 Back
BackChapter 19: The Heart – Structure, Function, and Clinical Correlates
Study Guide - Smart Notes

The Heart: Anatomy and Circulation
Overview of Heart Function
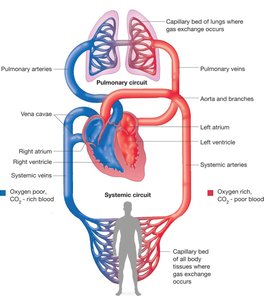
The heart is a muscular organ that acts as two coordinated pumps, propelling blood through the pulmonary and systemic circuits. Its primary function is to maintain continuous blood flow, delivering oxygen and nutrients to tissues and removing waste products.
Right side (Pump 1): Sends oxygen-poor blood to the lungs (pulmonary circuit).
Left side (Pump 2): Sends oxygen-rich blood to the body’s tissues (systemic circuit).
Location: Largest organ of the mediastinum, between the lungs, with the apex pointing left of the midline and the base as the broad posterior surface.
Weight: Typically 250–350 grams in a healthy adult.
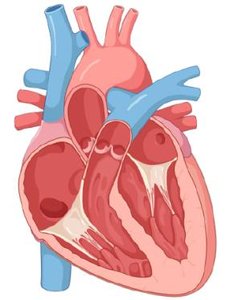
Gross Anatomy of the Heart
External and Internal Features
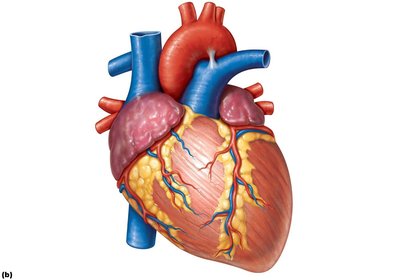
The heart is enclosed within the thoracic cavity, protected by the lungs and diaphragm. Its external surface is marked by major vessels and grooves that house coronary arteries and veins.
Major vessels: Aorta, pulmonary trunk, superior and inferior vena cava, pulmonary veins.
Surface features: Coronary sulcus, anterior and posterior interventricular sulci.
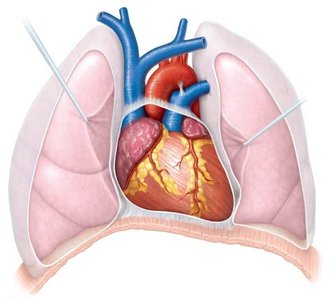
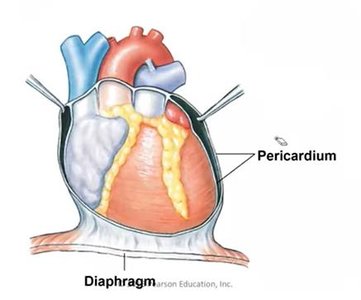
Heart Wall and Pericardium
Layers of the Heart Wall
The heart wall consists of three layers, each with distinct structure and function:
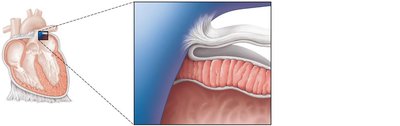
Epicardium: The visceral layer of the serous pericardium; outermost layer.
Myocardium: Thick middle layer composed of cardiac muscle tissue; responsible for contraction.
Endocardium: Innermost layer; a sheet of simple squamous epithelium lining the heart chambers and valves.
Cardiac Muscle Tissue
Structure and Function
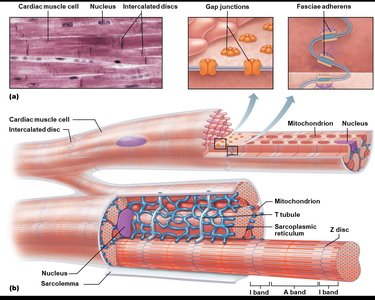
Cardiac muscle tissue forms the myocardium and is specialized for continuous, rhythmic contraction. It shares some features with skeletal muscle but has unique adaptations for heart function.
Striated: Contains sarcomeres like skeletal muscle.
Cells: Short, branching, typically with one or two nuclei.
Intercalated discs: Specialized junctions (desmosomes and gap junctions) that allow rapid electrical and mechanical coupling between cells.
Contraction mechanism: Sliding filament mechanism, similar to skeletal muscle.

Organization of Cardiac Muscle
Muscle Bundles and Terminology
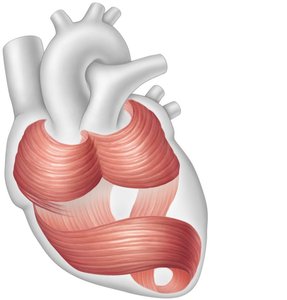
Cardiac muscle fibers are organized into bundles that spiral around the heart, facilitating efficient contraction and blood ejection.
Cardiac muscle fiber: A bundle of many fused cells, unlike the single-cell structure of skeletal muscle fibers.
Bundles: Spiral arrangement aids in wringing action during contraction.
Types of Cardiac Muscle Cells
Contractile vs. Autorhythmic Cells
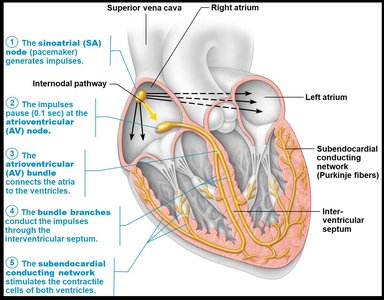
The heart contains two main types of cardiac muscle cells, each with distinct roles in cardiac function:
Contractile cells (99%): Generate force to pump blood.
Autorhythmic (conducting) cells: Initiate and distribute electrical impulses (e.g., SA node, AV node, conduction fibers).
Innervation of the Heart
Autonomic Regulation
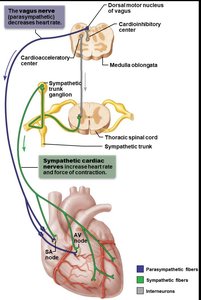
The heart is innervated by both sympathetic and parasympathetic fibers, which modulate heart rate and force of contraction:
Parasympathetic fibers: Branches of the vagus nerve; decrease heart rate; primarily affect SA node, AV node, and coronary arteries.
Sympathetic fibers: Originate from cervical and upper thoracic chain ganglia; increase heart rate and contractility; innervate SA node, AV node, coronary arteries, and cardiac muscle.
Chambers of the Heart
Atria and Ventricles
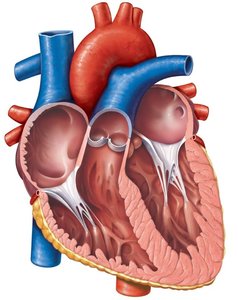
The heart has four chambers: two atria (superior) and two ventricles (inferior). Internal septa divide the right and left sides.
Right atrium: Receives deoxygenated blood from the body via the superior and inferior vena cava.
Left atrium: Receives oxygenated blood from the lungs via pulmonary veins.
Right ventricle: Pumps blood into the pulmonary circuit.
Left ventricle: Pumps blood into the systemic circuit; forms the apex of the heart.
Septa: Interatrial and interventricular septa separate the chambers.
Heart Valves
Structure and Function
Heart valves ensure unidirectional blood flow through the heart. They open and close in response to pressure changes during the cardiac cycle.
Atrioventricular (AV) valves: Between atria and ventricles; right AV (tricuspid), left AV (bicuspid/mitral).
Semilunar valves: At the junction of ventricles and great arteries; pulmonary and aortic valves.
Valve structure: Composed of endocardium with a connective tissue core; supported by chordae tendineae and papillary muscles (AV valves).
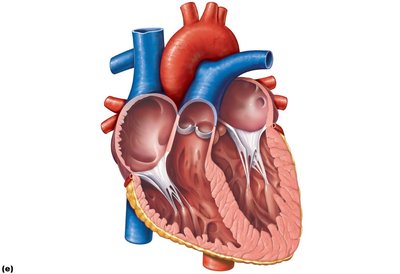
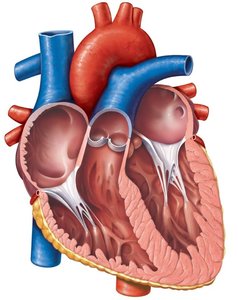
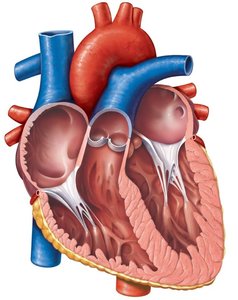
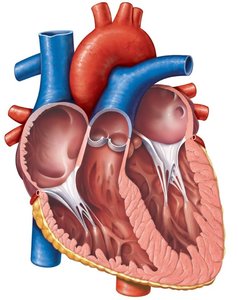
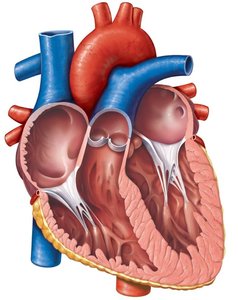
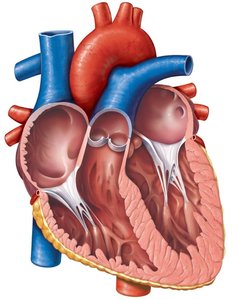
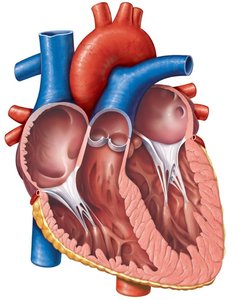
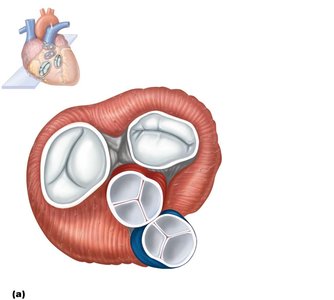
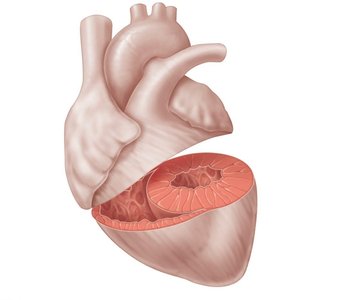
Valve Operation During Cardiac Cycle
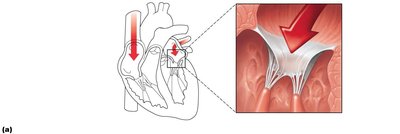
Valves open and close in response to pressure differences between chambers:
AV valves open: Atrial pressure > ventricular pressure; blood flows into ventricles.
AV valves close: Ventricular pressure > atrial pressure; prevents backflow into atria.
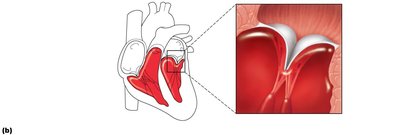
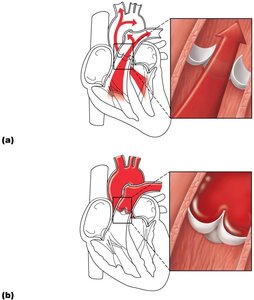
Semilunar valves open: Ventricular pressure > arterial pressure; blood ejected into arteries.
Semilunar valves close: Arterial pressure > ventricular pressure; prevents backflow into ventricles.
Heart Sounds
Origin of Heart Sounds
The characteristic "lub-dup" sounds of the heart are produced by the closing of the valves:
First sound ("lub"): Closure of AV valves at the start of ventricular systole.
Second sound ("dup"): Closure of semilunar valves at the start of ventricular diastole.
Coronary Circulation
Blood Supply to the Heart
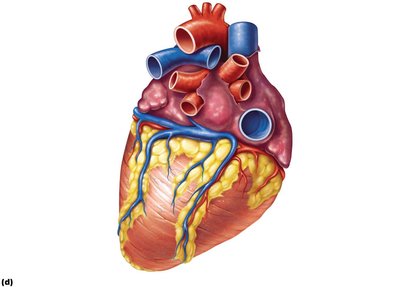
The heart muscle (myocardium) receives its own blood supply via the coronary arteries and is drained by cardiac veins.
Coronary arteries: Right and left coronary arteries arise from the base of the aorta; major branches include the anterior and posterior interventricular arteries and the circumflex artery.
Coronary veins: Great, middle, and small cardiac veins drain into the coronary sinus, which returns blood to the right atrium.
Anastomoses: Junctions between vessels provide collateral circulation.
Clinical Correlates: Disorders of the Heart
Coronary Artery Disease and Heart Failure
Coronary artery disease: Atherosclerosis (fatty deposits), angina pectoris (chest pain), myocardial infarction (heart attack), silent ischemia (no pain or warning).
Heart failure: Progressive weakening of the heart, inability to meet the body's oxygen demands.
Congestive heart failure (CHF): Heart enlarges, pumping efficiency declines.
Disorders of the Conduction System
Arrhythmias: Variations from normal heart rhythm.
Ventricular fibrillation: Rapid, random electrical impulses in ventricles; common cause of cardiac arrest.
Atrial fibrillation: Impulses circle within atrial myocardium, stimulating AV node; increases risk of clots and stroke.
Summary Table: Heart Valves and Blood Flow
Valve | Location | Function |
|---|---|---|
Tricuspid (Right AV) | Between right atrium and right ventricle | Prevents backflow into right atrium |
Pulmonary Semilunar | Between right ventricle and pulmonary trunk | Prevents backflow into right ventricle |
Bicuspid/Mitral (Left AV) | Between left atrium and left ventricle | Prevents backflow into left atrium |
Aortic Semilunar | Between left ventricle and aorta | Prevents backflow into left ventricle |
Key Equations
Cardiac Output (CO): The volume of blood pumped by each ventricle per minute. Where is heart rate (beats/min) and is stroke volume (mL/beat).
Additional info: The above notes integrate foundational knowledge of heart anatomy, physiology, and clinical relevance, suitable for ANP college students preparing for exams.
