 Back
BackThe Heart: Anatomy, Physiology, and Cardiac Function
Study Guide - Smart Notes

The Heart and the Cardiovascular System
Overview of the Cardiovascular System
The cardiovascular system consists of the heart, blood, and blood vessels. It is responsible for circulating blood throughout the body, delivering oxygen and nutrients, and removing waste products.
Heart: Pumps blood approximately 100,000 times per day, moving about 8,000 liters.
Blood Vessels: Include arteries (carry blood away from the heart), veins (return blood to the heart), and capillaries (exchange vessels).
Circuits:
Pulmonary circuit: Carries blood to and from the lungs for gas exchange.
Systemic circuit: Carries blood to and from the rest of the body.
Anatomy of the Heart
Chambers and Structure
The heart has four chambers and is located in the mediastinum, between the lungs.
Right Atrium: Receives blood from the systemic circuit.
Right Ventricle: Pumps blood into the pulmonary circuit.
Left Atrium: Receives blood from the pulmonary circuit.
Left Ventricle: Pumps blood into the systemic circuit.
Apex: Pointed tip of the heart (inferior).
Base: Superior part where great vessels connect.
Heart Wall Layers
Epicardium: Visceral layer of serous pericardium, covers the heart surface.
Myocardium: Cardiac muscle tissue, responsible for contraction.
Endocardium: Inner lining, composed of simple squamous epithelium and areolar tissue.
Pericardium and Pericardial Cavity
Pericardium: Surrounds the heart, consists of an outer fibrous layer and an inner serous layer (parietal and visceral).
Pericardial Cavity: Space between parietal and visceral layers, contains pericardial fluid.
Pericarditis: Inflammation of pericardial surfaces, can cause cardiac tamponade (restricted heart movement due to excess fluid).
Superficial Anatomy
Atria: Thin-walled, each with an expandable auricle.
Sulci: Grooves containing fat and blood vessels; coronary sulcus marks border between atria and ventricles.
Interventricular Sulci: Mark boundary between left and right ventricles.
Internal Anatomy
Septa: Muscular partitions separating chambers.
Interatrial septum: Separates atria.
Interventricular septum: Separates ventricles; thicker than interatrial septum.
Cardiac Skeleton: Dense bands of elastic tissue encircle valves and bases of pulmonary trunk/aorta, stabilize and electrically insulate.
Heart Valves and Blood Flow
Atrioventricular (AV) Valves
AV valves (tricuspid and mitral) permit blood flow from atria to ventricles and prevent backflow.
Tricuspid Valve: Right AV valve, three cusps.
Mitral Valve: Left AV valve (bicuspid), two cusps.
Chordae Tendineae: Attach valve edges to papillary muscles, prevent valve inversion.
Semilunar Valves
Pulmonary Valve: At the exit of the right ventricle.
Aortic Valve: At the exit of the left ventricle.
Prevent backflow into ventricles.
Blood Flow Pathway
Right atrium receives blood from superior and inferior vena cava.
Blood flows through tricuspid valve to right ventricle.
Right ventricle pumps blood through pulmonary valve to pulmonary trunk and arteries.
Left atrium receives blood from pulmonary veins.
Blood flows through mitral valve to left ventricle.
Left ventricle pumps blood through aortic valve to aorta and systemic circulation.
Structural Differences Between Ventricles
The left ventricle has thicker walls and develops more pressure than the right ventricle, which is more pouch-shaped.
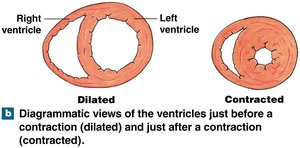
Valve Function During Cardiac Cycle
When ventricles are relaxed, AV valves are open and semilunar valves are closed.
When ventricles contract, AV valves close and semilunar valves open.
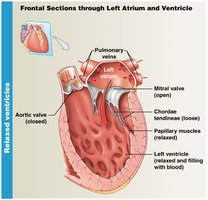
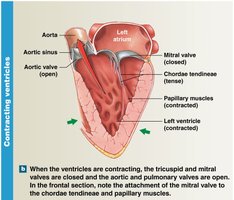
Coronary Circulation and Heart Disease
Coronary Circulation
Coronary Arteries: Originate at aortic sinuses, supply heart muscle.
Right Coronary Artery: Supplies right atrium, portions of both ventricles, and conducting system.
Left Coronary Artery: Supplies left ventricle, left atrium, and interventricular septum.
Cardiac Veins: Drain blood from heart muscle into coronary sinus, which opens into right atrium.
Coronary Artery Disease (CAD)
CAD involves partial or complete blockage of coronary circulation, often due to atherosclerotic plaque formation.
Coronary Ischemia: Reduced blood supply to heart muscle.
Angina Pectoris: Chest pain due to temporary ischemia.
Myocardial Infarction (MI): Heart attack caused by blockage, leading to cell death and infarct formation.
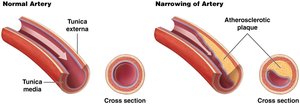
Treatment of CAD and MI
Risk Factor Modification: Stop smoking, treat hypertension, adjust diet, reduce stress, increase activity.
Drug Treatments: Reduce coagulation, block sympathetic stimulation, cause vasodilation, block calcium channels, relieve pain.
Noninvasive Surgery: Atherectomy, balloon angioplasty, stent placement.
Coronary Artery Bypass Graft (CABG): Surgical rerouting of blood around blocked arteries.
The Conducting System of the Heart
Cardiac Muscle Cells
Autorhythmic Cells: Control and coordinate heartbeat.
Contractile Cells: Produce contractions that propel blood.
Conducting System Components
SA Node: Pacemaker in right atrium, initiates heartbeat.
AV Node: Junction between atria and ventricles, delays impulse.
AV Bundle, Bundle Branches, Purkinje Fibers: Distribute impulse to ventricles.
Impulse Conduction
SA node activity begins, spreads across atria.
Impulse delayed at AV node, then travels through AV bundle, bundle branches, and Purkinje fibers.
Atrial contraction completes, ventricular contraction begins.
Electrocardiogram (ECG/EKG)
P Wave: Depolarization of atria.
QRS Complex: Depolarization of ventricles.
T Wave: Repolarization of ventricles.
Intervals (P–R, Q–T) measure timing of electrical events.
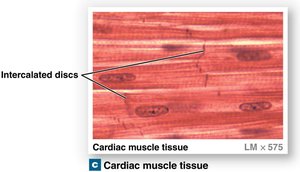
Cardiac Contractile Cells and Intercalated Discs
Form bulk of heart walls, receive stimulus from Purkinje fibers.
Resting membrane potential: –90 mV (ventricular), –80 mV (atrial).
Intercalated Discs: Specialized junctions connecting cells, transfer force and propagate action potentials.
Action Potential in Cardiac Contractile Cells
Rapid Depolarization: Influx of sodium ions.
Plateau: Influx of calcium ions.
Repolarization: Efflux of potassium ions.
Refractory Period: Absolute (200 msec, no response), relative (50 msec, response only to strong stimuli).
Prevents summation and tetany.
Role of Calcium Ions
Extracellular calcium enters during plateau phase, triggers release of more calcium from sarcoplasmic reticulum.
Cardiac muscle is sensitive to extracellular calcium concentrations.
Energy for Cardiac Contractions
Aerobic energy from mitochondrial breakdown of fatty acids and glucose.
Oxygen delivered by circulation; myoglobin stores oxygen in cells.
The Cardiac Cycle
Phases of the Cardiac Cycle
The cardiac cycle includes alternating periods of contraction (systole) and relaxation (diastole) in each chamber.
Atrial Systole: Atria contract, AV valves open, blood ejected into ventricles.
Atrial Diastole: Atria relax.
Ventricular Systole: Ventricles contract, AV valves close, semilunar valves open, blood ejected.
Ventricular Diastole: Ventricles relax, semilunar valves close, AV valves open, ventricles fill passively.
Pressure and Volume Relationships
Blood pressure rises during systole, falls during diastole.
Blood flows from higher to lower pressure, controlled by timing and valves.
At 75 bpm, cardiac cycle lasts about 800 msec.
Heart Sounds
Detected with a stethoscope.
Loud sounds: AV and semilunar valves closing.
Soft sounds: Blood flow and atrial contraction.
Heart Murmur: Sounds from regurgitation through valves.
Cardiac Output
Definition and Formula
Cardiac output (CO) is the volume of blood pumped by the left ventricle per minute.
Formula: Where: = cardiac output (mL/min) = heart rate (beats/min) = stroke volume (mL/beat)
Stroke Volume
Formula: Where: = end-diastolic volume (amount in ventricle at end of diastole) = end-systolic volume (amount remaining after systole)
Ejection Fraction: Percentage of EDV ejected during contraction.
Factors Affecting Cardiac Output
Heart Rate: Influenced by autonomic activity and hormones.
Stroke Volume: Influenced by EDV (filling time, venous return) and ESV (preload, contractility, afterload).
Autonomic Regulation
Cardiac Plexus: Innervates heart.
Vagus Nerves: Carry parasympathetic fibers.
Cardiac Centers (Medulla Oblongata):
Cardioacceleratory center: Sympathetic, increases HR.
Cardioinhibitory center: Parasympathetic, decreases HR.
Cardiac Reflexes: Baroreceptors and chemoreceptors monitor blood pressure and gas levels.
Autonomic Tone: Maintained by dual innervation and neurotransmitter release.
Effects on Pacemaker Cells
Acetylcholine (ACh): Parasympathetic, decreases HR.
Norepinephrine (NE): Sympathetic, increases HR.
Bainbridge Reflex
Adjusts HR in response to increased venous return.
Stretch receptors in right atrium trigger increased HR via sympathetic activity.
Hormonal Effects
HR increased by epinephrine, norepinephrine, thyroid hormone.
Factors Affecting Stroke Volume
EDV: Filling time and venous return.
Preload: Degree of ventricular stretching during diastole.
Frank–Starling Principle: As EDV increases, stroke volume increases.
ESV: Preload, contractility, afterload.
Contractility: Force produced during contraction, affected by autonomic activity and hormones.
Afterload: Tension required to open semilunar valve and eject blood; increased afterload decreases stroke volume.
Summary of Cardiac Output Control
Heart Rate: Controlled by autonomic nervous system, hormones, venous return, stretch receptors.
Stroke Volume: Controlled by EDV (filling time, venous return) and ESV (preload, contractility, afterload).
Cardiac Reserve
Difference between resting and maximal cardiac output.
Cardiovascular regulation ensures adequate circulation during changing activity and emergencies.
