 Back
BackEndocrine System: Hormone Actions, Regulation, and Major Glands
Study Guide - Smart Notes

Endocrine System Overview
Introduction to the Endocrine System
The endocrine system is a network of glands that secrete hormones to regulate and coordinate various physiological processes throughout the body. Hormones are chemical messengers that travel through the bloodstream to target tissues, where they elicit specific responses. The endocrine system works closely with the nervous system but differs in its mechanisms and speed of action.
Endocrine vs. Nervous System: The nervous system uses electrical impulses for rapid, short-term responses, while the endocrine system uses hormones for slower, longer-lasting effects.
Hierarchy of Control: Many endocrine functions are regulated by the central nervous system (CNS), particularly through the hypothalamus and pituitary gland.
Autonomous Glands: Some glands, such as the parathyroid, can respond directly to changes in blood chemistry without CNS input.
Hormone Actions and Mechanisms
Cellular Communication and Hormone Receptors
Hormones exert their effects by binding to specific receptors on or within target cells. The nature of the receptor and the hormone's solubility determine the mechanism of action.
Water-soluble hormones (e.g., insulin, glucagon, epinephrine) bind to cell surface receptors, often activating second messenger systems.
Lipid-soluble hormones (e.g., steroid hormones, thyroid hormones) cross the cell membrane and bind to intracellular receptors, directly influencing gene expression.
Example: Parathyroid hormone (PTH) is released in response to low blood calcium and acts on bones, kidneys, and the gut to restore calcium levels.
G-Protein Coupled Receptors (GPCRs)
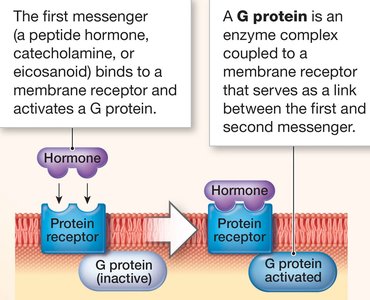
Many water-soluble hormones act through G-protein coupled receptors (GPCRs). When a hormone binds to its receptor, it activates a G protein, which then triggers intracellular signaling cascades.
First Messenger: The hormone itself (e.g., peptide hormone, catecholamine).
Second Messenger: Intracellular molecules (e.g., cAMP, IP3) that propagate the signal.
Intracellular Receptors and Gene Regulation
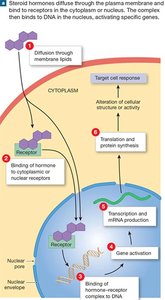
Lipid-soluble hormones, such as steroids and thyroid hormones, diffuse through the plasma membrane and bind to intracellular receptors. The hormone-receptor complex then acts as a transcription factor, altering gene expression and protein synthesis.
Direct gene activation: The hormone-receptor complex binds to DNA, promoting or inhibiting transcription of specific genes.
Longer-lasting effects: Changes in gene expression can have prolonged physiological impacts.
Structural Classes of Hormones
Peptides/Proteins
Peptide and protein hormones are chains of amino acids, typically water-soluble, and do not require carrier proteins in the blood. They have relatively short half-lives and act via membrane receptors.
Short chain polypeptides: e.g., ADH, oxytocin (~9 amino acids)
Small proteins: e.g., insulin, growth hormone (GH), prolactin (50–200 amino acids)
Glycoproteins: e.g., TSH, LH, FSH (200+ amino acids with carbohydrate side chains)
Steroids
Steroid hormones are lipid derivatives, requiring carrier proteins for transport in blood and having longer half-lives. They are derived from cholesterol and include hormones from the adrenal cortex, gonads, and kidneys.
Eicosanoids: Derived from arachidonic acid, act mainly as paracrine signals (e.g., prostaglandins, leukotrienes).
Steroids: e.g., estrogens, androgens, calcitriol, corticosteroids.
Amines
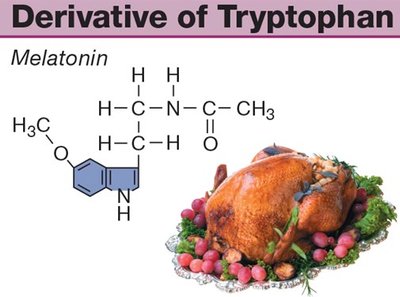
Amines are derived from amino acids (e.g., tyrosine, tryptophan) and can be water- or lipid-soluble. Their properties and mechanisms of action vary accordingly.
Example: Melatonin is derived from tryptophan.
Major Endocrine Glands and Hormonal Control
Hypothalamus and Pituitary Gland
The hypothalamus is a critical link between the nervous and endocrine systems, integrating information from the brain and body to regulate homeostasis. It controls the pituitary gland through both direct and indirect mechanisms.
Direct hormonal control: Hypothalamic hormones (e.g., ADH, oxytocin) are produced in the hypothalamus and released from the posterior pituitary.
Indirect control: Regulatory hormones (releasing/inhibiting factors) are secreted into the hypophyseal portal system to control the anterior pituitary.
Direct neural control: Sympathetic nervous system fibers directly stimulate the adrenal medulla.
Portal Systems
Portal systems are specialized vascular circuits that allow for direct communication between two capillary beds. The hypophyseal portal system connects the hypothalamus to the anterior pituitary, enabling efficient hormone delivery.
Normal circuit: Arteriole → Capillary → Venule
Portal circuit: Arteriole → Capillary 1 → Portal vessel → Capillary 2 → Venule
Anterior and Posterior Pituitary Hormones
The pituitary gland releases several key hormones that regulate other endocrine glands and physiological processes.
Anterior pituitary (Adenohypophysis): FLAT PEG mnemonic:
F: Follicle-stimulating hormone (FSH)
L: Luteinizing hormone (LH)
A: Adrenocorticotropic hormone (ACTH)
T: Thyroid-stimulating hormone (TSH)
P: Prolactin (PRL)
E: Endorphins
G: Growth hormone (GH)
Posterior pituitary (Neurohypophysis): Releases ADH (antidiuretic hormone) and oxytocin, both produced in the hypothalamus.
Feedback Inhibition and Pulsatile Release
Hormone secretion is tightly regulated by negative feedback mechanisms. The hypothalamic-pituitary axes (e.g., HPT, HPA, HPG) use feedback from target gland hormones to modulate further release. Hormones are often released in pulses, allowing for graded physiological control.
Thyroid and Parathyroid Glands
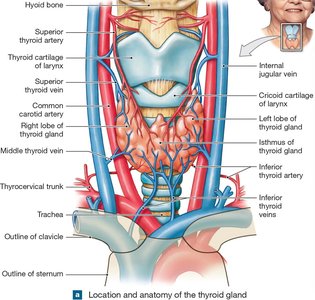
Thyroid Gland
The thyroid gland is located anterior to the larynx and produces thyroid hormones (T3 and T4), which increase basal metabolic rate (BMR) and affect multiple organ systems.
T3 (triiodothyronine): More active form, higher receptor affinity.
T4 (thyroxine): Circulating reservoir, converted to T3 in tissues.
Calcitonin: Produced by C cells, lowers elevated plasma calcium.
Thyroid Hormone Effects
Nervous system: High TH increases anxiety; low TH causes sluggishness.
Cardiovascular: High TH increases heart rate and cardiac output.
Reproductive: Low TH can cause infertility and depressed lactation.
Gastrointestinal: High TH increases motility; low TH causes constipation.
Integumentary: High TH leads to thin, moist skin; low TH causes dry skin.
Thyroid Hormone Regulation
Thyroid hormone release is regulated by the hypothalamic-pituitary-thyroid (HPT) axis:
Hypothalamus releases TRH (thyrotropin-releasing hormone).
Pituitary releases TSH (thyroid-stimulating hormone).
Thyroid releases T3 and T4, which exert feedback inhibition.
Parathyroid Glands and Calcium Homeostasis
The parathyroid glands are embedded in the posterior thyroid and regulate plasma calcium levels by releasing parathyroid hormone (PTH) in response to low calcium.
Kidney response: Increases calcium reabsorption and activates vitamin D.
Gut response: Vitamin D increases intestinal calcium absorption.
Bone response: Stimulates osteoclasts to release calcium from bone.
Example: Primary hyperparathyroidism leads to excessive PTH, increased bone resorption, and hypercalcemia.
Adrenal Glands
Adrenal Cortex and Medulla
The adrenal glands sit atop the kidneys and consist of two functionally distinct regions:
Adrenal cortex: Produces corticosteroids (e.g., cortisol, aldosterone).
Adrenal medulla: Produces catecholamines (epinephrine and norepinephrine) in response to sympathetic stimulation.
Hormonal Effects
Epinephrine: Increases blood glucose, heart rate, and ventilation; redistributes blood to skeletal muscle.
Glucocorticoids (e.g., cortisol): Increase blood glucose, suppress immune function, and are regulated by the HPA axis (CRH → ACTH → cortisol).
Pancreas
Endocrine and Exocrine Functions
The pancreas is both an endocrine and exocrine gland. Its endocrine portion, the islets of Langerhans, regulates blood glucose:
Alpha (α) cells: Secrete glucagon to increase blood glucose.
Beta (β) cells: Secrete insulin to decrease blood glucose and amylin to suppress glucagon and slow gastric emptying.
Delta (δ) cells: Secrete somatostatin to inhibit other hormones.
Summary Table: Major Endocrine Glands, Hormones, and Functions
Gland | Hormones | Main Functions |
|---|---|---|
Hypothalamus | Releasing/inhibiting hormones, ADH, oxytocin | Regulates pituitary, water balance, reproduction |
Pituitary (anterior) | FLAT PEG (FSH, LH, ACTH, TSH, PRL, Endorphins, GH) | Regulates other endocrine glands, growth, lactation |
Pituitary (posterior) | ADH, oxytocin | Water balance, uterine contraction, lactation |
Thyroid | T3, T4, calcitonin | Metabolism, calcium homeostasis |
Parathyroid | PTH | Calcium homeostasis |
Adrenal cortex | Cortisol, aldosterone | Metabolism, stress response, electrolyte balance |
Adrenal medulla | Epinephrine, norepinephrine | Fight-or-flight response |
Pancreas | Insulin, glucagon, somatostatin, amylin | Blood glucose regulation |
