 Back
BackCh. 14 Autonomic Nervous System and Homeostasis: ANP Study Notes
Study Guide - Smart Notes

Chapter 14: The Autonomic Nervous System and Homeostasis
Overview
The autonomic nervous system (ANS) is a critical component of the peripheral nervous system that regulates involuntary physiological processes, including heart rate, blood pressure, digestion, and urinary function. It operates largely below the level of conscious awareness and is essential for maintaining homeostasis.
Functions of the Autonomic Nervous System and Reflex Arcs
Visceral Reflex Arcs
Autonomic Nervous System (ANS): Oversees vital functions without conscious control, using visceral reflex arcs.
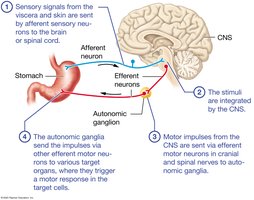
Pathway: Sensory signals from viscera and skin are sent by afferent sensory neurons to the CNS, where stimuli are integrated. Motor impulses are sent via efferent neurons to autonomic ganglia, which then relay signals to target organs, triggering a response.
Key Point: This system allows for rapid, automatic adjustments to internal and external changes.
Comparison of Somatic and Autonomic Nervous Systems
Somatic vs. Autonomic Motor Divisions
Somatic Motor Division: Controls voluntary movements by directly innervating skeletal muscle fibers with a single neuron; neurotransmitter is acetylcholine (ACh), always excitatory.
Autonomic (Visceral) Motor Division: Controls involuntary effectors (smooth muscle, cardiac muscle, glands) using a two-neuron chain (preganglionic and postganglionic neurons); neurotransmitters include ACh and norepinephrine, which can be excitatory or inhibitory.
Divisions of the Autonomic Nervous System
Sympathetic and Parasympathetic Divisions
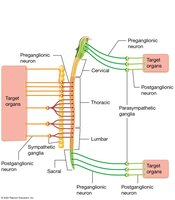
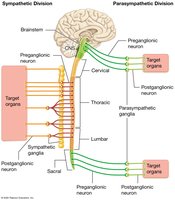
Sympathetic Nervous System (SNS): "Fight or Flight"; preganglionic neurons originate in thoracic and lumbar spinal cord (thoracolumbar division); ganglia are near the spinal cord; prepares the body for emergencies.
Parasympathetic Nervous System (PNS): "Rest and Digest"; preganglionic neurons originate in brainstem and sacral spinal cord (craniosacral division); ganglia are near or within target organs; promotes maintenance activities and conserves energy.
Balance: The two divisions generally have antagonistic effects, maintaining homeostasis through dual innervation.
Gross and Microscopic Anatomy of the Sympathetic Nervous System
Sympathetic Pathways and Ganglia
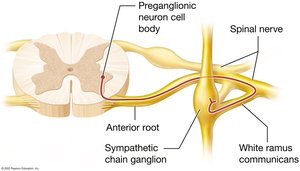
Preganglionic Neurons: Originate in the lateral horns of the thoracic and lumbar spinal cord; axons exit via the anterior root and travel through white rami communicantes to sympathetic chain ganglia.
Sympathetic Chain Ganglia: Series of ganglia running alongside the vertebral column; some preganglionic neurons synapse here, others in collateral (preaortic) ganglia near target organs.
Splanchnic Nerves: Preganglionic axons that synapse in collateral ganglia near abdominopelvic organs (e.g., celiac, superior mesenteric, inferior mesenteric ganglia).
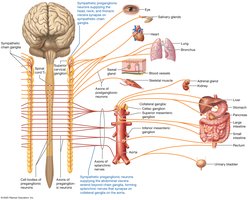
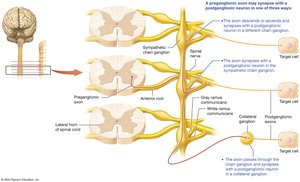
Three Pathways for Preganglionic Axons:
Synapse in the same chain ganglion.
Ascend or descend to synapse in a different chain ganglion.
Pass through the chain ganglion to synapse in a collateral ganglion.
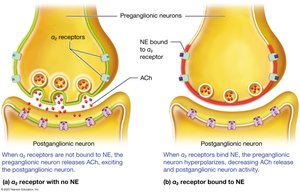
Sympathetic Neurotransmitters and Receptors
Types and Effects
Preganglionic Neurons: Release acetylcholine (ACh) at excitatory synapses with postganglionic neurons.
Postganglionic Neurons: Most release norepinephrine (noradrenaline); some release epinephrine (adrenaline) or ACh.
Adrenergic Receptors: Bind norepinephrine or epinephrine; include alpha (α1, α2) and beta (β1, β2, β3) subtypes, each with specific locations and effects.
Cholinergic Receptors: Bind ACh; include muscarinic (on sweat glands) and nicotinic (on all postganglionic neurons and adrenal medulla cells).
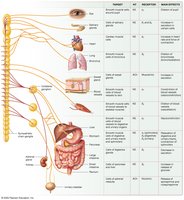
Effects of the Sympathetic Nervous System on Target Cells
Main Physiological Effects
Cardiac Muscle: Increases heart rate and force of contraction, raising blood pressure and blood flow to tissues.
Smooth Muscle:
Vasoconstriction of vessels to digestive, urinary, and integumentary systems (diverts blood to muscles).
Vasodilation of vessels to skeletal and cardiac muscle.
Bronchodilation (increased airway diameter).
Contraction of sphincters (inhibits urination and defecation).
Pupil dilation (more light enters the eye).
Metabolic Effects: Increases breakdown of lipids, release of glucose, and secretion of glucagon; raises cellular metabolic rate.
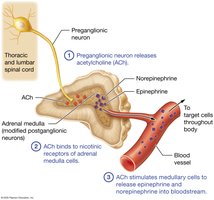
Adrenal Medulla: Releases epinephrine and norepinephrine into the bloodstream, prolonging sympathetic effects.
Other Effects: Increases mental alertness, blood clotting, and skeletal muscle tension; triggers "goose bumps" and ejaculation in males.
Pharmacology and Sympathetic Nervous System Receptors
Drug Actions
Antagonists (Blockers): Block adrenergic receptors, preventing norepinephrine binding; used to lower blood pressure and treat cardiovascular diseases.
Agonists: Mimic norepinephrine effects; used to treat asthma (bronchodilation) and other conditions.
The Parasympathetic Nervous System
Functions and Anatomy
Role: Maintains homeostasis during rest; promotes digestion, urination, and energy conservation.
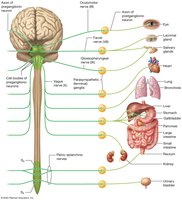
Preganglionic Neurons: Originate in cranial nerves (oculomotor, facial, glossopharyngeal, vagus) and sacral spinal nerves (S2–S4).
Terminal Ganglia: Located near or within target organs; postganglionic axons are short.
Parasympathetic Neurotransmitters and Receptors
Both pre- and postganglionic neurons release ACh.
Nicotinic Receptors: On all postganglionic neurons.
Muscarinic Receptors: On all target cells.
Effects of the Parasympathetic Nervous System on Target Cells
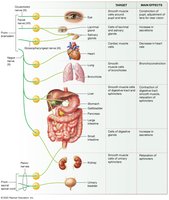
Main Physiological Effects
Cardiac Muscle: Decreases heart rate and blood pressure.
Smooth Muscle:
Pupil constriction (less light enters the eye).
Accommodation of the lens for near vision.
Bronchoconstriction (airway diameter decreases).
Stimulates peristalsis and relaxation of digestive/urinary sphincters (promotes digestion and urination).
Engorgement of erectile tissues (penis/clitoris).
Glandular Effects: Stimulates secretion of tears, saliva, and digestive enzymes; little effect on sweat glands.
Other Effects: No direct effect on metabolic rate, mental alertness, or skeletal muscle force; promotes storage of energy.
Pharmacology of the Parasympathetic Nervous System
Muscarinic Agonists: Stimulate parasympathetic effects; used to treat urinary retention and stimulate GI activity after surgery.
Muscarinic Antagonists: Block parasympathetic effects; used to increase heart rate, dilate pupils, and treat motion sickness.
Anticholinergic Side Effects: Many drugs can cause dry mouth, constipation, urinary retention, and blurred vision by blocking ACh or its receptors.

Interactions of Autonomic Divisions
Dual Innervation and Homeostasis
Most organs receive input from both sympathetic and parasympathetic divisions, which generally have opposing effects.
Sympathetic division dominates during stress or exercise; parasympathetic division dominates during rest and recovery.
Autonomic Tone
Autonomic Tone: Constant baseline activity from both divisions; sympathetic tone keeps blood vessels partially constricted, parasympathetic tone maintains resting heart rate and digestive/urinary activity.
Clinical Application: Postural Orthostatic Tachycardia Syndrome (POTS)
POTS: Characterized by an abnormal increase in heart rate upon standing, often with vasodilation and drop in blood pressure; symptoms include dizziness, fatigue, and more. May be treated with lifestyle changes and medications targeting sympathetic receptors.

Summary of Nervous System Control of Homeostasis
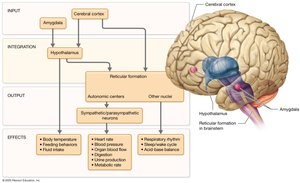
Central Regulation: The hypothalamus and brainstem reticular formation are central regulators of autonomic function, integrating input from higher brain centers (cerebral cortex, amygdala) and controlling preganglionic neurons.
Emotion and ANS: Emotional states can profoundly affect visceral functions via the hypothalamus and reticular formation.
Summary Table: Comparison of Somatic and Autonomic Motor Pathways
Feature | Somatic Motor | Autonomic Motor (Sympathetic) | Autonomic Motor (Parasympathetic) |
|---|---|---|---|
Number of Neurons | 1 (CNS to effector) | 2 (preganglionic and postganglionic) | 2 (preganglionic and postganglionic) |
Neurotransmitter | ACh (excitatory) | ACh (preganglionic), NE or ACh (postganglionic) | ACh (both) |
Effect on Target | Excitatory | Excitatory or inhibitory | Excitatory or inhibitory |
Effector Organs | Skeletal muscle | Smooth muscle, cardiac muscle, glands | Smooth muscle, cardiac muscle, glands |
Additional info: For further study, students are encouraged to use mnemonic devices and memory games to reinforce the differences between sympathetic and parasympathetic divisions, their neurotransmitters, and target organs.
