 Back
BackThe Integumentary System: Structure, Function, and Clinical Aspects
Study Guide - Smart Notes

The Integumentary System
Overview of the Skin (Integument)
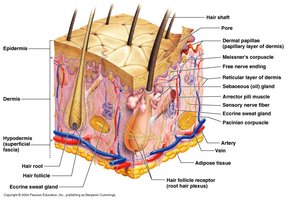
The integumentary system is composed of the skin and its derivatives (hair, nails, glands). The skin itself consists of three major regions: the epidermis (outermost layer), dermis (middle layer), and hypodermis (deepest layer, not technically part of the skin). Each region has distinct structures and functions essential for protection, sensation, and homeostasis.
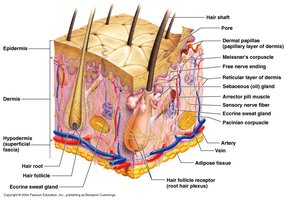
Epidermis
Structure and Cell Types
The epidermis is a keratinized stratified squamous epithelium, consisting of four main cell types and four or five layers (depending on skin thickness). The primary cell types are:
Keratinocytes: Produce keratin, a protein that provides strength and waterproofing.
Melanocytes: Synthesize melanin pigment, which protects against UV radiation.
Langerhans’ cells: Dendritic cells involved in immune defense.
Merkel cells: Sensory receptors for touch.
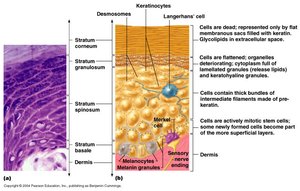
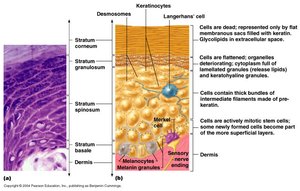
Layers of the Epidermis
The layers of the epidermis (from deep to superficial) are:
Stratum Basale: Single row of mitotically active keratinocytes; contains melanocytes and Merkel cells.
Stratum Spinosum: Several layers of keratinocytes connected by desmosomes; contains Langerhans’ cells and melanin granules.
Stratum Granulosum: Three to five layers where keratinocytes undergo significant changes; keratohyaline and lamellated granules accumulate.
Stratum Lucidum (only in thick skin): Thin, clear layer of dead keratinocytes.
Stratum Corneum: Outermost layer; many layers of dead, keratinized cells providing waterproofing and protection.
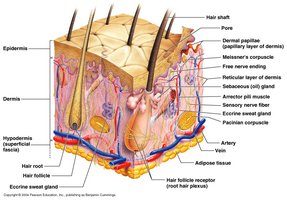
Dermis
Structure and Layers
The dermis is a strong, flexible connective tissue layer beneath the epidermis. It contains fibroblasts, macrophages, mast cells, and white blood cells. The dermis is divided into two layers:
Papillary Layer: Superficial, areolar connective tissue with dermal papillae (projections containing capillaries, Meissner’s corpuscles, and free nerve endings).
Reticular Layer: Deeper, dense irregular connective tissue; provides strength, extensibility, and elasticity due to collagen and elastin fibers.
Dermal Modifications
Friction Ridges: Formed by dermal papillae atop dermal ridges, creating fingerprints; enhance grip and tactile sensation.

Cleavage (Tension) Lines: Patterns of collagen fiber bundles; important for surgical incisions as cuts parallel to these lines heal better.
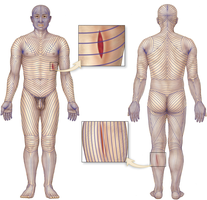
Flexure Lines: Dermal folds at or near joints where the skin is tightly bound to underlying structures (e.g., palms, fingers).
Hypodermis (Superficial Fascia)
The hypodermis is a subcutaneous layer deep to the skin, composed mainly of adipose and areolar connective tissue. It anchors the skin to underlying tissues, provides insulation, and stores energy.
Skin Color
Pigments Contributing to Skin Color
Melanin: Produced by melanocytes; protects DNA from UV damage. Amount and type determine skin color.
Carotene: Yellow to orange pigment, most visible in palms and soles; can be converted to vitamin A.
Hemoglobin: Oxygenated pigment in red blood cells; gives fair skin a pinkish hue.
Clinical Deviations in Skin Color
Cyanosis: Blue skin due to low oxygenation of hemoglobin.
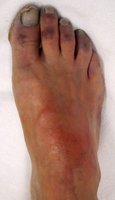
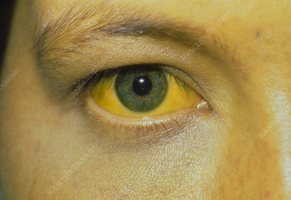
Jaundice: Yellow skin/eyes due to bilirubin accumulation from liver disorders.
Cutaneous Glands
Types of Glands
Ceruminous glands: Modified apocrine glands in the ear canal; secrete cerumen (earwax).
Mammary glands: Specialized sweat glands that secrete milk.
Clinical: Acne and Sebaceous Gland Disorders
Acne is an infectious inflammation of sebaceous glands, often associated with Propionibacterium acnes. Whiteheads are blocked glands; blackheads result from oxidized secretions. Overactive glands in infants can cause seborrhea (cradle cap).
Structure of a Nail
Nails are scalelike modifications of the epidermis on the distal, dorsal surface of fingers and toes. They protect the tips of digits and aid in picking up small objects.
Clinical View: Nail Disorders
Koilonychia: Spoon-shaped nails, often due to iron deficiency.
Ingrown nails: Nail edge grows into the skin, causing pain and inflammation.
Onychomycosis: Fungal infection of the nail.
Beau’s lines: Horizontal lines indicating severe illness or metabolic stress.
Hair
Structure and Function
Hair consists of dead, keratinized cells produced by hair follicles. It is composed of the shaft (above skin), root (within skin), medulla (core), cortex, and cuticle. Hair color is determined by melanocytes at the base of the follicle.
Functions: Insulation, protection, and sensory input.
Distribution: Found everywhere except palms, soles, lips, nipples, and parts of external genitalia.
Types of Hair
Vellus hair: Fine, pale hair on children and adult females.
Terminal hair: Coarse, long hair of scalp, eyebrows, axillary, and pubic regions.
Hair Thinning and Baldness
Alopecia: Hair thinning in both sexes; can be patchy (areata), total (totalis), or universal (universalis).
Male pattern baldness: Genetically determined, influenced by DHT (dihydrotestosterone).
Functions of the Integumentary System
Protection: Chemical, physical, and mechanical barriers against pathogens and injury.
Body Temperature Regulation: Vasoconstriction, vasodilation, sweating, and shivering maintain temperature homeostasis.
Cutaneous Sensation: Sensory receptors detect touch, pain, and temperature.
Metabolic Functions: Synthesis of vitamin D in dermal blood vessels.
Blood Reservoir: Stores up to 5% of body’s blood volume.
Excretion: Eliminates nitrogenous wastes via sweat.
Clinical: Heat Exhaustion and Heat Stroke
Heat Exhaustion: Characterized by heavy sweating, weakness, and faintness; treated by cooling and hydration.
Heat Stroke: Life-threatening; high body temperature, altered mental state, and dry or moist skin; requires immediate medical attention and rapid cooling.
Skin Cancer
Types and Characteristics
Basal Cell Carcinoma: Most common, least malignant; arises from stratum basale, rarely metastasizes.
Squamous Cell Carcinoma: Arises from keratinocytes of stratum spinosum; can metastasize if untreated.
Melanoma: Cancer of melanocytes; highly metastatic and resistant to chemotherapy.
Burns
Classification
First-degree: Only epidermis damaged; redness, swelling, pain.
Second-degree: Epidermis and upper dermis damaged; blisters present.
Third-degree: Entire thickness of skin destroyed; area appears gray-white, cherry red, or black; no initial pain due to nerve destruction.
Treatment includes debridement, antibiotics, temporary coverings, and skin grafts. Severity is estimated using the "Rule of Nines."
Developmental Aspects of the Integument
Fetal Development
Epidermis develops from ectoderm; dermis and hypodermis from mesoderm.
Lanugo: Fine hair covering fetus.
Vernix caseosa: Sebaceous secretion protecting fetal skin.
Adolescence to Old Age
In adolescence, skin and hair become oilier; acne may develop.
With age, skin thins, becomes dry, loses elasticity, and is more prone to injury and cancer due to decreased cell replacement and immune function.
