 Back
BackReproductive System: Structure, Function, and Regulation
Study Guide - Smart Notes

Male Reproductive System
Spermatogenesis and Spermatozoon Development
Spermatogenesis is the process by which sperm are produced in the testes. The final stage, spermiogenesis, involves the transformation of spermatids into mature spermatozoa, requiring structural reorganization of the nucleus and cytoplasm, and the development of a flagellum. Spermatozoa are released into the lumen of the seminiferous tubules but acquire full motility and fertilizing ability in the epididymis.
Spermiogenesis: Structural reorganization of spermatids.
Flagellum development: Essential for motility.
Epididymis: Sperm mature further, gaining sustained motility and ability to fertilize oocytes.
Timeframe: From spermatocyte to spermatozoon takes approximately 70 days.
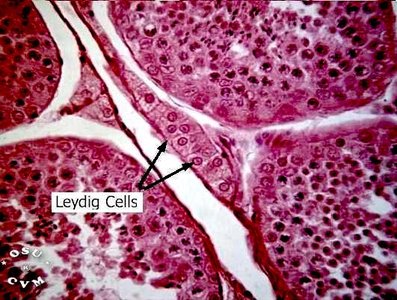
Blood-Testis Barrier and Sertoli & Leydig Cells
The blood-testis barrier is formed by tight junctions between Sertoli cells (sustentocytes), dividing the seminiferous tubule into basal and adluminal compartments. Sertoli cells nourish developing sperm, secrete fluid, digest discarded cytoplasm, bind FSH and testosterone, and produce inhibin. Leydig cells, located between seminiferous tubules, are vascularized and stimulated by LH to secrete testosterone, supporting spermatogenesis and accessory organs.
Sertoli Cells: Nourish sperm, secrete fluid, digest cytoplasm, bind hormones, produce inhibin.
Leydig Cells: Secrete testosterone in response to LH.
Blood-Testis Barrier: Protects developing sperm from immune system.
Hormonal Regulation of Spermatogenesis
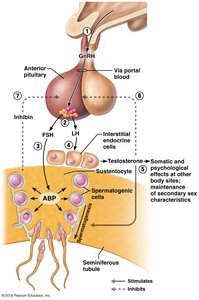
The hypothalamic-pituitary-gonadal axis regulates spermatogenesis. GnRH from the hypothalamus stimulates the anterior pituitary to release FSH and LH. FSH acts on Sertoli cells, while LH stimulates Leydig cells to produce testosterone. Inhibin from Sertoli cells provides negative feedback to the pituitary.
GnRH: Stimulates FSH and LH release.
FSH: Acts on Sertoli cells.
LH: Acts on Leydig cells.
Testosterone: Supports spermatogenesis and secondary sex characteristics.
Inhibin: Inhibits FSH release.
Functional Contributions of Epididymis and Accessory Organs
The epididymis is where sperm mature and gain motility. Accessory organs contribute to semen production: seminal vesicles secrete fructose-rich fluid and prostaglandins, the prostate gland secretes citrate-rich fluid, and bulbourethral glands produce mucus to neutralize acidic urine.
Epididymis: Sperm maturation and motility.
Seminal Vesicles: Fructose (energy), prostaglandins (motility).
Prostate Gland: Citrate (nutrient).
Bulbourethral Glands: Mucus (neutralizes urine).
Female Reproductive System
Anatomy of the Female Reproductive System
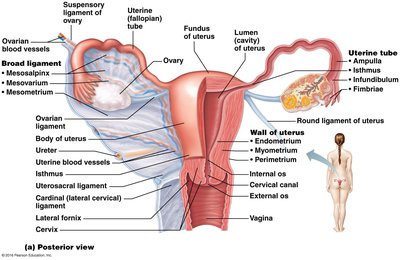
The female reproductive system includes internal genitalia (ovaries and accessory ducts: uterine tubes, uterus, vagina) and external genitalia (vulva). The ovaries are anchored by ligaments and supplied by ovarian arteries. The uterine tubes (oviducts) receive the egg and provide the site for fertilization, with specialized regions (ampulla, infundibulum, fimbriae, isthmus) facilitating oocyte movement.
Ovaries: Produce gametes and hormones.
Uterine Tubes: Site of fertilization; peristalsis and cilia move oocyte.
Uterus: Receives, retains, nourishes embryo.
Vagina: Passageway for sperm, menstrual flow, and delivery.
Vulva: External genitalia including mons pubis, labia, clitoris, vestibule.
Microscopic Anatomy of Ovaries and Oviducts
The ovary is covered by tunica albuginea and surface epithelium. The cortex contains follicles at various stages, including oocytes, granulosa cells, theca cells, and corpus luteum. The oviduct wall contains smooth muscle and ciliated/non-ciliated epithelial cells, aiding oocyte movement.
Follicles: Contain oocytes and supporting cells.
Corpus Luteum: Formed from ovulated follicle.
Oviduct Structure: Peristalsis and cilia facilitate oocyte transport.
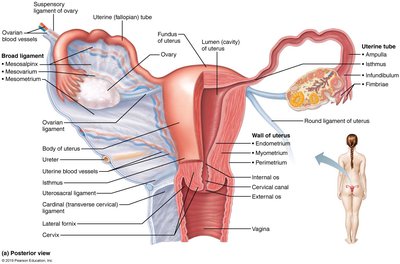
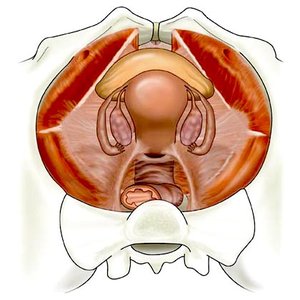
Gross and Microscopic Anatomy of the Uterus
The uterus is a muscular organ with three layers: perimetrium (outer), myometrium (middle, smooth muscle), and endometrium (inner, mucosal lining). The endometrium has two layers: stratum functionalis (shed during menstruation) and stratum basalis (regenerates functionalis). Vascular supply includes uterine, arcuate, straight, and spiral arteries.
Perimetrium: Visceral peritoneum.
Myometrium: Smooth muscle for labor.
Endometrium: Mucosal lining; site of implantation.
Vascular Supply: Uterine arteries and branches.
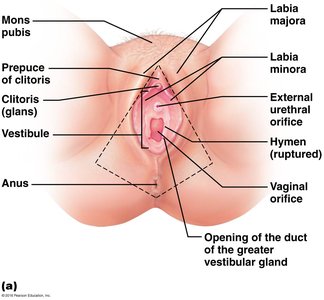
Anatomy of the Vagina and External Genitalia
The vagina is a muscular tube lined with stratified squamous epithelium, providing protection. It serves as a passageway for sperm, menstrual flow, and childbirth. The vulva includes the mons pubis, labia majora and minora, clitoris, vestibule, and associated glands.
Vagina: Three layers (adventitia, muscularis, mucosa); acidic pH deters infection.
Vulva: External structures; clitoris is erectile tissue.
Hymen: Incomplete partition of mucosa near vaginal orifice.
Regulation of Female Reproductive Function
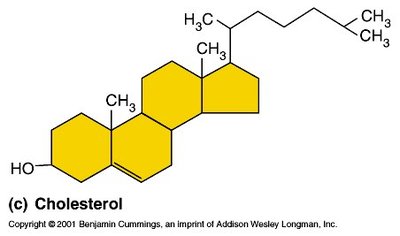
Ovarian Steroidogenesis
Ovarian steroidogenesis is compartmentalized, with different cell types producing progestins, androgens, and estrogens. Theca cells synthesize androgens, granulosa cells convert androgens to estrogens, and the corpus luteum produces progestins.
Progestins: Produced by granulosa, theca, and corpus luteum cells.
Androgens: Synthesized by theca cells; precursor for estrogens.
Estrogens: Synthesized by granulosa cells; essential for follicular development.
Hypothalamic & Pituitary Regulation
GnRH from the hypothalamus stimulates the anterior pituitary to release FSH and LH. FSH promotes follicular growth and estradiol production, while LH stimulates androgen production and ovulation.
GnRH: Stimulates FSH and LH release.
FSH: Stimulates follicular growth and estradiol production.
LH: Stimulates androgen production and ovulation.
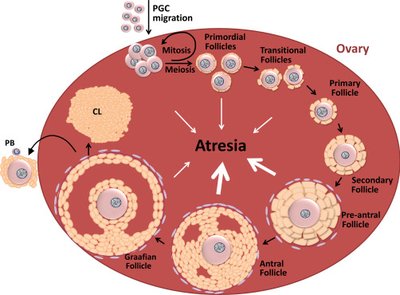
Ovarian Follicular Development and Hormonal Regulation
Follicular development begins with primordial follicles, progresses to primary and secondary follicles, and culminates in a dominant preovulatory follicle. FSH and LH regulate this process, with rising estrogen levels supporting follicular maturation.
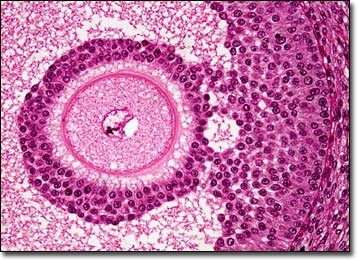
Primordial Follicle: Oocyte surrounded by granulosa cells.
Primary Follicle: Granulosa cells proliferate; theca cells differentiate.
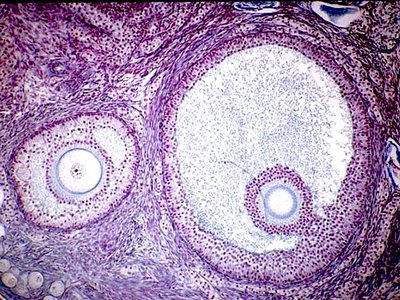
Secondary Follicle: Formation of antrum; FSH and LH responsiveness.
Dominant Follicle: Preovulatory; LH surge triggers ovulation.
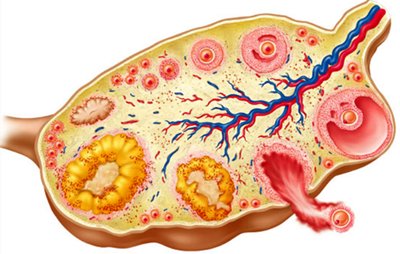
Ovulation and Corpus Luteum
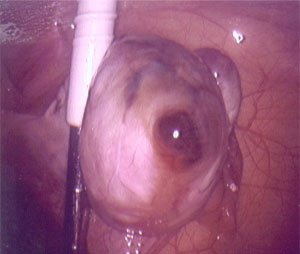
Ovulation is triggered by the LH surge, leading to the release of the oocyte. The corpus luteum forms from the remnants of the follicle and produces progesterone, supporting the uterine lining. If pregnancy does not occur, the corpus luteum degenerates.
LH Surge: Triggers ovulation and corpus luteum formation.
Corpus Luteum: Transient endocrine structure; produces progesterone.
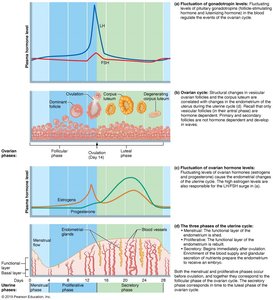
Cyclical Regulation of Uterine Endometrium
The endometrium undergoes cyclical changes: proliferative phase (cell proliferation and gland development in response to estrogen), secretory phase (thickening and fluid retention in response to progesterone), and menstruation (shedding of stratum functionalis).
Proliferative Phase: Resurfacing and cell proliferation.
Secretory Phase: Thickening and fluid retention.
Menstruation: Shedding of stratum functionalis.
Hormonal Regulation of Puberty and Menopause
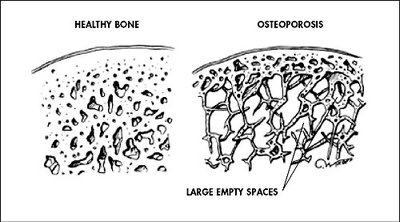
Puberty is initiated by increased FSH and LH secretion, leading to estradiol production and development of secondary sexual characteristics. Menopause is defined as cessation of menses for at least 12 months, primarily due to depletion of ovarian follicles, resulting in decreased estrogen and various physiological effects.
Puberty: Estradiol promotes breast, reproductive organ growth, fat redistribution, bone maturation.
Menopause: Loss of estrogen affects genital tissues, urinary tract, breasts, cardiovascular system, and skeleton.
Fertilization and Early Embryonic Development
Sperm Capacitation and Acrosome Reaction
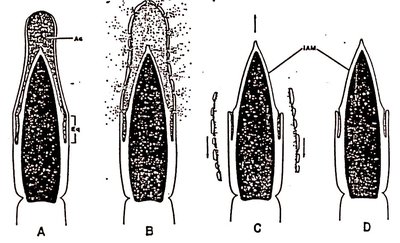
Sperm capacitation is a maturation process in the female reproductive tract, enabling sperm to fertilize the egg. The acrosome reaction occurs when sperm bind to the zona pellucida, releasing enzymes to penetrate the oocyte.
Capacitation: Increased motility and membrane fragility.
Acrosome Reaction: Release of digestive enzymes upon binding to zona pellucida.

Polyspermy Prevention and Zygote Formation
Polyspermy is prevented by fast and slow blocks after the first sperm penetrates the oocyte. The zygote forms when male and female pronuclei fuse, initiating embryonic development.
Fast Block: Immediate change in oocyte membrane potential.
Slow Block: Cortical reaction alters zona pellucida.
Zygote: Fusion of male and female pronuclei.
Early Embryonic Development
After fertilization, the embryo undergoes cleavage, forming a morula and then a blastocyst. Implantation begins around day 6, with the blastocyst burrowing into the endometrium.
Morula: Solid ball of cells.
Blastocyst: Hollow ball with inner cell mass.
Implantation: Blastocyst embeds in endometrium.
