Back
BackThe Female Reproductive System: Structure, Function, and Cycles
Study Guide - Smart Notes

Female Reproductive System Overview
Main Functions
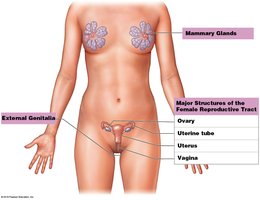
The female reproductive system is responsible for producing sex hormones, generating functional gametes (ova), supporting the development of embryos and fetuses, and nourishing newborns through lactation. It is composed of several organs, each with specialized roles in reproduction and development.
Production of Sex Hormones: Estrogen and progesterone regulate reproductive cycles and secondary sexual characteristics.
Production of Gametes: Oocytes are produced via meiosis.
Support of Embryo and Fetus: The uterus provides protection, nutrition, and waste removal.
Nourishment of Newborn: Mammary glands produce breast milk for infant nutrition.
The Ovary
Structure and Function
The ovaries are paired organs that produce immature female gametes (oocytes), secrete female sex hormones (estrogens and progesterone), and release inhibin to regulate follicle-stimulating hormone (FSH) production. Typically, only one oocyte is ovulated per month.
Oogenesis: The process of oocyte formation and development, which begins before birth, accelerates at puberty, and ends at menopause.
Hormone Secretion: Estrogens and progesterone are essential for regulating the menstrual cycle and preparing the uterus for pregnancy.
Inhibin: Inhibits FSH production to control the number of developing follicles.
Oogenesis
Stages of Oocyte Development
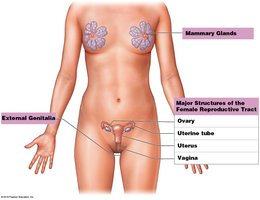
Oogenesis is the process by which oocytes are formed through meiosis. Unlike spermatogenesis, oogenesis results in only one mature ovum from each primary oocyte, with the majority of cytoplasm retained in the ovum to support early development.
Initiation: Begins before birth; primary oocytes are arrested in prophase I until puberty.
Completion: Each month, a few oocytes resume meiosis, but only one typically completes development and is ovulated.
End Point: Oogenesis ends at menopause.
Ovarian Cycle
Follicular Development and Ovulation
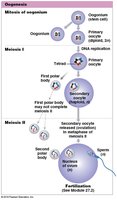
The ovarian cycle describes the monthly changes in ovarian follicles, which are specialized structures where oocyte growth and meiosis I occur. At birth, about 2 million primordial follicles exist, but only about 400,000 remain at puberty. Each month, FSH stimulates the development of several follicles, but only one is typically ovulated.
Primordial Follicles: Contain primary oocytes arrested in prophase I.
Follicular Development: Follicles mature through primary, secondary, and tertiary stages.
Ovulation: The dominant follicle releases its oocyte during ovulation.
Corpus Luteum: After ovulation, the follicle transforms into the corpus luteum, which secretes progesterone and estrogen.
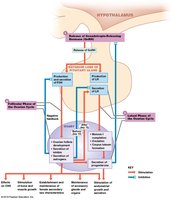
Hormonal Regulation of the Ovarian Cycle
The ovarian cycle is regulated by the hypothalamic-pituitary-gonadal axis. Gonadotropin-releasing hormone (GnRH) from the hypothalamus stimulates the release of FSH and LH from the anterior pituitary. These hormones regulate follicle development, ovulation, and corpus luteum function.
FSH: Stimulates follicle growth and estrogen production.
LH: Triggers ovulation and corpus luteum formation.
Feedback Loops: Estrogen and progesterone exert positive and negative feedback on GnRH, FSH, and LH secretion.
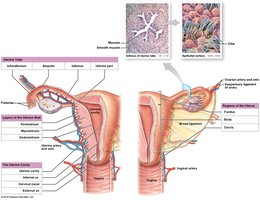
Uterine Tubes and Uterus
Oocyte Transport and Fertilization
The uterine tubes (fallopian tubes) transport the oocyte from the ovary to the uterus. This process involves ciliary movement and peristaltic contractions. Fertilization typically occurs in the ampulla of the uterine tube within 12–24 hours after ovulation.
Transport Time: 3–4 days for the oocyte to reach the uterine cavity.
Sperm Viability: Sperm can survive 24–48 hours in the female reproductive tract.
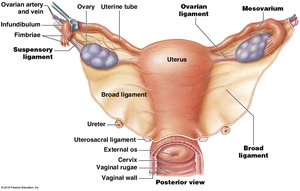
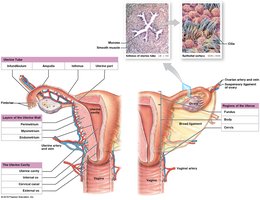
The Uterus
The uterus is a hollow, muscular organ that provides mechanical protection, nutritional support, and waste removal for the developing embryo and fetus. Its muscular wall contracts during childbirth to deliver the baby.
Regions: Fundus, body, and cervix.
Layers: Perimetrium (outer), myometrium (muscular), and endometrium (inner, functional layer).
Uterine (Menstrual) Cycle
Phases of the Uterine Cycle
The uterine cycle, or menstrual cycle, involves monthly changes in the endometrium in response to ovarian hormones. It averages 28 days but can range from 21 to 35 days. The cycle begins at menarche (~11–12 years) and ends at menopause (~45–55 years).
Menstrual Phase: Degeneration and shedding of the functional layer due to constricted spiral arteries. Lasts 1–7 days; 35–50 mL blood lost.
Proliferative Phase: Estrogens stimulate regeneration of the endometrium and uterine glands, which secrete glycogen-rich mucus.
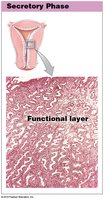
Secretory Phase: Progesterone and estrogens from the corpus luteum stimulate gland enlargement and increased secretion to support a potential embryo.
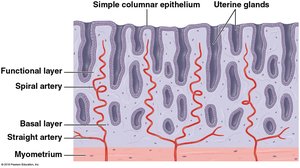
Uterine Vasculature
The blood supply to the uterus is crucial for supporting the endometrium and facilitating the menstrual cycle. The uterine artery branches into arcuate arteries, which encircle the endometrium, and radial arteries, which supply the endometrium. Spiral arteries supply the functional layer and are shed during menstruation.
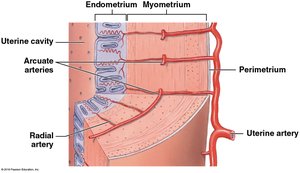
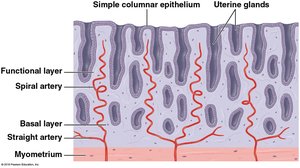
Histological Changes During the Uterine Cycle
Menstrual Phase: Shedding of the functional layer.
Proliferative Phase: Regeneration and thickening of the endometrium.
Secretory Phase: Glands enlarge and secrete nutrients.
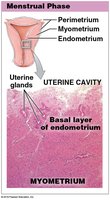
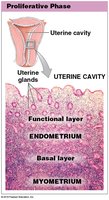
Vagina and External Genitalia
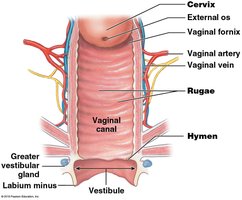
Vaginal Structure and Function
The vagina is an elastic, muscular tube extending from the cervix to the vestibule. It serves as a passageway for menstrual fluids, receives the penis during intercourse, and forms the lower portion of the birth canal.
Vaginal Canal: Lined by nonkeratinized stratified squamous epithelium, allowing for stretching and resistance to abrasion.
Rugae: Folds in the vaginal lining that allow for expansion.
Fornix: Recess around the cervix.
Hymen: Elastic fold that may partially cover the vaginal entrance.
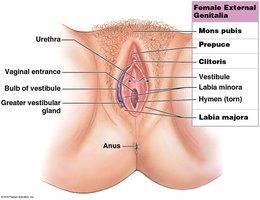
External Genitalia (Vulva)
The vulva includes the external genital structures such as the mons pubis, labia majora, labia minora, clitoris, and vestibule. The vestibule contains the openings to the urethra and vagina.
Lesser Vestibular Glands: Secrete moisture to prevent drying.
Greater Vestibular Glands (Bartholin’s glands): Secrete lubricating mucus during sexual arousal.
Mammary Glands
Structure and Function
Mammary glands are specialized organs located in the breasts that produce milk to nourish infants. Milk production (lactation) is regulated by hormones from the reproductive system and placenta. The glands develop during puberty and become functional during pregnancy.
Location: In the subcutaneous tissue over the pectoralis major muscle.
Structure: Composed of lobes, each containing lobules made up of secretory alveoli where milk is produced.
Suspensory Ligaments: Support the breast and separate lobes and lobules.
Milk Flow: Milk moves from alveoli into ducts, converging into lactiferous ducts and sinuses, which open at the nipple.
Nipple and Areola: The nipple is the projection where milk exits; the areola is the pigmented area around the nipple, containing sebaceous glands for protection during breastfeeding.