 Back
BackBones and Bone Tissue: Structure, Function, and Growth
Study Guide - Smart Notes

Bones and Bone Tissue
Overview of the Skeletal System
The skeletal system is a complex organ system that provides the framework for the human body. It consists of bones, cartilage, ligaments, and connective tissues, each contributing to the system's structure and function.
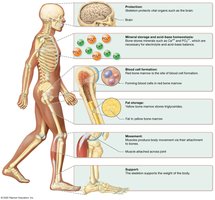
Support: The skeleton supports the body and maintains its shape.
Storage of Minerals and Lipids: Bones store essential minerals such as calcium and phosphate, as well as lipids in yellow marrow.
Blood Cell Production: Red marrow within bones produces red and white blood cells and platelets.
Protection: Bones protect vital organs (e.g., skull protects the brain, rib cage protects the heart and lungs).
Leverage: Bones act as levers for muscles, enabling movement.
Classification of Bones by Shape
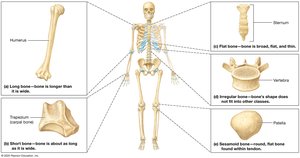
Bones are classified based on their shapes and internal tissue organization. There are six main types:
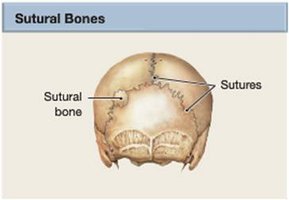
Sutural Bones: Small, irregular bones found between the flat bones of the skull. Their number and size can vary.
Irregular Bones: Complex shapes, such as vertebrae and pelvic bones.
Short Bones: Small and thick, found in the wrist and ankle.
Flat Bones: Thin with parallel surfaces, found in the skull, sternum, ribs, and scapula.
Long Bones: Long and thin, found in arms, legs, hands, feet, fingers, and toes.
Sesamoid Bones: Small, flat bones that develop inside tendons, commonly found near joints (e.g., patella).
Structure of a Long Bone
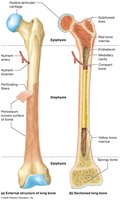
Long bones have a unique structure that supports their function in movement and support.
Diaphysis: The shaft, composed of compact bone surrounding a central medullary (marrow) cavity.
Epiphysis: The wide ends of the bone, mostly spongy bone covered by compact bone and articular cartilage.
Medullary Cavity: Central cavity filled with marrow (yellow or red, depending on age and bone).
Periosteum: Outer covering of bone, except at joint surfaces; consists of fibrous and cellular layers.
Endosteum: Lines the medullary cavity and covers trabeculae of spongy bone.
Bone Tissue Composition
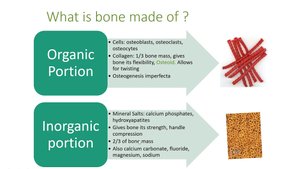
Bone is a specialized connective tissue with a dense matrix composed of organic and inorganic components.
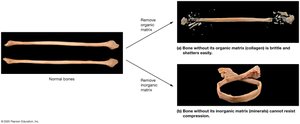
Organic Portion: Mainly collagen fibers (1/3 of bone mass), providing flexibility and tensile strength.
Inorganic Portion: Mainly hydroxyapatite (calcium phosphate crystals, 2/3 of bone mass), providing hardness and resistance to compression.
Osteocytes: Mature bone cells located in lacunae, responsible for maintaining the bone matrix.
Types of Bone Cells
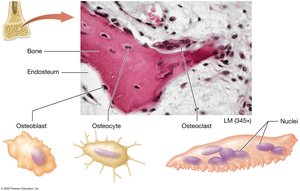
Bone contains four main types of cells, each with distinct functions:
Osteocytes: Mature bone cells that maintain the bone matrix and help repair damaged bone.
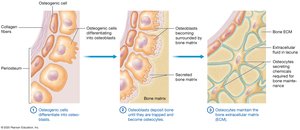
Osteoblasts: Immature bone cells that secrete osteoid (organic bone matrix) and eventually become osteocytes.
Osteoprogenitor Cells: Stem cells that divide to produce osteoblasts; important for bone growth and repair.
Osteoclasts: Large, multinucleate cells that break down bone matrix (osteolysis), releasing stored minerals.
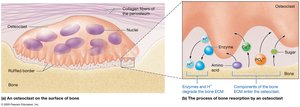
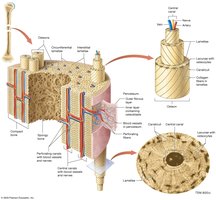
Histology of Bone: Compact and Spongy Bone
Bone tissue is organized into two main types: compact bone and spongy bone.
Compact Bone: Dense and strong, forms the outer layer of bones. The basic unit is the osteon, with concentric lamellae around a central canal containing blood vessels.
Spongy Bone: Consists of a network of trabeculae, making bones lighter and providing space for red marrow.
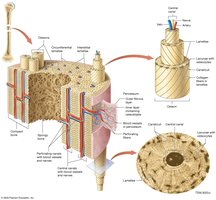
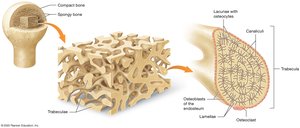
Bone Membranes
Bones are covered by specialized membranes that play roles in growth, repair, and attachment.
Periosteum: Covers the external surface of bones (except at joints); provides attachment for tendons and ligaments.
Endosteum: Lines the internal surfaces, including the medullary cavity and trabeculae of spongy bone; contains bone-forming and bone-resorbing cells.
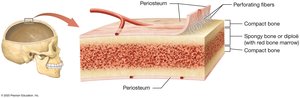
Bone Formation: Ossification
Ossification is the process of bone formation, which occurs through two main mechanisms:
Endochondral Ossification: Bone replaces a hyaline cartilage model; most bones form this way.
Intramembranous Ossification: Bone develops directly from mesenchymal tissue; forms flat bones like the skull and clavicle.
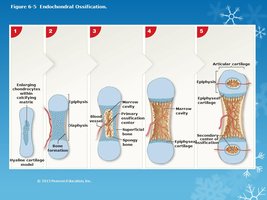
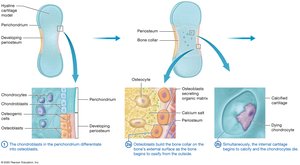
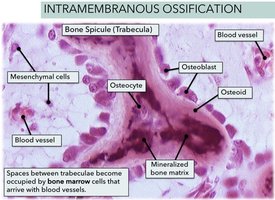
Bone Growth in Length and Width
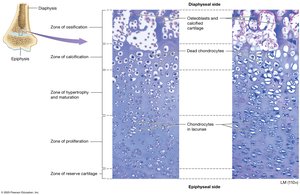
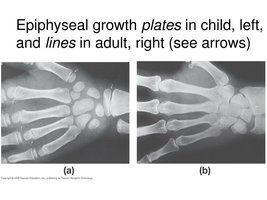
Bones grow in length at the epiphyseal plate and in width by appositional growth.
Longitudinal Growth: Occurs at the epiphyseal plate, which has five zones: reserve cartilage, proliferation, hypertrophy, calcification, and ossification.
Appositional Growth: Increases bone diameter by adding new bone to the surface.
Hormonal Regulation of Bone Growth
Bone growth and remodeling are regulated by hormones that maintain calcium homeostasis and stimulate bone formation or resorption.
Parathyroid Hormone (PTH): Increases blood calcium by stimulating osteoclasts, increasing intestinal absorption, and reducing kidney excretion.
Calcitonin: Lowers blood calcium by inhibiting osteoclasts and increasing calcium excretion by the kidneys.
Other Hormones: Growth hormone, thyroid hormone, estrogens, and androgens stimulate bone growth; vitamin D is essential for calcium absorption.
Bone Remodeling and Repair
Bone remodeling is a continuous process involving the resorption and deposition of bone tissue, allowing bones to adapt to stress and repair damage.
Remodeling: Involves osteocytes, osteoblasts, and osteoclasts; influenced by mechanical stress, hormones, and nutrition.
Repair: After a fracture, bone undergoes a series of steps: hematoma formation, fibrocartilaginous callus formation, bony callus formation, and bone remodeling.
Effects of Aging on the Skeletal System
With age, bones become thinner and weaker due to decreased osteoblast activity and unchanged osteoclast activity. This leads to osteopenia and increased risk of fractures, especially in women after menopause due to decreased estrogen levels.
Bone Cell Type | Function |
|---|---|
Osteocyte | Maintains bone matrix |
Osteoblast | Builds bone matrix |
Osteoprogenitor | Stem cell for osteoblasts |
Osteoclast | Resorbs bone matrix |
Key Equations:
Calcium Homeostasis (simplified):
Example: Weight-bearing exercise increases osteoblast activity, leading to stronger bones. In contrast, immobility or lack of stress leads to bone loss.
Additional info: Adequate intake of calcium, vitamin D, and regular physical activity are essential for maintaining bone health throughout life.
