 Back
BackBlood Vessels and Hemodynamics: Structure, Function, and Regulation
Study Guide - Smart Notes

Chapter 18: Blood Vessels
Overview of Blood Vessels
Blood vessels are essential components of the circulatory system, responsible for transporting blood throughout the body. They are classified into three main types: arteries, veins, and capillaries, each with distinct structures and functions.
Arteries: Carry blood away from the heart. They are subdivided into elastic arteries (large, stretchy, absorb pressure) and muscular arteries (smaller, control blood flow to organs).
Veins: Carry blood toward the heart. They have thinner walls, larger lumens, and often contain valves to prevent backflow.
Capillaries: Serve as sites of exchange for gases, nutrients, and wastes between blood and tissues. They have thin walls to facilitate diffusion.
Tunics of Blood Vessels
Blood vessel walls are composed of three layers, or tunics, each with specific tissue types and functions:
Tunica Intima (interna): The innermost layer, composed of endothelium (simple squamous epithelium), basal lamina, subendothelial connective tissue, and internal elastic lamina. Provides a smooth lining to reduce friction.
Tunica Media: The middle layer, made of smooth muscle cells and elastic fibers. Responsible for vasoconstriction and vasodilation, controlled by the autonomic nervous system (ANS).
Tunica Externa (adventitia): The outermost layer, consisting of connective tissue. Provides protection and structural support.
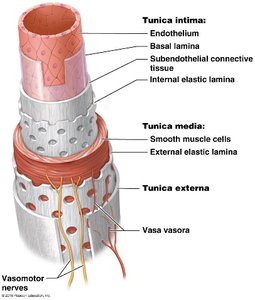
Structural Differences Between Arteries and Veins
Arteries: Thicker walls, smaller lumen, no valves. Designed to withstand higher pressure.
Veins: Thinner walls, larger lumen, contain valves to prevent backflow due to lower pressure.
Atherosclerosis
Atherosclerosis is a disease characterized by the buildup of plaque in arteries, leading to reduced blood flow and increased risk of cardiovascular events.
Causes: Injury to the endothelium from high blood pressure, high cholesterol, diabetes, and unhealthy lifestyle choices.
Treatment: Lifestyle changes, medications, and surgical interventions such as stents or bypass grafts.

Module 18.2: Hemodynamics – Physiology of Blood Flow
Factors Influencing Blood Flow
Hemodynamics refers to the study of blood flow and the forces involved. Blood flow is primarily influenced by pressure and resistance.
Pressure: As pressure increases, blood flow increases.
Resistance: As resistance increases, blood flow decreases.
Velocity of Blood Flow
As cross-sectional area increases, velocity of blood flow decreases.
Velocity is slowest in capillaries, which is beneficial for the exchange of gases and nutrients.
Factors Affecting Blood Pressure
Blood pressure is determined by several interrelated factors:
Peripheral Resistance (PR): Influenced by blood vessel length, blood viscosity, vessel radius, and obstructions.
Cardiac Output (CO): Product of heart rate and stroke volume. An increase in CO raises blood pressure.
Blood Volume: Regulated by the kidneys and hormones. Increased blood volume raises blood pressure.
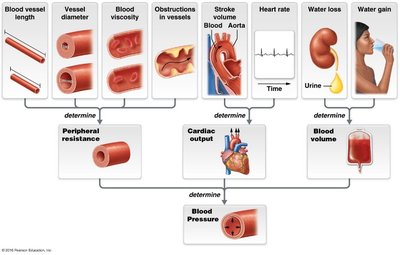
Summary Table: Factors Affecting Blood Pressure
Factor | Effect on Resistance (R) |
|---|---|
Blood vessel length | Increase length → Increase R |
Blood viscosity | Increase viscosity → Increase R |
Blood vessel radius | Decrease radius → Increase R |
Obstructions | Increase obstructions → Increase R |
Blood Pressure Variations in Circulation
Pulmonary Circuit: Low blood pressure, protects delicate lung tissue.
Systemic Circuit: High blood pressure, necessary for effective tissue perfusion.
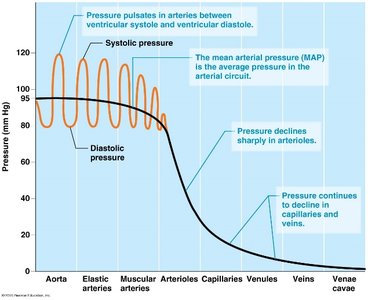
Systemic Arterial Pressure
Systolic Pressure: Pressure in the artery during ventricular contraction.
Diastolic Pressure: Pressure in the artery during ventricular relaxation.
Pulse Pressure: Difference between systolic and diastolic pressures.
Mean Arterial Pressure (MAP): Average pressure in the arteries, calculated as
Venous Return
Venous return is the flow of blood back to the heart. Because venous pressure is low, several mechanisms assist this process:
Valves prevent backflow.
Smooth muscle contraction in the tunica media helps propel blood.
Skeletal muscle pump squeezes veins during muscle contraction.
Respiratory pump uses pressure changes during breathing to move blood toward the heart.
Module 18.3: Regulation of Blood Pressure
Types of Regulation
Short-Term Regulation: Modifies cardiac output and resistance, primarily via the nervous and endocrine systems.
Long-Term Regulation: Modifies blood volume, primarily via the urinary and endocrine systems.
Short-Term Regulation
Sympathetic Nervous System: Increases heart rate, contractility, and vasoconstriction, raising blood pressure.
Parasympathetic Nervous System: Decreases heart rate and cardiac output, lowering blood pressure.
Baroreceptors: Detect changes in blood pressure and initiate feedback loops to maintain homeostasis.
Endocrine System in Short-Term Regulation
Hormone | Effect on Cardiac Output | Effect on Resistance |
|---|---|---|
Epinephrine/Norepinephrine | Increase CO | Increase R (vasoconstriction) |
Thyroid hormone | Upregulates receptors for E/NE | Upregulates receptors for E/NE |
Angiotensin II | - | Increase R (strong vasoconstrictor) |
ADH | - | Increase R (vasoconstriction) |
ANP | - | Decrease R (vasodilation) |
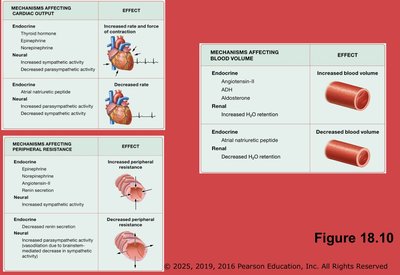
Long-Term Regulation
Achieved by adjusting blood volume through hormonal and renal mechanisms.
Key hormones: Angiotensin II, Aldosterone, ADH (increase blood volume); ANP (decreases blood volume).
Module 18.4: Capillaries and Tissue Perfusion
Capillary Exchange Mechanisms
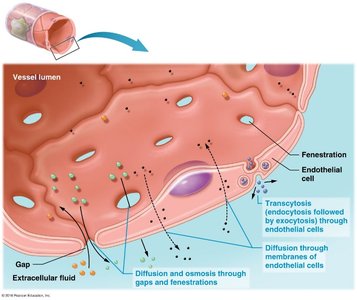
Capillaries allow for the exchange of gases, nutrients, and wastes through three main mechanisms:
Diffusion and osmosis through gaps and fenestrations
Diffusion through membranes of endothelial cells
Transcytosis (endocytosis followed by exocytosis)
Types of Capillaries
Type | Structure | Function | Location |
|---|---|---|---|
Continuous | Least leaky | Restricts passage of most substances | Muscle, brain |
Fenestrated | Have pores | Rapid exchange | Kidneys, intestine |
Sinusoid | Most leaky | Allows passage of large molecules | Liver, spleen |
Autoregulation of Blood Flow
Myogenic Mechanism: Smooth muscle in arterioles contracts in response to increased pressure, preventing excessive blood flow through capillaries.
Metabolic Mechanism: Local chemical changes (low O2, high CO2, low pH) cause vasodilation, increasing blood flow to meet metabolic needs.
Tissue Perfusion
Heart: Receives more blood during diastole.
Brain: Requires constant perfusion; interruption leads to loss of consciousness.
Skeletal Muscle: Perfusion increases with activity.
Skin: Perfusion regulated by the sympathetic nervous system to control temperature.
Module 18.5: Capillary Pressures and Fluid Movement
Types of Pressures in Capillaries
Hydrostatic Pressure (HP): The force exerted by a fluid against a wall. HPc (capillary hydrostatic pressure) pushes fluid out of the capillary; HPif (interstitial fluid hydrostatic pressure) pushes fluid into the capillary.
Osmotic Pressure (OP): The pull on water due to solute concentration. OPc (capillary osmotic pressure) pulls water into the capillary; OPif (interstitial fluid osmotic pressure) pulls water out.
Filtration and Reabsorption
Filtration: Movement of fluid out of the capillary (favored by HPc).
Reabsorption: Movement of fluid into the capillary (favored by OPc).
Net Filtration Pressure (NFP):
Edema
Edema is the accumulation of excess fluid in the interstitial space, caused by excessive filtration or inadequate reabsorption.
Capillary Bed Structure
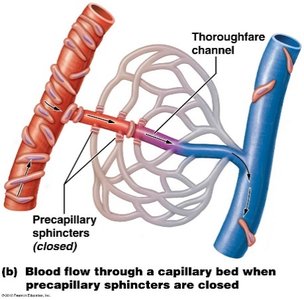
Additional info: These notes are based on the provided study materials and expanded with academic context for clarity and completeness. For further details, refer to your textbook and class resources.
