 Back
BackEndocrine Functions of the Pancreas, Gonads, and Other Organs
Study Guide - Smart Notes

Endocrine Role of the Pancreas, Gonads, and Other Organs
The Pancreas: Structure and Function
The pancreas is a mixed gland located partially behind the stomach, containing both endocrine and exocrine cells. Its endocrine function is carried out by the pancreatic islets (islets of Langerhans), which contain two main types of hormone-producing cells: alpha cells (secrete glucagon) and beta cells (secrete insulin). These hormones regulate blood glucose levels in an antagonistic manner.
Alpha cells: Release glucagon, a hyperglycemic hormone.
Beta cells: Release insulin, a hypoglycemic hormone.
Acinar cells: Exocrine cells producing digestive enzymes.
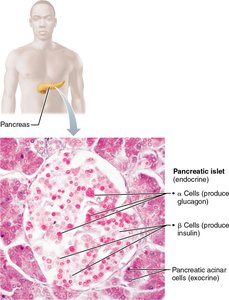
Additional info: The pancreas also produces somatostatin and pancreatic polypeptide, but their roles are less prominent in glucose regulation.
Regulation of Blood Glucose: Insulin and Glucagon
Blood glucose homeostasis is maintained by the opposing actions of insulin and glucagon. Insulin lowers blood glucose by promoting cellular uptake and storage, while glucagon raises blood glucose by stimulating hepatic glucose release.
Glucagon: Stimulates glycogenolysis and gluconeogenesis in the liver, increasing blood glucose.
Insulin: Enhances glucose uptake by cells, inhibits glycogen breakdown, and suppresses gluconeogenesis.
Stimuli: Low blood glucose triggers glucagon; high blood glucose triggers insulin.
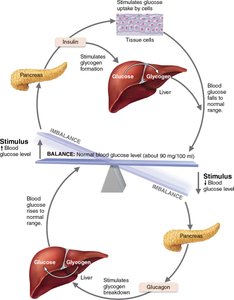
Additional info: Insulin is not required for glucose entry into liver, kidney, or brain cells, but is essential for muscle and adipose tissue.
Homeostatic Imbalance: Diabetes Mellitus and Hyperinsulinism
Diabetes mellitus results from insufficient insulin secretion or action, leading to chronic hyperglycemia. The three cardinal signs are polyuria, polydipsia, and polyphagia. Severe cases may result in ketoacidosis and electrolyte imbalance. Hyperinsulinism, the opposite condition, causes hypoglycemia and can be life-threatening.
Polyuria: Excessive urine output due to osmotic diuresis.
Polydipsia: Excessive thirst from dehydration.
Polyphagia: Excessive hunger due to inability to utilize glucose.
Ketoacidosis: Accumulation of ketone bodies lowers blood pH.
Hyperinsulinism: Causes hypoglycemia, anxiety, and neurological symptoms.
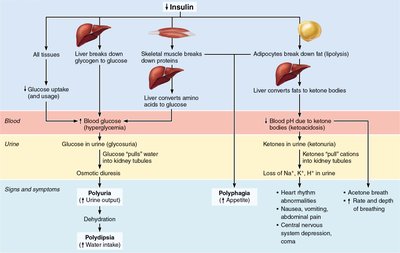
Additional info: Type 1 diabetes is due to autoimmune destruction of beta cells; type 2 diabetes involves insulin resistance.
Clinical Management of Diabetes Mellitus
Type 1 diabetes is managed with insulin therapy, often via injection or infusion pumps. Type 2 diabetes is managed with lifestyle changes, oral medications, and sometimes insulin. Continuous glucose monitoring and artificial pancreas devices are recent advances in diabetes care.
Type 1 diabetes: Autoimmune, requires insulin replacement.
Type 2 diabetes: Insulin resistance, managed with diet, exercise, and medications.
Complications: Vascular, neural, and metabolic issues.
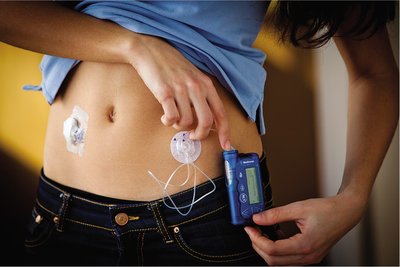
Additional info: Pancreatic islet cell transplants and immunosuppressive therapy are emerging treatments for type 1 diabetes.
Gonads and Placenta: Hormone Production
Gonadal Hormones
The gonads (testes and ovaries) produce steroid sex hormones. Ovaries secrete estrogens and progesterone, which regulate female reproductive development and menstrual cycles. Testes secrete testosterone, which regulates male reproductive development and function.
Estrogens: Promote female secondary sex characteristics and reproductive organ maturation.
Progesterone: Supports pregnancy and menstrual cycle regulation.
Testosterone: Promotes male secondary sex characteristics, sperm production, and sex drive.
Inhibin: Inhibits FSH secretion.
Additional info: Gonadal hormones are regulated by gonadotropins from the anterior pituitary.
Placental Hormones
The placenta is a temporary endocrine organ during pregnancy, producing estrogens, progesterone, and human chorionic gonadotropin (hCG) to sustain fetal development and regulate maternal physiology.
Estrogens and progesterone: Maintain pregnancy and fetal development.
hCG: Supports corpus luteum and early pregnancy.
Additional info: Placental hormones are discussed in detail in reproductive system and pregnancy chapters.
Hormone Secretion by Other Organs
Overview of Non-Endocrine Hormone Sources
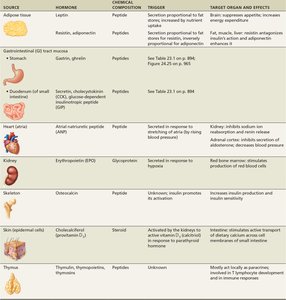
Several organs not traditionally classified as endocrine glands produce hormones that regulate diverse physiological processes. These include adipose tissue, gastrointestinal tract, heart, kidneys, skeleton, skin, and thymus.
Source | Hormone | Chemical Composition | Trigger | Target Organ and Effects |
|---|---|---|---|---|
Adipose Tissue | Leptin, resistin, adiponectin | Peptide | Secretion proportional to fat stores | Regulates appetite, energy expenditure, insulin sensitivity |
GI Tract | Gastrin, ghrelin, secretin, cholecystokinin | Peptide | Food intake, digestive activity | Regulates digestive functions |
Heart | Atrial natriuretic peptide (ANP), brain natriuretic peptide (BNP) | Peptide | Stretch in heart chambers | Reduces blood volume and pressure by promoting sodium excretion |
Kidney | Erythropoietin (EPO), renin | Glycoprotein, enzyme | Low oxygen, low blood pressure | Stimulates red blood cell production, regulates blood pressure |
Skeleton | Osteocalcin | Peptide | Insulin presence | Enhances insulin production, restricts fat storage |
Skin | Cholecalciferol (vitamin D precursor) | Steroid | UV exposure | Regulates calcium absorption, immune function |
Thymus | Thymosins, thymulin, thymopoietins | Peptide | Unknown | Regulates lymphocyte development and immune response |
Additional info: Many hormones produced by these organs act locally as paracrines or autocrines.
Developmental Aspects and Environmental Effects
Development of Endocrine Glands
Endocrine glands arise from all three primary germ layers. Mesoderm-derived glands produce steroid hormones, while others produce amines, peptides, or proteins.
Mesoderm: Steroid hormone production.
Other germ layers: Amine, peptide, or protein hormone production.
Effects of Environmental Pollutants
Exposure to environmental pollutants such as pesticides and industrial chemicals can disrupt endocrine function, particularly affecting sex hormones, thyroid hormone, and glucocorticoids. This disruption may contribute to increased cancer rates and other health issues.
Pollutants: Arsenic, dioxin, pesticides, industrial chemicals.
Vulnerable hormones: Sex hormones, thyroid hormone, glucocorticoids.
Endocrine Function Throughout Life
Most endocrine organs function smoothly until late in life, but aging can alter hormone secretion, breakdown, and receptor sensitivity. Structural changes in glands, such as the anterior pituitary and adrenal glands, may affect hormone production. Gonadal hormone production declines with age, especially in females, leading to menopause and associated health risks.
Anterior pituitary: Increased connective tissue, decreased hormone-secreting cells.
Adrenal glands: Structural changes, persistent cortisol regulation.
Gonads: Ovarian hormone production declines, leading to menopause; testosterone wanes in late life.
Glucose tolerance: Decreases with age, possibly due to reduced insulin receptor sensitivity.
Thyroid: Reduced hormone synthesis and release, decreased basal metabolic rate.
Parathyroid: Little change with age; estrogen protects against bone loss.
Additional info: Estrogen deficiency after menopause increases risk for osteoporosis and atherosclerosis.
Paracrines and Autocrines
Local Chemical Messengers
Paracrines and autocrines are local chemical messengers that act similarly to hormones but affect only nearby cells or the cell that secretes them. Examples include prostaglandins, growth factors, nitric oxide, and cytokines.
Prostaglandins: Involved in inflammation and other local processes.
Growth factors: Regulate cell growth and differentiation.
Nitric oxide: Vasodilation and neurotransmission.
Cytokines: Immune regulation.
Additional info: Paracrines and autocrines are discussed in detail in other chapters.
Key Equations and Concepts
Glucose Regulation Equations
Glycogenolysis:
Gluconeogenesis:
Insulin action:
Additional info: These equations represent the core metabolic pathways regulated by pancreatic hormones.
