 Back
BackPre-Conception Nutrition and Reproductive Physiology: Study Notes
Study Guide - Smart Notes

Pre-Conception Nutrition
Introduction to Pre-Conception Nutrition
Pre-conception nutrition refers to the nutritional status and dietary practices of individuals, particularly women, in the months leading up to conception. This period is critical because it influences fertility, pregnancy outcomes, and the health of the newborn. Both undernutrition and overnutrition can negatively impact reproductive capacity and pregnancy success.
Preconceptional nutritional status affects maternal health and the course and outcome of pregnancy.
Dietary intake, supplement use, and body composition are key factors in reproductive health.
Undernutrition can result in the birth of small, frail infants with high mortality risk.
Nutrition before and during early pregnancy is crucial for embryonic development and reducing complications.
Key Point: Food and healthy nutrition are associated with fertility health in both women and men. Optimal nutrition is also essential for the success of assisted reproductive technologies.
Why Nutrition is Important at the Preconception Stage
Fertility is maintained by complex physiological processes that can be disrupted by poor nutrition, body composition, or unhealthy lifestyle factors. Achieving optimal nutritional status before pregnancy increases the likelihood of conception and supports a healthy pregnancy and newborn.
Obesity can affect ovulation, menstrual cycles, and increase the risk of pregnancy complications such as miscarriage and preeclampsia.
Iron deficiency can cause irregular periods, poor egg quality, and low sperm count in men.
Folic acid supplementation reduces the risk of neural tube defects (NTDs).
Nutrition Objectives Related to Pre-Conception
National health objectives focus on improving preconception health through nutrition. These include increasing healthy weight, reducing obesity, and addressing micronutrient deficiencies.
Increase the proportion of adults at a healthy weight.
Reduce obesity and iron deficiency among adults of childbearing age.
Increase folic acid supplementation and pre-conceptional nutrition counseling.
Objective | Description |
|---|---|
Healthy Weight | Increase the proportion of women at a healthy weight prior to pregnancy by 10%. |
Obesity | Reduce the proportion of women aged 18 to 44 years who are obese by 10%. |
Iron Deficiency | Reduce iron deficiency among females of childbearing age by 10%. |
Folic Acid Intake | Increase the proportion of women of childbearing potential with adequate folic acid intake by 10%. |
Preconception Care | Increase the proportion of women receiving preconception care by 10%. |

Key Concepts in Reproductive Physiology
Definitions
Infertility: Biological inability to bear children after one year of unprotected intercourse.
Fertility: Actual ability to reproduce or bear children.
Fecundity: Biological ability to bear children.
Subfertility: Reduced fertility characterized by a long time to conception or repeated early pregnancy losses.
Miscarriage: Loss of conception in the first 20 weeks of pregnancy (spontaneous abortion).
Approximately 15% of couples are infertile, but many will conceive within three years without technology. Healthy couples have a 23% to 30% chance of conception per menstrual cycle.

Premenstrual Syndrome (PMS) and Premenstrual Dysphoric Disorder (PMDD)
PMS: Life-disrupting physiological and psychological changes during the luteal phase, affecting about 40% of menstruating women.
PMDD: Severe form of PMS, diagnosed when five or more symptoms occur in at least two consecutive cycles.
Reproductive Physiology: Female
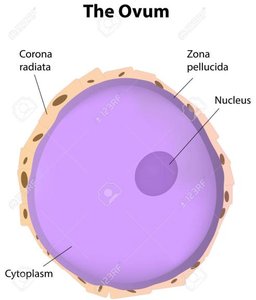
The female reproductive system is responsible for producing ova (eggs) and supporting fertilization and pregnancy. Females are born with a finite number of immature ova, which decrease with age and exposure to environmental factors.
Ova are produced and stored in the ovaries.
Only 400–500 ova mature and are released during a woman's reproductive years.
Ova can be damaged by oxidation, radiation, and aging, increasing the risk of chromosomal disorders in children born to older women.
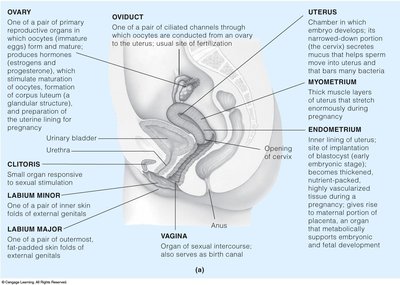
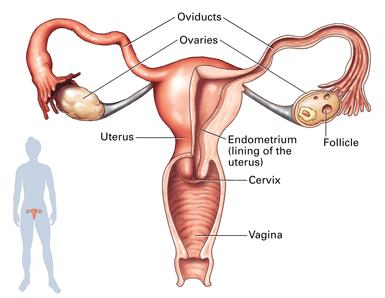
Female Reproductive System Anatomy
The female reproductive system includes the ovaries, oviducts (fallopian tubes), uterus, cervix, and vagina. Each part plays a specific role in reproduction, from egg production to fertilization and fetal development.
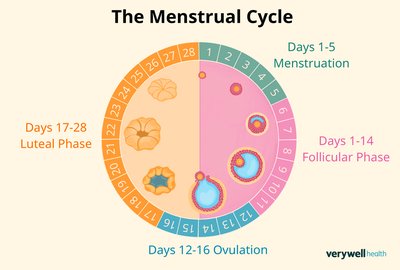
Menstrual Cycle
The menstrual cycle is a roughly 28-day process involving hormonal changes that prepare the uterus for pregnancy. It consists of the follicular phase, ovulation, and luteal phase.
Follicular Phase: First half of the cycle; follicle growth and maturation; main hormones: GnRH, FSH, estrogen, progesterone.
Ovulation: Release of a mature egg from the ovary.
Luteal Phase: Second half; corpus luteum forms, progesterone rises, uterine lining thickens for possible implantation.
If fertilization does not occur, hormone levels drop and menstruation begins.
Reproductive Physiology: Male
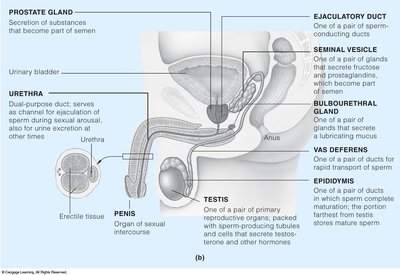
Male Reproductive System Anatomy
The male reproductive system produces and delivers sperm. Key structures include the testes, epididymis, vas deferens, seminal vesicles, prostate gland, and penis.
Androgens: Steroid hormones (e.g., testosterone) that stimulate development and function of male sex organs.
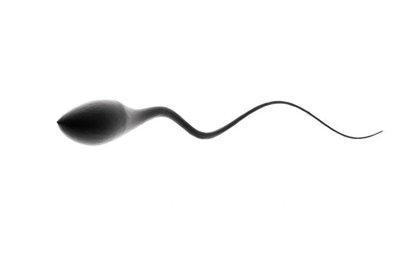
Semen: Ejaculate containing sperm and secretions, rich in nutrients like zinc and fructose.
Sperm production begins at puberty and continues throughout life, though it decreases after age 35.
Nutrition-Related Disruptions in Fertility
Factors Affecting Fertility
Adverse nutritional exposure
Contraceptive use
Severe stress
Infection
Tubal or structural damage
Chromosomal damage
Undernutrition and Fertility
Both acute and chronic undernutrition can reduce fertility. Acute undernutrition in previously well-nourished women leads to a dramatic decline in fertility, which recovers with improved food intake. Chronic undernutrition primarily results in the birth of small, frail infants with high mortality risk.
Body Fat and Fertility
Both low and high body fat can alter hormone levels (estrogen, leptin), reducing fertility.
Infertility is more common with BMI <20 or >30.
Weight Loss and Fertility
Weight loss >10-15% of usual weight decreases estrogen, LH, FSH, leading to amenorrhea and anovulatory cycles in women.
In men, weight loss of 10-15% below normal reduces sperm viability and motility; losses >25% can cease sperm production.
Oxidative Stress, Antioxidant Status, and Fertility
Oxidative stress decreases sperm motility and egg quality.
Antioxidants (vitamin E, C, beta-carotene, selenium) protect reproductive cells and improve fertility.
Zinc is essential for sperm maturation and testosterone synthesis; deficiency leads to poor sperm quality.
Other Nutrition-Related Factors
Folate: Adequate intake reduces risk of neural tube defects and improves fertility in both sexes.
Iron: Supplementation lowers infertility risk and supports ovulation.
Exercise: Moderate exercise improves fertility; excessive exercise can inhibit ovulation.
Caffeine: Intake below 200 mg/day does not affect fertility.
Alcohol: High intake disrupts menstrual cycles and ovulation.
Heavy Metals: Exposure reduces fertility, especially in men.
Summary Table: Nutrition-Related Factors Affecting Fertility
Factor | Effect on Fertility |
|---|---|
Undernutrition | Decreases fertility, increases risk of small, frail infants |
Obesity | Disrupts ovulation, increases pregnancy complications |
Iron Deficiency | Irregular periods, poor egg/sperm quality |
Folate Deficiency | Increases risk of neural tube defects |
Antioxidant Deficiency | Reduces sperm/egg quality |
Excessive Exercise | Inhibits ovulation |
Alcohol | Disrupts menstrual cycles, ovulation |
Heavy Metals | Reduces fertility, especially in men |
Conclusion
Optimal pre-conception nutrition is essential for fertility, healthy pregnancy, and positive birth outcomes. Key strategies include maintaining a healthy weight, ensuring adequate intake of iron, folate, and antioxidants, and avoiding excessive alcohol, caffeine, and exposure to heavy metals.
