 Back
BackChapter 17: Blood – Structure, Function, and Disorders
Study Guide - Smart Notes

Blood: The Internal Transport System
Overview and Learning Goals
Blood is a specialized fluid tissue essential for maintaining homeostasis and transporting substances throughout the body. This chapter explores the composition, functions, formation, and disorders of blood, as well as its role in clinical diagnostics.
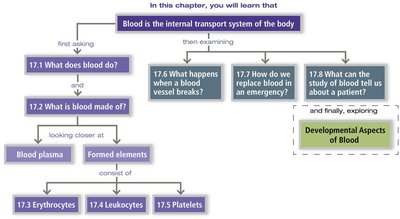
Functions of Blood
Distribution, Regulation, and Protection
Distribution: Blood transports oxygen, nutrients, metabolic wastes, and hormones.
Regulation: Maintains body temperature, pH balance, and fluid volume.
Protection: Prevents blood loss (clotting) and infection (immune response).
Composition of Blood
Physical Characteristics and Components
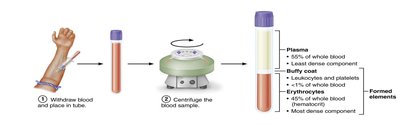
Blood consists of plasma (liquid matrix) and formed elements (cells and cell fragments). The hematocrit measures the percentage of red blood cells (RBCs) in total blood volume.
Plasma: ~90% water, contains proteins (albumin, globulins, clotting factors), nutrients, electrolytes, gases, and hormones.
Formed Elements: Erythrocytes (RBCs), Leukocytes (WBCs), Thrombocytes (Platelets).
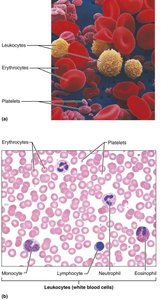
Formed Elements of Blood
Types and Characteristics
Formed elements are the cellular components of blood, each with distinct functions and lifespans.
Erythrocytes: Red blood cells, most numerous, responsible for oxygen transport.
Leukocytes: White blood cells, involved in immune defense.
Platelets: Cell fragments essential for blood clotting.
Erythrocytes (Red Blood Cells)
Structure and Function
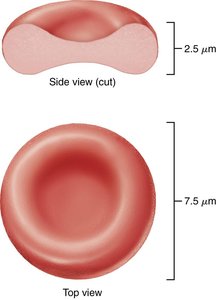
Erythrocytes are biconcave, anucleate cells optimized for gas transport. Their shape increases surface area for efficient oxygen exchange.
Biconcave Shape: Enhances flexibility and gas exchange.
Hemoglobin: Protein responsible for binding and transporting oxygen.
Spectrin: Membrane protein providing structural flexibility.
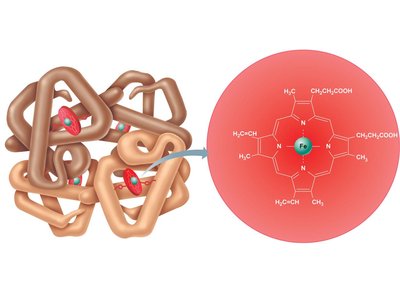
Hemoglobin Structure
Hemoglobin consists of four globin chains (two alpha, two beta) and four heme groups, each containing iron that binds oxygen.
Oxyhemoglobin: Hemoglobin bound to oxygen.
Deoxyhemoglobin: Hemoglobin after oxygen release.
Carbaminohemoglobin: Hemoglobin bound to carbon dioxide.
Production and Life Cycle of Blood Cells
Hematopoiesis and Erythropoiesis
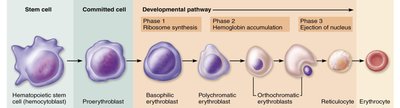
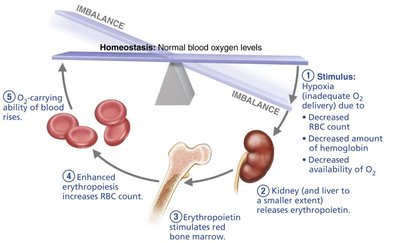
Blood cell formation occurs in red bone marrow from stem cells called hemocytoblasts. Erythropoiesis is the process of RBC production, regulated by erythropoietin (EPO).
Developmental Pathway: Hemocytoblast → Proerythroblast → Erythroblast → Reticulocyte → Erythrocyte
Regulation: EPO released in response to hypoxia stimulates RBC production.
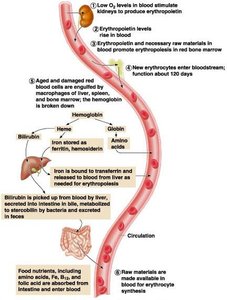
Life Cycle and Fate of Erythrocytes
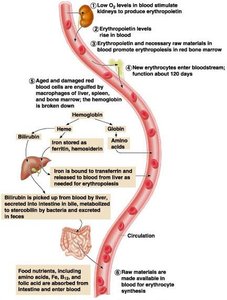
RBCs have a lifespan of 100–120 days. Old cells are removed by macrophages, and their components are recycled.
Hemoglobin Breakdown: Heme is converted to bilirubin, excreted as bile; globin is broken down to amino acids.
Erythrocyte Disorders
Anemia and Polycythemia
Anemia is characterized by reduced oxygen-carrying capacity, while polycythemia involves excess RBCs, increasing blood viscosity.
Types of Anemia: Hemorrhagic, hemolytic, aplastic, iron-deficiency, pernicious, thalassemia, sickle-cell.
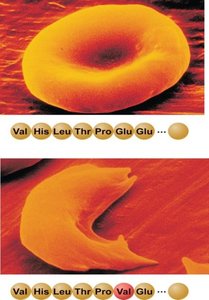
Sickle-Cell Anemia: Caused by a single amino acid substitution in hemoglobin, leading to sickle-shaped RBCs.
Leukocytes (White Blood Cells)
Classification and Functions
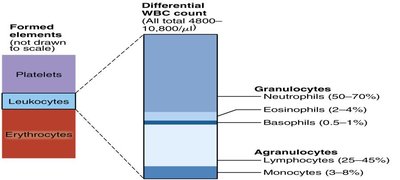
Leukocytes are nucleated cells involved in immune defense. They are classified as granulocytes or agranulocytes based on the presence of cytoplasmic granules.
Granulocytes: Neutrophils, eosinophils, basophils.
Agranulocytes: Lymphocytes, monocytes.
Granulocytes
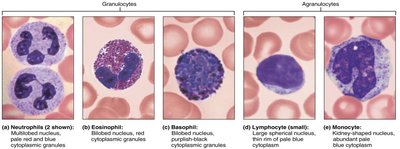
Neutrophils: Most abundant, phagocytize bacteria.
Eosinophils: Combat parasitic infections, modulate allergic responses.
Basophils: Release histamine and heparin, involved in inflammation.


Agranulocytes
Lymphocytes: Mount immune responses via direct cell attack or antibody production.
Monocytes: Develop into macrophages, phagocytize pathogens.


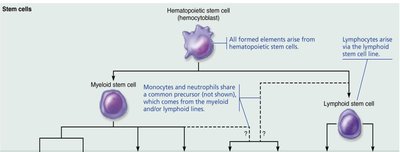
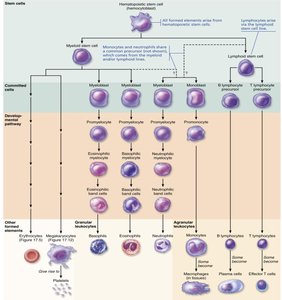
Leukopoiesis: Formation of Leukocytes
Stem Cell Differentiation
Leukocytes originate from hemocytoblasts, differentiating into myeloid or lymphoid stem cells, which further develop into specific WBC types.


Platelets (Thrombocytes)
Structure and Function
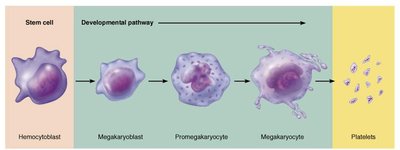
Platelets are cell fragments derived from megakaryocytes, essential for blood clotting and repair of blood vessels.
Developmental Pathway: Hemocytoblast → Megakaryoblast → Promegakaryocyte → Megakaryocyte → Platelets


Hemostasis: Prevention of Blood Loss
Phases of Hemostasis
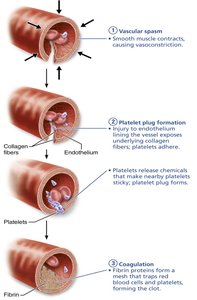
Hemostasis is the process of stopping bleeding, involving vascular spasm, platelet plug formation, and coagulation.
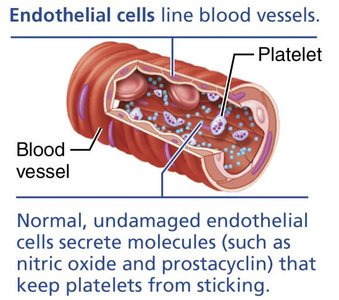
Vascular Spasm: Immediate vasoconstriction after vessel injury.
Platelet Plug Formation: Platelets adhere to exposed collagen and aggregate.
Coagulation: Blood is transformed from liquid to gel, forming a clot.
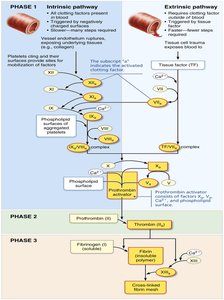
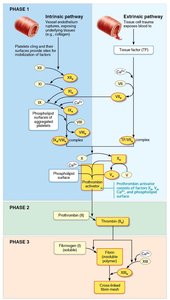
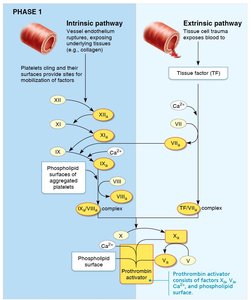
Coagulation Pathways
Coagulation involves intrinsic and extrinsic pathways, both leading to the formation of prothrombin activator, conversion of prothrombin to thrombin, and transformation of fibrinogen to fibrin.
Requirements: Calcium ions, vitamin K, clotting factors.


Blood Disorders
Thromboembolytic and Bleeding Disorders
Blood disorders include excessive clotting (thromboembolytic disorders) and bleeding disorders (thrombocytopenia, hemophilia).
Thrombocytopenia: Low platelet count, leading to spontaneous bleeding.
Hemophilia: Hereditary deficiency of clotting factors, resulting in prolonged bleeding.
Human Blood Groups
ABO and Rh Blood Groups
Blood groups are determined by antigens (agglutinogens) on RBC membranes. The ABO and Rh systems are clinically significant for transfusions.
ABO System: Based on presence of A and/or B antigens; plasma contains anti-A and/or anti-B antibodies.
Rh System: Presence of Rh antigen (D) determines Rh+ or Rh– status.
Transfusion Reactions and Hemolytic Disease of the Newborn
Transfusion reactions occur when mismatched blood is infused, leading to agglutination and hemolysis. Hemolytic disease of the newborn results from Rh incompatibility between mother and fetus.
Clinical Applications
Plasma Volume Expanders and Diagnostic Blood Tests
Plasma expanders are used to restore blood volume in emergencies. Laboratory blood tests provide valuable diagnostic information about health status.
Summary Table: Formed Elements of the Blood
Cell Type | Description | Cells/μL | Duration of Development (D) and Life Span (LS) | Function |
|---|---|---|---|---|
Erythrocyte | Biconcave, anucleate | 4-6 million | D: 7 days, LS: 100-120 days | Transport oxygen and carbon dioxide |
Neutrophil | Multilobed nucleus, pale granules | 3,000-7,000 | D: 14 days, LS: hours to days | Phagocytize bacteria |
Eosinophil | Bilobed nucleus, red granules | 100-400 | D: 14 days, LS: hours to days | Kill parasitic worms, modulate allergies |
Basophil | Bilobed nucleus, large purple granules | 20-50 | D: 1-7 days, LS: hours to days | Release histamine, contain heparin |
Lymphocyte | Spherical nucleus, pale blue cytoplasm | 1,500-3,000 | D: days to weeks, LS: hours to years | Mount immune response |
Monocyte | U/kidney-shaped nucleus, pale blue cytoplasm | 100-700 | D: 2-3 days, LS: months | Phagocytosis, develop into macrophages |
Platelet | Cytoplasmic fragments, stain deep purple | 150,000-400,000 | D: 4-5 days, LS: 5-10 days | Seal tears, blood clotting |
