 Back
BackChapter 19: The Cardiovascular System – Blood Vessels
Study Guide - Smart Notes

Blood Vessel Anatomy
Structure and Types of Blood Vessels
Blood vessels are a series of enclosed structures that convey blood to and from the heart, forming a closed circulatory system. There are three main types of blood vessels: arteries (carry blood away from the heart), capillaries (site of exchange), and veins (carry blood toward the heart). Each vessel type has a unique structure suited to its function.
Arteries: Thick-walled, high-pressure vessels, mostly carry oxygenated blood.
Veins: Thinner-walled, low-pressure vessels, mostly carry deoxygenated blood.
Capillaries: Smallest vessels, one cell layer thick, site of exchange between blood and tissues.
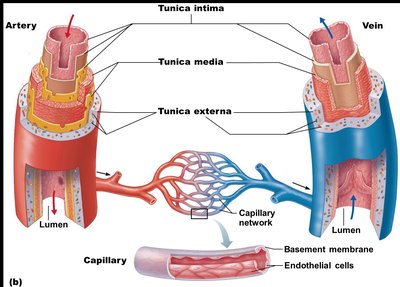
Layers of Blood Vessel Walls
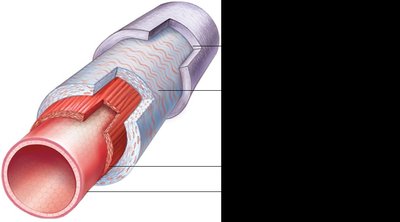
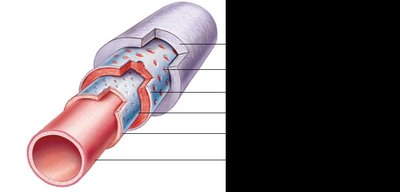
Most blood vessel walls (except capillaries) are composed of three layers, called tunics:
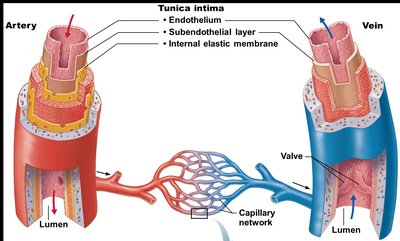
Tunica intima: Innermost layer, direct contact with blood, composed of endothelium (simple squamous epithelium), subendothelial layer, and internal elastic membrane (not present in veins).
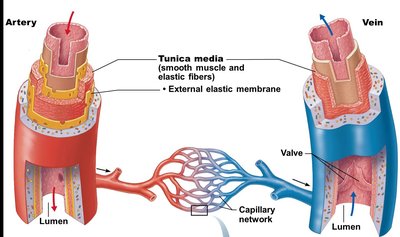
Tunica media: Middle layer, mostly smooth muscle and elastic fibers, responsible for vasoconstriction and vasodilation, contains external elastic membrane (not present in veins).
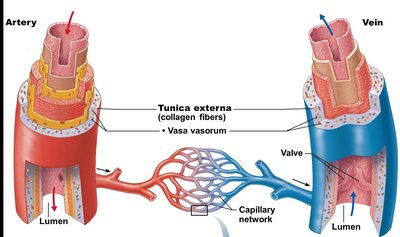
Tunica externa (adventitia): Outermost layer, primarily loose collagen fibers, contains vasa vasorum (tiny blood vessels that supply the tunica externa in large vessels).
Capillaries are composed only of endothelium (single layer of squamous cells) and a small amount of basal lamina.
Types of Arteries
Elastic, Muscular, and Arterioles
Arteries are classified based on size and function:
Elastic arteries: Largest diameter, high pressure, thick walls, low resistance, conduct blood to smaller arteries (e.g., aorta and major branches).
Muscular arteries: Distributing arteries, deliver blood to body organs, more smooth muscle, less elastic tissue, account for most vasoconstrictive activities.
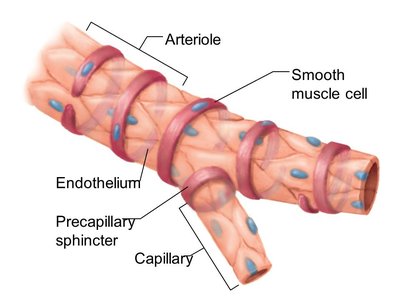
Arterioles: Smallest arteries, also called resistance arteries, diameters change due to smooth muscle constriction, control distribution of blood to capillary beds.
Capillaries: Exchange Vessels
Structure and Function
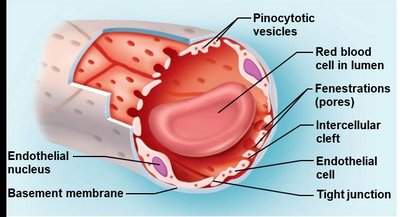
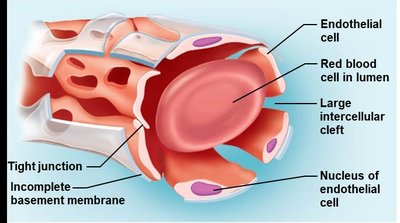
Capillaries are the smallest blood vessels, with a diameter similar to that of a red blood cell. Their walls are one cell layer thick, composed of endothelium. Pericytes are stem cells found on some capillaries, helping generate new vessels, stabilize capillary walls, and control permeability.
Types of Capillaries
Continuous capillaries: Most common, tightly joined endothelial cells, least permeable, associated with pericytes, transport occurs via transcytosis.
Fenestrated capillaries: Have fenestrations (pores), small intercellular clefts, increased permeability, found in kidneys, small intestine, and endocrine organs.
Sinusoid capillaries: Most permeable, large fenestrations and intercellular clefts, allow passage of large molecules and cells, found in liver, bone marrow, and spleen.
Capillary Beds
Organization and Blood Flow
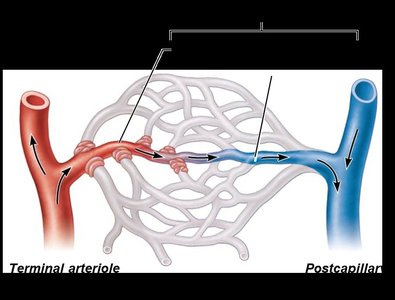
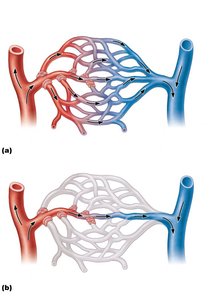
Capillary beds are networks of capillaries between arterioles and venules. Blood flow is regulated and can be directed through two types of vessels:
Vascular shunt: Direct path between terminal arteriole and postcapillary venule, composed of metarteriole (artery side) and thoroughfare channel (venous side).
True capillaries: Branch off metarterioles, mediate exchange between blood and tissues, blood flow regulated by precapillary sphincters.
Veins: Blood Reservoirs
Structure and Function
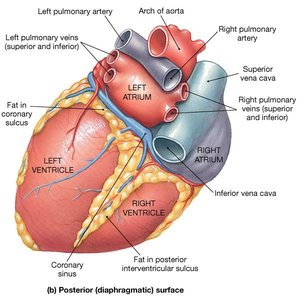
Veins carry blood toward the heart, mostly deoxygenated except for pulmonary veins. Small veins (venules) drain into larger veins. Veins contain the same three tunics as arteries, but are thinner and function as capacitance vessels and blood reservoirs.
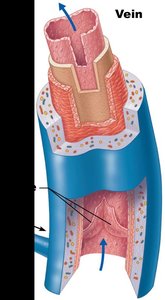
Venous valves: Prevent backflow, especially in lower limbs, movement of blood promoted by skeletal muscle contraction.
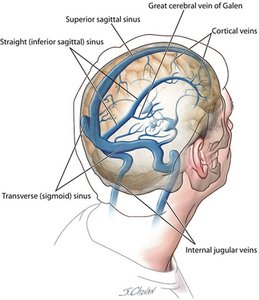
Venous sinuses: Specialized veins without tunics, supported by surrounding tissue (e.g., dural venous sinus, coronary sinus).
Anastomoses: Interconnections Between Blood Vessels
Types and Functions
Anastomoses are direct connections between blood vessels, providing alternate routes of blood flow to an area. Types include:
Arterial anastomoses: Joins two arteries.
Venous anastomoses: Joins two veins.
Arteriovenous anastomoses: Joins an artery and vein.
Physiology of Circulation
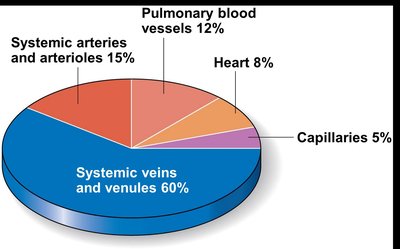
Blood Flow, Pressure, and Resistance
Blood must circulate to sustain life. Three main factors affect circulation:
Blood flow: Volume of blood flowing through a vessel per unit time (ml/min), equivalent to cardiac output.
Blood pressure: Force per unit area exerted on vessel wall by blood, measured in mmHg, highest in arteries near the heart.
Resistance: Forces that oppose blood flow, mainly peripheral resistance (systemic circulation), affected by blood viscosity, vessel length, and vessel diameter.
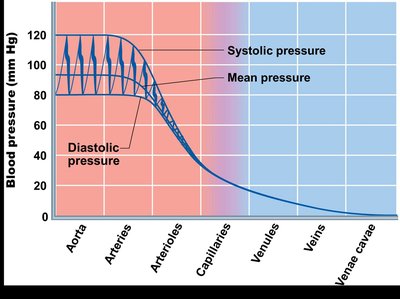
Blood Flow Equation
Blood flow depends on blood pressure and resistance:
Blood flow (F) is directly proportional to pressure difference (ΔP).
Blood flow is inversely proportional to resistance (R).
Equation:
Regulation of Blood Pressure
Short-Term and Long-Term Controls
Blood pressure is regulated by both short-term and long-term mechanisms:
Short-term regulation: Neural (cardiovascular center, baroreceptor and chemoreceptor reflexes, higher brain centers) and hormonal controls (epinephrine/norepinephrine, angiotensin II, ANP, ADH).
Long-term regulation: Renal mechanisms (direct and indirect), primarily affecting blood volume.
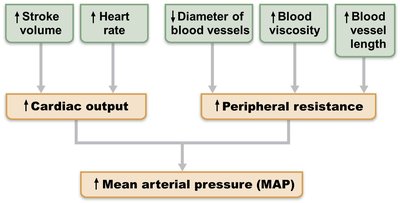
Blood Pressure Relationships
Blood pressure is directly proportional to cardiac output (CO), peripheral resistance (R), stroke volume (SV), and heart rate (HR):
Short-Term Regulation: Neural Controls
Cardiovascular center: Located in medulla oblongata, regulates HR, force of contraction, and vessel diameter.
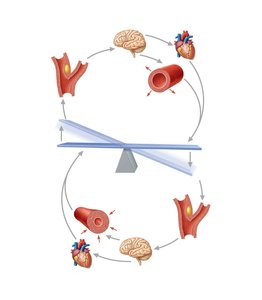
Baroreceptor reflexes: Detect changes in blood pressure, located in aorta and large arteries. High BP causes vasodilation and decreased CO; low BP causes vasoconstriction and increased CO.
Chemoreceptor reflexes: Detect changes in CO2, O2, and pH, stimulate increased BP when blood is not adequately reaching tissues.
Higher brain centers: Hypothalamus and cerebral cortex can modify BP by affecting reflex centers in medulla oblongata.
Short-Term Regulation: Hormonal Controls
Epinephrine/Norepinephrine: Increase CO and promote vasoconstriction.
Angiotensin II: Stimulates vasoconstriction, ADH and aldosterone secretion, increases BV and BP.
Atrial natriuretic peptide (ANP): Inhibits aldosterone, increases Na+ and H2O excretion, decreases BV and BP.
Antidiuretic hormone (ADH): Promotes water reabsorption, increases BV and BP.
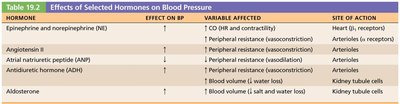
Hormone | Effect on BP | Variable Affected | Site of Action |
|---|---|---|---|
Epinephrine/Norepinephrine | ↑ | CO (HR and contractility), Peripheral resistance (vasoconstriction) | Heart (β receptors), Arterioles (α receptors) |
Angiotensin II | ↑ | Peripheral resistance (vasoconstriction) | Arterioles |
ANP | ↓ | Peripheral resistance (vasodilation) | Arterioles |
ADH | ↑ | Peripheral resistance (vasoconstriction), Blood volume (↑ water reabsorption) | Arterioles, Kidney tubule cells |
Aldosterone | ↑ | Blood volume (↑ salt and water reabsorption) | Kidney tubule cells |
Long-Term Regulation: Renal Mechanisms
Direct mechanism: Alters blood volume independent of hormones; high BP increases fluid loss, low BP increases fluid retention.
Indirect mechanism: Renin-angiotensin-aldosterone system; low BP triggers renin release, leading to angiotensin II production, which increases BV and BP through multiple effects.
Capillary Exchange
Mechanisms of Exchange
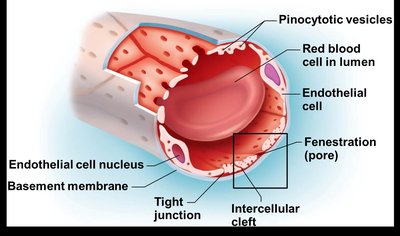
Capillary exchange is the movement of substances between plasma and interstitial fluid. The velocity of blood flow affects exchange efficiency; slow flow allows for effective diffusion.
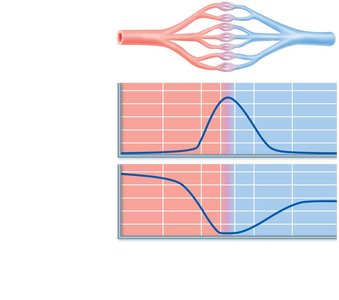
Diffusion: Main mechanism, solutes move down concentration gradients.
Routes: Direct diffusion through endothelial membranes (lipid-soluble), passage between intercellular clefts (water-soluble), through fenestrations (larger water-soluble), and active transport via pinocytotic vesicles/caveolae (large particles).
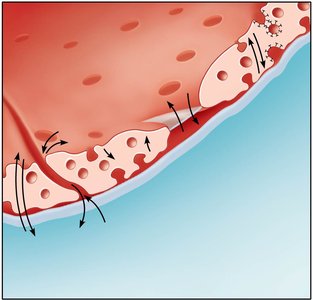
Bulk Flow
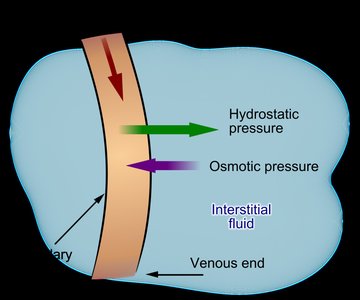
Bulk flow is the movement of fluid between capillaries and tissues, driven by hydrostatic and osmotic pressures. Most fluid returns to blood at the venous end; the remainder is returned via the lymphatic system.
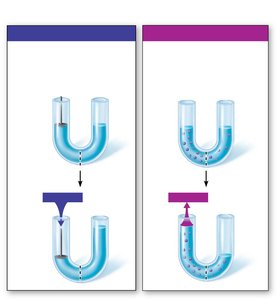
Hydrostatic pressure (HP): Force exerted by fluid pressing against a wall, pushes fluid out of capillaries.
Colloid osmotic pressure (OP): Force opposing HP, created by nondiffusible solutes (plasma proteins), pulls fluid into capillaries.
Net Filtration Pressure (NFP)
The direction of fluid flow is determined by net filtration pressure:
At the arterial end: net movement out of capillary (filtration).
At the venous end: net movement into capillary (reabsorption).

Summary: Blood vessels are essential for transporting blood throughout the body, with specialized structures and functions for arteries, veins, and capillaries. Blood flow, pressure, and resistance are tightly regulated to ensure proper tissue perfusion and homeostasis. Capillary exchange and bulk flow are critical for nutrient and waste movement between blood and tissues.
