 Back
BackBones and Skeletal Tissues: Structure, Function, and Development
Study Guide - Smart Notes

Bones and Skeletal Tissues
Introduction
The skeletal system is fundamental to human anatomy and physiology, providing structure, protection, and facilitating movement. Understanding bone anatomy and bone remodeling is essential for clinical practice, especially in the context of bone diseases such as osteoporosis.
Cartilages Help Form the Skeleton
Structure and Function of Cartilage
Cartilage is a resilient, flexible tissue that forms the initial skeleton in the human embryo and persists in areas requiring flexibility. It is composed primarily of water, lacks blood vessels and nerves, and is surrounded by the perichondrium, a dense connective tissue layer that resists expansion and delivers nutrients.
Skeletal cartilage: Made of chondrocytes in lacunae within a jelly-like matrix.
Perichondrium: Surrounds cartilage, provides nutrients, and resists expansion.
Types of Cartilage
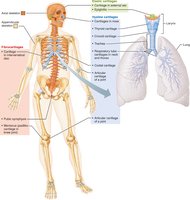
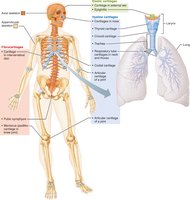
Hyaline cartilage: Most abundant; provides support and flexibility. Found in joints, ribs, respiratory passages, and nose.
Elastic cartilage: Contains elastic fibers; found in external ear and epiglottis.
Fibrocartilage: Thick collagen fibers; high tensile strength. Found in knee menisci, pubic symphysis, and intervertebral discs.
Growth of Cartilage
Appositional growth: New matrix added to the surface by cells in the perichondrium.
Interstitial growth: Chondrocytes divide and secrete new matrix within the cartilage.
Cartilage growth ends during adolescence.
Functions of Bones
Seven Major Functions
Support: Framework for the body and soft organs.
Protection: Shields brain, spinal cord, and vital organs.
Anchorage: Acts as levers for muscle action.
Mineral storage: Stores calcium and phosphorus.
Blood cell formation: Hematopoiesis in red bone marrow.
Triglyceride storage: Fat stored in bone cavities.
Hormone production: Osteocalcin regulates insulin and energy expenditure.
Classification of Bones
By Location
Axial skeleton: Skull, vertebral column, rib cage.
Appendicular skeleton: Limbs and girdles attaching limbs to axial skeleton.
By Shape
Long bones: Longer than wide, with a medullary cavity. Example: femur.
Short bones: Cube-shaped. Example: wrist and ankle bones. Sesamoid bones form within tendons (e.g., patella).
Flat bones: Thin, flat, slightly curved. Example: sternum, ribs, cranial bones.
Irregular bones: Complex shapes. Example: vertebrae, hip bones.
Bone Structure
Gross Anatomy of Compact and Spongy Bone
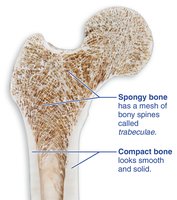
Bones are organs composed of various tissues. The two main types of bone tissue are compact bone and spongy bone.
Compact bone: Dense, smooth, and solid outer layer.
Spongy bone: Honeycomb structure of trabeculae, with spaces filled by bone marrow.
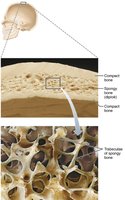
Structure of Short, Irregular, and Flat Bones
Thin plates of spongy bone (diploe) covered by compact bone.
Periosteum covers outside; endosteum covers inside.
Bone marrow scattered throughout spongy bone; no defined cavity.
Hyaline cartilage covers joint surfaces.
Structure of a Typical Long Bone
Diaphysis: Shaft; compact bone surrounds medullary cavity (yellow marrow in adults).
Epiphyses: Ends; compact bone externally, spongy bone internally. Articular cartilage covers joint surfaces.
Epiphyseal line: Remnant of growth plate.
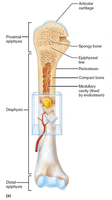
Membranes of Long Bones
Periosteum: Double-layered membrane covering external surfaces (except joints). Fibrous layer (outer), osteogenic layer (inner).
Endosteum: Delicate membrane covering internal surfaces, including trabeculae and canals.
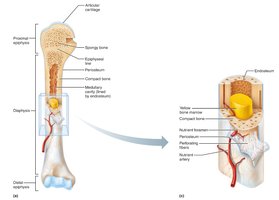
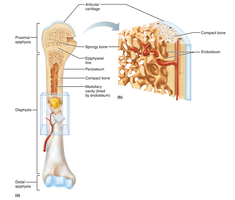
Hematopoietic Tissue in Bones (Bone Marrow)
Red and Yellow Marrow
Red marrow: Hematopoietic tissue producing blood cells. In children, found in nearly every bone; in adults, limited to axial skeleton and proximal limb bones.
Yellow marrow: Fatty marrow; replaces red marrow in adults, does not produce blood cells. Can revert to red marrow if needed.
Microscopic Anatomy of Bone
Cells of Bone Tissue
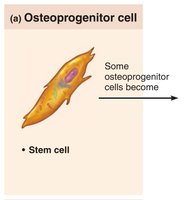
Bone tissue contains five major cell types, all derived from a common lineage.
Osteoprogenitor (osteogenic) cells: Stem cells from mesenchyme; differentiate into osteoblasts or bone-lining cells.
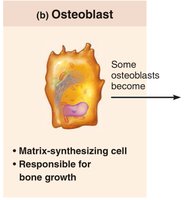
Osteoblasts: Bone-forming cells; secrete osteoid (collagen and calcium-binding proteins).
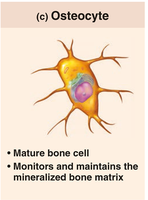
Osteocytes: Mature bone cells in lacunae; maintain matrix and act as stress sensors.
Bone-lining cells: Flat cells maintaining matrix; periosteal (external) and endosteal (internal).
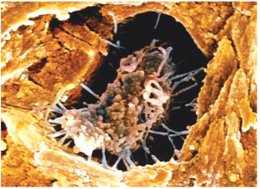
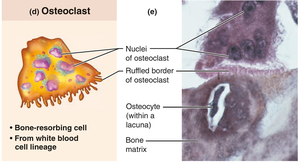
Osteoclasts: Multinucleate cells from hematopoietic lineage; resorb bone.
Microscopic Anatomy of Compact Bone
Osteon (Haversian System)
The osteon is the structural unit of compact bone, consisting of concentric rings (lamellae) that withstand stress and resist twisting.
Lamellae: Collagen fibers run in different directions in adjacent rings.
Bone salts: Located between collagen fibers.
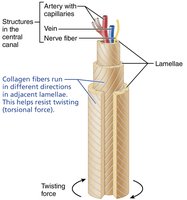
Canals and Canaliculi
Central (Haversian) canal: Contains blood vessels and nerves.
Perforating (Volkmann's) canals: Connect periosteum, medullary cavity, and central canal.
Lacunae: Small cavities with osteocytes.
Canaliculi: Hairlike canals connecting lacunae and central canal; allow communication and nutrient/waste exchange.
Interstitial and Circumferential Lamellae
Interstitial lamellae: Fill gaps between osteons or are remnants of old osteons.
Circumferential lamellae: Extend around the diaphysis, resist twisting.
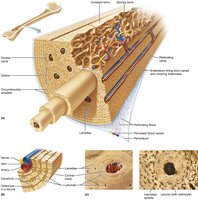
Microscopic Anatomy of Spongy Bone
Structure and Function
Spongy bone is organized along lines of stress, with trabeculae conferring strength. It lacks osteons but contains lamellae and osteocytes interconnected by canaliculi. Capillaries in the endosteum supply nutrients.
Chemical Composition of Bone
Organic Components
Includes bone cells and osteoid (ground substance and collagen fibers).
Provides tensile strength and flexibility.
Sacrificial bonds in collagen dissipate energy and prevent fractures.
Inorganic Components
Hydroxyapatites (mineral salts): Calcium phosphate crystals; 65% of bone mass.
Responsible for hardness and resistance to compression.
Bones are strong and durable, lasting long after death.
Bone Development (Ossification)
Overview
Ossification is the process of bone tissue formation, beginning in the second month of development and continuing throughout life.
Endochondral ossification: Bone replaces hyaline cartilage; forms most bones below the skull.
Intramembranous ossification: Bone develops from fibrous membrane; forms cranial bones and clavicles.
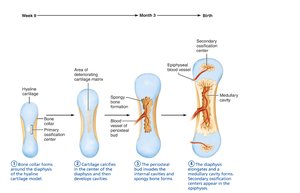
Endochondral Ossification
Begins at primary ossification center in shaft.
Blood vessels infiltrate perichondrium, converting it to periosteum.
Mesenchymal cells become osteoblasts.
Five main steps: bone collar formation, cartilage calcification, periosteal bud invasion, diaphysis elongation, epiphyses ossification.
Hyaline cartilage remains in epiphyseal plates and articular cartilages.
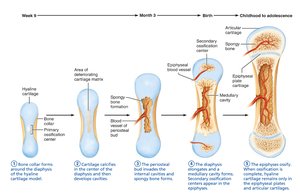
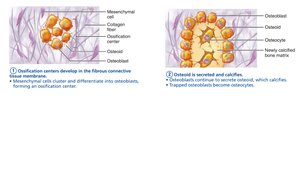
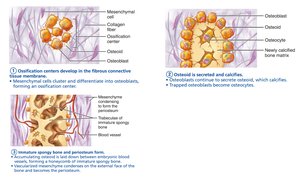
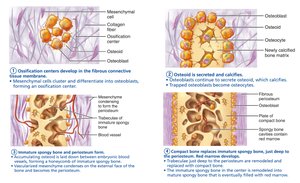
Intramembranous Ossification
Begins within fibrous connective tissue membranes.
Four steps: formation of ossification centers, secretion and calcification of osteoid, formation of woven bone and periosteum, replacement by lamellar bone and appearance of red marrow.
Postnatal Bone Growth
Growth Mechanisms
Interstitial (longitudinal) growth: Lengthwise growth at epiphyseal plate.
Appositional growth: Increase in thickness.
Bones stop growing during adolescence, except some facial bones.
