 Back
BackRepro 4 - March 27
Study Guide - Smart Notes

Female Reproduction
Primary and Secondary Sex Characteristics
The female reproductive system is responsible for the production of gametes, secretion of sex hormones, and support of embryonic development. Sex characteristics are divided into primary and secondary types:
Primary sex characteristics: Internal sexual organs (ovaries, uterus, fallopian tubes, vagina) and external genitalia, which differentiate during embryonic development under the influence of androgens.
Secondary sex characteristics: Features that develop at puberty, such as body shape, breast development, distribution of body hair, and changes in voice and behavior. Androgens and estrogens regulate these changes.
Androgens: Anabolic hormones that promote protein synthesis and influence organs such as the brain, kidneys, heart, skin, liver, and bones.
External Genitalia
The external female genitalia are collectively referred to as the vulva or pudendum. These structures protect the internal reproductive organs and play a role in sexual arousal and intercourse.
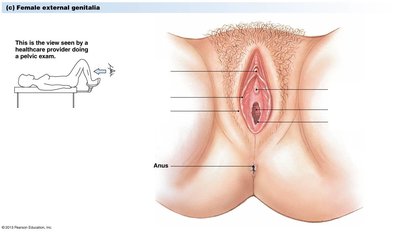
Internal Reproductive Anatomy
The internal reproductive organs include the vagina, uterus, fallopian tubes, and ovaries. The vagina leads to the uterus, which is the site of implantation and development of the embryo during pregnancy. The cervix is the opening of the uterus.
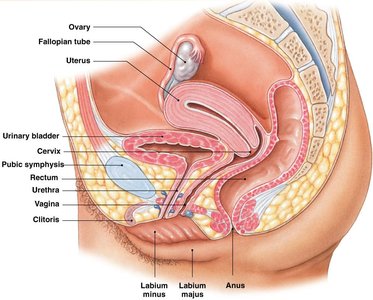
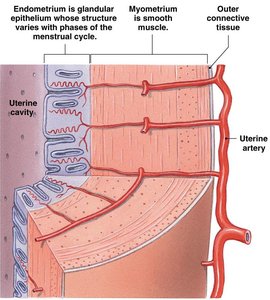
Uterine Structure
Perimetrium: Thin outer connective tissue layer.
Myometrium: Thick layer of smooth muscle responsible for uterine contractions.
Endometrium: Inner glandular layer that undergoes cyclical changes during the menstrual cycle.
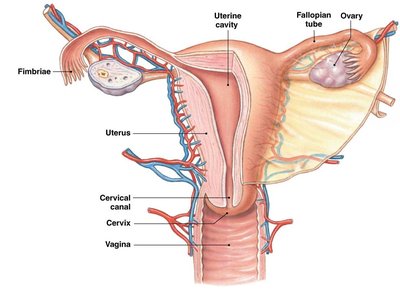
Fallopian Tubes and Ovaries
Fallopian tubes: Muscular tubes lined with cilia that transport eggs from the ovaries to the uterus. Fimbriae at the end of the tubes help capture the ovulated egg.
Ovaries: Produce eggs (oocytes) and secrete hormones such as estrogen and progesterone. The ovary contains follicles at various stages of development.
Ovarian Follicle Development
Folliculogenesis
Folliculogenesis is the maturation process of ovarian follicles, which contain the developing oocyte. Females are born with a finite number of primordial follicles, which decrease with age.
At birth: ~500,000 primordial follicles
At puberty: ~180,000 primordial follicles
Each menstrual cycle: A cohort of follicles is recruited, but usually only one becomes dominant and ovulates.
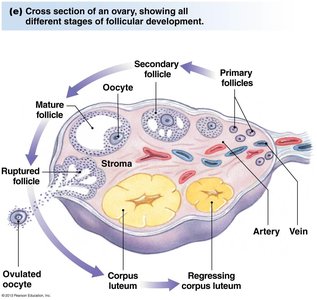
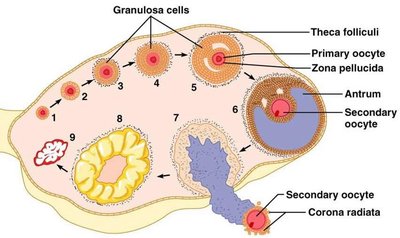
Stages of Follicular Development
Primordial follicle: Contains a primary oocyte arrested in prophase I of meiosis.
Primary follicle: Oocyte surrounded by a single layer of granulosa cells.
Secondary follicle: Multiple layers of granulosa cells and theca cells develop.
Tertiary (antral) follicle: Formation of a fluid-filled cavity called the antrum.
Dominant follicle: One follicle becomes dominant and completes maturation.
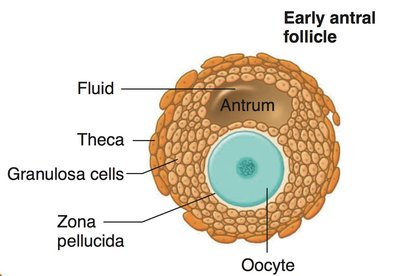
Follicular Atresia
Most follicles undergo atresia (degeneration) and do not reach ovulation. Only a small fraction of follicles ovulate during a woman's reproductive lifespan.
The Menstrual Cycle
Overview and Phases
The menstrual cycle is a recurring process averaging 28 days (range: 24–35 days), during which the female body prepares for possible pregnancy. It is divided into ovarian and uterine cycles, which are tightly coordinated by hormonal signals.
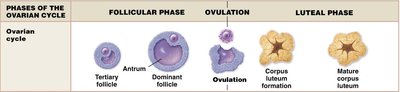
Follicular phase (Ovarian): Follicular growth and maturation (variable length, ~10–21 days).
Ovulation: Release of the mature oocyte from the dominant follicle (triggered by LH surge).
Luteal phase (Ovarian): Corpus luteum forms from the ruptured follicle and secretes hormones (fixed length, ~14 days).
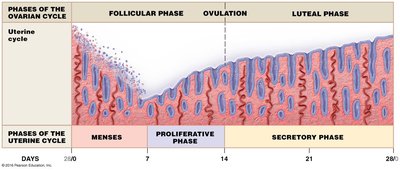
Uterine Cycle Phases
Menses: Shedding of the endometrial lining (menstrual bleeding, days 1–5).
Proliferative phase: Endometrial regeneration and thickening (under estrogen influence).
Secretory phase: Endometrium becomes secretory and prepares for implantation (under progesterone influence).
Hormonal Regulation of the Menstrual Cycle
Key Hormones and Feedback Loops
The menstrual cycle is regulated by a complex interplay of hormones from the hypothalamus, anterior pituitary, and ovaries:
GnRH (Gonadotropin-releasing hormone): Released from the hypothalamus; stimulates FSH and LH secretion from the anterior pituitary.
FSH (Follicle-stimulating hormone): Promotes follicular growth and estrogen production.
LH (Luteinizing hormone): Triggers ovulation and corpus luteum formation.
Estrogen: Dominant in the follicular phase; stimulates endometrial proliferation and exerts feedback on the hypothalamus and pituitary.
Progesterone: Dominant in the luteal phase; maintains the secretory endometrium.
Inhibin: Inhibits FSH secretion.
AMH (Anti-Müllerian hormone): Prevents excessive follicle recruitment.
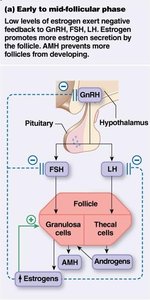
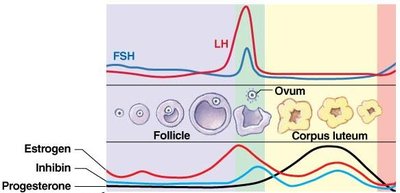
Hormonal Events by Phase
Early to mid-follicular phase: Low estrogen exerts negative feedback on GnRH, FSH, and LH. Estrogen promotes further follicle growth. AMH prevents additional follicle recruitment.
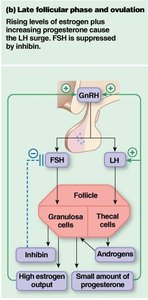
Late follicular phase and ovulation: High estrogen switches to positive feedback, causing an LH surge that triggers ovulation. Inhibin suppresses FSH.
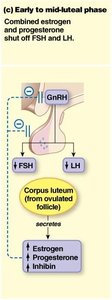
Luteal phase: Corpus luteum secretes progesterone, estrogen, and inhibin, which exert negative feedback on GnRH, FSH, and LH.
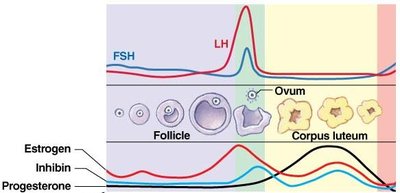
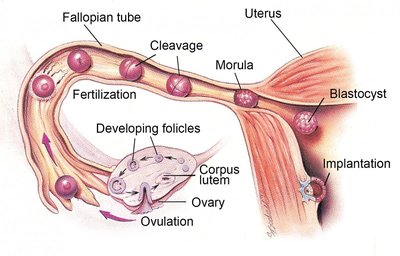
Ovulation and Corpus Luteum Formation
Ovulation
Ovulation occurs 16–24 hours after the LH peak. The mature follicle releases prostaglandins and proteolytic enzymes, which break down the follicular wall, allowing the secondary oocyte to be released and swept into the fallopian tube by the fimbriae.
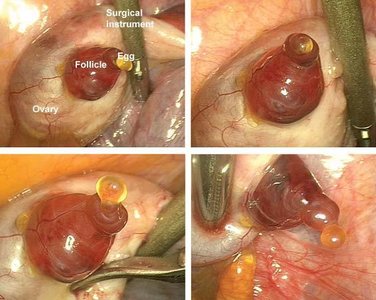
Corpus Luteum
After ovulation, the remnants of the follicle transform into the corpus luteum, which secretes progesterone and estrogen. These hormones maintain the endometrium in a secretory state, preparing for possible implantation. If pregnancy does not occur, the corpus luteum degenerates, hormone levels fall, and menstruation begins.
Summary Table: Ovarian and Uterine Cycle Phases
Ovarian Cycle Phase | Uterine Cycle Phase | Main Events | Dominant Hormone(s) |
|---|---|---|---|
Follicular | Menses/Proliferative | Follicle growth, endometrial regeneration | Estrogen |
Ovulation | End of Proliferative | Oocyte release | LH surge, Estrogen |
Luteal | Secretory | Corpus luteum activity, endometrial maintenance | Progesterone, Estrogen |
Key Terms and Concepts
Atresia: Degeneration of non-dominant follicles.
Corpus luteum: Temporary endocrine structure formed after ovulation.
Endometrium: Uterine lining that undergoes cyclical changes.
Fimbriae: Finger-like projections at the end of the fallopian tubes.
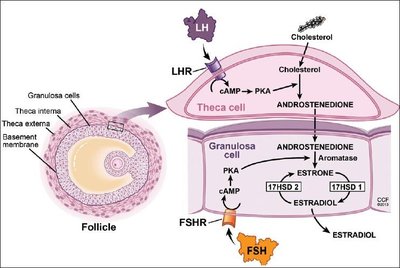
Granulosa cells: Follicular cells that produce estrogen and support oocyte development.
Theca cells: Follicular cells that produce androgens, which are converted to estrogens by granulosa cells.
Additional info: The menstrual cycle is essential for female fertility and is regulated by intricate hormonal feedback mechanisms. Disruptions in this cycle can lead to infertility or menstrual disorders.
