 Back
BackFemale Reproductive System: Structure, Function, and Hormonal Regulation
Study Guide - Smart Notes

Female Reproductive Structures
Main Organs and Functions
The female reproductive system is responsible for producing sex hormones and gametes, supporting the development of the embryo, and nourishing the newborn. The main organs include the ovaries, uterine tubes, uterus, vagina, and external genitalia. Accessory glands such as the urethral glands and greater vestibular gland also play supportive roles.
Ovaries: Produce oocytes, secrete estrogens, progesterone, and inhibin.
Uterine tubes (fallopian tubes): Transport oocytes from the ovaries to the uterus.
Uterus: Provides mechanical protection, nutritional support, and waste removal for the developing embryo and fetus.
Vagina: Serves as the passageway for menstrual fluids, receives sperm, and forms the birth canal.
External genitalia (vulva): Includes the vestibule, labia minora, and clitoris.
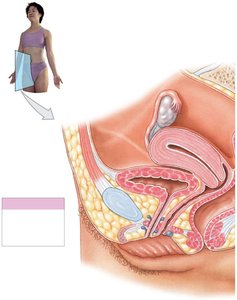
Ovaries
The ovaries are small, almond-shaped organs located near the lateral walls of the pelvic cavity. They are responsible for:
Producing immature female gametes (oocytes)
Secreting female sex hormones (estrogens and progesterone)
Secreting inhibin, which regulates FSH secretion
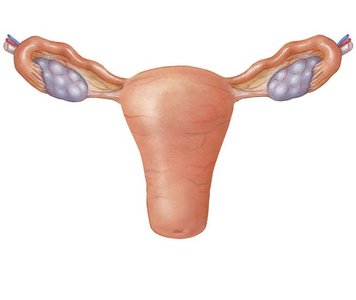
Uterine Tubes
The uterine tubes are hollow, muscular tubes about 13 cm long that transport oocytes to the uterus. They have three segments:
Infundibulum: Expanded funnel near the ovary with fimbriae that help capture the oocyte.
Ampulla: Middle segment where fertilization typically occurs.
Isthmus: Short segment connecting to the uterine wall.
Uterus
The uterus is a pear-shaped organ that provides protection, support, and waste removal for the embryo and fetus. It consists of the uterine body, fundus, and cervix. The uterine wall has three layers:
Perimetrium: Outer serous membrane.
Myometrium: Thick muscular layer responsible for contractions during labor.
Endometrium: Inner glandular layer that undergoes cyclical changes during the uterine cycle.
Vagina and External Genitalia
The vagina is a highly distensible, muscular tube that serves as the passageway for menstrual fluids, receives sperm, and forms the birth canal. The external genitalia, or vulva, includes the vestibule, labia minora, and clitoris.
Mammary Glands
Mammary glands consist of lobes containing secretory lobules. Ducts from these lobules converge to form lactiferous ducts, which open at the nipple. These glands are responsible for milk production and secretion.
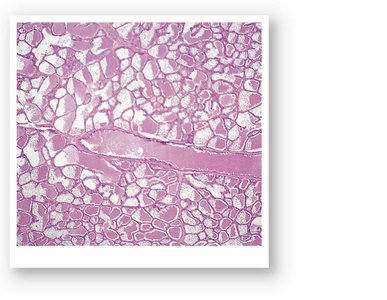
Female Reproductive Functions
Oogenesis
Oogenesis is the process of ovum (egg) production. It begins before birth, accelerates at puberty, and ends at menopause. Oogonia undergo mitosis to produce primary oocytes, which remain in suspended development until puberty.
At birth: ~2 million primary oocytes are present; most degenerate (atresia).
By puberty: ~400,000 primary oocytes remain.
Each month, some primary oocytes complete meiosis I to form secondary oocytes and polar bodies.
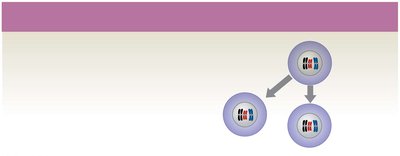
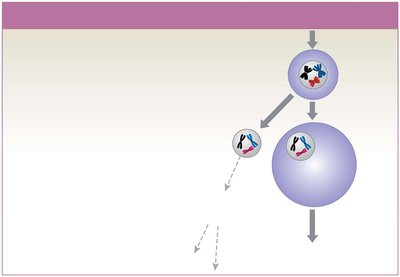
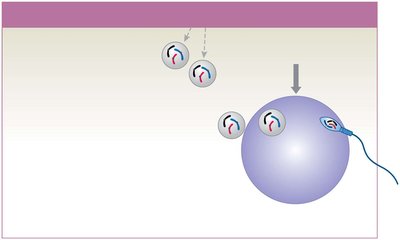
Ovarian Follicles and Cycle
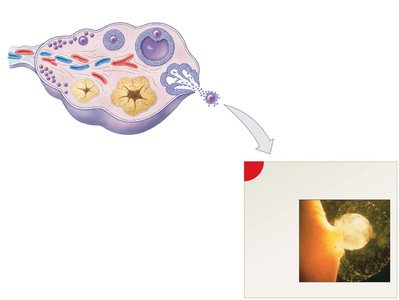
Ovarian follicles are specialized structures where oocyte growth and meiosis I occur. The ovarian cycle consists of the follicular phase (maturation of follicles), ovulation (release of secondary oocyte), and luteal phase (formation and degeneration of corpus luteum).
Primordial follicle: Primary oocyte + follicle cells
Primary follicle: Activated primordial follicle
Secondary follicle: Forms from primary follicle
Tertiary follicle: Large, fluid-filled follicle ready for ovulation
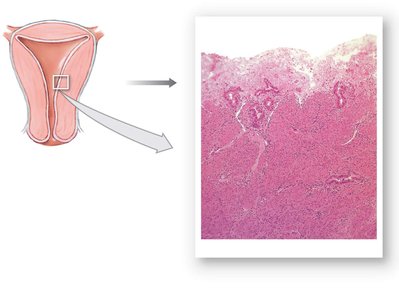
Uterine (Menstrual) Cycle
The uterine cycle is a repeating series of changes in the endometrium, typically lasting 28 days. It consists of three phases:
Menstrual phase: Shedding of the functional layer of the endometrium (menses).
Proliferative phase: Regeneration and thickening of the endometrium, stimulated by estrogens.
Secretory phase: Enlargement of uterine glands and increased secretion, driven by progesterone from the corpus luteum.
Hormonal Regulation of the Female Reproductive Cycle
Hormonal Control
The female reproductive cycle is regulated by hormones from the hypothalamus, pituitary gland, and ovaries. GnRH from the hypothalamus stimulates FSH and LH release from the anterior pituitary, which in turn regulate ovarian and uterine cycles.
FSH: Stimulates follicular development
LH: Triggers ovulation and corpus luteum formation
Estrogens: Stimulate endometrial growth, secondary sex characteristics
Progesterone: Prepares endometrium for implantation, maintains pregnancy
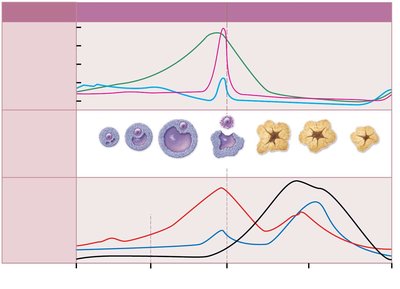
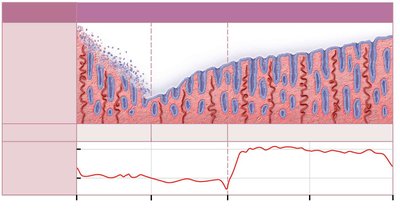
Hormonal Regulation of Uterine Cycle
Estrogen and progesterone levels fluctuate throughout the cycle, causing changes in the endometrium. Menstruation occurs when hormone levels drop, and the proliferative phase begins as estrogen rises. The secretory phase is initiated by progesterone.
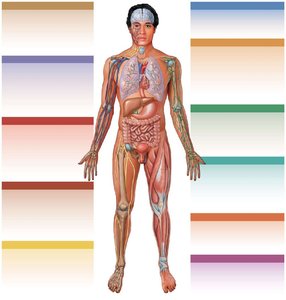
Integration with Other Body Systems
The female reproductive system interacts with multiple organ systems, including the integumentary, nervous, endocrine, respiratory, lymphatic, cardiovascular, urinary, digestive, muscular, and skeletal systems. These interactions are essential for reproductive health, sexual function, and successful pregnancy.
Changes in Reproductive Function and Aging
Menopause and Perimenopause
Menopause marks the end of ovulation and menstruation, typically occurring between ages 45–55. Perimenopause is the transitional period before menopause, characterized by irregular cycles and declining estrogen levels. Effects include reduced size of reproductive organs, thinning of vaginal epithelium, and decreased bone deposition.
Male Climacteric (Andropause)
In males, reproductive function declines gradually with age, with decreased testosterone and increased FSH and LH. Sperm production continues, but sexual activity may decrease.
Summary Table: Key Hormones and Their Functions
Hormone | Source | Main Functions |
|---|---|---|
GnRH | Hypothalamus | Stimulates FSH and LH release |
FSH | Anterior pituitary | Stimulates follicle development |
LH | Anterior pituitary | Triggers ovulation, corpus luteum formation |
Estrogens | Ovarian follicles | Stimulate endometrial growth, secondary sex characteristics |
Progesterone | Corpus luteum | Prepares endometrium for implantation, maintains pregnancy |
Inhibin | Ovarian follicles | Inhibits FSH secretion |
