 Back
BackChapter 19: Blood – Structure, Function, and Clinical Relevance
Study Guide - Smart Notes

Chapter 19: Blood
General Functions of Blood
Blood is a specialized connective tissue that performs vital functions necessary for maintaining homeostasis and supporting life. Its unique composition allows it to transport substances, regulate physiological parameters, and defend the body against threats.
Transport: Blood carries gases (O2, CO2), nutrients, hormones, and metabolic wastes throughout the body.
Regulation of pH and Ion Composition: Maintains acid-base balance and proper ion concentrations in interstitial fluid.
Restriction of Fluid Losses: Initiates clotting to prevent excessive blood loss at injury sites.
Defense: Contains cells and antibodies that protect against toxins and pathogens.
Stabilization of Body Temperature: Distributes heat generated by metabolic processes.

Composition of Blood
Blood consists of two main components: plasma (the liquid matrix) and formed elements (cells and cell fragments).
Plasma: Makes up about 55% of blood volume and is composed of:
92% water
7% proteins (albumin, globulins, fibrinogen)
1% other solutes (electrolytes, nutrients, wastes)
Formed Elements: Include red blood cells (erythrocytes), white blood cells (leukocytes), and platelets (thrombocytes).

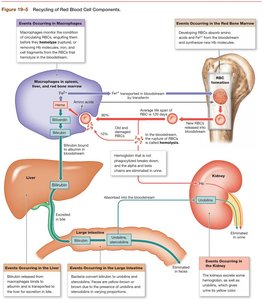
Formed Elements of Blood
The formed elements are the cellular components of blood, each with specialized functions:
Platelets: Small cell fragments essential for blood clotting.
White Blood Cells (Leukocytes): Defend the body against infection and foreign substances. Types include neutrophils, eosinophils, basophils, lymphocytes, and monocytes.
Red Blood Cells (Erythrocytes): Specialized for oxygen transport.
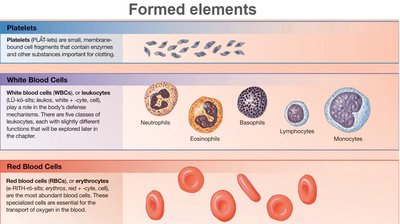
Red Blood Cells: Structure and Function
Red blood cells (RBCs) are uniquely adapted for their role in oxygen transport:
Biconcave Shape: Increases surface area-to-volume ratio, facilitating efficient gas exchange and allowing RBCs to form stacks (rouleaux) for smooth flow through capillaries.
Lack of Nucleus and Organelles: Maximizes space for hemoglobin, the oxygen-carrying protein.
Flexible Plasma Membrane: Enables RBCs to deform as they pass through narrow capillaries.
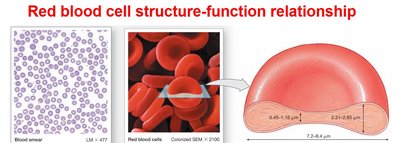

Hemoglobin Structure and Function
Hemoglobin is the protein responsible for oxygen transport in RBCs. Each molecule consists of four polypeptide chains (two alpha, two beta), each with a heme group containing an iron atom that binds oxygen.
Oxygen Binding: Each hemoglobin molecule can carry up to four oxygen molecules.
Role in CO2 Transport: Hemoglobin also assists in transporting carbon dioxide from tissues to the lungs.
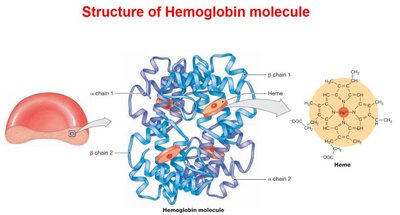
Red Blood Cell Recycling
RBCs have a lifespan of about 120 days. Old or damaged RBCs are removed from circulation and their components are recycled:
Hemoglobin Breakdown: Macrophages in the liver, spleen, and bone marrow phagocytize RBCs, breaking hemoglobin into heme and globin.
Iron Recycling: Iron from heme is stored or transported for reuse.
Bilirubin Formation: Non-iron portion of heme is converted to bilirubin, which is excreted in bile.
Blood Types and Transfusion Compatibility
Blood types are determined by the presence or absence of specific antigens on RBC surfaces. The two main systems are ABO and Rh.
ABO System
Type A: A antigen on RBCs, anti-B antibodies in plasma.
Type B: B antigen on RBCs, anti-A antibodies in plasma.
Type AB: Both A and B antigens, no anti-A or anti-B antibodies (universal recipient).
Type O: No A or B antigens, both anti-A and anti-B antibodies (universal donor).
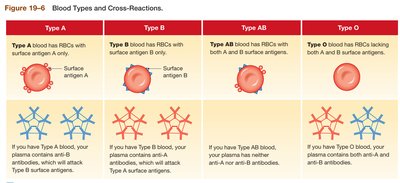
Blood Group | Antigens on RBCs | Antibodies in Plasma | Key Transfusion Rule |
|---|---|---|---|
A | A antigen | Anti-B | Can receive A or O |
B | B antigen | Anti-A | Can receive B or O |
AB | A and B antigens | Neither anti-A nor anti-B | Universal Recipient |
O | Neither A nor B | Anti-A and Anti-B | Universal Donor |

Rh System
Rh Positive (Rh+): D antigen present; no anti-Rh antibodies naturally.
Rh Negative (Rh−): D antigen absent; can develop anti-Rh antibodies after exposure to Rh+ blood.
Rh Type | RhD Antigen on RBCs | Antibodies in Plasma | Key Transfusion Rule |
|---|---|---|---|
Rh-Positive (Rh+) | Present | None | Can receive Rh+ or Rh− |
Rh-Negative (Rh−) | Absent | None naturally; can form after exposure | Should only receive Rh− |

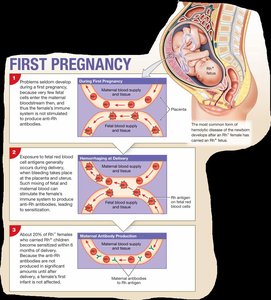
Hemolytic Disease of the Newborn (HDN)
HDN occurs when an Rh− mother carries an Rh+ fetus. Maternal exposure to fetal Rh+ blood can lead to the formation of anti-Rh antibodies, which may attack fetal RBCs in subsequent pregnancies.
Prevention: Administration of Rh-immune globulin (RhoGAM) to the mother prevents antibody formation.

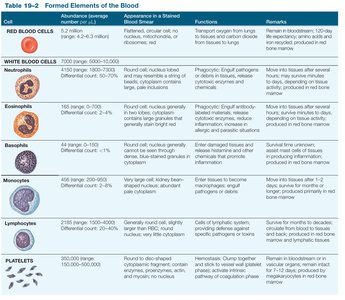
Formed Elements: Detailed Table
The following table summarizes the main characteristics of the formed elements of blood:
Cell | Abundance | Appearance | Functions | Remarks |
|---|---|---|---|---|
Red Blood Cells | ~4.2–6.1 million/μL | Biconcave, no nucleus | Transport O2 and CO2 | 120-day lifespan |
Neutrophils | 4150/μL | Multi-lobed nucleus | Phagocytosis of bacteria | Most abundant WBC |
Eosinophils | 165/μL | Bilobed nucleus | Attack parasites, modulate allergies | Increase in parasitic infections |
Basophils | 44/μL | Large granules | Release histamine, mediate inflammation | Rare |
Monocytes | 456/μL | Large, kidney-shaped nucleus | Phagocytosis, become macrophages | Largest WBC |
Lymphocytes | 2185/μL | Large, round nucleus | Adaptive immunity (T, B, NK cells) | Second most abundant WBC |
Platelets | 350,000/μL | Small fragments | Clotting | Remain in bloodstream ~10 days |
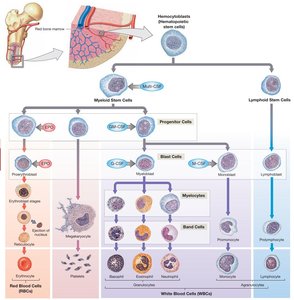
Hematopoiesis
Hematopoiesis is the process of blood cell formation, occurring primarily in the red bone marrow. All blood cells originate from hematopoietic stem cells (HSCs), which differentiate into myeloid and lymphoid lineages.
Myeloid Stem Cells: Give rise to RBCs, platelets, and most WBCs.
Lymphoid Stem Cells: Give rise to lymphocytes (T cells, B cells, NK cells).
Hemostasis
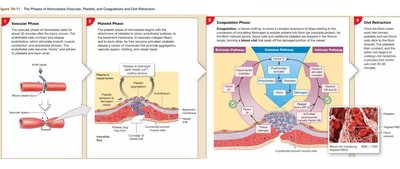
Hemostasis is the process that stops bleeding and involves three main phases:
Vascular Phase: Blood vessel constriction reduces blood flow.
Platelet Phase: Platelets adhere to the injury site and form a temporary plug.
Coagulation Phase: A cascade of reactions leads to the formation of a stable fibrin clot.
Additional info: These notes provide a comprehensive overview of blood structure, function, and clinical relevance, suitable for ANP college students preparing for exams.
