 Back
BackSkeletal System: Bones & Bone Tissue – Structure, Function, and Physiology
Study Guide - Smart Notes

Chapter 6. Skeletal System: Bones & Bone Tissue
Overview of Connective Tissues in the Skeletal System
The skeletal system is composed of various connective tissues that provide structure, support, and facilitate movement. These include bone, cartilage, and blood, each with specialized cells and matrix compositions.
Mesenchymal cells: Stem cells that give rise to all connective tissues.
Cartilage Types:
Hyaline cartilage
Fibrocartilage
Elastic cartilage
Bone: Mineralized connective tissue providing rigidity and support.
Blood: Fluid connective tissue with red blood cells, white blood cells, and platelets.
Classification of Connective Tissue
Supporting Connective Tissue: Cartilage and bone.
Connective Tissue Proper:
Loose CT: Areolar, adipose, reticular
Dense CT: Dense regular, dense irregular, elastic
Fluid Connective Tissue: Blood
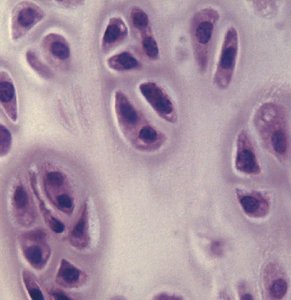
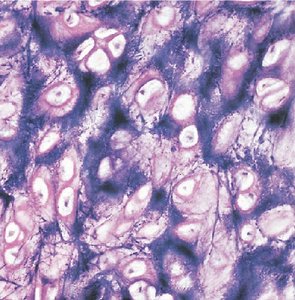
Cartilage: Structure and Function
Cartilage is a semi-rigid connective tissue that is more flexible than bone but less strong. It is avascular in its mature form and contains specialized cells:
Chondroblast: Produces cartilage matrix.
Chondrocyte: Mature cartilage cell surrounded by matrix.
Functions of Cartilage:
Support (e.g., trachea, ears, nose)
Gliding surface at joints (articulations)
Precursor model for bone growth
Bone: Structure, Classification, and Function
Bones are sturdy and rigid due to mineral deposition (calcification). They are primarily composed of bone connective tissue but also contain blood vessels, nerves, and other tissues.
Functions of Bone:
Support and protection (e.g., ribs, skull)
Movement (leverage for muscles)
Hematopoiesis (blood cell production)
Storage of minerals (calcium, phosphorus) and energy (fat)
Classification by Shape:
Long bones
Short bones
Flat bones
Irregular bones
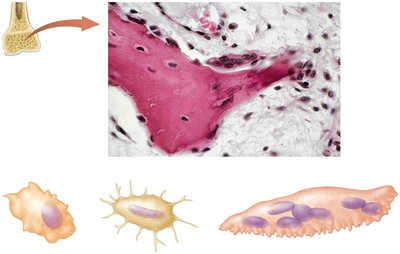
Bone Cells
Osteoblast: Produces bone matrix.
Osteocyte: Mature bone cell surrounded by matrix.
Osteoclast: Dissolves bone matrix for remodeling and calcium release.
Structure of a Long Bone
Diaphysis: Shaft of the bone.
Epiphysis: Knobby ends of the bone (may contain epiphyseal line).
Metaphysis: Region where diaphysis and epiphysis meet (contains epiphyseal plate in growing bones).
Medullary cavity: Central cavity containing red and yellow bone marrow.
Periosteum: Membrane covering the outer surface of bone.
Endosteum: Membrane lining the inner surface of bone.
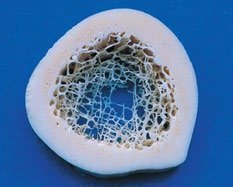
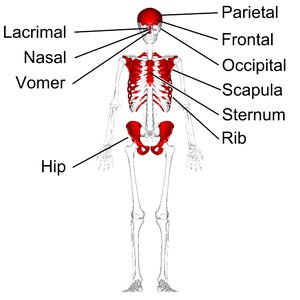
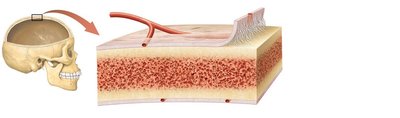
Structure of Flat Bone
Composed of two layers of compact bone with spongy bone (diploë) in between.
No medullary cavity or yellow bone marrow.
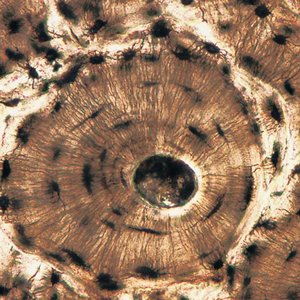
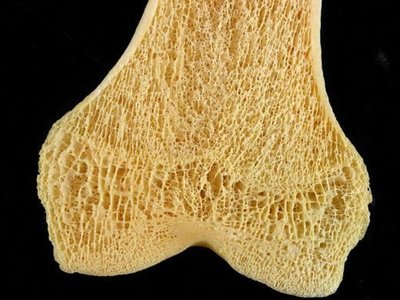
Microscopic Structure of Bone
Compact Bone: Organized into osteons (Haversian systems) with central canals, lamellae, and osteocytes in lacunae.
Spongy Bone: Composed of trabeculae with spaces for bone marrow.
Bone Development: Ossification
Ossification is the process of bone formation. There are two main types:
Endochondral Ossification: Bone develops from a hyaline cartilage model (most long bones).
Intramembranous Ossification: Bone develops directly from mesenchymal tissue (flat bones of skull, mandible, clavicle).
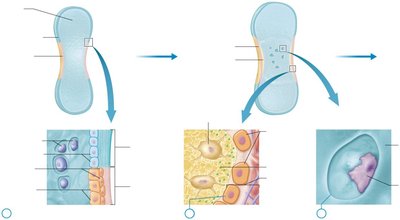
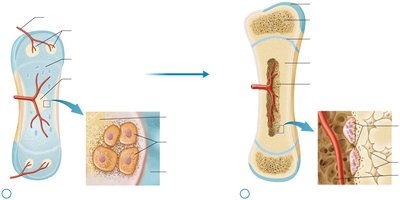
Endochondral Ossification
Chondroblasts in perichondrium differentiate into osteoblasts.
Osteoblasts build a bone collar on the external surface; internal cartilage calcifies and chondrocytes die.
Primary ossification center forms; osteoblasts replace calcified cartilage with spongy bone.
Secondary ossification centers form in epiphyses; medullary cavity develops.
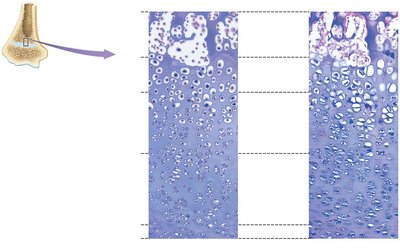
Epiphyseal Plate and Bone Growth
The epiphyseal plate is responsible for longitudinal growth of long bones through interstitial growth. It consists of several zones:
Zone of Resting Cartilage
Zone of Proliferation
Zone of Hypertrophy
Zone of Calcification
Zone of Ossified Bone
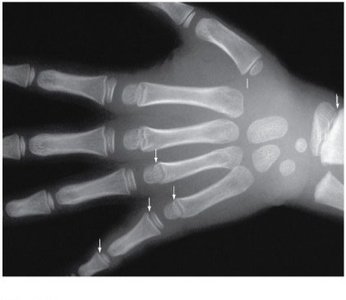
Epiphyseal Plate vs. Epiphyseal Line
During growth, the epiphyseal plate is present. After growth ceases, it is replaced by the epiphyseal line, indicating the end of longitudinal bone growth.
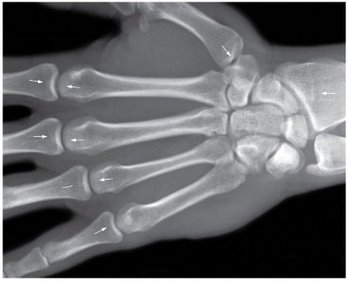
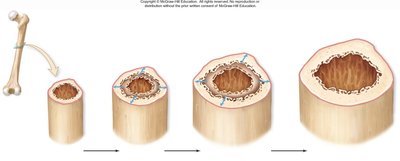
Appositional Growth
Appositional growth increases the diameter of bones. Osteoblasts in the periosteum build new bone matrix on the outer surface, while osteoclasts in the endosteum resorb bone on the inner surface.
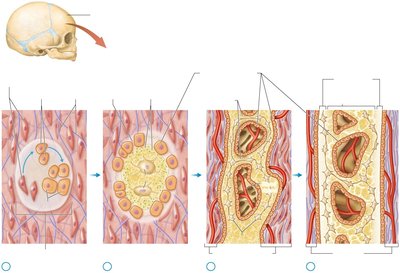
Intramembranous Ossification
Occurs in flat bones. Mesenchymal cells differentiate into osteoblasts, which secrete organic matrix that calcifies. Trabeculae of spongy bone form, and compact bone develops on the surfaces.
Bone Physiology: Health and Homeostasis
Calcification: Deposition of calcium salts in the matrix.
Vitamin D3 (Calcitriol): Essential for calcium absorption and bone health.
Exercise: Weight-bearing activities stimulate bone formation.
Hormonal Regulation:
Estrogen limits osteoclast activity.
Testosterone stimulates osteoblast activity.
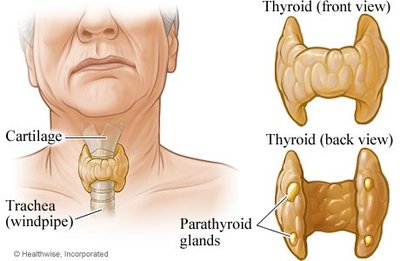
Hormonal Regulation of Blood Calcium Levels
Parathyroid Hormone (PTH): Released when blood Ca2+ is low; stimulates osteoclasts, increases intestinal absorption and kidney reabsorption of Ca2+.
Calcitonin: Released when blood Ca2+ is high; inhibits osteoclasts, decreases intestinal absorption and kidney reabsorption of Ca2+.
Bone Fractures and Repair
Types of Fractures:
Greenstick: Incomplete break, common in children.
Comminuted: Bone shattered into fragments.
Spiral: Caused by twisting forces.
Compression: Bone crushed, common in elderly.
Avulsion: Tendon or ligament pulls off bone fragment.
Epiphyseal plate: Involves growth plate, may affect growth.
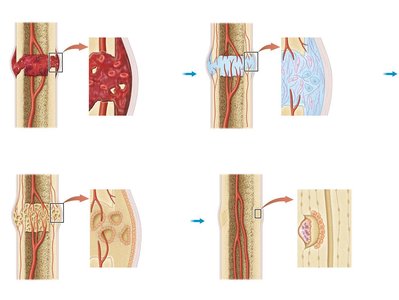
Repair Process:
Hematoma formation
Soft callus formation by fibroblasts and chondroblasts
Bone callus formation by osteoblasts
Remodeling to form secondary bone
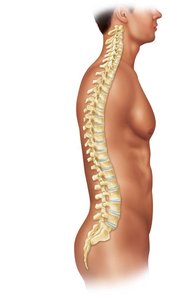
Vertebral Column Curvatures
Normal Curvatures: Cervical (concave), thoracic (convex), lumbar (concave), sacral (convex).
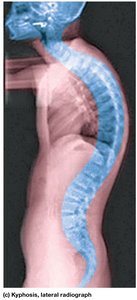
Abnormal Spinal Curvatures
Scoliosis: Lateral curvature of the spine.
Lordosis: Exaggerated lumbar curvature.
Kyphosis: Exaggerated thoracic curvature.
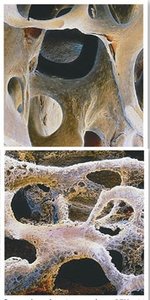
Effects of Aging on the Skeletal System
Bones become thinner and weaker with age (osteopenia).
Osteoporosis: Severe loss of bone mass, more common in women after menopause.
Bone cancer can stimulate abnormal osteoblast or osteoclast activity.
Summary Table: Types of Cartilage
Type | Main Locations | Key Features |
|---|---|---|
Hyaline cartilage | Articular surfaces, trachea, nose, costal cartilage | Most common, smooth matrix, supports and reduces friction |
Fibrocartilage | Intervertebral discs, pubic symphysis, menisci | Thick collagen fibers, resists compression |
Elastic cartilage | Ear, epiglottis | Elastic fibers, flexible and resilient |
Summary Table: Bone Cells
Cell Type | Function |
|---|---|
Osteoblast | Builds bone matrix |
Osteocyte | Maintains bone tissue |
Osteoclast | Resorbs bone matrix |
