 Back
BackHuman Development and Heredity: Structured Study Notes for Anatomy & Physiology
Study Guide - Smart Notes

Chapter 27: Development and Heredity
Overview of Human Development
Human development begins at fertilization and continues throughout life, encompassing both prenatal and postnatal periods. Developmental biology studies these changes, while embryology focuses on the prenatal period (about 38 weeks in utero). The postnatal period extends from birth through all life stages.
Prenatal Period: Divided into pre-embryonic, embryonic, and fetal stages.
Postnatal Period: Includes neonatal, infancy, childhood, adolescence, and adulthood (maturity).
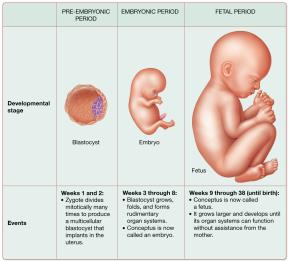
The Process of Prenatal Development
Pre-Embryonic Period (Weeks 1–2): Begins with fertilization, formation of the zygote, and ends with implantation of the blastocyst.
Embryonic Period (Weeks 3–8): Formation of rudimentary organ systems; the conceptus is now called an embryo.
Fetal Period (Weeks 9–38): Growth and maturation of organ systems; the conceptus is now called a fetus.
Infertility and Assisted Reproductive Technology (ART)
Infertility is the inability to achieve pregnancy after one year of unprotected intercourse. ART involves direct manipulation of the reproductive process to treat infertility.
Common ART Methods:
Intrauterine Insemination (IUI): Sperm placed directly into the uterus.
Gamete Intrafallopian Transfer (GIFT): Sperm and oocytes placed into the uterine tube.
Zygote Intrafallopian Transfer (ZIFT): Zygote placed into the uterine tube.
In Vitro Fertilization (IVF): Fertilization occurs outside the body; pre-embryonic stages completed before transfer to the uterus.
Prenatal Development: Cellular and Molecular Events
Fertilization
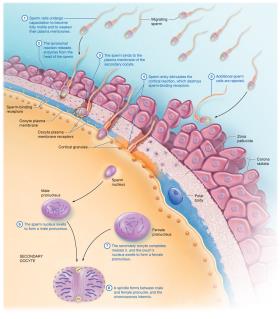
Fertilization is the union of haploid gametes (sperm and secondary oocyte) to form a diploid zygote. Sperm must undergo capacitation and the acrosomal reaction to penetrate the oocyte's protective layers.
Capacitation: Functional changes in sperm to allow fusion with the oocyte.
Acrosomal Reaction: Release of enzymes to penetrate the corona radiata and zona pellucida.
Cortical Reaction: Prevents polyspermy by destroying sperm-binding receptors.
Amphimixis: Fusion of male and female pronuclei to form the zygote.
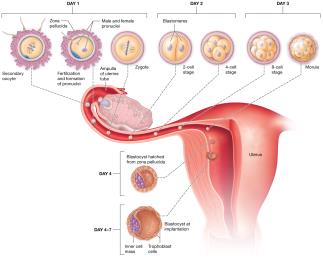
Cleavage and Blastocyst Formation
Cleavage is a series of rapid mitotic divisions producing smaller cells (blastomeres). By day 3, the morula forms, and by day 4–5, the blastocyst forms and enters the uterine cavity.
Blastocyst: Outer trophoblast (forms placenta) and inner cell mass (forms embryo).
Monozygotic Twins: Result from separation of blastomeres within 8 days.
Dizygotic Twins: Result from fertilization of two oocytes.
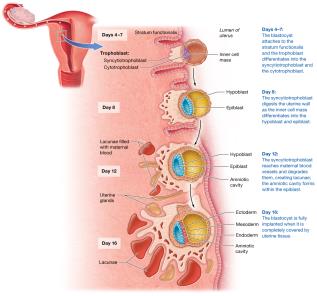
Implantation
Implantation occurs 4–7 days after fertilization when the blastocyst attaches to and invades the endometrium. The trophoblast differentiates into cytotrophoblast and syncytiotrophoblast, which secretes hCG to maintain the corpus luteum.
hCG: Basis for pregnancy tests; maintains uterine lining.
Ectopic Pregnancy: Implantation outside the uterus, most commonly in the uterine tube.
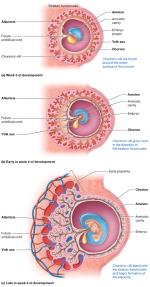
Development of the Extraembryonic Membranes
Four extraembryonic membranes form to support the conceptus: yolk sac, amnion, allantois, and chorion.
Yolk Sac: Source of first blood cells and germ cells.
Amnion: Encloses the embryo in amniotic fluid for protection.
Allantois: Forms the base of the umbilical cord and part of the urinary bladder.
Chorion: Outermost membrane; forms chorionic villi and the main embryonic part of the placenta.
Extraembryonic Membrane | Primary Functions |
|---|---|
Yolk sac | Forms digestive tract, first blood cells/vessels, germ cells |
Amnion | Surrounds conceptus, produces amniotic fluid for protection |
Allantois | Base for umbilical cord, becomes part of urinary bladder |
Chorion | Encloses other membranes, forms chorionic villi and placenta |
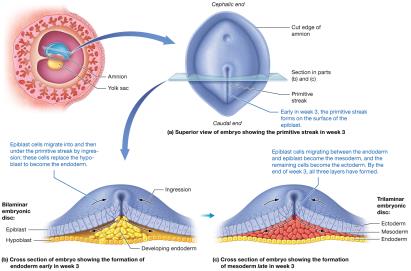
Formation of the Germ Layers (Gastrulation)
During week 3, the bilaminar embryonic disc becomes trilaminar through gastrulation, forming the ectoderm, mesoderm, and endoderm. These germ layers give rise to all tissues and organs.
Primitive Streak: Establishes body axes and initiates cell migration.
Ingression: Movement of cells to form germ layers.
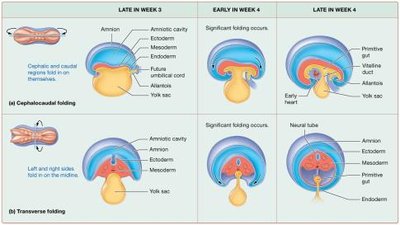
Embryonic Folding and Organogenesis
By week 4, cephalocaudal and transverse folding transform the flat embryonic disc into a cylindrical embryo, establishing the basic body plan and primitive gut.
Cephalocaudal Folding: Forms head and buttocks regions.
Transverse Folding: Forms trunk and primitive gut.
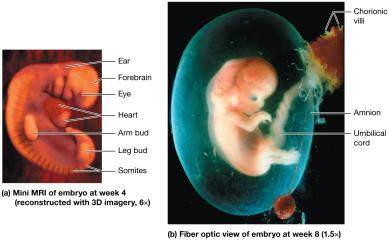
Organogenesis
Organogenesis is the differentiation of the three germ layers into organs and organ systems. By week 8, the embryo has recognizable organ systems.
Ectoderm: Forms epidermis, nervous system, sense organs.
Mesoderm: Forms skeleton, muscle, cardiovascular system, kidneys, gonads.
Endoderm: Forms epithelial lining of digestive, respiratory, urinary, and reproductive tracts.
Layer | Major Structures |
|---|---|
Ectoderm | Nervous system, epidermis, sense organs |
Mesoderm | Skeleton, muscle, cardiovascular system, kidneys, gonads |
Endoderm | Digestive, respiratory, urinary, reproductive tract linings |
Teratogens
Teratogens are substances that cause congenital disorders or death, especially harmful during the embryonic period. Examples include infectious agents (rubella), alcohol, nicotine, certain drugs, and chemicals like thalidomide.
Placentation and Fetal Development
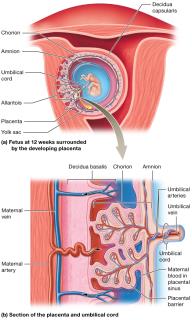
Placentation
The placenta forms as a temporary organ for exchange of nutrients, gases, and wastes between mother and fetus. It also produces hormones to support pregnancy.
Umbilical Cord: Contains two arteries (deoxygenated blood) and one vein (oxygenated blood), protected by Wharton's jelly.
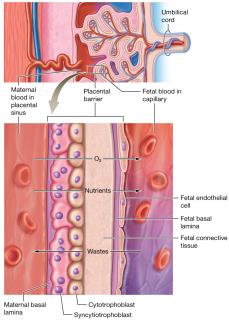
Placental Barrier: Separates maternal and fetal blood; exchange occurs by diffusion.
Fetal Development
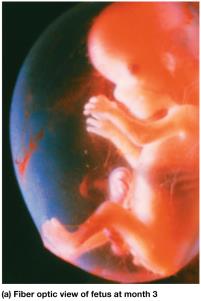
The fetal period is marked by rapid growth and maturation of tissues and organs. Major events are summarized by month.
Month 3: Body lengthens, ossification begins, genitals distinguishable.
Month 4: Rapid growth, joints form, heartbeat audible.
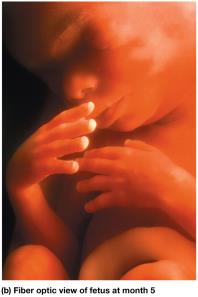
Month 5: Hair (lanugo) and vernix caseosa develop, mother feels movement (quickening).
Month 6–9: Organs mature, fat accumulates, lungs produce surfactant, fetus assumes vertex position.
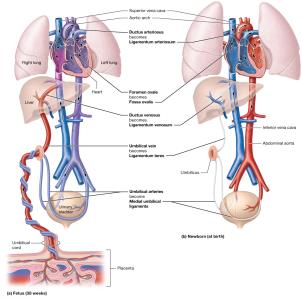
Fetal Circulation
Fetal circulation includes unique structures that bypass nonfunctional fetal lungs and liver. After birth, these shunts close and normal circulation is established.
Ductus Venosus: Bypasses fetal liver.
Foramen Ovale: Shunts blood from right to left atrium.
Ductus Arteriosus: Connects pulmonary trunk to aorta.
Maternal Changes During Pregnancy
Trimesters and Hormonal Changes
Pregnancy is divided into three trimesters, each with distinct developmental milestones and maternal symptoms. Hormonal changes support pregnancy and prepare the body for childbirth and lactation.
hCG: Maintains corpus luteum early in pregnancy.
Estrogens and Progesterone: Maintain uterine lining, suppress ovarian cycle.
Relaxin, hPL, MSH, CRH, Prolactin, Oxytocin, Aldosterone, PTH: Various roles in supporting pregnancy, fetal development, and lactation.
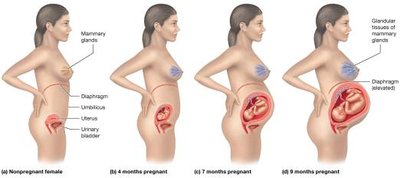
Anatomical and Physiological Changes
Reproductive System: Uterus enlarges, mammary glands develop.
Cardiovascular System: Blood volume and cardiac output increase; risk of varicose veins and edema.
Respiratory System: Increased ventilation, nasal congestion.
Digestive System: Increased caloric needs, morning sickness, constipation.
Urinary System: Increased GFR, frequent urination, stress incontinence.
Integumentary System: Pigmentation changes, stretch marks, thicker hair.
Parturition (Labor and Delivery)
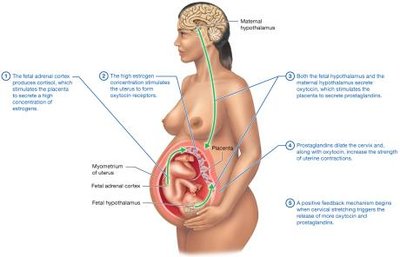
Initiation and Stages of Labor
Labor is initiated by hormonal signals from the fetus and mother, involving a positive feedback loop of oxytocin and prostaglandins. Labor consists of dilation, expulsion, and placental stages.
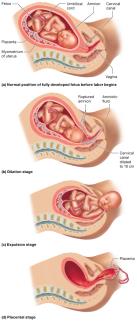
Dilation Stage: Cervix dilates to 10 cm; amniotic sac ruptures.
Expulsion Stage: Delivery of the newborn; crowning and possible episiotomy.
Placental Stage: Delivery of the placenta (afterbirth).
Neonatal and Maternal Changes After Birth
Neonatal Period
The first 4 weeks after birth are critical for adaptation to extrauterine life. The Apgar score assesses newborn health based on five criteria: skin color, pulse, respiration, muscle activity, and reflexes.
Circulatory Changes: Closure of fetal shunts and establishment of normal circulation.
Thermoregulation: Brown adipose tissue helps maintain body temperature.
Immunity: Passive IgG from placenta; IgA from colostrum in breast milk.
Maternal Changes (Postpartum Period and Lactation)
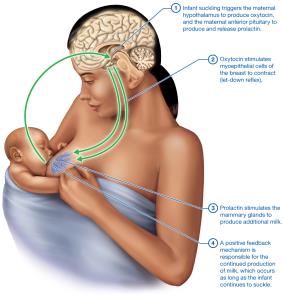
After birth, maternal hormone levels drop, and physiological systems return to pre-pregnancy states. Lactation is regulated by prolactin and oxytocin in a positive feedback loop.
Colostrum: First milk, rich in antibodies.
Let-Down Reflex: Oxytocin-mediated milk ejection.
Heredity and Patterns of Inheritance
Genes, Alleles, and Chromosomes
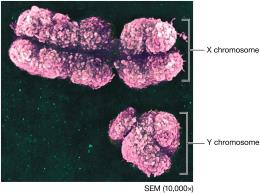
Genes are DNA segments coding for proteins; alleles are variants of a gene. The human genome consists of about 20,000 genes on 46 chromosomes (23 pairs: 22 autosomes, 1 pair sex chromosomes).
Genotype: Genetic makeup.
Phenotype: Physical expression of genotype.
Patterns of Inheritance
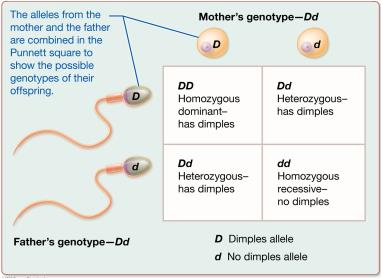
Autosomal Dominant-Recessive: Traits determined by dominant or recessive alleles (e.g., dimples).
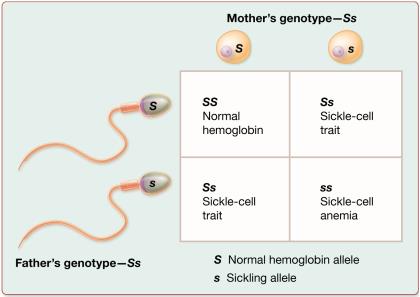
Incomplete Dominance: Heterozygotes show intermediate phenotype (e.g., sickle-cell trait).
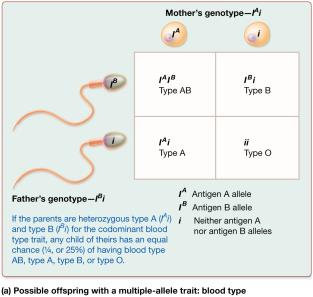
Multiple-Allele Traits: Traits influenced by more than two alleles (e.g., ABO blood group).
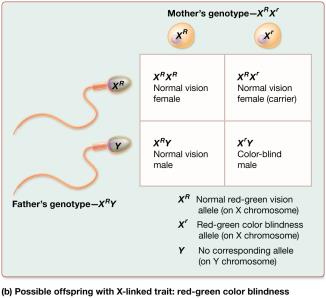
Sex-Linked Traits: Traits on X or Y chromosomes (e.g., color blindness, hemophilia).
Polygenic Inheritance: Traits controlled by multiple genes (e.g., height, skin color).
Multifactorial Inheritance: Traits influenced by genes and environment.
Genotype | Phenotype |
|---|---|
I^A I^A | Blood type A |
I^A i | Blood type A |
I^B I^B | Blood type B |
I^B i | Blood type B |
I^A I^B | Blood type AB |
ii | Blood type O |
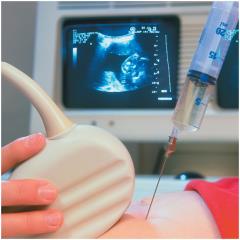
Prenatal and Newborn Genetic Screening
Genetic disorders can be detected prenatally by amniocentesis or chorionic villus sampling, and newborns are screened for metabolic and genetic disorders to allow early intervention.
Additional info: These notes provide a comprehensive overview of human development and heredity, integrating key concepts, definitions, and clinical applications relevant to anatomy and physiology students.
