 Back
BackHuman Reproductive System and Development: ANP College Study Notes
Study Guide - Smart Notes

Reproductive System Overview
Introduction to Human Reproduction
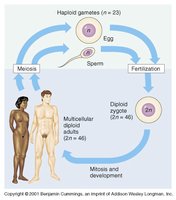
The human reproductive system ensures the continuation of the species by producing haploid gametes, facilitating fertilization, and supporting the development of the next generation. Both male and female systems share the fundamental process of gamete production but differ significantly in structure and function.
Haploid gametes (n = 23) are produced by meiosis in both males (sperm) and females (egg).
Fertilization restores the diploid state (2n = 46), forming a zygote that develops into a multicellular adult.
Sex Determination and Differentiation
Genetic Sex Determination
Sex is determined at fertilization by the combination of sex chromosomes. The presence or absence of the Y chromosome, specifically the SRY gene, directs the development of male or female gonads.
XX = Female; XY = Male
The SRY gene on the Y chromosome triggers testes development; absence leads to ovary formation.
Development of Internal Reproductive Structures
During early embryogenesis, both Wolffian (mesonephric) and Mullerian (paramesonephric) ducts are present. Hormonal signals determine which duct system develops:
Testosterone (from testes) promotes Wolffian duct development into male internal structures (epididymis, vas deferens, ejaculatory ducts).
Mullerian Inhibiting Factor (MIF) causes regression of Mullerian ducts in males.
In females, absence of testosterone allows Mullerian ducts to form the uterus and fallopian tubes.
Development of External Genitalia
Both sexes start with undifferentiated external structures. Testosterone presence leads to male differentiation; absence results in female structures.
Male Reproductive System
Anatomy of the Male Reproductive System
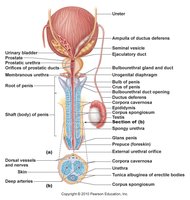
The male reproductive system is specialized for the production, maturation, and delivery of sperm. The primary sex organs are the testes, which produce sperm and secrete testosterone.
Testes: Site of spermatogenesis and testosterone production.
Epididymis: Sperm storage and maturation.
Vas deferens: Transports sperm to the ejaculatory duct.
Accessory glands: Seminal vesicles, prostate, and bulbourethral glands contribute fluids to semen.
Penis: Copulatory organ for sperm delivery.
Spermatogenesis
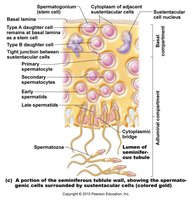
Spermatogenesis is the process of sperm production in the seminiferous tubules of the testes. It involves mitosis, meiosis, and spermiogenesis (maturation of spermatids into spermatozoa).
Spermatogonia (stem cells) divide by mitosis; one remains a stem cell, the other becomes a primary spermatocyte.
Primary spermatocytes undergo meiosis I to form secondary spermatocytes (haploid).
Secondary spermatocytes undergo meiosis II to form spermatids.
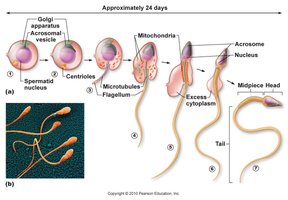
Spermiogenesis: Spermatids mature into spermatozoa with a head, midpiece, and tail.
Hormonal Regulation of Male Reproduction
The hypothalamic-pituitary-gonadal axis regulates spermatogenesis and testosterone production:
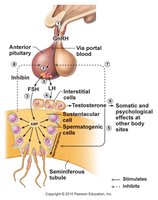
GnRH (hypothalamus) stimulates the anterior pituitary to release FSH and LH.
FSH: Stimulates Sertoli cells and spermatogenesis.
LH: Stimulates Leydig cells to produce testosterone.
Testosterone: Supports spermatogenesis and secondary sex characteristics; negative feedback on GnRH and LH.
Inhibin: Inhibits FSH release.
Female Reproductive System
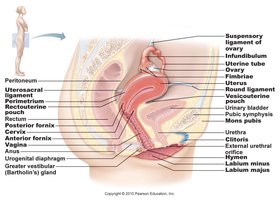
Anatomy of the Female Reproductive System
The female reproductive system is designed for the production of ova, reception of sperm, fertilization, and support of fetal development. The primary sex organs are the ovaries.
Ovaries: Produce ova and secrete estrogen and progesterone.
Fallopian tubes: Site of fertilization; transport ova to uterus.
Uterus: Site of implantation and fetal development.
Vagina: Receives sperm and serves as the birth canal.
Mammary glands: Milk production.
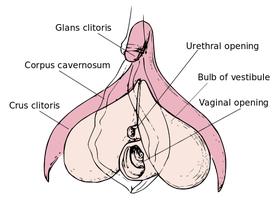
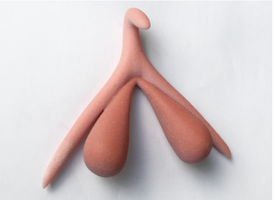
The Clitoris
The clitoris is a highly innervated erectile structure, homologous to the male penis, and plays a key role in female sexual response.
Oogenesis and Follicular Development
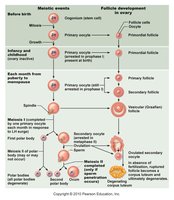
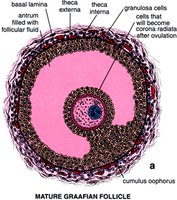
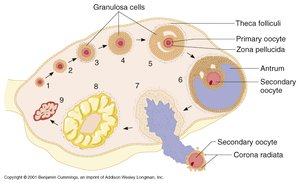
Oogenesis is the process of ovum formation, beginning before birth and continuing through the reproductive years. Each cycle, one oocyte completes meiosis and is ovulated.
Oogonia divide by mitosis during fetal development, then become primary oocytes arrested in prophase I.
At puberty, primary oocytes resume meiosis; one dominant follicle completes meiosis I each cycle, forming a secondary oocyte and a polar body.
Secondary oocyte is ovulated and arrested in metaphase II; meiosis II completes only if fertilization occurs.

Hormonal Regulation and the Menstrual Cycle
The menstrual cycle is regulated by the interplay of pituitary and ovarian hormones, resulting in cyclical changes in the ovaries (ovarian cycle) and uterus (uterine cycle).
FSH: Stimulates follicle growth.
Estrogen: Promotes endometrial proliferation; peak triggers LH surge.
LH: Triggers ovulation and corpus luteum formation.
Progesterone: Maintains endometrium for implantation.
Fertilization and Early Development
Fertilization
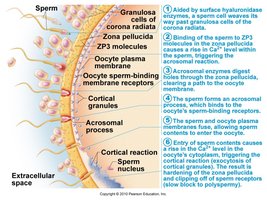
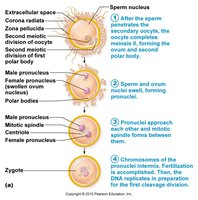
Fertilization occurs when a capacitated sperm penetrates the secondary oocyte, restoring the diploid chromosome number and forming a zygote.
Capacitation: Sperm undergoes changes in the female tract to become capable of fertilizing the egg.
Acrosomal reaction: Enzymes from the sperm head digest the zona pellucida, allowing sperm entry.
Blocks to polyspermy: Fast (membrane depolarization) and slow (cortical reaction) blocks prevent entry of additional sperm.

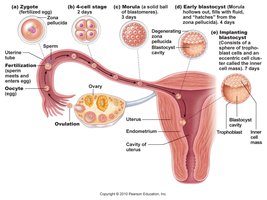
Cleavage, Blastocyst Formation, and Implantation
After fertilization, the zygote undergoes rapid mitotic divisions (cleavage), forming a morula and then a blastocyst, which implants in the uterine wall.
Cleavage: Rapid cell divisions without growth.
Morula: Solid ball of cells.
Blastocyst: Hollow ball with inner cell mass (embryo) and trophoblast (placenta).
Implantation: Blastocyst embeds in endometrium, trophoblast forms extraembryonic membranes.
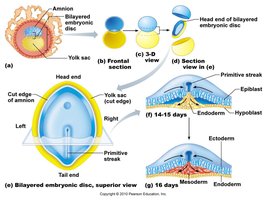
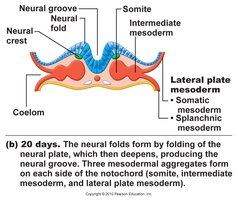
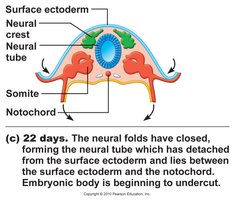
Gastrulation and Neurulation
Gastrulation forms the three primary germ layers (ectoderm, mesoderm, endoderm), which give rise to all tissues and organs. Neurulation forms the neural tube, precursor to the central nervous system.
Ectoderm: Skin, nervous system.
Mesoderm: Muscle, bone, blood, urogenital organs.
Endoderm: Gut lining, respiratory tract, glands.
Placenta and Fetal Circulation
Placenta and Extraembryonic Membranes
The placenta forms from fetal (chorion) and maternal tissues, facilitating nutrient and gas exchange. Extraembryonic membranes include the amnion, yolk sac, allantois, and chorion.
Fetal Circulatory Adaptations
Fetal circulation includes shunts (foramen ovale, ductus arteriosus, ductus venosus) that bypass nonfunctional fetal lungs and liver. At birth, these shunts close as the newborn transitions to independent life.
Parturition (Birth) and Neonatal Adaptations
Labor and Delivery
Labor is initiated by hormonal signals from the fetus and placenta, leading to uterine contractions and birth. It consists of dilation, expulsion, and placental stages.
Neonatal Circulatory Changes
Closure of fetal shunts and establishment of pulmonary circulation are critical for newborn survival.
Summary Table: Comparison of Spermatogenesis and Oogenesis
Feature | Spermatogenesis | Oogenesis |
|---|---|---|
Location | Seminiferous tubules (testes) | Ovarian follicles (ovaries) |
Timing | Puberty to old age | Begins before birth, continues to menopause |
Number of gametes per precursor | 4 sperm per spermatogonium | 1 ovum + 2-3 polar bodies per oogonium |
Completion of meiosis II | Before fertilization | Only if fertilization occurs |
