 Back
BackCh 9Muscles and Muscle Tissue: Structure, Function, and Physiology
Study Guide - Smart Notes

Muscle Tissue Types
Overview of Muscle Tissue
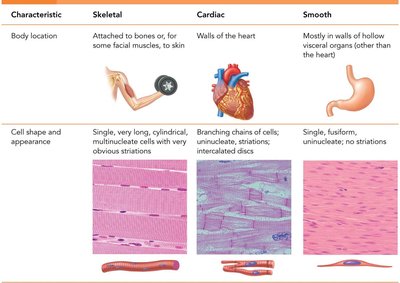
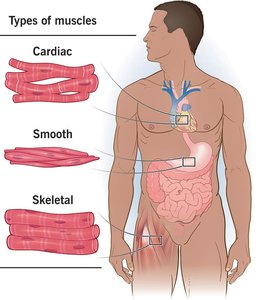
Muscle tissue is specialized for contraction and is essential for movement, posture, and various bodily functions. There are three main types of muscle tissue: skeletal, cardiac, and smooth muscle, each with distinct structures and functions.
Skeletal Muscle: Attached to bones and skin, responsible for voluntary movements, striated, and multinucleated.
Cardiac Muscle: Found only in the heart, responsible for pumping blood, striated, involuntary, and contains intercalated discs.
Smooth Muscle: Located in walls of hollow organs (except the heart), non-striated, involuntary, and spindle-shaped cells.
Functions and Characteristics of Muscle Tissue
Special Characteristics
Muscle tissue exhibits four key characteristics that enable its function:
Excitability (Responsiveness): Ability to receive and respond to stimuli.
Contractility: Ability to shorten forcibly when stimulated.
Extensibility: Ability to be stretched.
Elasticity: Ability to recoil to resting length after stretching.
Functions
Movement of bones or fluids (e.g., blood)
Maintaining posture and body position
Stabilizing joints
Heat generation (especially skeletal muscle)
Additional: Protects organs, forms valves, controls pupil size, causes "goosebumps"

Connective Tissue Wrappings of Skeletal Muscle
Organization and Structure
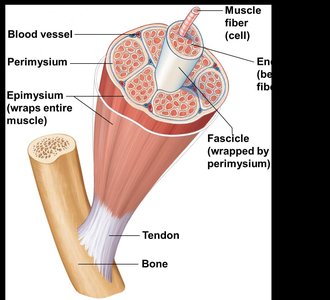
Skeletal muscles are organized into bundles and surrounded by connective tissue layers that provide support and transmit force.
Endomysium: Areolar connective tissue surrounding each muscle fiber (cell).
Perimysium: Fibrous connective tissue wrapping around a fascicle (bundle of muscle fibers).
Epimysium: Dense irregular connective tissue covering the entire muscle.
Tendons: Cordlike structures connecting muscle to bone, mostly collagen fibers.
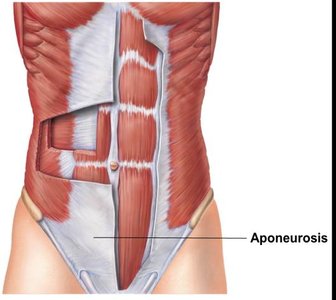
Aponeuroses: Sheetlike structures attaching muscles indirectly to bones or other muscles.
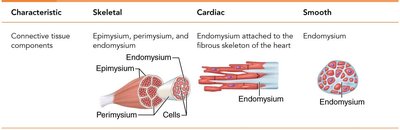
Skeletal Muscle Structure and Microscopic Anatomy
Muscle Fiber Structure
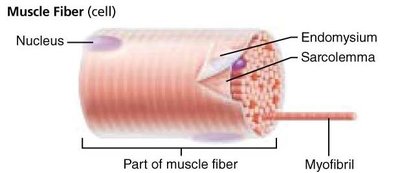
Each skeletal muscle fiber is a long, cylindrical cell containing multiple nuclei and specialized organelles for contraction.
Sarcolemma: Specialized plasma membrane of muscle fiber.
Myofibrils: Long organelles inside muscle cell, responsible for striations.
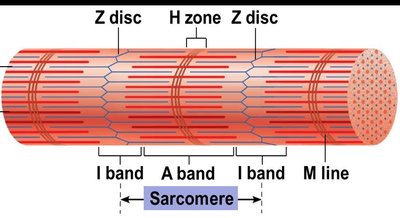
Sarcomere: The contractile unit, extending from one Z disc to another.
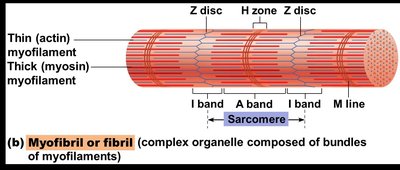

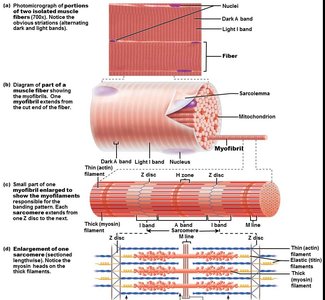
Myofilaments
Thin Filaments: Composed of actin proteins, anchored to Z discs.
Thick Filaments: Composed of myosin proteins, contain ATPase enzymes and myosin heads (cross bridges).
The arrangement of thin and thick filaments creates the characteristic banding pattern of skeletal muscle.
Sarcoplasmic Reticulum (SR)
Specialized smooth endoplasmic reticulum that stores and releases calcium ions, essential for muscle contraction.

The Nerve Stimulus and Action Potential
Neuromuscular Junction and Motor Unit
Muscle contraction is initiated by stimulation from a motor neuron at the neuromuscular junction.
Motor Unit: One motor neuron and all the muscle fibers it stimulates.
Neuromuscular Junction: Site where the axon terminal of a motor neuron communicates with the sarcolemma of a muscle fiber.
Neurotransmitter: Acetylcholine (ACh) is released to stimulate muscle contraction.
Synaptic Cleft: Gap between nerve and muscle, filled with interstitial fluid.

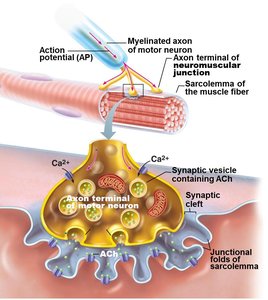
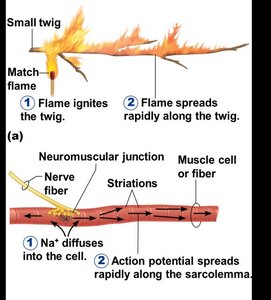
Transmission of Nerve Impulse
The action potential generated at the neuromuscular junction spreads along the sarcolemma, triggering muscle contraction.
Muscle Contraction: Sliding Filament Model and Cross Bridge Cycling
Sliding Filament Model
Muscle contraction occurs when myosin heads bind to actin, forming cross bridges and pulling thin filaments toward the center of the sarcomere. This process shortens the muscle fiber.
In the relaxed state, thin and thick filaments overlap only at the ends of the A band.
During contraction, the H zone and I bands shorten, Z discs move closer, and the muscle shortens.
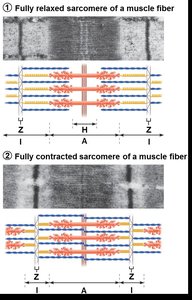
Cross Bridge Cycling
ATP is required for cross bridge detachment and re-cocking of the myosin head.
Absence of ATP (as in rigor mortis) prevents detachment, causing muscle stiffness after death.
Graded Response and Muscle Tension
Muscle Fiber Contraction
Muscle fiber contraction is "all or none"—a fiber contracts fully or not at all.
Graded responses occur when different numbers of fibers contract, producing varying degrees of muscle tension.
Tetanus is a sustained, smooth contraction resulting from rapid stimulation.
Types of Muscle Contractions
Isometric Contractions: Muscle tension increases, but the muscle does not shorten or produce movement (e.g., pushing against a wall).
Isotonic Contractions: Muscle shortens and movement occurs (e.g., bending the knee).
Muscle Tone: Continuous, partial contraction of muscles keeps them healthy and ready to respond.
Energy for Muscle Contraction
ATP Generation Pathways
Direct Phosphorylation: Creatine phosphate donates a phosphate to ADP to form ATP.
Aerobic Respiration: Uses oxygen to generate ATP from glucose; efficient but slower.
Anaerobic Glycolysis: Generates ATP quickly without oxygen, producing lactic acid as a byproduct.
ATP is the immediate source of energy for muscle contraction, but muscle fibers store only small amounts, requiring continuous regeneration during activity.
Muscle Fatigue and Oxygen Deficit
Fatigue occurs due to ionic imbalances, lactic acid accumulation, and decreased ATP supply.
After exercise, oxygen deficit is repaid by rapid, deep breathing to restore normal metabolic conditions.
Smooth Muscle Structure and Function
Location and Organization
Smooth muscle is found in the walls of most hollow organs (except the heart) and is organized in two layers: longitudinal and circular. This arrangement allows for peristalsis, the coordinated contraction and relaxation that moves substances through organs.
Microscopic Structure
Spindle-shaped, uninucleate cells without striations.
SR is less developed; most Ca2+ influx is from outside the cell.
No sarcomeres, myofibrils, or T tubules.
Innervation and Myofilaments
Innervated by autonomic nerve fibers at diffuse junctions.
Varicosities release neurotransmitters into the extracellular space.
Thick to thin filament ratio is lower than in skeletal muscle; calmodulin binds Ca2+ instead of troponin.
Dense bodies anchor filaments, analogous to Z discs in skeletal muscle.
Contraction and Regulation of Smooth Muscle
Mechanism of Contraction
Slow, synchronized contractions; cells are electrically coupled by gap junctions.
Some cells are self-excitatory and act as pacemakers.
Contraction is triggered by increased intracellular Ca2+, primarily from the extracellular space.
ATP is required for contraction; relaxation requires Ca2+ detachment from calmodulin and active transport out of the cell.
Regulation and Special Features
Regulated by nerves, hormones, and local chemical changes.
Stress-relaxation response allows adaptation to stretching (e.g., in the bladder).
Smooth muscle can undergo hyperplasia (increase in cell number), unlike skeletal muscle.
Developmental Aspects and Disorders of Muscle Tissue
Development and Aging
All muscle tissue develops from myoblasts.
Cardiac and skeletal muscle become amitotic after birth; smooth muscle retains regenerative ability.
With aging, muscle fibers are lost and replaced by connective tissue, leading to decreased strength and mass.
Muscular System Disorders
Fibromyalgia: Chronic inflammation of muscles and connective tissues, cause unknown.
Hernia: Protrusion of an organ through a muscle wall, often due to muscle weakness or strain.
Duchenne Muscular Dystrophy: Inherited disease causing muscle degeneration due to lack of dystrophin.
Myasthenia Gravis: Autoimmune disease where acetylcholine receptors are attacked, leading to muscle weakness and possible respiratory failure.
