 Back
BackChapter 15: The Respiratory System – Structure, Function, and Physiology
Study Guide - Smart Notes

The Respiratory System: Overview
Introduction to the Respiratory System
The respiratory system is responsible for the movement of air into and out of the lungs and for gas exchange between the air and the bloodstream. Gas exchange occurs at specialized structures called alveoli. The system also plays roles in sound production and olfaction (sense of smell).
Gas exchange between air and blood
Movement of air along passageways to and from gas-exchange surfaces
Protection of respiratory surfaces from dehydration, temperature changes, and pathogens
Production of sounds for communication
Assistance in olfaction
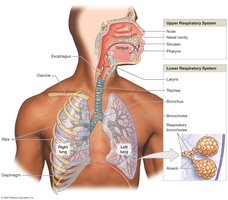
Organization of the Respiratory System
Anatomical Divisions
The respiratory system is divided into the upper respiratory system and the lower respiratory system:
Upper respiratory system: Nose, nasal cavity, paranasal sinuses, pharynx. Functions to filter, warm, and humidify incoming air.
Lower respiratory system: Larynx, trachea, bronchi, lungs (including bronchioles and alveoli).
Functional Zones
Conducting portion: Nasal cavity to larger bronchioles; filters, warms, and humidifies air.
Respiratory portion: Smallest bronchioles and alveoli; site of gas exchange.
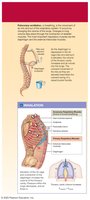
Respiratory Mucosa and Defense Mechanisms
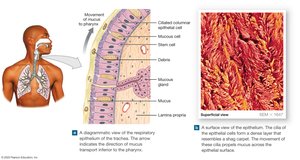
Respiratory Mucosa
The conducting portion is lined with respiratory mucosa, a ciliated columnar epithelium with mucous cells. The mucociliary escalator sweeps mucus and trapped debris toward the pharynx, where it is swallowed and destroyed in the stomach.
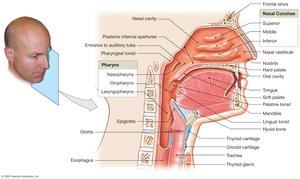
Structures of the Upper Respiratory System
The Nose and Nasal Cavity
Air enters through the nares (nostrils) into the nasal cavity, which is divided by the nasal septum. The hard palate forms the floor, and the soft palate lies posteriorly. Nasal conchae increase turbulence, warming and humidifying air. The nasal cavity is flushed by mucus and tears, which help trap debris and pathogens.
The Pharynx
The pharynx (throat) is a shared chamber for the respiratory and digestive systems. It is divided into three regions:
Nasopharynx: Posterior to nasal cavity; contains pharyngeal tonsil and auditory tube openings.
Oropharynx: Posterior to oral cavity; contains palatine tonsils.
Laryngopharynx: Posterior to larynx; leads to esophagus.
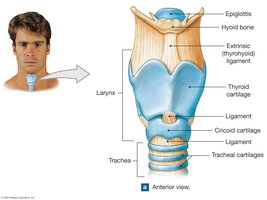
Structures of the Lower Respiratory System
The Larynx
The larynx (voice box) surrounds and protects the glottis. It is composed of nine cartilages, including the epiglottis (prevents food entry during swallowing), thyroid cartilage (Adam's apple), and cricoid cartilage. The larynx contains the vocal cords for sound production.
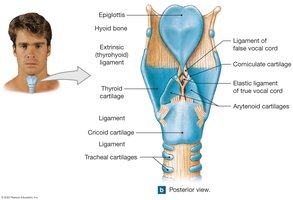
Vocal Cords and Sound Production
False vocal cords: Upper, inelastic; protect true vocal cords.
True vocal cords: Lower, elastic; produce sound when air passes through.
Pitch is determined by the length, thickness, and tension of the vocal cords.
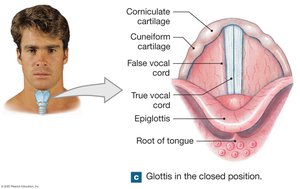
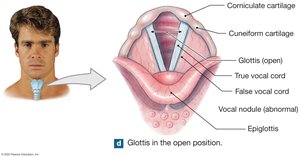
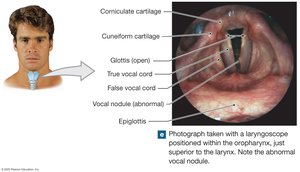
The Trachea and Bronchi
The trachea (windpipe) is a flexible tube supported by C-shaped cartilages, which keep the airway open and allow food to pass through the esophagus. The trachea branches into the right and left main bronchi, which enter the lungs.
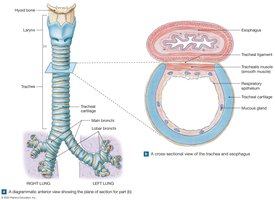
The Bronchial Tree and Bronchioles
The bronchial tree consists of branching airways: main bronchi, lobar bronchi (2 left, 3 right), segmental bronchi, and bronchioles. As airways branch, their diameter decreases and cartilage is replaced by smooth muscle. Bronchioles control airflow via muscle contraction (bronchodilation and bronchoconstriction).
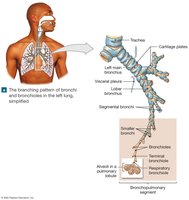
Gas Exchange Structures
Terminal and Respiratory Bronchioles
Terminal bronchioles are the smallest conducting airways, each supplying a pulmonary lobule. They branch into respiratory bronchioles, which may participate in gas exchange and lead to alveolar ducts.
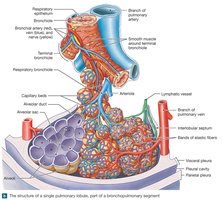
Alveolar Ducts and Alveoli
Alveolar ducts end in alveolar sacs composed of many alveoli. Each lung contains about 150 million alveoli, providing a large surface area (~140 m2) for rapid gas diffusion.
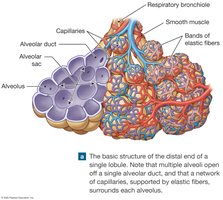
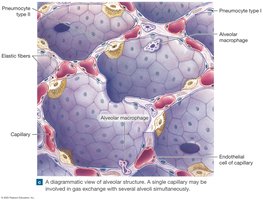
Alveolar Cells and Surfactant
Pneumocytes type I: Thin squamous cells for gas exchange.
Pneumocytes type II: Produce surfactant, reducing surface tension and preventing alveolar collapse.
Alveolar macrophages: Phagocytize debris and pathogens.
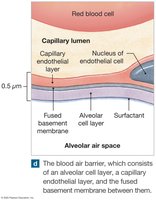
Lung Anatomy and Pleural Cavities
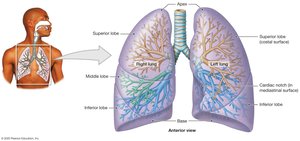
Lobes and Surfaces of the Lungs
Right lung: Three lobes (superior, middle, inferior)
Left lung: Two lobes (superior, inferior), with a cardiac notch for the heart
Apex: Top of the lung; base: rests on diaphragm
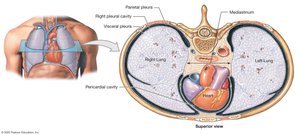
Pleural Cavities and Membranes
Each lung is surrounded by a pleural cavity lined by serous membranes:
Visceral pleura: Covers lung surface
Parietal pleura: Lines thoracic wall and diaphragm
Pleural fluid: Reduces friction between layers
Mechanics of Breathing (Pulmonary Ventilation)
Pressure and Volume Changes
Air moves into and out of the lungs due to pressure gradients created by changes in thoracic volume. When lung volume increases, pressure decreases and air flows in (inhalation). When volume decreases, pressure increases and air flows out (exhalation).
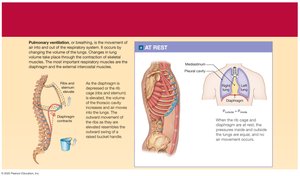
Muscles of Respiration
Diaphragm: Main muscle of inspiration; contraction increases thoracic volume.
External intercostals: Assist in elevating the rib cage.
Accessory muscles: Used during forced breathing.
Lung Compliance
Compliance is the ease with which the lungs expand. High compliance means lungs expand easily; low compliance requires more effort. Factors affecting compliance include alveolar damage, surfactant levels, and thoracic mobility.
Lung Volumes and Capacities
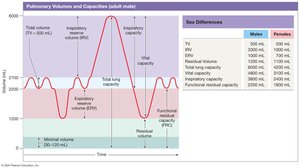
Definitions and Values
Tidal volume (TV): Air moved in or out during quiet breathing (~500 mL)
Expiratory reserve volume (ERV): Air expelled after normal exhalation
Inspiratory reserve volume (IRV): Air inhaled above tidal volume
Vital capacity:
Residual volume: Air remaining after maximal exhalation
Anatomic dead space: Air in conducting passages not involved in gas exchange (~150 mL)
Summary Table: Lung Volumes and Capacities
Volume/Capacity | Definition | Typical Value (Male) | Typical Value (Female) |
|---|---|---|---|
Tidal Volume (TV) | Air moved per breath at rest | 500 mL | 500 mL |
Expiratory Reserve Volume (ERV) | Max air exhaled after normal exhalation | 1000 mL | 700 mL |
Inspiratory Reserve Volume (IRV) | Max air inhaled after normal inhalation | 3300 mL | 1900 mL |
Residual Volume | Air remaining after maximal exhalation | 1200 mL | 1100 mL |
Vital Capacity | TV + IRV + ERV | 4800 mL | 3100 mL |
Key Terms and Concepts
External respiration: Exchange of gases between lungs and blood
Internal respiration: Exchange of gases between blood and tissues
Hypoxia: Low tissue oxygen
Anoxia: Absence of oxygen, leading to cell death
Clinical Notes
Pneumothorax: Air in pleural cavity causing lung collapse
Pulmonary embolism: Blockage of pulmonary artery branch
Respiratory distress syndrome: Lack of surfactant, leading to alveolar collapse
