 Back
BackComprehensive Study Notes: The Reproductive System (Male & Female) and Gametogenesis
Study Guide - Smart Notes

Introduction to the Male and Female Reproductive Systems
Overview
The reproductive system is essential for the survival of a species, though not for the individual. It remains inactive until puberty, when reproductive organs mature and become functional. Both male and female systems share similarities, including the presence of gonads (testes in males, ovaries in females), which produce gametes and secrete sex hormones.
Gonads: Primary sex organs; produce gametes (sperm and ova) and secrete sex hormones (testosterone, estrogens).
Accessory reproductive organs: Support gamete transport and reproductive function.
Overview of Meiosis
Chromosome Structure and Genetic Variation
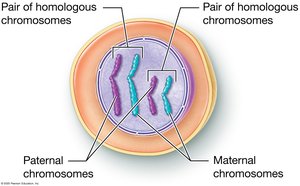
Somatic cells are diploid (2n), containing 46 chromosomes (23 pairs), with one set from each parent. Each pair is called homologous chromosomes, carrying the same genes but possibly different alleles. Meiosis is the process by which gametes are produced, reducing the chromosome number by half to ensure genetic stability across generations.
Homologous chromosomes: One maternal and one paternal chromosome per pair.
Alleles: Variants of a gene found at the same locus on homologous chromosomes.
Fertilization: Fusion of sperm and ovum to form a zygote with 46 chromosomes.
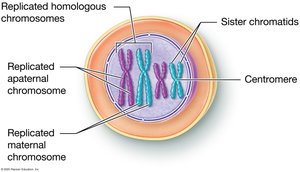
DNA Replication and Chromosome Structure
Before meiosis, DNA is replicated, resulting in chromosomes composed of two identical sister chromatids joined at a centromere. Chromatin is the less condensed form of DNA present when the cell is not dividing.
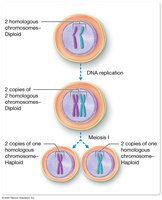
Diploid and Haploid Cells
Meiosis reduces the chromosome number from diploid (2n) to haploid (n). After DNA replication, cells have two copies of each chromosome. Meiosis I separates homologous chromosomes, and Meiosis II separates sister chromatids, resulting in four genetically unique haploid cells.
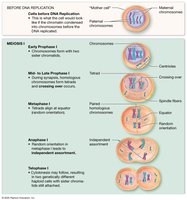
Stages of Meiosis I
Meiosis I includes several stages:
Prophase I: Homologous chromosomes pair and exchange segments (crossing over), increasing genetic diversity.
Metaphase I: Homologous pairs align at the cell equator.
Anaphase I: Homologous chromosomes separate (independent assortment).
Telophase I: Two haploid cells form, each with duplicated chromosomes.
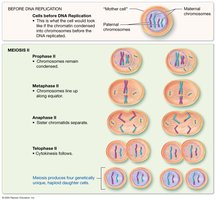
Stages of Meiosis II
Meiosis II resembles mitosis:
Prophase II: Chromosomes condense.
Metaphase II: Chromosomes align at the equator.
Anaphase II: Sister chromatids separate.
Telophase II: Four genetically unique haploid cells are produced.
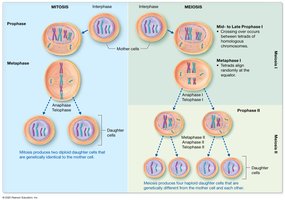
Comparison of Mitosis and Meiosis
Mitosis produces two genetically identical diploid cells for growth and repair, while meiosis produces four genetically unique haploid gametes for reproduction. Key differences include crossing over and independent assortment in meiosis, which increase genetic diversity.
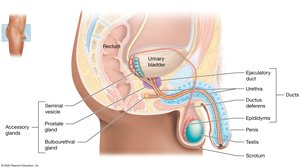
Anatomy of the Male Reproductive System
Internal and External Structures
The male reproductive system includes the testes, duct system, accessory glands, and external genitalia (penis and scrotum). Sperm are produced in the testes and transported through the duct system, with fluids from accessory glands forming semen.
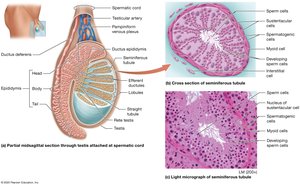
Testes
The testes are paired organs located in the scrotum. They contain seminiferous tubules where spermatogenesis occurs. Interstitial (Leydig) cells between tubules produce testosterone. Myoid cells help move sperm and fluid out of the testis.
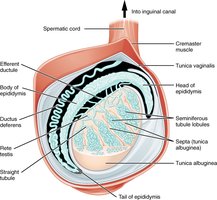
Duct System
The duct system includes the epididymis (site of sperm maturation and storage), ductus (vas) deferens (transports sperm), ejaculatory duct (joins with seminal vesicle duct), and urethra (transports urine and semen).
Penis
The penis is the male copulatory organ, containing erectile tissue that fills with blood during sexual arousal, resulting in an erection. The glans penis is the enlarged tip, and the prepuce (foreskin) may be removed by circumcision.
Accessory Sex Glands
Accessory glands include the seminal vesicles (produce seminal fluid), prostate gland (produces prostatic fluid), and bulbourethral glands (secrete alkaline mucus). These fluids nourish sperm and facilitate their movement.
Support Structures: Scrotum and Spermatic Cord
The scrotum houses the testes and regulates their temperature. The spermatic cord contains blood vessels, nerves, and the ductus deferens. Temperature regulation is essential for spermatogenesis.
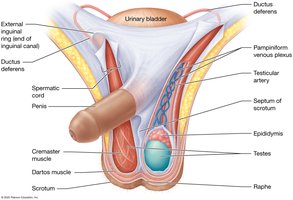
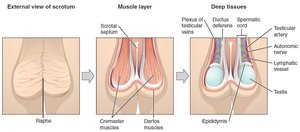
Spermatogenesis and Spermiogenesis
Spermatogenesis
Spermatogenesis is the process of sperm cell development, beginning at puberty and continuing throughout life. It occurs in the seminiferous tubules and involves mitosis, meiosis, and maturation.
Spermatogonia: Diploid stem cells that divide by mitosis.
Primary spermatocytes: Undergo meiosis I to form secondary spermatocytes.
Secondary spermatocytes: Undergo meiosis II to form spermatids.
Spermatids: Mature into spermatozoa (sperm cells).
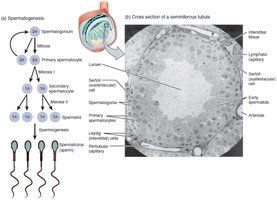
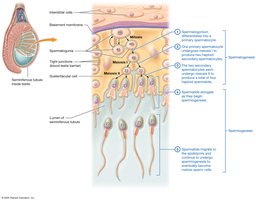
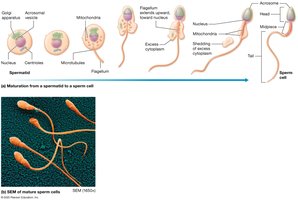
Spermiogenesis
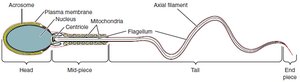
Spermiogenesis is the maturation of spermatids into spermatozoa, involving the formation of the acrosome, development of the flagellum, and condensation of the nucleus.
Sustentacular (Sertoli) Cells
Sertoli cells support and nourish developing sperm, form the blood-testis barrier, and secrete substances that regulate spermatogenesis.
Hormonal Control of Male Reproduction
Hypothalamic-Pituitary-Gonadal (HPG) Axis
The HPG axis regulates testosterone production and spermatogenesis through a multi-tiered feedback loop:
GnRH (from hypothalamus) stimulates the anterior pituitary.
LH stimulates Leydig cells to produce testosterone.
FSH stimulates Sertoli cells to support spermatogenesis.
Negative feedback by testosterone and inhibin regulates hormone levels.
Anatomy of the Female Reproductive System
Internal Organs
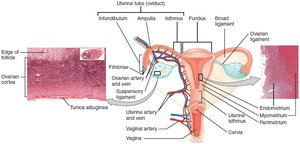
The female reproductive system includes the ovaries, uterine tubes (fallopian tubes), uterus, and vagina. Most organs are located in the pelvic cavity and are supported by ligaments.
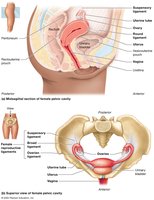
Ovaries
Ovaries produce oocytes and secrete estrogens and progesterone. The cortex contains follicles at various stages of development, while the medulla houses blood vessels and nerves.
Uterine Tubes
Uterine tubes transport oocytes from the ovaries to the uterus. Fimbriae help capture the oocyte during ovulation.
Uterus
The uterus is the site of implantation and fetal development. It has three layers: perimetrium (outer), myometrium (muscular), and endometrium (inner mucosa).
Vagina
The vagina is the female copulatory organ and birth canal. Its mucosa is stratified squamous epithelium, and it maintains an acidic pH to reduce infection risk.
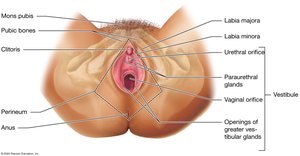
External Genitalia (Vulva)
The vulva includes the mons pubis, labia majora and minora, clitoris, and vestibule. The perineum is the region between the vulva and anus.
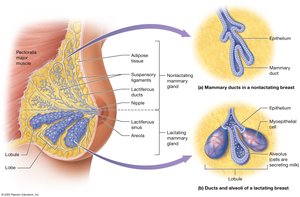
Mammary Glands
Mammary glands are modified sweat glands that produce milk. Each breast contains lobes, lobules, and ducts leading to the nipple.
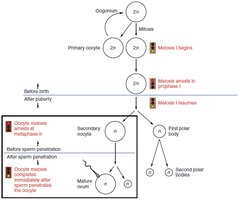
Oogenesis and the Ovarian Cycle
Oogenesis
Oogenesis is the process of ovum development. It begins before birth, pauses until puberty, and resumes with each ovarian cycle. Only one secondary oocyte is typically released per cycle.
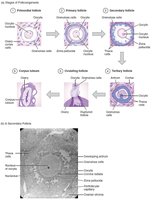
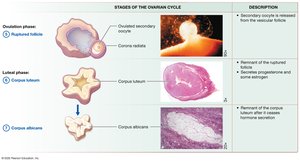
Folliculogenesis and the Ovarian Cycle
Follicles mature through several stages: primordial, primary, secondary, and vesicular (tertiary). The ovarian cycle consists of the follicular phase, ovulation, and luteal phase.
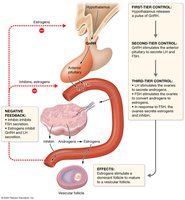
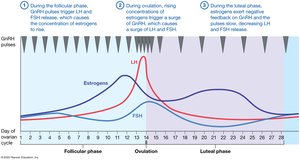
Hormonal Regulation of the Ovarian Cycle
The ovarian cycle is regulated by the HPG axis, with GnRH, LH, and FSH controlling follicle development and hormone secretion. Estrogen and inhibin provide feedback to regulate the cycle.
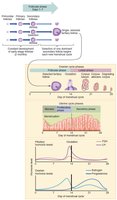
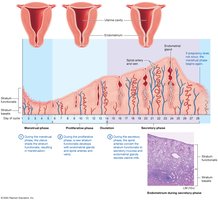
The Uterine (Menstrual) Cycle
Phases of the Uterine Cycle
The uterine cycle involves cyclic changes in the endometrium:
Menstrual phase (days 1–5): Shedding of the functional layer.
Proliferative phase (days 6–14): Regeneration of the endometrium.
Secretory phase (days 15–28): Endometrium prepares for implantation; if no fertilization, the cycle restarts.
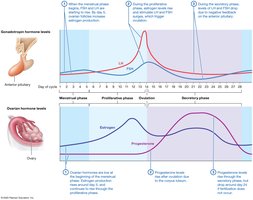
Hormonal Control of the Uterine Cycle
Estrogen and progesterone from the ovaries regulate the uterine cycle. LH and FSH surges trigger ovulation, while progesterone maintains the secretory phase. If fertilization does not occur, hormone levels drop, leading to menstruation.
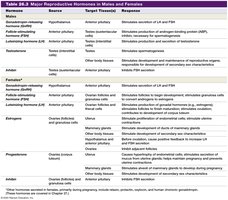
Major Reproductive Hormones in Males and Females
Summary Table
The following tables summarize the major reproductive hormones, their sources, target tissues, and responses in males and females.
Hormone | Source | Target Tissue(s) | Response |
|---|---|---|---|
GnRH | Hypothalamus | Anterior pituitary | Stimulates secretion of LH and FSH |
LH | Anterior pituitary | Testes/Ovaries | Stimulates testosterone/estrogen and ovulation |
FSH | Anterior pituitary | Testes/Ovaries | Stimulates spermatogenesis/follicle development |
Testosterone | Testes | Various | Male secondary sex characteristics, spermatogenesis |
Estrogens | Ovaries | Various | Female secondary sex characteristics, endometrial growth |
Progesterone | Ovaries | Uterus, mammary glands | Maintains endometrium, prepares for pregnancy |
Inhibin | Sertoli/Granulosa cells | Anterior pituitary | Inhibits FSH secretion |
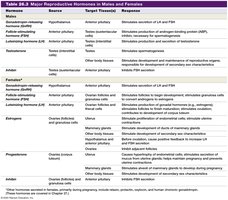
Additional info: Other hormones such as relaxin, prolactin, oxytocin, and human chorionic gonadotropin are important during pregnancy and lactation (covered in later chapters).
