 Back
BackEndocrine Regulation of the Gastrointestinal Tract and the Brain-Gut-Microbiota Axis
Study Guide - Smart Notes

Endocrine Function of the Gastrointestinal (GI) Tract
Overview of GI Endocrine Activity
The gastrointestinal tract is not only responsible for digestion and absorption but also acts as the largest endocrine organ in the body. Specialized cells within the GI tract secrete hormones that regulate digestive processes and communicate with other organs and systems.
Enteric Endocrine System: Comprises about 1% of all epithelial cells in the GI tract, producing hormones that act locally (autocrine/paracrine) or systemically (endocrine).
Major Sites: Hormones are produced throughout the GI tract, including the esophagus, stomach, small intestine, and large intestine.
Historical Note: The first recognized hormone, secretin, was discovered in the GI tract.
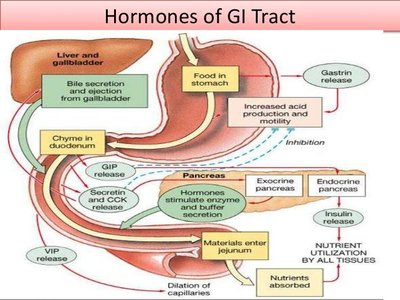
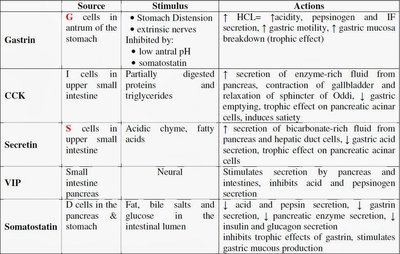
Major Gastrointestinal Hormones
Several key hormones are produced by the GI tract, each with specific sources, stimuli, and actions. These hormones coordinate digestive processes and communicate with other organs.
Hormone | Source | Stimulus | Actions |
|---|---|---|---|
Gastrin | G cells in antrum of the stomach | Stomach distension, extrinsic nerve actions; inhibited by low pH and somatostatin | Increases HCl, pepsinogen, and intrinsic factor secretion; enhances gastric motility; trophic effect on gastric mucosa |
CCK (Cholecystokinin) | I cells in upper small intestine | Partially digested proteins and triglycerides | Stimulates enzyme-rich pancreatic fluid, gallbladder contraction, relaxation of sphincter of Oddi; inhibits gastric emptying |
Secretin | S cells in upper small intestine | Acidic chyme, fatty acids | Stimulates bicarbonate-rich pancreatic and hepatic fluid secretion; inhibits gastric acid secretion |
VIP (Vasoactive Intestinal Peptide) | Small intestine, pancreas | Neural | Stimulates secretion by pancreas and intestines; inhibits acid and pepsin secretion |
Somatostatin | D cells in the pancreas and stomach | Fat, bile salts, glucose in the intestinal lumen | Inhibits acid, pepsin, and gastrin secretion; inhibits trophic effects of gastrin; stimulates gastric mucous production |
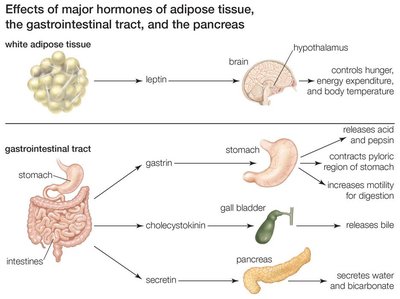
Hormonal Interactions with Other Organs
GI hormones interact with other organs, including the pancreas, gallbladder, and adipose tissue, to coordinate digestion and energy balance.
Leptin: Produced by adipose tissue, signals the brain to regulate hunger, energy expenditure, and body temperature.
Gastrin: Stimulates acid and pepsin secretion in the stomach, increases gastric motility.
Cholecystokinin (CCK): Stimulates gallbladder contraction and pancreatic enzyme secretion.
Secretin: Stimulates pancreatic secretion of water and bicarbonate.
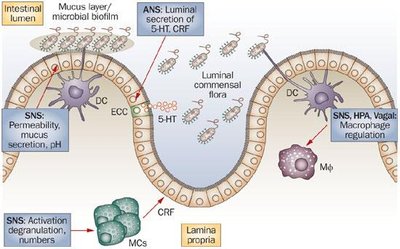
Integration of the Enteric Endocrine System with the Nervous and Immune Systems
Local and Systemic Actions of GI Hormones
GI hormones can act locally within the gut or systemically via the bloodstream. They interact with the enteric nervous system (ENS), central nervous system (CNS), and immune cells to regulate digestive and immune functions.
Autocrine/Paracrine Actions: Hormones act on neighboring cells or the same cell that secreted them.
Endocrine Actions: Hormones enter the bloodstream to affect distant targets.
Neural Integration: The ENS and CNS communicate with GI endocrine cells to modulate secretion and motility.
Brain-Gut Axis and the Role of Microbiota
The brain-gut axis (BGA) is a bidirectional communication system involving the CNS, ENS, endocrine, and immune systems. The intestinal microbiota plays a crucial role in maintaining the integrity of this axis.
Neurohumoral Communication: The brain, via the hypothalamus, pituitary, and adrenal glands, communicates with the gut through neural and hormonal signals.
Microbiota Influence: Gut microbes produce metabolites and signaling molecules that affect gut and brain function.
Functional GI Disorders: Dysregulation of the microbiota-brain-gut axis is implicated in conditions such as irritable bowel syndrome (IBS).
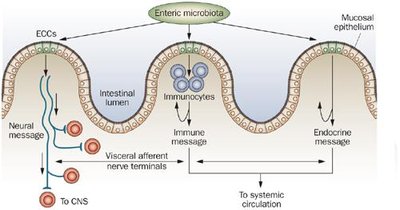
Microbiota-Brain-Gut Axis: Clinical and Functional Implications
Mechanisms of Microbiota Influence
The gut microbiota communicates with the brain and other organs through neural, endocrine, and immune pathways. This interaction affects mood, cognition, immune function, and gastrointestinal health.
Neurotransmitters: Gut microbes can produce or modulate neurotransmitters such as serotonin and short-chain fatty acids (SCFAs).
Immune Modulation: Microbiota influence cytokine production and immune cell activity.
Stress Response: The hypothalamic-pituitary-adrenal (HPA) axis is affected by gut-derived signals, influencing cortisol release and systemic stress responses.
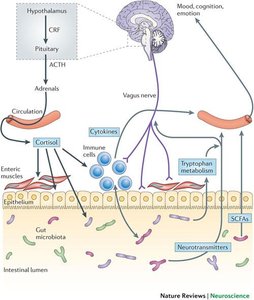
Clinical Relevance of the Microbiota-Brain-Gut Axis
Dysfunction of the microbiota-brain-gut axis is associated with a range of disorders, including functional GI disorders, mood disorders, and metabolic diseases.
Functional GI Disorders (FGIDs): Conditions such as IBS are now considered to involve dysregulation of the microbiota-brain-gut axis.
Systemic Effects: Alterations in the axis are linked to anxiety, depression, obesity, cardiovascular risk, and neurological conditions.
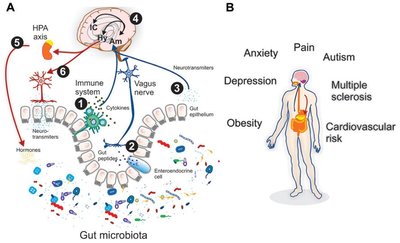
Summary Table: Major GI Hormones and Their Actions
Hormone | Source | Main Actions |
|---|---|---|
Gastrin | Stomach (G cells) | Increases gastric acid secretion, motility |
CCK | Small intestine (I cells) | Stimulates pancreatic enzyme secretion, gallbladder contraction |
Secretin | Small intestine (S cells) | Stimulates bicarbonate secretion from pancreas, inhibits gastric acid |
VIP | Small intestine, pancreas | Stimulates intestinal and pancreatic secretion, inhibits acid secretion |
Somatostatin | Stomach, pancreas (D cells) | Inhibits secretion of many GI hormones, reduces gastric acid |
Key Equations and Concepts
Hormone Secretion Rate: Hormone secretion is regulated by feedback mechanisms involving neural, hormonal, and local signals.
Feedback Regulation: Many GI hormones are regulated by negative feedback loops to maintain homeostasis.
Example Equation: Feedback inhibition of gastrin by low gastric pH:
Additional info: The integration of the GI endocrine system with the nervous and immune systems highlights the complexity of digestive regulation and its impact on overall health. Understanding these interactions is crucial for diagnosing and treating functional GI disorders and related systemic conditions.
