Back
BackComprehensive Study Notes: The Reproductive System (Male & Female) and Gametogenesis
Study Guide - Smart Notes

Introduction to the Male and Female Reproductive Systems
Overview
The reproductive system is essential for the survival of a species, though not for the individual. Both male and female systems share core similarities, including the presence of gonads (testes in males, ovaries in females), which produce gametes and secrete sex hormones. Accessory reproductive organs support the function of these systems. The reproductive system remains inactive until puberty, when it becomes functional.
Gonads: Primary sex organs; produce gametes and sex hormones (testosterone, estrogens).
Gametes: Sperm (male), ova (female); produced via meiosis.
Accessory Organs: Aid in the transport, nourishment, and maturation of gametes.
Cell Chemistry & Cell Components: Chromosomes and Meiosis
Chromosome Structure and Types
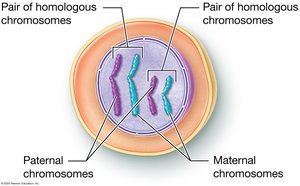
Somatic cells are diploid (2n), containing 46 chromosomes (23 pairs), with one set from each parent. Each pair is termed homologous chromosomes, carrying genes for the same traits but possibly different alleles.
Homologous Chromosomes: One maternal and one paternal chromosome per pair.
Alleles: Variants of a gene found at the same locus on homologous chromosomes.
DNA Replication and Chromatid Formation
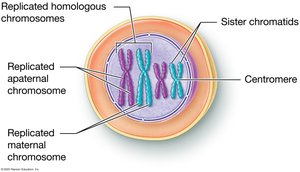
Before cell division, DNA replicates, forming sister chromatids joined at a centromere. Chromatin is the uncondensed form of DNA present when the cell is not dividing.
Sister Chromatids: Identical copies of a chromosome, joined at the centromere.
Centromere: Region where sister chromatids are attached.
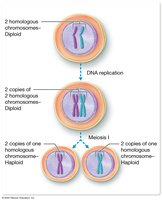
Diploid and Haploid Cells
Meiosis reduces chromosome number by half, producing haploid (n) gametes. Fertilization restores diploidy in the zygote.
Diploid (2n): Two sets of chromosomes (somatic cells).
Haploid (n): One set of chromosomes (gametes).
Fertilization: Fusion of sperm and ovum to form a zygote (2n).
Energy & Cell Processes: Meiosis
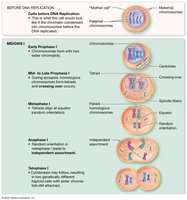
Overview of Meiosis
Meiosis consists of two sequential divisions (Meiosis I and II) that result in four genetically unique haploid cells. Genetic variability is introduced through crossing over and independent assortment.
Crossing Over (Prophase I): Exchange of genetic material between homologous chromosomes, increasing genetic diversity.
Independent Assortment (Anaphase I): Random distribution of maternal and paternal chromosomes to gametes.
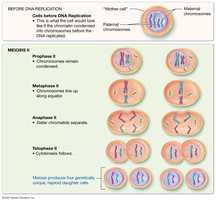
Stages of Meiosis II
Meiosis II resembles mitosis, separating sister chromatids into four unique haploid cells.
Prophase II: Chromosomes condense, nuclear envelope breaks down.
Metaphase II: Chromosomes align at the equator.
Anaphase II: Sister chromatids separate.
Telophase II: Nuclear membranes reform, cytokinesis produces four haploid cells.
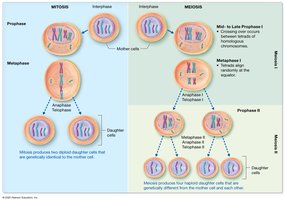
Comparing Mitosis and Meiosis
Key Differences
Mitosis produces two genetically identical diploid cells for growth and repair, while meiosis produces four genetically unique haploid gametes for sexual reproduction.
Mitosis: One division, no crossing over, identical daughter cells.
Meiosis: Two divisions, crossing over, unique daughter cells.
Anatomy of the Male Reproductive System
Internal and External Structures
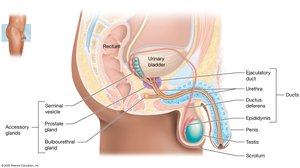
The male reproductive system includes the testes, duct system, accessory glands, and external genitalia. Sperm are produced in the testes and transported through the duct system, with fluids from accessory glands forming semen.
Testes: Produce sperm and testosterone.
Duct System: Epididymis, ductus deferens, ejaculatory duct, urethra.
Accessory Glands: Seminal vesicles, prostate, bulbourethral glands.
External Structures: Scrotum, penis.
Testes and Spermatogenesis
Testicular Structure
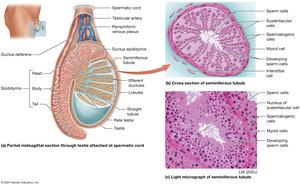
The testes are divided into lobules containing seminiferous tubules, where spermatogenesis occurs. Sertoli (sustentacular) cells support developing sperm, while Leydig (interstitial) cells produce testosterone.
Seminiferous Tubules: Site of sperm production.
Sertoli Cells: Support and nourish developing sperm.
Leydig Cells: Secrete testosterone.
Duct System and Penis
Pathway of Sperm
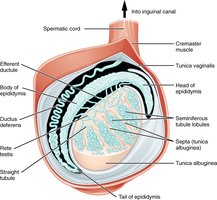
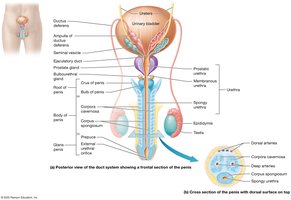
Sperm mature in the epididymis, travel through the ductus deferens, and are expelled via the urethra during ejaculation. The penis serves as the copulatory organ, delivering sperm into the female reproductive tract.
Epididymis: Sperm maturation and storage.
Ductus Deferens: Transports sperm to the ejaculatory duct.
Urethra: Passage for urine and semen.
Penis: Contains erectile tissue for erection and ejaculation.
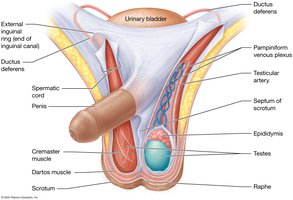
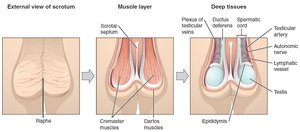
Support Structures: Scrotum and Spermatic Cord
Temperature Regulation
The scrotum and spermatic cord maintain optimal temperature for spermatogenesis, about 3°C below core body temperature. The pampiniform venous plexus and cremaster/dartos muscles regulate heat exchange and testicular position.
Scrotum: Houses testes, regulates temperature.
Spermatic Cord: Contains ductus deferens, vessels, nerves.
Pampiniform Plexus: Cools arterial blood.
Cremaster/Dartos Muscles: Adjust testicular proximity to body.
Spermatogenesis and Spermiogenesis
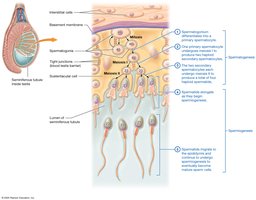
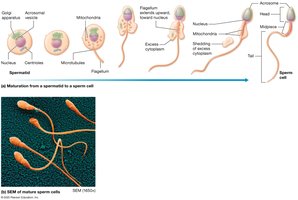
Stages of Sperm Development
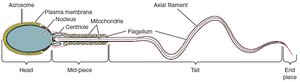
Spermatogenesis is the process of sperm cell development, beginning with spermatogonia and ending with mature spermatozoa. Spermiogenesis is the final maturation phase, involving morphological changes.
Spermatogonia: Diploid stem cells.
Primary Spermatocyte: Undergoes meiosis I.
Secondary Spermatocyte: Undergoes meiosis II.
Spermatids: Undergo spermiogenesis to become spermatozoa.
Hormonal Control of Male Reproduction
Hypothalamic-Pituitary-Gonadal (HPG) Axis
Testosterone production and spermatogenesis are regulated by the HPG axis. GnRH from the hypothalamus stimulates LH and FSH release from the anterior pituitary. LH stimulates Leydig cells to produce testosterone; FSH acts on Sertoli cells to support spermatogenesis and secrete inhibin.
GnRH: Gonadotropin-releasing hormone from hypothalamus.
LH: Stimulates testosterone production.
FSH: Stimulates Sertoli cells and spermatogenesis.
Inhibin: Inhibits FSH release (negative feedback).
Anatomy of the Female Reproductive System
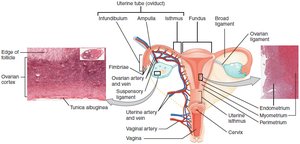
Internal and External Structures
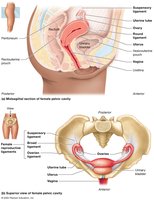
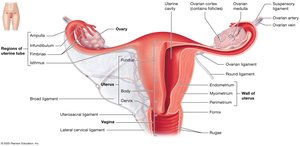
The female reproductive system includes the ovaries, uterine tubes, uterus, and vagina. External genitalia (vulva) and mammary glands are also part of the system. The system supports fertilization, gestation, and parturition.
Ovaries: Produce oocytes and secrete estrogens and progesterone.
Uterine Tubes: Transport oocyte; site of fertilization.
Uterus: Site of implantation and fetal development.
Vagina: Receives penis and serves as birth canal.
Oogenesis and the Ovarian Cycle
Oogenesis
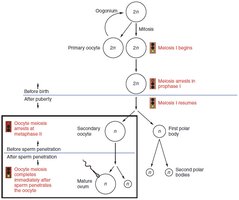
Oogenesis is the process of ovum development, beginning before birth and continuing until menopause. It involves mitosis, meiosis, and the formation of polar bodies.
Oogonia: Diploid stem cells; undergo mitosis before birth.
Primary Oocytes: Arrested in prophase I until puberty.
Secondary Oocyte: Arrested in metaphase II; completes meiosis if fertilized.
Polar Bodies: Small cells that degenerate.
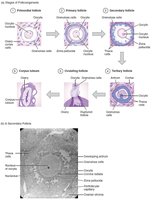
Ovarian Follicles and Cycle
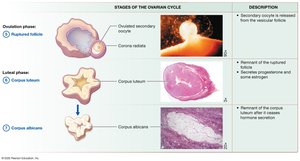
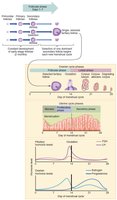
Folliculogenesis is the maturation of ovarian follicles. The ovarian cycle consists of the follicular phase, ovulation, and luteal phase, regulated by the HPG axis.
Follicular Phase: Follicle growth and maturation.
Ovulation: Release of secondary oocyte.
Luteal Phase: Corpus luteum formation and hormone secretion.
Hormonal Regulation of the Ovarian and Uterine Cycles
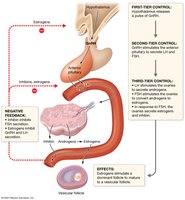
Hormonal Feedback Loops
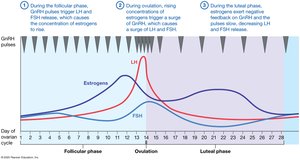
The ovarian and uterine cycles are regulated by feedback loops involving GnRH, LH, FSH, estrogens, and progesterone. The timing and levels of these hormones coordinate follicle development, ovulation, and preparation of the endometrium for implantation.
GnRH: Pulsatile release controls LH and FSH secretion.
Estrogens: Stimulate endometrial growth, exert positive/negative feedback.
Progesterone: Maintains endometrium, inhibits GnRH/LH/FSH.
The Uterine (Menstrual) Cycle
Phases of the Uterine Cycle
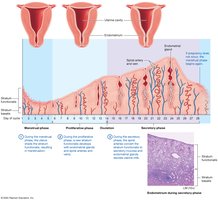
The uterine cycle involves cyclic changes in the endometrium, preparing for possible implantation. It consists of the menstrual, proliferative, and secretory phases.
Menstrual Phase (Days 1–5): Shedding of the stratum functionalis.
Proliferative Phase (Days 6–14): Regeneration of the endometrium.
Secretory Phase (Days 15–28): Endometrial glands secrete nutrients; maintained by progesterone.
Major Reproductive Hormones in Males and Females
Summary Table
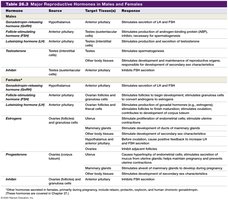
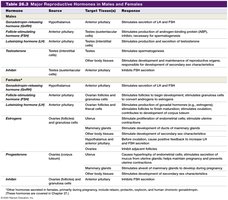
The following table summarizes the major reproductive hormones, their sources, target tissues, and responses in males and females.
Hormone | Source | Target Tissue(s) | Response |
|---|---|---|---|
GnRH | Hypothalamus | Anterior pituitary | Stimulates secretion of LH and FSH |
LH | Anterior pituitary | Testes/Ovaries | Stimulates testosterone/estrogen and ovulation |
FSH | Anterior pituitary | Testes/Ovaries | Stimulates spermatogenesis/follicle development |
Testosterone | Testes | Various | Male secondary sex characteristics, spermatogenesis |
Estrogens | Ovaries | Various | Female secondary sex characteristics, endometrial growth |
Progesterone | Ovaries | Uterus | Maintains endometrium |
Inhibin | Sertoli/Granulosa cells | Anterior pituitary | Inhibits FSH secretion |