 Back
BackLab Exam Review 3: Digestive, Urinary, and Respiratory Systems
Study Guide - Smart Notes

Digestive, Urinary, and Respiratory Systems: Lab Exam Review
Organs of the Digestive, Urinary, and Respiratory Systems
The human body contains several organ systems essential for maintaining homeostasis, including the digestive, urinary, and respiratory systems. Each system is composed of specialized organs with distinct anatomical and physiological roles.
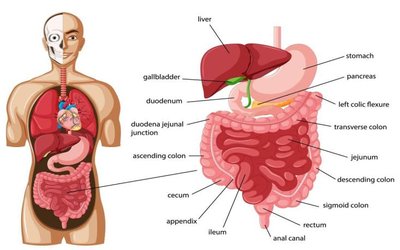
Digestive System: Includes the mouth, pharynx, esophagus, stomach, small intestine, large intestine, rectum, anus, and accessory organs (liver, gallbladder, pancreas).
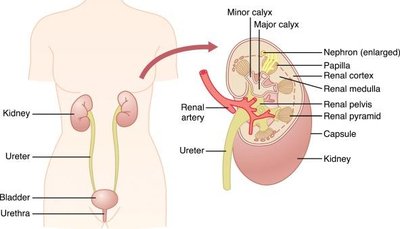
Urinary System: Composed of the kidneys, ureters, urinary bladder, and urethra.
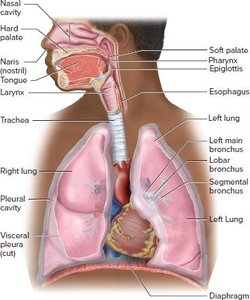
Respiratory System: Consists of the nasal cavity, pharynx, larynx, trachea, bronchi, and lungs.
Anatomy of the Lungs
Pulmonary Tree and Gas Exchange
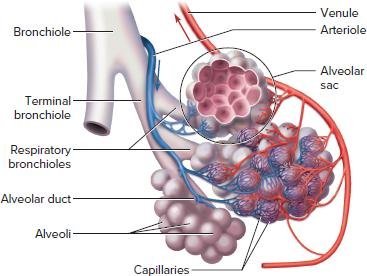
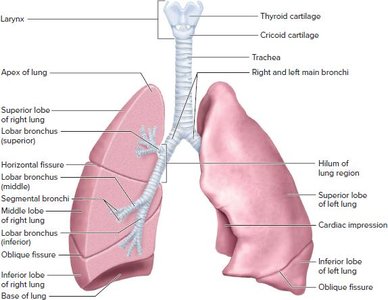
The lungs are essential for respiration, facilitating the exchange of oxygen and carbon dioxide. The pulmonary tree describes the branching airway system within the lungs, from the trachea to the alveoli, where gas exchange occurs.
Trachea: Main airway leading to the bronchi.
Bronchi: Branch into smaller bronchioles within the lungs.
Bronchioles: Further divide into terminal and respiratory bronchioles.
Alveolar Ducts and Alveoli: Terminal ends where gas exchange occurs across the respiratory membrane.
Anatomy of the Stomach
Structure and Function
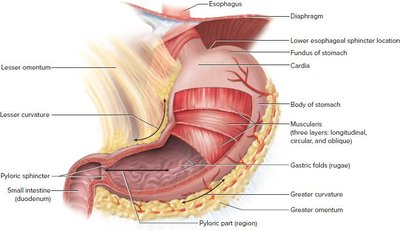
The stomach is a J-shaped organ that serves as a major site for mechanical and chemical digestion. It stores food, mixes it with gastric secretions, and regulates its passage into the small intestine.
Regions: Cardia, fundus, body, pylorus.
Muscularis: Three layers (longitudinal, circular, oblique) for churning food.
Sphincters: Lower esophageal (cardiac) sphincter and pyloric sphincter regulate entry and exit of stomach contents.
Functions of the Digestive and Urinary Systems
Digestive System Functions
Ingestion: Intake of food.
Propulsion: Movement of food through the tract (e.g., peristalsis).
Mechanical Digestion: Physical breakdown (chewing, churning).
Chemical Digestion: Enzymatic breakdown of macromolecules.
Absorption: Uptake of nutrients into blood or lymph.
Defecation: Elimination of indigestible substances.
Urinary System Functions
Filtration of Blood: Removal of wastes and excess fluid.
Urine Production: Concentration of waste into urine.
Regulation of Blood Volume and Pressure: Adjusting fluid levels.
Electrolyte Balance: Maintaining ion concentrations (Na+, K+).
Blood pH Regulation: Acid-base balance.
Excretion: Removal of metabolic wastes (urea, uric acid).
Functions of Various Digestive Organs
Mouth: Chewing, carbohydrate digestion (salivary amylase), lubrication.
Pharynx & Esophagus: Propulsion via peristalsis.
Stomach: Churning, protein digestion (pepsin), food storage, chyme production.
Small Intestine: Main site for digestion and absorption; receives enzymes and bile.
Large Intestine: Absorbs water/electrolytes, forms feces, houses gut bacteria.
Rectum & Anus: Storage and elimination of feces.
Liver: Produces bile, processes nutrients, detoxifies.
Gallbladder: Stores/concentrates bile.
Pancreas: Produces digestive enzymes and bicarbonate.
Functions of Urinary Organs
Kidneys: Filter blood, produce urine, regulate blood pressure, electrolyte balance, and erythropoiesis.
Ureters: Transport urine to bladder.
Urinary Bladder: Stores urine.
Urethra: Conducts urine out of the body.
Histology of the Wall of the Digestive Canal
General Structure
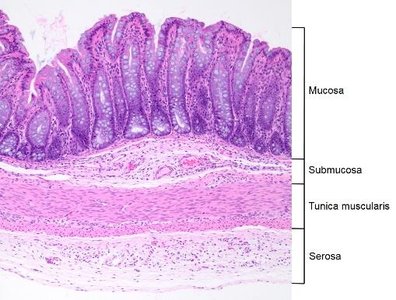
The digestive canal (alimentary canal) from the esophagus to the large intestine consists of four main layers (tunics):
Mucosa: Innermost layer; epithelium, lamina propria, muscularis mucosae. Functions in secretion, absorption, and protection.
Submucosa: Connective tissue with blood vessels, nerves, and glands.
Muscularis Externa: Smooth muscle (usually two layers) for peristalsis and segmentation.
Serosa (or Adventitia): Outermost layer; connective tissue covering.
Cells in the Wall of the Stomach and Their Secretions
Gastric Gland Cell Types
Mucous Neck Cells: Secrete alkaline mucus to protect the stomach lining.
Parietal Cells: Secrete hydrochloric acid (HCl) and intrinsic factor (for vitamin B12 absorption).
Chief Cells: Secrete pepsinogen (inactive), which is activated to pepsin by HCl for protein digestion.
Enteroendocrine Cells (e.g., G cells): Secrete hormones such as gastrin, stimulating acid secretion and motility.
Fluid Secretions and Reabsorption in the Digestive Tract
Role of Water
Secretions: Saliva, gastric juice, pancreatic juice, bile, and intestinal juice contain water, serving as a solvent and medium for digestion.
Reabsorption: Most water is reabsorbed in the small intestine (80-90%), with the large intestine absorbing most of the remainder, concentrating feces.
Osmotic Gradients: Water movement is driven by osmotic gradients created by solute absorption.
Sphincters Along the Digestive Tract
Major Digestive Sphincters
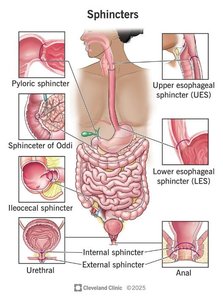
Sphincters are muscular rings that regulate the passage of contents and prevent backflow in the digestive tract.
Upper Esophageal Sphincter: Prevents air entry and reflux into the pharynx.
Lower Esophageal (Cardiac) Sphincter: Prevents reflux of stomach contents into the esophagus.
Pyloric Sphincter: Controls passage of chyme into the duodenum.
Hepatopancreatic (Sphincter of Oddi): Regulates bile and pancreatic juice entry into the duodenum.
Ileocecal Valve: Controls flow from ileum to cecum, prevents backflow.
Anal Sphincters (Internal/External): Control defecation.
Renal Capsule: Structure and Function
Protective Layer of the Kidney
Structure: Tough, fibrous connective tissue layer surrounding the kidney.
Function: Protects against trauma/infection, maintains kidney shape, prevents excessive swelling.
Order of Urine Flow: Collecting Duct to Urethra
Pathway of Urine
Collecting Duct
Renal Pelvis
Ureter
Bladder
Urethra
Order of Filtrate Flow: Bowman's Capsule to Minor Calyx
Bowman's Capsule
Proximal Convoluted Tubule (PCT)
Loop of Henle (descending and ascending limbs)
Distal Convoluted Tubule (DCT)
Collecting Duct
Papillary Duct
Minor Calyx
Types of Nephrons in the Kidney
Cortical vs. Juxtamedullary Nephrons
Cortical Nephrons: Located in the renal cortex, short loops of Henle, ~85% of nephrons, main function is filtration and reabsorption.
Juxtamedullary Nephrons: Located near the corticomedullary junction, long loops of Henle extending into the medulla, ~15% of nephrons, crucial for urine concentration and water conservation.
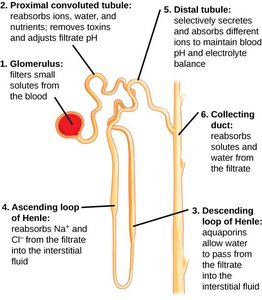
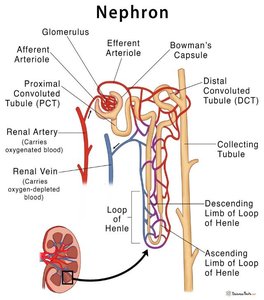
Parts and Structures of the Nephron
Renal Corpuscle: Includes the glomerulus (capillary network for filtration) and Bowman's capsule (collects filtrate).
Renal Tubule: Proximal convoluted tubule (reabsorption), loop of Henle (osmotic gradient), distal convoluted tubule (secretion/reabsorption).
Collecting Duct: Receives fluid from multiple nephrons, final urine concentration.
Functions of Bile
Role in Digestion and Excretion
Emulsification of Fats: Breaks large fat globules into smaller droplets for enzyme action.
Absorption: Facilitates absorption of fatty acids and fat-soluble vitamins (A, D, E, K).
Excretion: Removes waste products (bilirubin, cholesterol) from the body via feces.
