 Back
BackBones and Skeletal Tissues: Structure, Composition, and Development
Study Guide - Smart Notes

Bones and Skeletal Tissues
Microscopic Anatomy of Bone
The microscopic structure of bone reveals specialized cells and organized matrix that provide strength, flexibility, and the ability to remodel in response to stress. Bone tissue contains several distinct cell types, each with unique functions in bone formation, maintenance, and resorption.
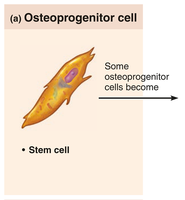
Osteoprogenitor (Osteogenic) Cells: Stem cells located in the periosteum and endosteum; they differentiate into osteoblasts or bone-lining cells when stimulated. Some remain as stem cells for future repair and growth.
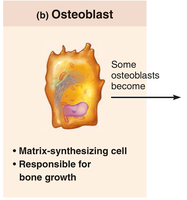
Osteoblasts: Bone-forming cells that secrete unmineralized bone matrix called osteoid, which is rich in collagen and calcium-binding proteins. Osteoblasts are actively mitotic and responsible for bone growth.
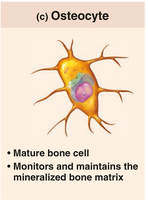
Osteocytes: Mature bone cells found in lacunae; they maintain the bone matrix and act as mechanosensors, communicating with osteoblasts and osteoclasts to coordinate bone remodeling.
Bone-Lining Cells: Flat cells on bone surfaces that help maintain the bone matrix. On external surfaces, they are called periosteal cells; on internal surfaces, endosteal cells.
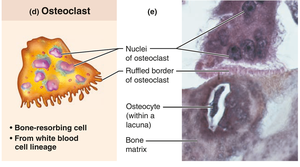
Osteoclasts: Large, multinucleate cells derived from hematopoietic stem cells; they resorb (break down) bone by secreting enzymes and acids. Osteoclasts are found in resorption bays and have ruffled borders to increase surface area for bone degradation.

Microscopic Anatomy of Compact Bone
Compact bone, also known as lamellar bone, is highly organized and forms the dense outer layer of all bones. Its structure is optimized for strength and resistance to stress.
Osteon (Haversian System): The structural unit of compact bone, consisting of concentric rings (lamellae) of bone matrix surrounding a central canal. Osteons run parallel to the long axis of the bone and act as weight-bearing pillars.
Lamellae: Layers of bone matrix within an osteon. Collagen fibers in adjacent lamellae run in different directions, providing resistance to twisting forces (torsion).
Central (Haversian) Canal: Runs through the core of each osteon, containing blood vessels and nerve fibers.
Perforating (Volkmann’s) Canals: Canals that run perpendicular to the central canals, connecting blood vessels and nerves of the periosteum, medullary cavity, and central canal.
Lacunae: Small cavities between lamellae that house osteocytes.
Canaliculi: Tiny channels connecting lacunae, allowing communication and nutrient/waste exchange between osteocytes.
Interstitial Lamellae: Incomplete lamellae that fill gaps between osteons or are remnants of old osteons.
Circumferential Lamellae: Lamellae that encircle the entire diaphysis, just deep to the periosteum, helping the bone resist twisting.





Microscopic Anatomy of Spongy Bone
Spongy (cancellous) bone appears less organized than compact bone but is structured to provide strength along lines of stress. It consists of a network of trabeculae, which are small, needle-like pieces of bone.
Trabeculae: Irregularly arranged lamellae and osteocytes interconnected by canaliculi. Trabeculae align along lines of stress, providing structural support without excessive weight.
Spaces: The spaces between trabeculae are filled with bone marrow and blood vessels, which supply nutrients to the bone cells.

Chemical Composition of Bone
Bone is a composite material made up of organic and inorganic components, each contributing to its unique properties.
Organic Components (30% of bone tissue):
Bone Cells: Make up about 2% of the organic component.
Osteoid: Unmineralized bone matrix formed by osteoblasts, comprising 95% collagen fibers. Collagen provides tensile strength and flexibility.
Sacrificial Bonds: Weak bonds between collagen molecules that break under stress to dissipate energy and prevent fractures. These bonds can reform if no additional trauma occurs.
Inorganic Components (70% of bone tissue):
Hydroxyapatites (Mineral Salts): Make up 95% of the inorganic component and 65% of bone mass. Composed mainly of calcium phosphate crystals, these provide hardness and resistance to compression.
Mechanical Properties: Bone is about half as strong as steel in resisting compression and as strong as steel in resisting tension.
Chemical Formula:


Bone Development (Ossification)
Overview of Ossification
Ossification, or osteogenesis, is the process of bone tissue formation. It occurs in three main stages: formation of the bony skeleton (prenatal), postnatal bone growth, and bone remodeling and repair throughout life.
Prenatal Ossification: Involves two processes—endochondral ossification and intramembranous ossification.
Postnatal Bone Growth: Occurs from birth until early adulthood, primarily through the activity of the epiphyseal plates.
Bone Remodeling and Repair: Continues throughout life to maintain bone strength and integrity.
Endochondral Ossification
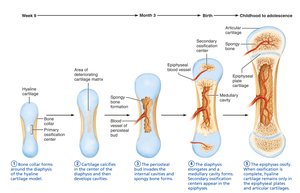
Endochondral ossification is the process by which most bones of the body are formed, especially those inferior to the base of the skull (except the clavicles). Bone develops by replacing hyaline cartilage models.
Bone collar forms around the diaphysis of the cartilage model.
Central cartilage in the diaphysis calcifies and develops cavities.
Periosteal bud invades the cavities, forming spongy bone.
Diaphysis elongates and a medullary cavity forms; secondary ossification centers appear in the epiphyses.
Epiphyses ossify; hyaline cartilage remains only in the epiphyseal plates and articular cartilages.
Intramembranous Ossification
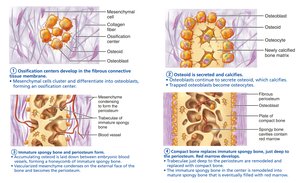
Intramembranous ossification forms the cranial bones of the skull and the clavicles. Bone develops directly from fibrous connective tissue membranes.
Ossification centers form when mesenchymal cells cluster and become osteoblasts.
Osteoid is secreted and then calcified.
Woven bone and periosteum form as osteoid is laid down around blood vessels, resulting in trabeculae.
Lamellar bone replaces woven bone, and red bone marrow appears.
Postnatal Bone Growth
Growth in Length of Long Bones
Long bones grow in length by interstitial (longitudinal) growth at the epiphyseal plate, a layer of hyaline cartilage. The plate maintains a constant thickness as cartilage growth on one side is balanced by bone replacement on the other.
Zones of the Epiphyseal Plate:
Resting (quiescent) zone: Relatively inactive cartilage on the epiphyseal side.
Proliferation (growth) zone: Rapidly dividing cartilage cells on the diaphysis side; new cells push the epiphysis away from the diaphysis, lengthening the bone.
Hypertrophic zone: Older chondrocytes enlarge, and lacunae erode, forming spaces.
Calcification zone: Surrounding cartilage matrix calcifies; chondrocytes die and deteriorate.
Ossification (osteogenic) zone: Calcified cartilage spicules are eroded by osteoclasts and covered with new bone by osteoblasts, forming spongy bone.
Near the end of adolescence, the epiphyseal plate thins and is replaced by bone, resulting in epiphyseal plate closure and cessation of bone lengthening (around age 18 in females, 21 in males).

Growth in Width (Thickness)
Bones increase in thickness (appositional growth) throughout life in response to stress from muscle activity or added weight. Osteoblasts beneath the periosteum secrete bone matrix on the external surface, while osteoclasts remove bone from the endosteal surface. Usually, more bone is built than removed, resulting in thicker, stronger bones.
Hormonal Regulation of Bone Growth
Bone growth is regulated by several hormones:
Growth Hormone: Stimulates epiphyseal plate activity in infancy and childhood.
Thyroid Hormone: Modulates the activity of growth hormone, ensuring proper skeletal proportions.
Sex Hormones (Testosterone and Estrogens): Promote adolescent growth spurts and induce epiphyseal plate closure, ending longitudinal bone growth.
Imbalances in these hormones can lead to abnormal skeletal growth.
