 Back
BackChapter 6: Bones and Bone Structure – Study Notes
Study Guide - Smart Notes

Introduction to the Skeletal System
Overview of the Skeletal System
The skeletal system is a complex framework that provides structure, protection, and support for the human body. It consists of bones, cartilages, ligaments, and other connective tissues that stabilize or interconnect the bones.
Structural Support: The skeleton forms the internal framework that supports the body and maintains its shape.
Mineral and Lipid Storage: Bones store essential minerals such as calcium and phosphate, as well as lipids in yellow bone marrow.
Blood Cell Production: Red bone marrow produces red blood cells, white blood cells, and platelets.
Protection: Bones protect vital organs, including the brain, heart, and lungs.
Leverage for Movement: Bones act as levers that muscles pull on to produce movement.

Classification of Bones by Shape
Categories of Bone Shapes
Bones are classified into six broad categories based on their shapes, each with distinct structural and functional characteristics.
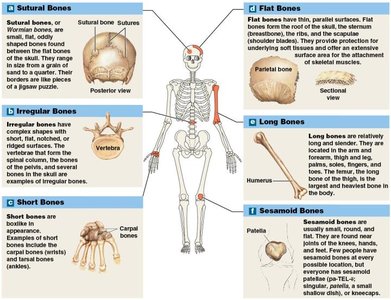
Sutural Bones (Wormian Bones): Small, flat, irregularly shaped bones found between the flat bones of the skull, associated with cranial sutures. Their number and position vary among individuals.
Irregular Bones: Complex shapes not fitting other categories, such as vertebrae and pelvic bones.
Short Bones: Boxy in appearance, found in the wrists (carpals) and ankles (tarsals).
Flat Bones: Thin with parallel surfaces, including the skull roof, sternum, ribs, and scapulae. They provide protection and surfaces for muscle attachment.
Long Bones: Long and slender, found in the arms, legs, palms, soles, fingers, and toes (e.g., humerus, femur).
Sesamoid Bones: Small, round, and flat bones found within tendons near joints (e.g., patella). Their number and position can vary among individuals.
Bone Markings
Types and Functions of Bone Markings
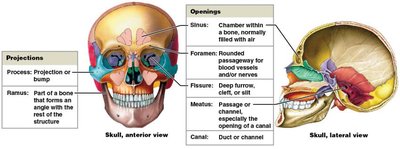
Bones display characteristic surface features known as bone markings, which serve as sites for muscle, tendon, and ligament attachment, as well as passages for blood vessels and nerves.
Projections: Sites for attachment or articulation (e.g., process, ramus, head, condyle, crest, tuberosity, trochanter).
Openings: Allow passage of blood vessels and nerves (e.g., foramen, canal, fissure, meatus, sinus).
Depressions: May accommodate soft tissues or form articulations (e.g., fossa, sulcus).
Type | Example | Description |
|---|---|---|
Projection | Process, Ramus | Bony prominence or angle |
Opening | Foramen, Canal | Passage for nerves/vessels |
Depression | Fossa, Sulcus | Shallow basin or groove |
Bone Structure
Structure of Long and Flat Bones
Bones have specialized structures that reflect their functions and locations in the body.
Long Bone Structure:
Diaphysis: The shaft, composed of compact bone surrounding a medullary (marrow) cavity.
Epiphysis: The expanded ends, mostly spongy bone covered by compact bone.
Metaphysis: The narrow region connecting diaphysis and epiphysis.
Flat Bone Structure: Consists of a layer of spongy bone (diploë) sandwiched between two layers of compact bone.
Bone Tissue and Matrix
Composition and Properties of Bone Tissue
Bone tissue is a specialized connective tissue with a dense matrix composed of inorganic and organic components.
Matrix: Contains calcium phosphate (Ca3(PO4)2), which interacts with calcium hydroxide (Ca(OH)2) to form hydroxyapatite crystals. These crystals incorporate other salts and ions, making bone hard and resistant to compression.
Collagen Fibers: Provide flexibility and a framework for mineral deposition, making bone strong yet somewhat flexible.
Osteocytes: Mature bone cells located in lacunae, connected by canaliculi for nutrient and waste exchange.
Key Equation:
(Hydroxyapatite formation)
Bone Cells
Types and Functions of Bone Cells
There are four main types of bone cells, each with distinct roles in bone formation, maintenance, and remodeling.
Osteogenic Cells: Stem cells that divide to produce osteoblasts; found in periosteum and endosteum; important for fracture repair.
Osteoblasts: Immature bone cells that synthesize new bone matrix (osteoid) and promote mineralization; become osteocytes when surrounded by matrix.
Osteocytes: Mature bone cells that maintain bone matrix and help repair damaged bone; reside in lacunae and communicate via canaliculi.
Osteoclasts: Large, multinucleate cells that resorb bone matrix (osteolysis); derived from macrophage lineage; regulate calcium and phosphate levels.
Compact and Spongy Bone
Organization and Function
Bone tissue is organized into two main types: compact and spongy bone, each with unique structural features.
Compact Bone:
Composed of osteons (Haversian systems) with central canals containing blood vessels.
Lamellae are arranged in concentric, interstitial, and circumferential layers.
Perforating (Volkmann's) canals connect blood supply between osteons and the medullary cavity.
Spongy Bone:
Composed of trabeculae (lattice-like matrix) without osteons.
Spaces between trabeculae contain red bone marrow (hematopoiesis) or yellow bone marrow (fat storage).
Bone Membranes
Periosteum and Endosteum
Bones are covered and lined by specialized membranes that play roles in growth, repair, and nutrition.
Periosteum: A double-layered membrane covering the outer surface of bones; consists of an outer fibrous layer and an inner cellular layer; isolates bone, provides routes for blood vessels and nerves, and participates in growth and repair.
Endosteum: A thin, incomplete cellular layer lining the medullary cavity, trabeculae, and central canals; active in bone growth, repair, and remodeling.
Bone Formation and Growth
Ossification Processes
Bone formation (ossification) occurs through two main processes: endochondral and intramembranous ossification.
Endochondral Ossification: Bone replaces a pre-existing cartilage model; primary process for long bones. Steps include cartilage model formation, calcification, invasion by blood vessels, formation of primary and secondary ossification centers, and replacement of cartilage by bone.
Intramembranous Ossification: Bone develops directly from mesenchymal tissue without a cartilage model; primary process for flat bones (e.g., skull, mandible, clavicles).
Growth in Length: Occurs at the epiphyseal plate by interstitial growth until epiphyseal closure (formation of epiphyseal line).
Growth in Width: Appositional growth adds bone to the outer surface while osteoclasts enlarge the medullary cavity.
Bone Vascularization and Innervation
Blood and Nerve Supply
Bones are highly vascularized and innervated, ensuring nutrient delivery, waste removal, and sensory perception.
Nutrient Artery and Vein: Supply the diaphysis via nutrient foramina.
Metaphyseal Vessels: Supply the metaphysis and epiphyseal cartilage.
Periosteal Vessels: Supply superficial osteons and secondary ossification centers.
Nerves: Sensory nerves innervate periosteum, endosteum, medullary cavity, and epiphyses, making bone injuries painful.
Bone Remodeling
Continuous Bone Renewal
Bone remodeling is a lifelong process involving the coordinated activity of osteocytes, osteoblasts, and osteoclasts. It maintains bone strength and mineral homeostasis.
Osteoclasts: Remove bone matrix (resorption).
Osteoblasts: Add new bone matrix.
Balance: If osteoclast activity exceeds osteoblast activity, bones weaken; the reverse strengthens bones.
Exercise: Weight-bearing activities stimulate bone strengthening.
Calcium Homeostasis
Regulation of Blood Calcium Levels
The skeleton acts as a reservoir for calcium, which is essential for many physiological processes. Blood calcium levels are tightly regulated by hormones.
Parathyroid Hormone (PTH): Released when blood calcium is low; increases osteoclast activity, enhances intestinal absorption (via calcitriol), and decreases renal excretion of calcium.
Calcitonin: Released when blood calcium is high; inhibits osteoclasts, increases renal excretion, and decreases intestinal absorption of calcium.
Hormone | Source | Effect on Blood Calcium | Mechanism |
|---|---|---|---|
Parathyroid Hormone (PTH) | Parathyroid glands | Increases | Stimulates osteoclasts, increases absorption, decreases excretion |
Calcitonin | Thyroid gland (C cells) | Decreases | Inhibits osteoclasts, increases excretion, decreases absorption |
Fractures
Types of Bone Fractures
Fractures are breaks in bones caused by physical stress. They are classified based on their characteristics and whether the bone pierces the skin.
Open (Compound) Fracture: Bone projects through the skin, increasing risk of infection.
Closed (Simple) Fracture: Bone remains internal, not breaking the skin.
