 Back
BackThe Autonomic Nervous System: Structure, Function, and Homeostasis
Study Guide - Smart Notes

Overview of the Autonomic Nervous System (ANS)
Introduction to the ANS
The autonomic nervous system (ANS) is the involuntary branch of the peripheral nervous system (PNS), also known as the visceral motor division. It regulates most vital functions, including heart rate, blood pressure, and digestive and urinary processes, without conscious control. The ANS is divided into two main divisions: the sympathetic and parasympathetic nervous systems, which work together to maintain homeostasis.
Functions of the ANS and Visceral Reflex Arcs
Visceral Reflex Arcs
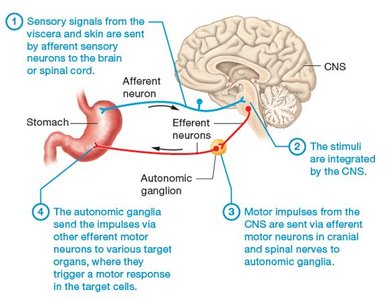
The ANS manages vital processes through visceral reflex arcs, where a sensory stimulus leads to a predictable motor response. The process involves:
Sensory signals from the viscera and skin are sent by afferent sensory neurons to the brain or spinal cord.
The CNS integrates these stimuli.
Motor impulses from the CNS are sent via efferent neurons in cranial and spinal nerves to autonomic ganglia.
The autonomic ganglia send impulses via other efferent neurons to various target organs, triggering a motor response in the target cells.
Comparison of Somatic and Autonomic Nervous Systems
Somatic vs. Autonomic Motor Pathways
The motor division of the PNS is divided into the somatic and autonomic systems:
Somatic motor neurons innervate skeletal muscle, leading to voluntary muscle contractions initiated consciously.
Autonomic motor neurons innervate smooth muscle, cardiac muscle, and glands, producing involuntary actions.
ANS motor pathways require a two-neuron circuit:
Preganglionic neuron: Cell body in the CNS; axon releases acetylcholine (ACh).
Postganglionic neuron: Cell body in autonomic ganglion in the PNS; axon travels to target cells and releases either ACh or norepinephrine (NE).
Divisions of the ANS
Sympathetic and Parasympathetic Divisions
The ANS is divided into two main divisions with distinct anatomical and functional characteristics:
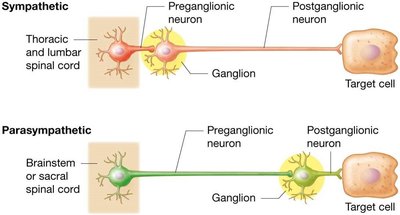
Sympathetic nervous system: Preganglionic axons are usually short; postganglionic axons are long. Originates in the thoracic and upper lumbar spinal cord (thoracolumbar division). Ganglia are located near the spinal cord.
Parasympathetic nervous system: Preganglionic axons are long; postganglionic axons are short. Originates in the brainstem and sacral spinal cord (craniosacral division). Ganglia are located near or within target organs.
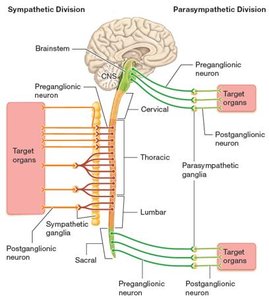
The sympathetic division is known as the "fight or flight" system, preparing the body for emergencies, while the parasympathetic division is the "rest and digest" system, maintaining homeostasis at rest.
Gross and Microscopic Anatomy of the Sympathetic Nervous System
Sympathetic Chain and Pathways
The sympathetic nervous system features a chain of ganglia running parallel to the vertebral column. Preganglionic neurons originate in the lateral horns of the thoracic and lumbar spinal cord and exit via the anterior root. They quickly separate to form white rami communicantes, leading to the sympathetic chain ganglia.
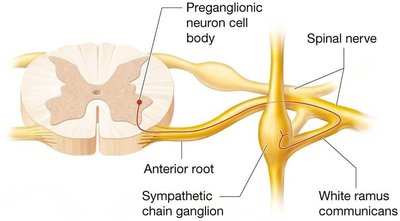
Preganglionic axons may synapse in the chain ganglia, ascend or descend to other ganglia, or pass through to collateral ganglia near target organs (especially in the abdominopelvic cavity).
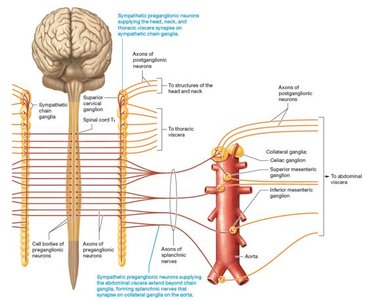
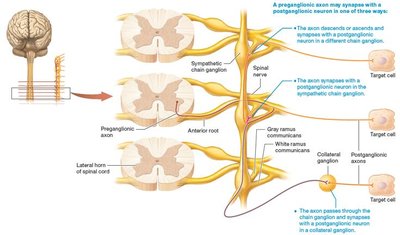
There are three possible synapse locations between pre- and postganglionic neurons:
At the same level in the sympathetic chain ganglion
At a different level in the chain ganglia
In collateral ganglia near target organs
Sympathetic Neurotransmitters and Receptors
Types and Actions of Receptors
Sympathetic neurotransmitters include acetylcholine (ACh), norepinephrine (NE), and epinephrine. Receptors are classified as:
Adrenergic receptors (bind NE and epinephrine):
Alpha-1: Smooth muscle of blood vessels, GI tract, kidneys, etc.
Alpha-2: Preganglionic sympathetic neurons (negative feedback)
Beta-1: Cardiac muscle, kidneys, adipose tissue
Beta-2: Smooth muscle of bronchioles, bladder, liver, pancreas
Beta-3: Adipose tissue, digestive tract
Cholinergic receptors (bind ACh):
Muscarinic: Sweat glands
Nicotinic: All postganglionic neurons in sympathetic ganglia and adrenal medullae
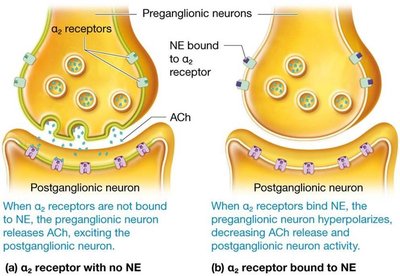
Alpha-2 receptors provide negative feedback to prevent excessive sympathetic output.
Effects of the Sympathetic Nervous System on Target Cells
Major Physiological Effects
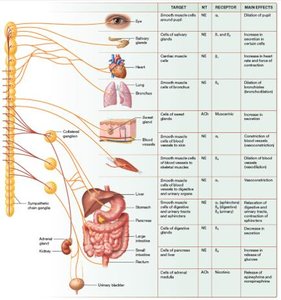
Cardiac muscle: NE binds beta-1 receptors, increasing heart rate and force of contraction, raising blood pressure and blood flow.
Smooth muscle: NE causes vasoconstriction in digestive, urinary, and integumentary systems (alpha-1), bronchodilation (beta-2), vasodilation in skeletal/cardiac muscle (beta-2), and contraction of sphincters (beta-2, beta-3).
Metabolism: NE triggers lipid breakdown (beta-3), glucose release (beta-2), and glucagon secretion (beta-2).
Sweat glands: ACh increases secretion via muscarinic receptors.
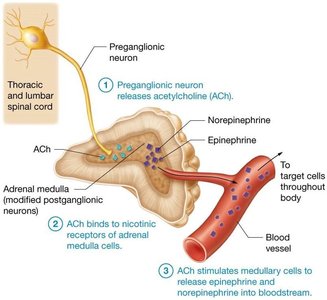
Adrenal medulla: Preganglionic neurons stimulate release of NE and epinephrine into the bloodstream, acting as hormones.
Other effects: Increased mental alertness, muscle tension, blood clotting, "goose bumps," and ejaculation in males.
Gross and Microscopic Anatomy of the Parasympathetic Nervous System
Parasympathetic Pathways
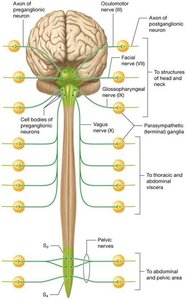
The parasympathetic division is known as the "rest and digest" system. Preganglionic neurons originate in the brainstem (cranial nerves III, VII, IX, X) and sacral spinal cord. The vagus nerve (CN X) provides the majority of parasympathetic output to thoracic and abdominal viscera. Preganglionic fibers synapse in terminal ganglia near or within target organs.
Parasympathetic Neurotransmitters and Receptors
Cholinergic Transmission
Both pre- and postganglionic parasympathetic neurons release ACh. The two main receptor types are:
Nicotinic receptors: On all postganglionic neurons
Muscarinic receptors: On all parasympathetic target cells
Effects of the Parasympathetic Nervous System on Target Cells
Major Physiological Effects
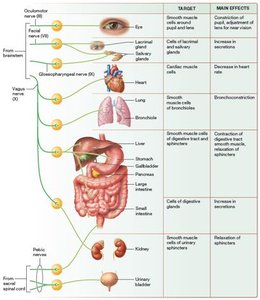
Cardiac muscle: Decreases heart rate and blood pressure (via vagus nerve).
Smooth muscle: Constriction of pupils (CN III), accommodation for near vision, bronchoconstriction (CN X), increased peristalsis, relaxation of sphincters, and engorgement of erectile tissues.
Glandular cells: Increased secretion from lacrimal, nasal, salivary, and digestive glands.
Other effects: No direct effect on metabolic rate, mental alertness, or skeletal muscle force; promotes fuel replenishment and recovery.
Interactions and Homeostasis
Dual Innervation and Autonomic Tone
Most organs receive dual innervation from both sympathetic and parasympathetic divisions, which often have antagonistic effects. This balance maintains homeostasis. Autonomic tone refers to the constant activity of both divisions, with sympathetic tone dominating in blood vessels and parasympathetic tone in the heart.
Central Control of the ANS
Role of the Hypothalamus and Brainstem
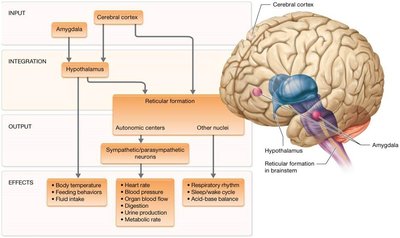
The hypothalamus and brainstem reticular formation centrally control homeostasis by regulating the activity of preganglionic sympathetic and parasympathetic neurons. Autonomic centers in the reticular formation coordinate these responses to maintain internal balance.
Summary Table: Sympathetic vs. Parasympathetic Nervous System
Feature | Sympathetic Nervous System | Parasympathetic Nervous System |
|---|---|---|
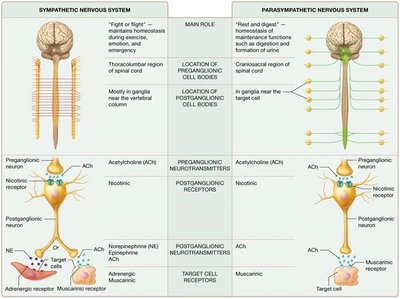
Main Role | "Fight or flight"; maintains homeostasis during exercise, emotion, and emergencies | "Rest and digest"; maintains homeostasis during rest and digestion |
Origin of Preganglionic Neurons | Thoracolumbar region of spinal cord | Brainstem and sacral region of spinal cord |
Location of Ganglia | Near vertebral column (sympathetic chain or collateral ganglia) | Near or within target organs (terminal ganglia) |
Preganglionic Neurotransmitter | Acetylcholine (ACh) | Acetylcholine (ACh) |
Postganglionic Neurotransmitter | Norepinephrine (NE), ACh (sweat glands), epinephrine (adrenal medulla) | Acetylcholine (ACh) |
Target Cell Receptors | Adrenergic (alpha, beta), muscarinic (sweat glands) | Muscarinic |
