 Back
BackReproductive System Physiology: Cell Division, Gametogenesis, and Early Development
Study Guide - Smart Notes

Cell Division: Mitosis vs. Meiosis
Overview of Cell Division
Cell division is fundamental to growth, development, and reproduction. Two main types of cell division exist in humans: mitosis and meiosis.
Mitosis: Occurs in somatic (body) cells, producing two genetically identical diploid (2n = 46) daughter cells. This process is essential for tissue growth and repair.
Meiosis: Occurs only in gamete stem cells (spermatogonia and oogonia). It involves two sequential divisions, resulting in four genetically unique haploid (n = 23) cells. This reduction ensures that fertilization restores the diploid chromosome number.
Gametogenesis: Spermatogenesis vs. Oogenesis
Production of Gametes
Gametogenesis is the process by which gametes (sperm and ova) are produced. The process differs significantly between males and females.
Spermatogenesis: Occurs continuously in the testes from puberty onward. Each stem cell yields four functional, motile spermatozoa.
Oogenesis: Begins before birth, pauses, and resumes at puberty in the ovaries. Each cycle produces one functional ovum and three non-functional polar bodies.
Gamete Differences: Sperm are small, motile, and contribute only DNA. Ova are large, non-motile, and provide organelles and nutrients for early development.
Histology of the Masculinized Reproductive Tract
The Testis
Seminiferous Tubules: Coiled structures where spermatogenesis occurs.
Sustentacular (Sertoli/Nurse) Cells: Support developing sperm, facilitate spermatogenesis in response to FSH, and secrete inhibin to regulate sperm production.
Interstitial (Leydig) Cells: Located between tubules, produce testosterone when stimulated by LH.
The Spermatogenesis Sequence
Spermatogonia (Stem Cells): Type A cells remain as stem cells; Type B cells become primary spermatocytes.
Spermatocytes: Primary spermatocytes undergo Meiosis I to become secondary spermatocytes.
Spermatids: Haploid cells formed after Meiosis II.
Spermatozoa (Sperm): Final stage after spermiogenesis, where spermatids mature and develop tails.
Epididymis
Histology: Lined by pseudostratified columnar epithelium with stereocilia for absorption and nutrient transfer.
Function: Site of sperm maturation and storage; contracts during ejaculation.
Ductus (Vas) Deferens
Histology: Ciliated columnar epithelium and thick smooth muscle for strong peristaltic movement of sperm.
Hormonal Regulation of Gametogenesis
Key Hormones and Their Roles
FSH (Follicle Stimulating Hormone): Stimulates Sertoli cells (testes) and granulosa cells (ovaries) to promote gametogenesis.
LH (Luteinizing Hormone): Stimulates Leydig cells to produce testosterone and triggers ovulation in females.
Inhibin: Provides negative feedback to the pituitary, reducing FSH release.
Hormonal Cycles in the Female Reproductive System
Ovarian and Uterine Cycles
The female reproductive system operates through two interconnected cycles: the ovarian cycle and the uterine cycle, regulated by hormonal feedback loops.
Ovarian Cycle Hormones:
FSH: Stimulates follicle growth and estrogen production.
LH: Triggers ovulation and maintains the corpus luteum.
Uterine Cycle Hormones:
Estrogen: Stimulates endometrial proliferation and cilia formation in uterine tubes.
Progesterone: Maintains the endometrium during the secretory phase and inhibits further FSH/LH release.
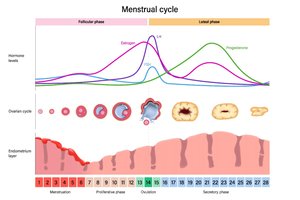
The 28-Day Cycle: Ovarian vs. Uterine
The menstrual cycle is divided into three main phases, each with distinct hormonal and structural changes.
Days 1–5: Menstrual Phase / Early Follicular Phase
Uterine: Endometrial shedding (menstruation) due to low estrogen/progesterone.
Ovarian: FSH rises, stimulating follicle development.
Days 6–14: Proliferative Phase / Late Follicular Phase
Uterine: Estrogen rebuilds the endometrium.
Ovarian: Dominant follicle matures; LH surge triggers ovulation on Day 14.
Days 15–28: Secretory Phase / Luteal Phase
Ovarian: Corpus luteum forms, secreting progesterone.
Uterine: Endometrium maintained for potential implantation; cycle restarts if no fertilization.
Histology of the Feminized Reproductive Tract
The Ovary
Oocyte: The egg cell itself.
Follicle: Surrounding cells that protect and nourish the oocyte and produce hormones.
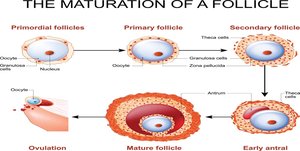
Follicle Stages:
Primordial & Primary: Early stages; granulosa cells produce estrogen in response to FSH.
Secondary: Larger, multilayered structure.
Tertiary (Graafian): Mature, with a large antrum; ovulation occurs from this stage.
Post-Ovulation Structures:
Corpus Luteum: Secretes progesterone.
Corpus Albicans: Scar tissue after hormone production ceases.
Uterine (Fallopian) Tube
Mucosal Folds: Guide the oocyte toward the uterus.
Ciliated Columnar Epithelium: Cilia move the oocyte; cilia increase with estrogen.
Smooth Muscle: Peristaltic contractions assist gamete movement.
The Uterus
Perimetrium: Outer serous layer.
Myometrium: Thick smooth muscle layer for contractions.
Endometrium: Inner lining, site of implantation; undergoes menstrual, proliferative, and secretory phases.
Vaginal Canal
Histology: Non-keratinized stratified squamous epithelium, adapted for friction and maintaining an acidic environment.
Conception and Early Development
Fertilization and Zygote Formation
Fertilization: Usually occurs in the uterine tube; sperm and oocyte fuse to form a diploid zygote.
Polyspermy Prevention: The oocyte undergoes changes to block additional sperm entry, ensuring correct chromosome number.
Early Cleavage and Blastocyst Formation
Morula: Solid ball of 16–32 cells (about 3 days post-fertilization).
Blastocyst: Hollow ball of cells (4–6 days), ready for implantation.
Trophoblast: Forms the chorion and placenta; secretes hCG to maintain the corpus luteum.
Inner Cell Mass (ICM): Becomes the embryo.
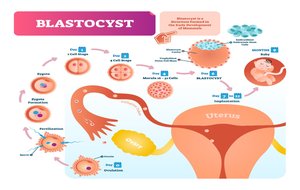
Implantation and Embryonic Development
Implantation: Blastocyst embeds in the endometrium (6–7 days post-fertilization).
Gastrula (Week 3): Formation of three germ layers (ectoderm, mesoderm, endoderm) via gastrulation.
Embryo (Implantation to Week 9): Major organ systems begin to form; supporting structures include the amnion, yolk sac, chorion, and umbilical cord.
Fetal Stage
Fetus (After Week 9): Characterized by growth and maturation of organs and tissues established during the embryonic period.
Summary Table: Key Differences in Gametogenesis
Feature | Spermatogenesis | Oogenesis |
|---|---|---|
Location | Testes | Ovaries |
Timing | Puberty to old age | Begins before birth, resumes at puberty |
Number of functional gametes per stem cell | 4 | 1 |
Motility | Motile (flagellum) | Non-motile |
Cytoplasmic content | Minimal | Abundant (nutrients, organelles) |
Additional info: This table summarizes the main distinctions between male and female gamete production, which are essential for understanding reproductive physiology.
