 Back
BackCartilage and Bone: Structure, Types, Growth, and Repair
Study Guide - Smart Notes

Cartilage
Structure of Cartilage
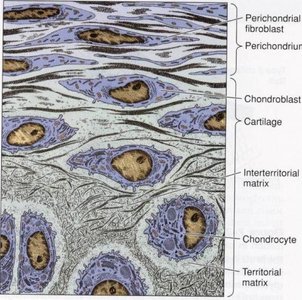
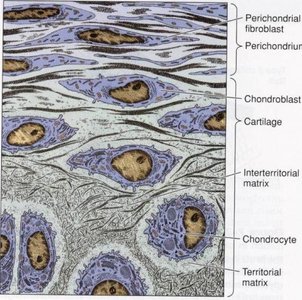
Cartilage is a specialized connective tissue composed of cells and an extensive extracellular matrix. It is avascular, meaning it lacks blood vessels, and receives nutrients by diffusion from surrounding tissues.
Cells: Chondroblasts (immature, matrix-secreting cells) and chondrocytes (mature cells residing in lacunae).
Matrix: Contains fibers (collagen and elastin), ground substance (rich in chondroitin sulfates and hyaluronic acid), and water.
Perichondrium: A dense connective tissue sheath covering most cartilage types, containing blood vessels, nerves, and fibroblasts.
Types of Cartilage
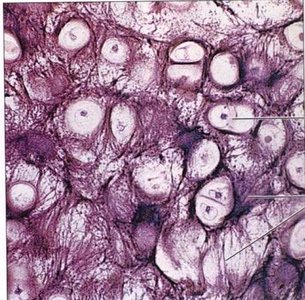
Cartilage is classified based on the composition of its matrix and location in the body.
Hyaline Cartilage: Most common type; matrix contains fine collagen fibers. Found in the epiphyseal plate, articular surfaces, larynx, trachea, and fetal skeleton.
Elastic Cartilage: Contains abundant elastic fibers, providing flexibility. Located in the external ear and epiglottis.
Fibrocartilage: Contains thick bundles of collagen fibers, making it very strong. Found in intervertebral discs and menisci of the knee joint.
Cartilage Growth
Cartilage grows by two mechanisms:
Appositional Growth: New chondrocytes are derived from the differentiation of perichondrial fibroblasts, adding layers to the surface.
Interstitial Growth: Division of existing chondrocytes within the matrix, expanding cartilage from within. Occurs in areas without perichondrium, such as articular cartilage and the epiphyseal plate.
Bone
Structure of Bone
Bone is a rigid connective tissue with a mineralized matrix, providing support and protection. It is highly vascularized and contains several cell types:
Osteoblasts: Bone-forming cells that secrete osteoid (unmineralized bone matrix).
Osteocytes: Mature bone cells residing in lacunae, maintaining bone tissue.
Osteoclasts: Large, multinucleated cells responsible for bone resorption.
The bone matrix consists of:
Organic components: Collagen type I, proteoglycans, and glycoproteins.
Inorganic components: Hydroxyapatite crystals (calcium and phosphate).
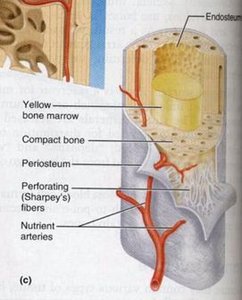
Periosteum and Endosteum
The periosteum is the external covering of bones, consisting of an outer fibrous layer and an inner osteogenic layer. The endosteum lines internal bone cavities and contains osteoprogenitor cells.
Functions: Nutrition, supply of bone-forming cells, and attachment via Sharpey's fibers.
Bone Cells
Osteoblasts: Develop from periosteal and endosteal osteoprogenitor cells, synthesize bone matrix, and are essential for bone formation.
Osteocytes: Derived from osteoblasts, maintain bone matrix, and reside in lacunae with cytoplasmic processes extending through canaliculi.
Osteoclasts: Derived from hematopoietic stem cells, responsible for bone resorption by secreting lysosomal enzymes and H+ ions.
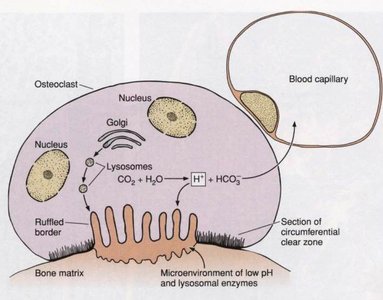
Types of Bone
Bones are classified by shape:
Long bones: e.g., humerus
Short bones: e.g., trapezoid (wrist)
Flat bones: e.g., sternum
Irregular bones: e.g., vertebrae
Bone Texture
Compact bone: Dense, solid, and smooth with no spaces.
Spongy bone (cancellous/trabecular): Honeycomb appearance with trabeculae and spaces filled with marrow.
Microscopic Arrangement of Compact Bone
The structural unit is the osteon (Haversian system):
Concentric lamellae of bone matrix surround a central canal containing blood vessels, nerves, and lymphatics.
Osteocytes occupy lacunae between lamellae, connected by canaliculi.
Haversian canals communicate with each other, the periosteum, and the marrow cavity via Volkmann's canals.
Microscopic Structure of Spongy Bone
Irregularly arranged lamellae form trabeculae.
Osteocytes reside in lacunae with canaliculi, but there are no osteons.
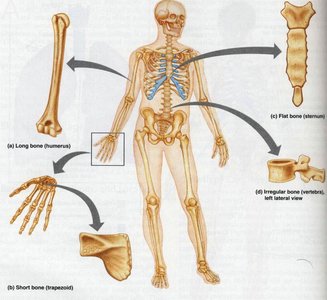
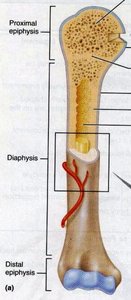
Parts of a Long Bone
Diaphysis: Shaft, composed of compact bone surrounding a marrow cavity.
Epiphysis: Ends of the bone, with an outer layer of compact bone and inner spongy bone; joint surfaces covered with hyaline cartilage.
Metaphysis: Region where diaphysis and epiphysis meet.
Blood Supply of Bone
Nutrient artery: Supplies the medullary cavity and inner compact bone.
Periosteal arteries: Supply the outer compact bone.
Epiphyseal arteries: Supply the epiphyses.
The metaphysis has the richest blood supply, with slow blood flow due to capillary loops.
Bone Formation (Ossification/Osteogenesis)
Bone develops from either fibrous membranes or hyaline cartilage in the fetal skeleton (before 8 weeks).
Intramembranous ossification: Mesenchymal cells differentiate into osteoblasts, which secrete osteoid that calcifies. Blood vessels invade, and compact bone forms externally with spongy bone at the center. Occurs in the skull cap and clavicle.
Endochondral ossification: Bone forms by replacing hyaline cartilage. A bone collar forms, cartilage calcifies and is destroyed, and osteoblasts form osteoid. The medullary cavity develops, and ossification centers appear in the diaphysis (primary) and epiphyses (secondary). All bones except the skull cap and clavicle form this way.
Bone Growth
Longitudinal bone growth occurs at the epiphyseal plate:
Growth zone: Cartilage cells multiply on the epiphyseal side.
Transformation zone: Cartilage cells enlarge, matrix calcifies, and cells die.
Osteogenic zone: Osteoblasts secrete osteoid, and osteoclasts remove calcified cartilage on the diaphyseal side.
Bone Repair
Bone repair occurs after a fracture through several stages:
Blood clot forms, and bone cells die.
Dead tissue is removed; fibroblasts invade and differentiate into chondroblasts, forming a soft callus of collagen and cartilage.
Osteoblasts invade, replacing cartilage with bone (bony callus).
Excess bone is removed, and the bone is remodeled to restore its original shape.
