 Back
BackChapter 27: The Male Reproductive System – Structure, Development, and Function
Study Guide - Smart Notes

Male Reproductive System Overview
Introduction
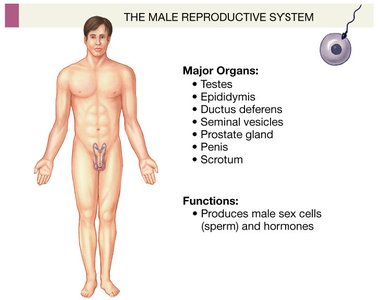
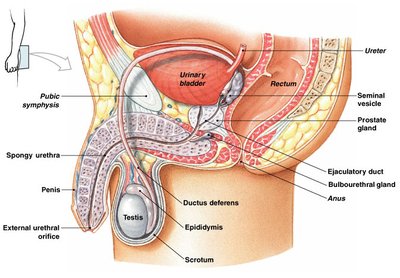
The male reproductive system is responsible for the production, maturation, and delivery of male gametes (sperm), as well as the secretion of male sex hormones. It consists of primary sex organs (gonads), secondary sex organs (ducts and genitalia), and accessory glands.
Primary Sex Organs (Gonads): Testes
Secondary Sex Organs: Internal duct system and external genitalia (scrotum, penis)
Accessory Glands: Seminal vesicles, prostate gland, bulbourethral glands
Embryonic Development of the Male Reproductive System
Genotypic and Phenotypic Sex Determination
Sex determination in humans is governed by the combination of sex chromosomes inherited at fertilization. The presence or absence of the SRY gene on the Y chromosome triggers the development of male or female reproductive structures.
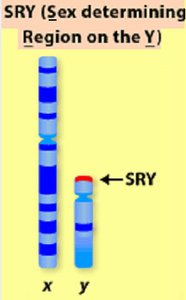
Genotypic Sex: Determined by chromosomes (XX = female, XY = male)
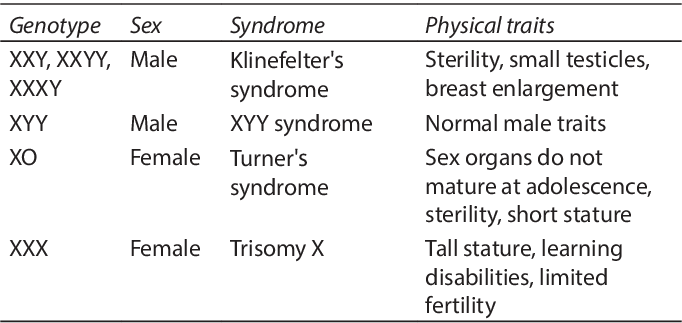
SRY Region: The Sex-determining Region on the Y chromosome contains the TDF (Testis Determining Factor) gene, which initiates testis development.
Phenotypic Sex: The physical expression of sex, influenced by hormones such as testosterone and estrogen.
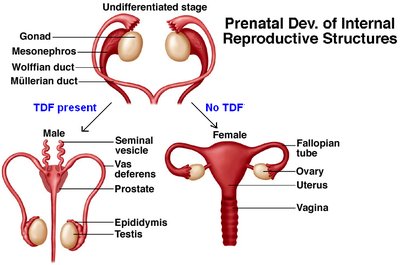
Development of Internal Reproductive Structures
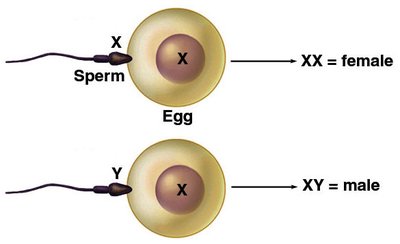
During early embryonic development (around week 6), both male and female embryos possess two sets of ducts: mesonephric (Wolffian) and paramesonephric (Müllerian) ducts. The presence of TDF and testosterone leads to the development of male structures, while their absence results in female structures.
Wolffian (Mesonephric) Ducts: Develop into male reproductive tract (epididymis, vas deferens, seminal vesicles)
Müllerian (Paramesonephric) Ducts: Develop into female reproductive tract (uterus, fallopian tubes, upper vagina) if no TDF/testosterone is present
Sex Chromosome Differences and Disorders of Sex Development (DSD)
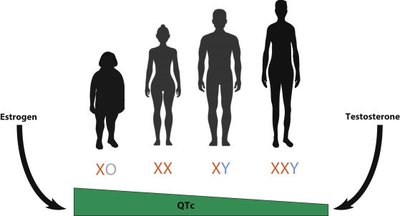
Variations in sex chromosomes can lead to differences in sexual development and associated syndromes.
Common Karyotypes: XX (female), XY (male), XO, XXY, XYY, XXX
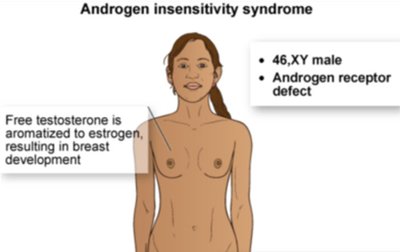
DSD: Conditions where there is a discrepancy between external and internal genitalia
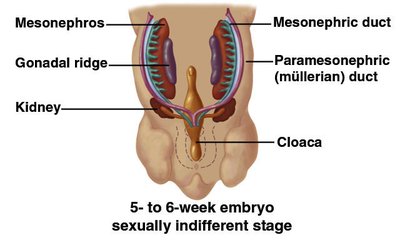
Genotype | Sex | Syndrome | Physical traits |
|---|---|---|---|
XXY, XXXY, XXXXY | Male | Klinefelter's syndrome | Sterility, small testicles, breast enlargement |
XYY | Male | XYY syndrome | Normal male traits |
XO | Female | Turner's syndrome | Sex organs do not mature at adolescence, sterility, short stature |
XXX | Female | Trisomy X | Tall stature, learning disabilities, limited fertility |
Male Gonads: Testes
Structure and Function
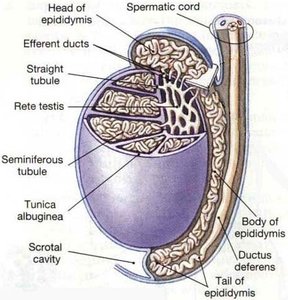
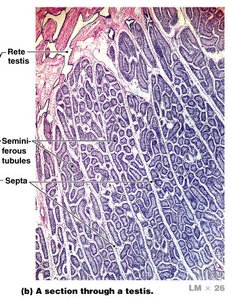
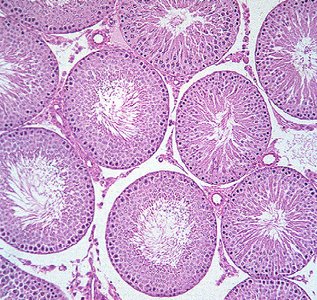
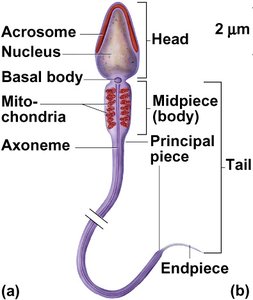
The testes are the primary male gonads responsible for producing sperm and testosterone. Each testis contains numerous seminiferous tubules, which are the site of spermatogenesis (sperm formation).
Seminiferous Tubules: Site of meiosis and spermatogenesis; about 800 tubules per testis
Sustentacular (Sertoli) Cells: Support and nourish developing sperm cells; form the blood-testis barrier
Interstitial (Leydig) Cells: Located between tubules; secrete testosterone
Sperm Formation (Spermatogenesis and Spermiogenesis)
Overview of Sperm Formation
Spermatogenesis is the process by which diploid germ cells undergo meiosis to produce haploid spermatozoa. Spermiogenesis refers to the morphological changes that transform spermatids into mature sperm cells.
Spermatogonium: Diploid stem cell that divides by mitosis
Primary Spermatocyte: Undergoes meiosis I to form secondary spermatocytes
Secondary Spermatocyte: Undergoes meiosis II to form spermatids
Spermatid: Undergoes spermiogenesis to become a mature spermatozoon
Chromosome Numbers:
Diploid (2n): 46 chromosomes (23 pairs)
Haploid (n): 23 chromosomes (single set)
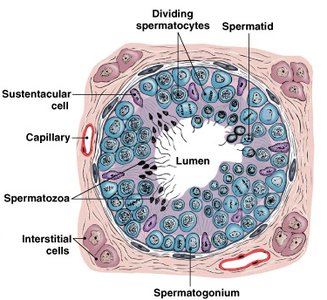
Sperm Structure
Mature sperm cells are highly specialized for motility and fertilization. They consist of a head, midpiece, and tail.
Head: Contains the nucleus and acrosome (enzymes for egg penetration)
Midpiece: Packed with mitochondria for energy
Tail (Flagellum): Provides motility
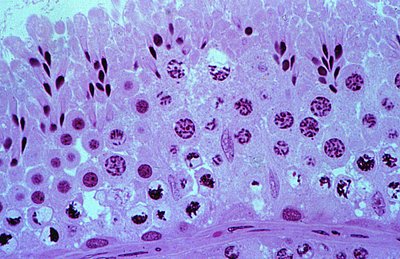
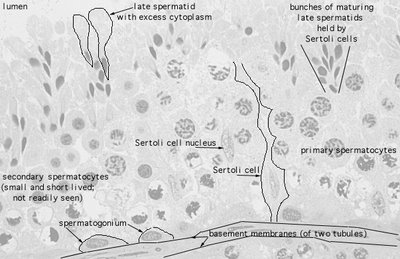
Blood-Testis Barrier
The blood-testis barrier is formed by tight junctions between Sertoli cells. It protects developing sperm from the immune system and harmful substances in the blood.
Function: Prevents autoimmune reactions against sperm antigens
Duct System
Pathway of Sperm
Sperm produced in the seminiferous tubules travel through a series of ducts before exiting the body during ejaculation.
Seminiferous Tubules → Rete Testis → Efferent Ductules → Epididymis → Vas (Ductus) Deferens → Ejaculatory Duct → Urethra
Epididymis
The epididymis is a coiled tube where sperm mature and are stored. It is lined with pseudostratified ciliated columnar epithelium with stereocilia.
Function: Sperm maturation (about 3 weeks) and storage
Vas (Ductus) Deferens
The vas deferens is a muscular tube that transports sperm from the epididymis to the ejaculatory duct.
Length: 16-18 inches
Function: Propels sperm during ejaculation
Ejaculatory Duct and Urethra
The ejaculatory duct is formed by the union of the vas deferens and the duct of the seminal vesicle. The urethra serves as the final passageway for sperm to exit the body.
External Genitalia
Penis
The penis is the male copulatory organ, containing three columns of erectile tissue: two corpora cavernosa and one corpus spongiosum (surrounding the urethra).
Glans: Expanded distal end
Prepuce: Foreskin covering the glans (if present)
Scrotum
The scrotum is a pouch of skin that houses the testes outside the body, providing a cooler environment necessary for normal sperm development.
Cremaster Muscle: Raises and lowers the testes in response to temperature changes
Spermatic Cord: Contains vas deferens, blood vessels, nerves, and cremaster muscle
Accessory Glands
Seminal Vesicles
Located posterior to the bladder
Secrete fructose (energy for sperm) and substances that buffer vaginal pH
Prostate Gland
Surrounds the prostatic urethra
Secretes seminalplasmin (antibiotic)
Bulbourethral (Cowper's) Glands
Secrete thick alkaline mucus to neutralize urinary acids and lubricate the glans
Summary Table: Pathway of Sperm
Order | Structure |
|---|---|
1 | Seminiferous tubules |
2 | Epididymis |
3 | Vas deferens |
4 | Ejaculatory duct |
5 | Prostatic urethra |
6 | Membranous urethra |
7 | Spongy (penile) urethra |
Key Concepts and Definitions
Spermatogenesis: The process of sperm cell development, involving meiosis and differentiation
Spermiogenesis: The final stage of spermatogenesis, involving morphological changes of spermatids into spermatozoa
Blood-Testis Barrier: A physical barrier that protects developing sperm from the immune system
Accessory Glands: Glands that contribute fluids to semen, supporting sperm viability and motility
Relevant Equations
Chromosome Number in Gametes and Zygote:
Meiosis:
Mitosis:
Additional info:
Development of the male reproductive system is dependent on the presence of testosterone and the SRY gene product (TDF).
Disorders of sex development (DSD) can result from chromosomal, genetic, or hormonal variations.
The reproductive system is unique in that it is not essential for individual survival, but is crucial for species propagation.
