 Back
BackBlood Vessels and Circulatory Pathways: Structure, Function, and Regulation
Study Guide - Smart Notes

Blood Vessel Structure and Function
General Structure of Blood Vessels
Blood vessels are the organs of the cardiovascular system, responsible for transporting blood throughout the body. They consist of three main types: arteries, veins, and capillaries, each with distinct structural and functional characteristics.
Arteries: Carry blood away from the heart; have thick walls, especially a robust tunica media (smooth muscle and elastic fibers), and a more circular lumen. They withstand high pressure and can vasoconstrict or vasodilate to regulate blood pressure.
Veins: Return blood to the heart; have thinner walls, a thicker tunica externa (collagen fibers), irregularly shaped lumens, and often contain valves to prevent backflow. They accommodate large blood volumes at low pressure.
Capillaries: Smallest and most numerous vessels; consist only of endothelium and a basement membrane, facilitating exchange of gases, nutrients, and wastes between blood and tissues.
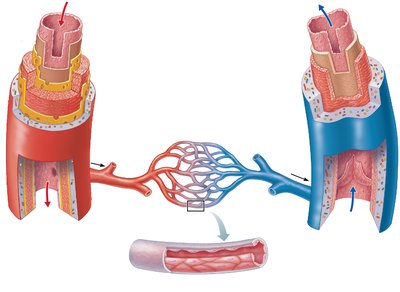
Relationship of Blood Vessels and Lymphatic Vessels
Blood vessels work closely with the lymphatic system to circulate body fluids. Lymphatic vessels collect excess interstitial fluid from capillary beds and return it to the bloodstream near the heart.
Arteries: Carry blood away from the heart toward capillaries.
Veins: Carry blood from capillaries back toward the heart.
Lymphatic vessels: Collect and transport interstitial fluid (lymph) to large veins near the heart.
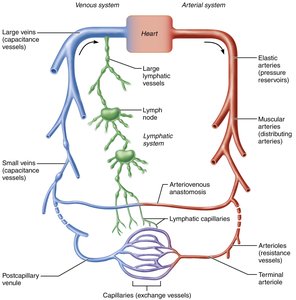
Circulatory Pathways
Pulmonary Circulation
Pulmonary circulation is a short loop that carries deoxygenated blood from the heart to the lungs for gas exchange and returns oxygenated blood to the heart.
Pulmonary arteries: Carry oxygen-poor blood from the right ventricle to the lungs.
Pulmonary veins: Return oxygen-rich blood from the lungs to the left atrium.

Systemic Circulation
Systemic circulation is a long loop that delivers oxygenated blood from the heart to all body tissues and returns deoxygenated blood to the heart.
Aorta: Main systemic artery distributing oxygenated blood.
Venae cavae: Main systemic veins returning deoxygenated blood.
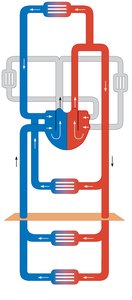
Major Arterial Pathways
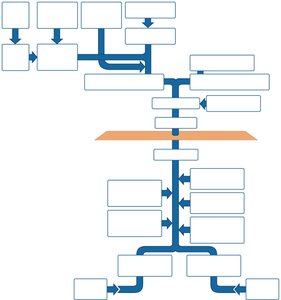
Branching and Naming of Arteries
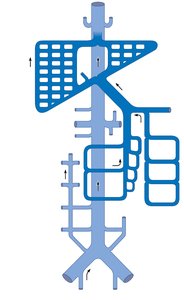
Arteries branch and change names as they move away from the aorta and enter different regions or organs. Schematic flowcharts help visualize these branching patterns.
Arteries are named for: Region or organ served, bone followed, or direction of blood flow.
Arteries change names: As they branch or change region.
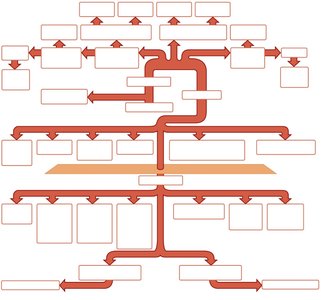
Arteries of the Head, Neck, and Brain
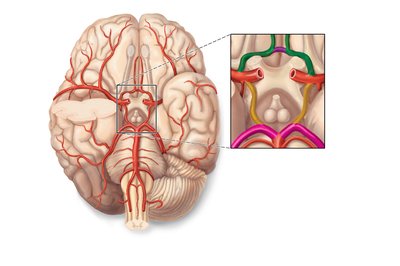
Cerebral Arterial Circle (Circle of Willis)
The Circle of Willis is a series of interconnected arteries on the inferior surface of the brain, ensuring continuous oxygenated blood supply to the entire brain.
Components: Anterior and posterior communicating arteries, anterior and posterior cerebral arteries, internal carotid arteries, basilar artery.
Function: Provides collateral circulation to prevent ischemia.
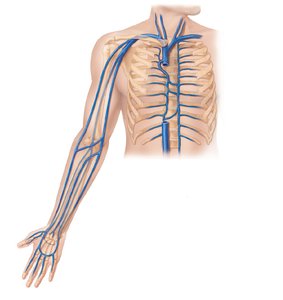
Arteries of the Upper Limb and Thorax
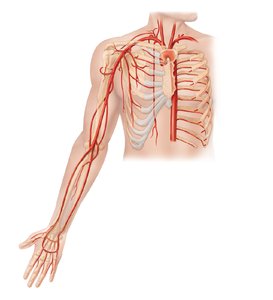
Major Branches
Arteries supplying the upper limb and thorax include the subclavian, axillary, brachial, radial, and ulnar arteries, as well as branches to the thoracic wall and mediastinal structures.
Subclavian artery: Supplies neck and upper limb.
Brachial artery: Main artery of the arm.
Radial and ulnar arteries: Supply forearm and hand.
Arteries of the Abdomen and Pelvis
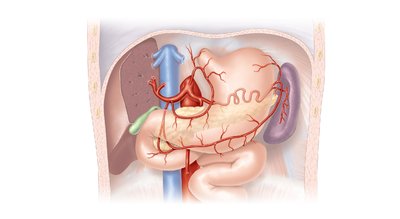
Celiac Trunk and Major Branches
The celiac trunk is a major abdominal artery supplying the liver, stomach, spleen, and other organs. The abdominal aorta gives rise to several important branches.
Celiac trunk: Branches into left gastric, splenic, and common hepatic arteries.
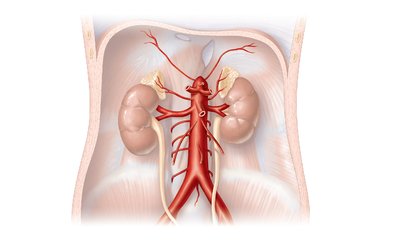
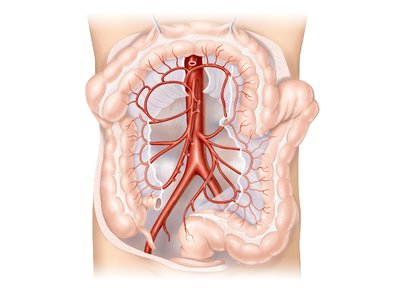
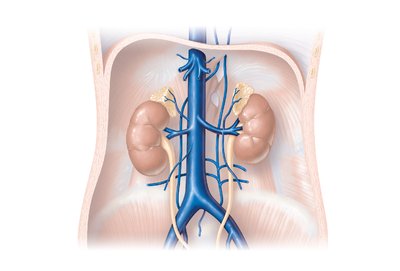
Superior and inferior mesenteric arteries: Supply intestines and colon.
Renal and gonadal arteries: Supply kidneys and reproductive organs.
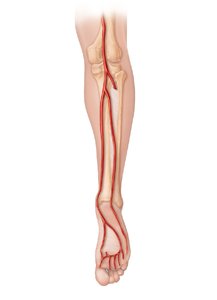
Arteries of the Lower Limb
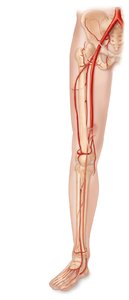
Major Branches
Arteries of the pelvis and lower limb include the common iliac, internal and external iliac, femoral, popliteal, tibial, and fibular arteries.
Femoral artery: Main artery of the thigh.
Popliteal artery: Supplies knee region.
Tibial and fibular arteries: Supply lower leg and foot.
Major Venous Pathways
Systemic Veins and Venae Cavae
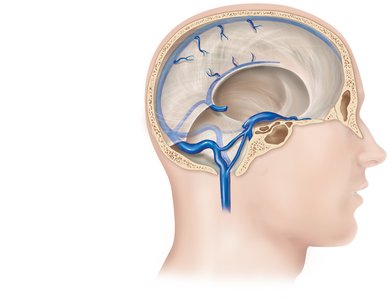
Veins return blood to the heart via the superior and inferior venae cavae. Venous pathways are more interconnected than arterial pathways, with many anastomoses and unique drainage systems for the brain and digestive organs.
Superficial and deep veins: Superficial veins are under the skin; deep veins often share names with arteries.
Dural venous sinuses: Drain blood from the brain.
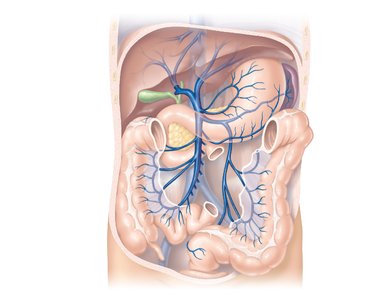
Hepatic portal system: Drains blood from digestive organs through the liver before returning to the heart.
Blood Vessel Walls: Layers
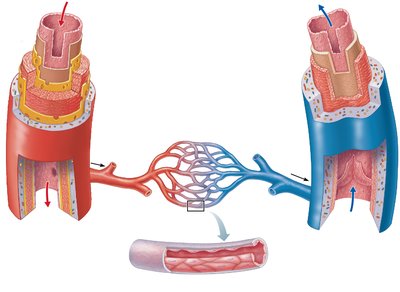
Three Layers (Tunics)
All blood vessels except capillaries have three layers:
Tunica intima: Innermost layer; endothelium and subendothelial layer.
Tunica media: Middle layer; smooth muscle and elastic fibers, regulated by sympathetic nerves.
Tunica externa: Outermost layer; collagen fibers, vasa vasorum, and nerve fibers.
Types of Arteries
Elastic (Conducting) Arteries
Elastic arteries are thick-walled vessels near the heart (e.g., aorta), acting as pressure reservoirs that expand and recoil with each heartbeat.
Function: Conduct blood from heart to medium-sized arteries; maintain continuous blood flow.
Clinical note: Aneurysms may occur if walls are weakened.
Muscular (Distributing) Arteries
Muscular arteries deliver blood to specific organs and have the thickest tunica media, allowing for active regulation of blood flow.
Function: Distribute blood to various regions; more vasoactive than elastic arteries.
Arterioles (Resistance Vessels)
Arterioles are the smallest arteries, controlling blood flow into capillary beds via vasoconstriction and vasodilation.
Function: Regulate resistance and blood flow to tissues.
Types of Capillaries
Continuous Capillaries
Continuous capillaries are the least permeable and most common, found in skin, muscles, lungs, and CNS.
Structure: Endothelial cells joined by tight junctions, with intercellular clefts for limited passage.
Function: Provide selective exchange; form blood-brain barrier in CNS.
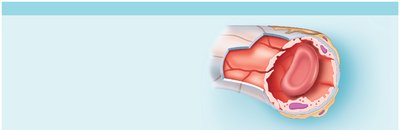
Fenestrated Capillaries
Fenestrated capillaries have pores (fenestrations) that increase permeability, found in kidneys, intestines, and endocrine glands.
Function: Facilitate rapid filtration and absorption.
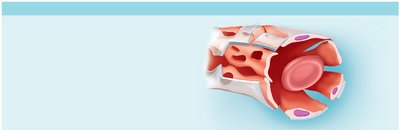
Sinusoidal Capillaries
Sinusoidal capillaries are the most permeable, found in liver, bone marrow, spleen, and adrenal medulla.
Structure: Large lumens, incomplete basement membrane, large intercellular clefts.
Function: Allow passage of large molecules and cells.
Capillary Beds and Blood Flow Regulation
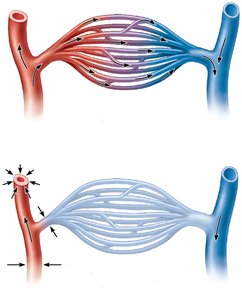
Typical Capillary Bed Anatomy
Capillary beds are networks of capillaries between arterioles and venules, providing sites for exchange of gases, nutrients, and wastes.
Blood flow regulation: Controlled by diameter of terminal arteriole and upstream arterioles.
Metabolic demand: Changes in tissue activity alter blood flow requirements.
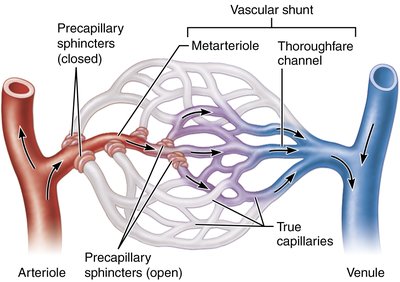
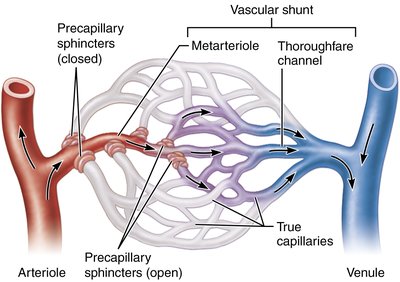
Mesenteric Capillary Bed
Capillary beds in intestinal mesenteries feature vascular shunts and precapillary sphincters, regulating blood flow based on local chemical conditions.
Vascular shunt: Direct channel connecting arteriole to venule, bypassing true capillaries.
Precapillary sphincters: Smooth muscle cuffs controlling entry into capillaries.
Venous System and Adaptations
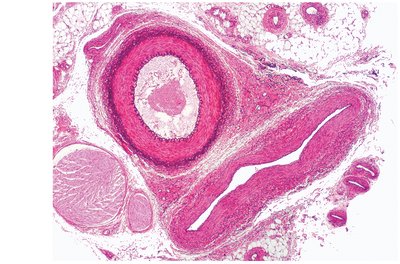
Vein Structure and Function
Veins have thinner walls, larger lumens, and lower pressure than arteries. They serve as capacitance vessels and blood reservoirs, containing up to 65% of blood volume.
Venous valves: Prevent backflow, especially in limbs.
Venous sinuses: Specialized, flattened veins with thin walls (e.g., coronary sinus, dural sinuses).
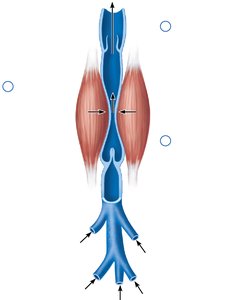
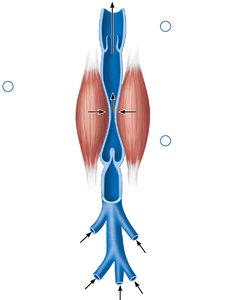
Venous Return Mechanisms
Venous return is aided by several mechanisms:
Large diameter lumens: Reduce resistance.
Valves: Ensure one-way flow.
Skeletal muscle pump: Muscle contractions compress veins, propelling blood toward the heart.
Respiratory pump: Pressure changes during breathing move blood toward the heart.
Anastomoses and Special Circulatory Features
Arterial and Venous Anastomoses
Anastomoses are interconnections between blood vessels, providing alternate pathways for blood flow.
Arterial anastomoses: Ensure continuous blood flow to tissues.
Venous anastomoses: So abundant that occluded veins rarely block blood flow.
Arteriovenous anastomoses: Shunts across capillary beds.
Blood Flow, Pressure, and Resistance
Key Terms and Relationships
Blood flow, blood pressure, and resistance are fundamental concepts in circulatory physiology.
Blood flow (F): Amount of blood flowing through a vessel per unit time (ml/min).
Blood pressure (BP): Force exerted by blood on vessel walls, measured in mmHg.
Resistance (TPR): Opposition to flow, mainly due to vessel diameter, length, and blood viscosity.
Relationship:
Where is the pressure gradient and TPR is total peripheral resistance.

Blood Pressure Regulation
Short-Term Regulation
Short-term regulation of blood pressure involves neural and hormonal controls.
Neural controls: Baroreceptor and chemoreceptor reflexes, cardiovascular center in medulla oblongata.
Hormonal controls: Epinephrine, norepinephrine, angiotensin II, ADH, aldosterone, and ANP.
Long-Term Regulation
Long-term regulation is achieved by renal mechanisms, controlling blood volume via direct and indirect (renin-angiotensin-aldosterone system) pathways.
Direct renal mechanism: Adjusts urine output to regulate blood volume.
Indirect mechanism: Renin release triggers angiotensin II formation, increasing blood pressure and volume.
Summary Table: Effects of Selected Hormones on Blood Pressure
Hormone | Effect on BP | Variable Affected | Site of Action |
|---|---|---|---|
Epinephrine/Norepinephrine | Increase | CO (HR & contractility), TPR (vasoconstriction) | Heart, arterioles |
Angiotensin II | Increase | TPR (vasoconstriction) | Arterioles |
ADH | Increase | TPR (vasoconstriction), blood volume (water retention) | Arterioles, kidneys |
Aldosterone | Increase | Blood volume (salt & water retention) | Kidneys |
ANP | Decrease | Blood volume (salt & water loss), TPR (vasodilation) | Kidneys, arterioles |
Summary
The cardiovascular system relies on a complex network of arteries, veins, and capillaries to transport blood, regulate pressure, and ensure tissue perfusion. Understanding the structure, function, and regulation of blood vessels is essential for comprehending circulatory physiology and its clinical implications.
