 Back
BackThe Autonomic Nervous System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Autonomic Nervous System (ANS)
Overview of the Autonomic Nervous System
The Autonomic Nervous System (ANS) is the involuntary division of the motor division of the peripheral nervous system (PNS). It regulates the activity of smooth muscle, cardiac muscle, and glands, maintaining homeostasis without conscious control.
Involuntary control is primarily from the limbic system, hypothalamus, brain stem, and spinal cord.
Receives input mainly from interoceptors (internal environment receptors).
Controls visceral functions such as heart rate, digestion, respiratory rate, salivation, perspiration, pupil diameter, and urination.
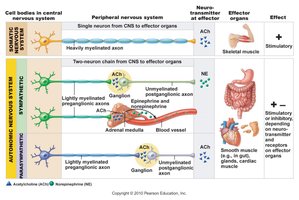
Comparison: Somatic vs. Autonomic Nervous Systems
The somatic and autonomic nervous systems differ in structure, neurotransmitters, and effectors.
Somatic Nervous System: Voluntary control, one-neuron pathway, all motor neurons release acetylcholine (ACh), effect is always stimulatory (skeletal muscle contraction).
Autonomic Nervous System: Involuntary control, two-neuron pathway (preganglionic and postganglionic), preganglionic neurons release ACh, postganglionic neurons release ACh or norepinephrine (NE), effect can be stimulatory or inhibitory (smooth/cardiac muscle, glands).
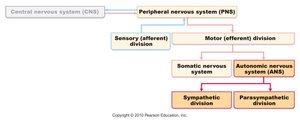
Divisions of the Autonomic Nervous System
Sympathetic and Parasympathetic Divisions
The ANS is divided into the sympathetic and parasympathetic divisions, which generally have opposing effects on target organs.
Sympathetic Division: "Fight or Flight" – mobilizes the body for action, increases heart rate, dilates pupils, inhibits digestion.
Parasympathetic Division: "Rest, Repose, Digest" – conserves energy, decreases heart rate, stimulates digestion, constricts pupils.
Most organs receive dual innervation, with antagonistic effects (e.g., one stimulates, the other inhibits).
Anatomical Organization
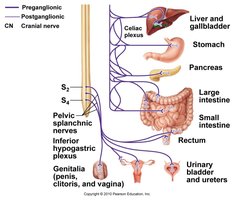
Parasympathetic Division: Craniosacral origin (cranial nerves III, VII, IX, X and sacral spinal nerves S2–S4). Ganglia are near or within the effector organ. Preganglionic axons are long; postganglionic axons are short.
Sympathetic Division: Thoracolumbar origin (thoracic and lumbar spinal cord). Ganglia are close to the spinal cord (sympathetic trunk). Preganglionic axons are short; postganglionic axons are long.
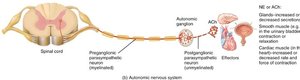
Parasympathetic Division: Cranial and Sacral Outflow
Cranial Nerves:
III (Oculomotor): Focus on close objects
VII (Facial): Stimulates salivary and tear glands
IX (Glossopharyngeal): Stimulates salivary glands
X (Vagus): Innervates thoracic and abdominal organs (heart, lungs, liver, stomach, pancreas, etc.)
Sacral Outflow: S2–S4 spinal segments innervate urinary bladder, reproductive organs, and lower digestive tract.
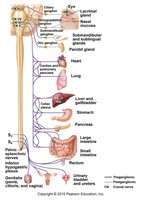
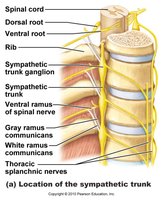
Sympathetic Division: Thoracolumbar Outflow
Preganglionic neuron cell bodies are in the lateral horns of the thoracic and lumbar spinal cord.
Axons exit via the ventral root, pass through white rami communicantes, and enter the sympathetic trunk ganglia (usually 23 pairs).
Some preganglionic fibers synapse in the trunk, others pass to collateral ganglia or the adrenal medulla.
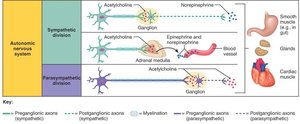
Functional Comparison of Sympathetic and Parasympathetic Effects
The two divisions have distinct effects on various organs, summarized in the table below:
Organ/System | Sympathetic Effect | Parasympathetic Effect |
|---|---|---|
Pupil | Dilation | Constriction |
Salivary Glands | Reduced secretion | Increased secretion |
Heart Rate & Force | Increased | Decreased |
Bronchioles | Relaxed (dilated) | Constricted |
Digestive Motility | Decreased | Increased |
Urine Secretion | Decreased | Increased |
Adrenal Medulla | Secretes NE/Epinephrine | No effect |
Neurotransmitters and Receptors in the ANS
Neurotransmitters
All preganglionic neurons (both divisions) release acetylcholine (ACh).
All parasympathetic postganglionic neurons release ACh.
Most sympathetic postganglionic neurons release norepinephrine (NE); some release ACh (e.g., sweat glands).
The effect on the target organ depends on the type of receptor present.
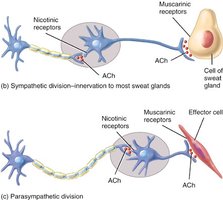
Receptors
Cholinergic Receptors (ACh):
Nicotinic receptors: Found on all postganglionic neurons, adrenal medulla cells, and skeletal muscle; always excitatory.
Muscarinic receptors: Found on all parasympathetic effector cells, sweat glands, and some blood vessels; effect can be excitatory or inhibitory depending on the subclass (e.g., inhibits heart, stimulates GI organs).
Adrenergic Receptors (NE):
Alpha receptors: Stimulate vasoconstriction, increase sweat, inhibit digestion.
Beta receptors: Stimulate the heart, relax airways.
Central Control of the Autonomic Nervous System
Hierarchy of ANS Control
Spinal Cord: Controls reflexes such as defecation and micturition (urination).
Brain Stem:
Medulla: Regulates heart rate, blood vessel diameter, gastrointestinal activity.
Pons: Controls respiratory rhythm.
Midbrain: Regulates pupil size and lens shape.
Hypothalamus: The main integration center for ANS activity; regulates heart rate, blood pressure, body temperature, water balance, and endocrine activity.
Cerebral Cortex: Can influence ANS activity through biofeedback, meditation, and emotional responses.
