 Back
BackChapter 6: Bones and Bone Structure – Comprehensive Study Notes
Study Guide - Smart Notes

Bones and Bone Structure
Functions of the Skeletal System
The skeletal system is essential for structural support, movement, and protection of the body. It consists of bones, cartilages, ligaments, and other connective tissues that stabilize and interconnect bones.
Structural Support: Provides the framework for the body and supports soft tissues.
Storage of Minerals and Lipids: Stores calcium, phosphorus, and lipids in yellow bone marrow.
Blood Cell Production: Red bone marrow produces red and white blood cells and platelets.
Protection: Shields vital organs (e.g., brain, heart, lungs).
Leverage: Bones act as levers for muscles, enabling movement.
Classification of Bones
Bones are classified by shape and structure, each with functional significance and characteristic markings.
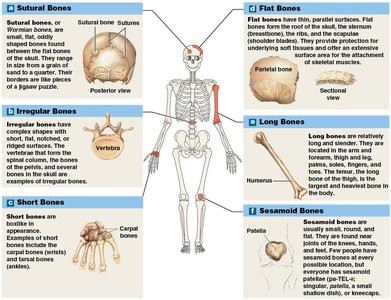
Sutural Bones: Small, flat, irregular bones found between skull bones. Number varies among individuals.
Irregular Bones: Complex shapes (e.g., vertebrae, pelvic bones).
Short Bones: Boxy, found in wrists (carpals) and ankles (tarsals).
Flat Bones: Thin, parallel surfaces (e.g., skull roof, sternum, ribs, scapulae).
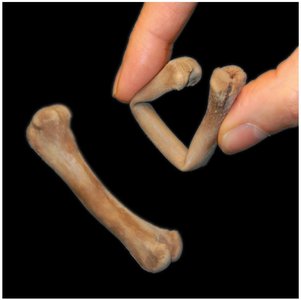
Long Bones: Long and slender (e.g., humerus, femur, fingers, toes).
Sesamoid Bones: Small, round, flat bones within tendons (e.g., patella).
Bone Markings
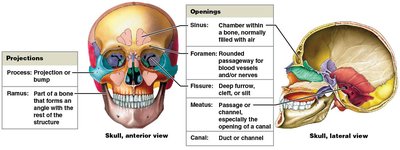
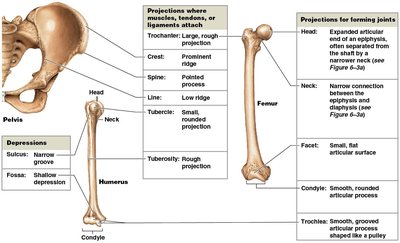
Bone markings are surface features that serve as sites for muscle attachment, articulation, or passage of blood vessels and nerves.
Projections: Attachment points for muscles, tendons, ligaments; articulation with other bones.
Openings and Depressions: Passageways for blood vessels and nerves.
Structure of Long and Flat Bones
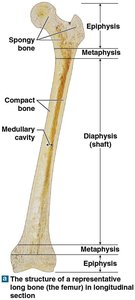
Long Bone: Consists of diaphysis (shaft, compact bone), epiphysis (ends, spongy bone), and metaphysis (connects shaft and ends).
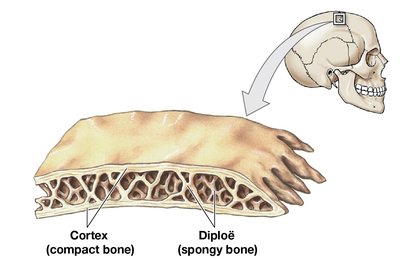
Flat Bone: Core of spongy bone (diploë) between two layers of compact bone (cortex).
Bone Tissue
Bone (osseous) tissue is a dense connective tissue composed of specialized cells and a solid extracellular matrix.
Matrix: Two-thirds calcium phosphate (hydroxyapatite crystals), one-third collagen fibers.
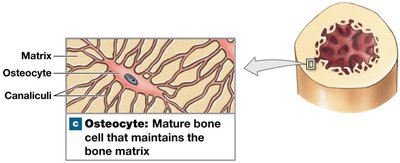
Osteocytes: Bone cells in lacunae, connected by canaliculi for nutrient/waste exchange.
Periosteum: Covers bone surfaces (except joints), with fibrous and cellular layers.
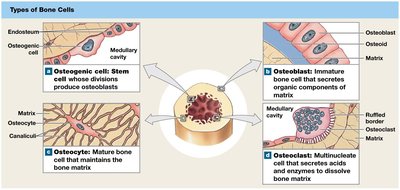
Types of Bone Cells
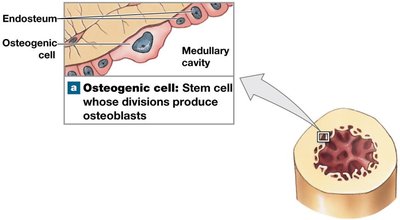
Osteogenic (Osteoprogenitor) Cells: Stem cells that produce osteoblasts; important for fracture repair.
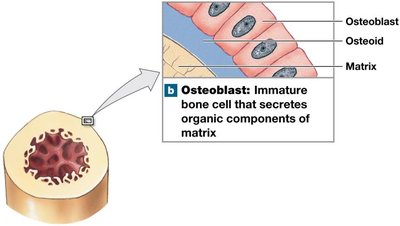
Osteoblasts: Immature cells responsible for osteogenesis (new bone matrix production).
Osteocytes: Mature bone cells maintaining matrix and aiding repair.
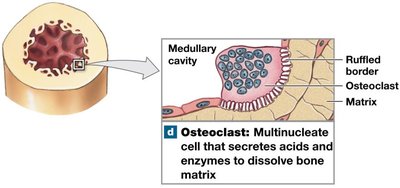
Osteoclasts: Multinucleate cells that absorb and remove bone matrix (osteolysis).
Compact Bone and Spongy Bone
Compact and spongy bone have distinct structures and functions, contributing to bone strength and flexibility.
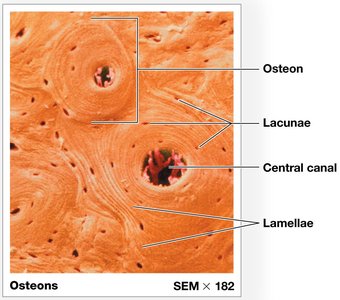
Compact Bone: Organized into osteons (central canal, lamellae, lacunae); provides strength and protection.
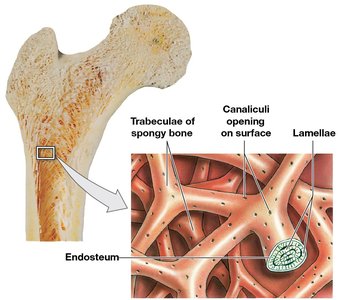
Spongy Bone: Network of trabeculae; lighter, withstands stress from multiple directions, supports red bone marrow.
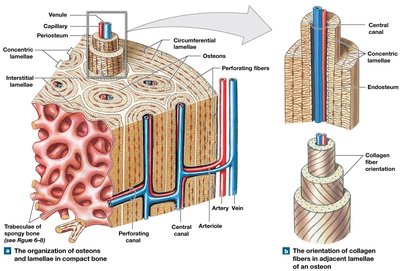
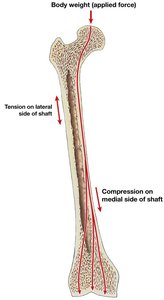
Distribution of Forces
The femur demonstrates how compact and spongy bone coordinate to transfer and resist forces.
Medial shaft compresses under weight; lateral shaft resists bending (tension).
Surface Coverings: Periosteum and Endosteum
Periosteum: Membrane covering bone; isolates bone, provides blood vessel/nerves route, aids growth/repair.
Endosteum: Incomplete cellular layer lining inner surfaces; active in growth, repair, remodeling.
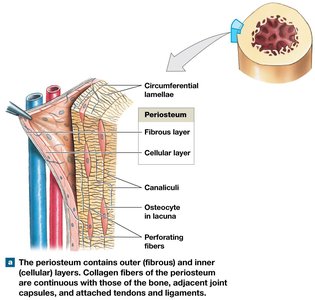
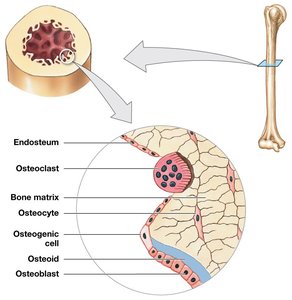
Bone Formation and Growth
Bone formation (ossification) occurs via two mechanisms: endochondral and intramembranous ossification.
Endochondral Ossification: Bone replaces cartilage; primary and secondary ossification centers form, leading to growth in length and width.
Intramembranous Ossification: Bone forms directly from mesenchymal tissue; produces flat bones (skull, mandible, clavicle).
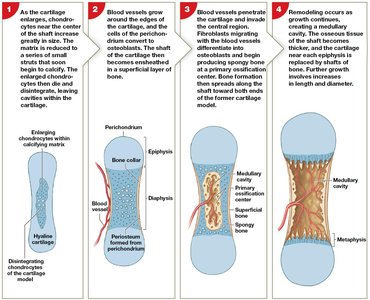
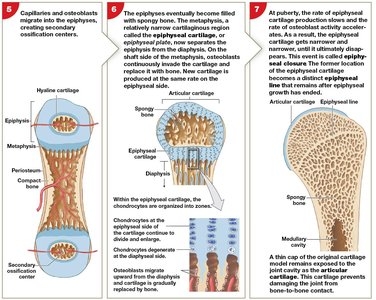
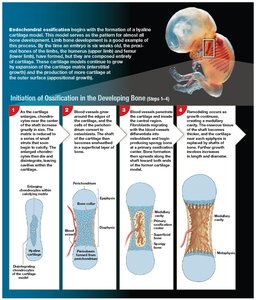
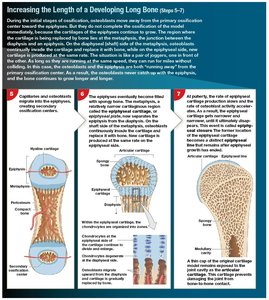
Bone Growth
Interstitial Growth: Growth in length at epiphyseal plate; ends with epiphyseal closure (epiphyseal line remains).
Appositional Growth: Growth in width; osteoblasts add lamellae, osteoclasts enlarge medullary cavity.
Bone Remodeling
Bone remodeling is a continuous process involving osteocytes, osteoblasts, and osteoclasts, maintaining bone structure and mineral content.
Balanced activity keeps bones healthy; imbalance leads to weakening or strengthening.
Exercise, Nutrition, and Hormones
Bone health is influenced by physical activity, nutrition, and hormones.
Exercise: Stimulates bone strength; inactivity causes bone loss.
Nutrition: Essential minerals (calcium, phosphorus, magnesium, etc.), vitamins (D, C, A, K, B12).
Hormones: Growth hormone, thyroxine, sex hormones, parathyroid hormone, calcitonin regulate growth and calcium homeostasis.
Abnormal Bone Development
Pituitary Growth Failure: Short bones due to low growth hormone.
Gigantism: Excess growth hormone before puberty.
Acromegaly: Excess growth hormone after epiphyseal closure.
Marfan Syndrome: Excess cartilage formation, tall stature.
Calcium Homeostasis
Bones store most of the body's calcium, which is vital for physiological processes. Calcium levels are regulated by hormones.
Parathyroid Hormone (PTH): Increases blood calcium by stimulating osteoclasts, increasing intestinal absorption, decreasing kidney excretion.
Calcitonin: Decreases blood calcium by inhibiting osteoclasts, increasing kidney excretion, decreasing intestinal absorption.
Osteomalacia: Weak, flexible bones due to poor mineralization; rickets is a form caused by vitamin D deficiency.
Fractures and Repair
Fractures are breaks in bone due to stress. They are classified by type and undergo a multi-step repair process.
Types: Open (compound), closed (simple), transverse, displaced, compression, spiral, epiphyseal, comminuted, greenstick, Colles, Pott's.
Repair Steps:
Fracture hematoma formation (blood clot).
Callus formation (internal and external callus).
Spongy bone formation (osteoblasts replace cartilage).
Compact bone formation (remodeling).
The Effects of Aging on Bones
Aging leads to reduced bone mass and increased fragility.
Osteopenia: Begins between ages 30–40; more pronounced in women.
Osteoporosis: Severe bone loss, common in postmenopausal women; increases fracture risk.
