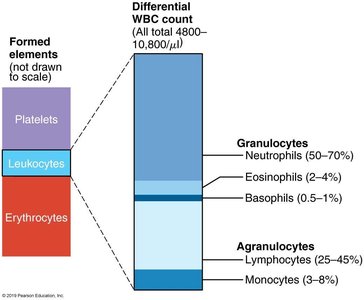
Granulocytes
Neutrophils: Most numerous, phagocytic "bacteria slayers," kill microbes by respiratory burst.
Eosinophils: Digest parasitic worms, modulate immune response, involved in allergies and asthma.
Basophils: Rarest, contain histamine (inflammatory chemical), functionally similar to mast cells.
Agranulocytes
Lymphocytes: Crucial to immunity; T cells act against virus-infected and tumor cells, B cells produce antibodies.
Monocytes: Largest WBCs, differentiate into macrophages, phagocytic, activate lymphocytes.
Summary Table of Formed Elements
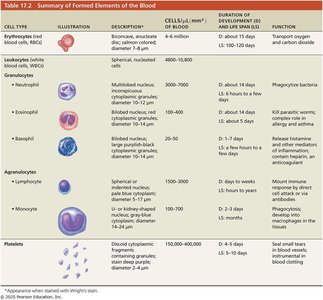
Leukocyte Disorders
Leukemias
Leukemias are cancerous conditions involving overproduction of abnormal WBCs, usually clones of a single abnormal cell.
Acute leukemia: Derives from stem cells, affects children.
Chronic leukemia: Involves proliferation of later cell stages, more prevalent in older people.
Symptoms: Anemia, bleeding, infections; treatments include irradiation, drugs, stem cell transplants.
Infectious Mononucleosis
A highly contagious viral disease caused by Epstein-Barr virus, resulting in enlarged lymphocytes and symptoms like fatigue, sore throat, and low fever.
Platelets (Thrombocytes)
Structure and Function
Platelets are fragments of megakaryocytes, containing chemicals involved in clotting. They form temporary plugs to seal breaks in blood vessels and are kept inactive by nitric oxide and prostacyclin.
Formation: Regulated by thrombopoietin; megakaryocytes send cytoplasmic projections into capillaries, which break off into platelets.
Lifespan: About 10 days.
Normal count: 150,000–400,000 platelets/ml.
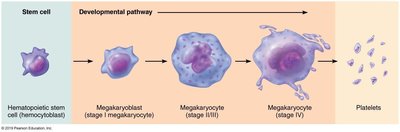
Blood Transfusions and Blood Groups
Blood Transfusions
The cardiovascular system compensates for blood loss by reducing vessel volume and increasing RBC production. Loss of 15–30% causes pallor and weakness; more than 30% can be fatal.
Volume replacement: Normal saline or Ringer’s solution restores circulation but not oxygen-carrying capacity.
Whole-blood transfusions: Used for rapid, substantial blood loss.
Packed RBCs: Preferred for restoring oxygen-carrying capacity.
Human Blood Groups
RBC membranes bear antigens (agglutinogens) that can generate immune responses. ABO and Rh groups are the most clinically significant.
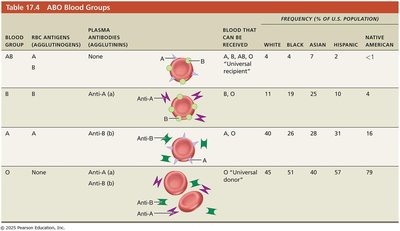
ABO Blood Groups: Based on presence/absence of A and B agglutinogens.
Type A: Only A agglutinogen; anti-B antibodies.
Type B: Only B agglutinogen; anti-A antibodies.
Type AB: Both A and B agglutinogens; no antibodies (universal recipient).
Type O: Neither A nor B agglutinogens; both anti-A and anti-B antibodies (universal donor).
Rh Blood Groups and Disorders
Rh factor: Presence or absence of Rh antigen (D antigen).
Hemolytic disease of the newborn: Occurs in Rh– mothers with Rh+ fetuses; anti-Rh antibodies can cross placenta and destroy fetal RBCs in subsequent pregnancies.
Prevention: RhoGAM serum prevents sensitization.
Transfusion Reactions
Transfusion reactions occur if mismatched blood is infused, leading to agglutination, vessel blockage, and hemoglobin release, which can cause renal failure.
Symptoms: Fever, chills, low blood pressure, rapid heartbeat, nausea, vomiting.
Treatment: Preventing kidney damage with fluids and diuretics.
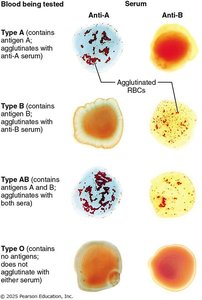
Blood typing: Donor blood is mixed with antibodies; agglutination indicates presence of agglutinogen.
Cross matching: Ensures compatibility between donor and recipient.
Key Tables
Composition of Plasma
Constituent | Description and Importance |
|---|---|
Water | 90% of plasma volume; dissolving and suspending medium for solutes; absorbs heat |
Electrolytes | Most abundant solutes by number; cations include sodium, potassium, calcium, magnesium; anions include chloride, phosphate, sulfate, bicarbonate; help maintain plasma osmotic pressure and normal pH |
Plasma proteins | Albumin (60%): carrier, buffer, osmotic pressure; Globulins (36%): transport and immune functions; Fibrinogen (4%): forms fibrin threads of blood clot |
Nutrients | Materials absorbed from digestive tract: glucose, amino acids, fatty acids, vitamins |
Respiratory gases | O2 and CO2; O2 mostly bound to hemoglobin, CO2 transported dissolved or bound to hemoglobin |
Hormones | Steroid and thyroid hormones carried by plasma proteins |

Summary of Formed Elements
Cell Type | Description | Cells/μl | Duration of Development and Life Span | Function |
|---|---|---|---|---|
Erythrocytes | Biconcave, anucleate | 4-6 million | D: 7 days; LS: 100-120 days | Transport O2 and CO2 |
Leukocytes | Multilobed nucleus | 4800-10,800 | D: about 4 days; LS: 6 hours to days | Phagocytize bacteria |
Eosinophils | Bilobed nucleus | 100-400 | D: about 14 days; LS: about 5 days | Kill parasitic worms; allergy and asthma |
Basophils | Lobed nucleus | 20-50 | D: 1-7 days; LS: about 5 days | Release histamine; inflammation |
Lymphocytes | Spherical nucleus | 1500-3000 | D: days to weeks; LS: hours to years | Mount immune response |
Monocytes | U- or kidney-shaped nucleus | 100-700 | D: 2-3 days; LS: months | Phagocytosis; develop into macrophages |
Platelets | Discoid cytoplasmic fragments | 150,000-400,000 | D: 4-5 days; LS: 5-10 days | Seal small tears in blood vessels; clotting |

ABO Blood Groups
Blood Group | RBC Antigens | Plasma Antibodies | Blood That Can Be Received | Frequency (%) |
|---|---|---|---|---|
AB | A, B | None | A, B, AB, O | White: 4, Black: 7, Asian: 10, Hispanic: 4, Native American: <1 |
B | B | Anti-A | B, O | White: 11, Black: 19, Asian: 23, Hispanic: 10, Native American: 4 |
A | A | Anti-B | A, O | White: 40, Black: 26, Asian: 28, Hispanic: 31, Native American: 16 |
O | None | Anti-A, Anti-B | O | White: 45, Black: 48, Asian: 39, Hispanic: 55, Native American: 79 |

Blood Typing and Agglutination
Blood typing involves mixing donor blood with antibodies against common agglutinogens. Agglutination indicates the presence of the agglutinogen. 
Additional info:
Blood is classified as a connective tissue due to its origin and matrix composition.
Hemoglobin's structure is crucial for its function; mutations can lead to disorders like sickle-cell anemia.
Blood group compatibility is essential for safe transfusions; cross-matching is performed to prevent reactions.
