 Back
BackThe Male Reproductive System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Male Reproductive System
Introduction to Reproduction and Gonads
Reproduction is the biological process by which new individual organisms are produced. In humans, this involves the replication of genetic material and the formation of specialized sex cells called gametes. The primary reproductive organs, or gonads, are the testes in males and the ovaries in females. These organs are responsible for producing gametes and secreting sex hormones.
Male Reproductive Anatomy
Scrotum
The scrotum is an outpouching of the abdominal wall composed of loose skin, muscle, and fascia. It houses the testes and maintains a temperature approximately 3 degrees Fahrenheit cooler than core body temperature, which is essential for proper sperm development. The two testes are separated by the scrotal septum. The scrotum can adjust its position relative to the body to regulate temperature: it hangs lower in warm conditions and is drawn closer in cooler conditions.
Cryptorchidism: A condition where one or both testes fail to descend into the scrotum, increasing the risk of testicular cancer.
Median raphe: The external seam along the midline of the scrotum, often used as an incision site for vasectomy.
Dartos muscle: Smooth muscle fibers that contract or relax to regulate scrotal size and temperature.
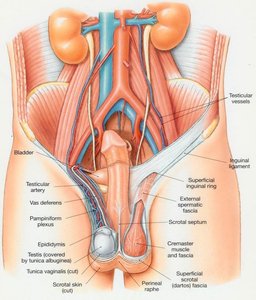
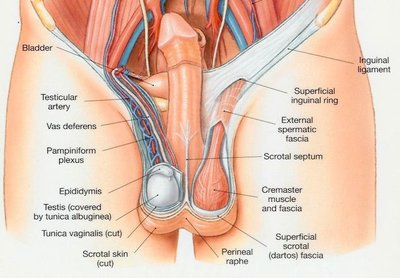
Testes
The testes are paired oval glands located within the scrotum. They are the site of sperm production and testosterone secretion. Each testis is covered by a dense connective tissue layer called the tunica albuginea, which divides the testis into lobules. Each lobule contains tightly coiled seminiferous tubules where spermatogenesis occurs.
Tunica albuginea: Dense fibrous covering that partitions the testis into lobules.
Seminiferous tubules: Site of sperm production.
Rete testis: Network of tubules that collect sperm from seminiferous tubules.
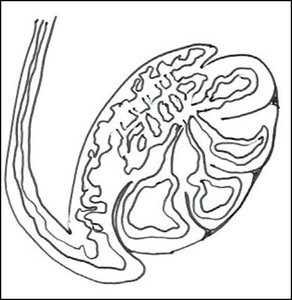
Epididymis and Ductus Deferens
The epididymis is a highly coiled tube (about 20 feet long) where sperm mature and are stored. Sperm move from the seminiferous tubules to the epididymis via the straight tubules and rete testis. The ductus deferens (vas deferens) is a muscular tube that transports sperm from the epididymis to the ejaculatory duct. It ascends from the scrotum through the inguinal canal into the pelvic cavity, looping over the bladder to join the urethra.
Spermatic cord: Contains the ductus deferens, blood vessels, nerves, and the cremaster muscle, which helps regulate testicular temperature.
Vasectomy: Surgical procedure for male sterilization involving cutting and sealing the ductus deferens.
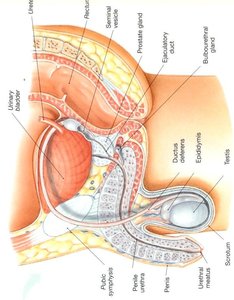
Urethra and Penis
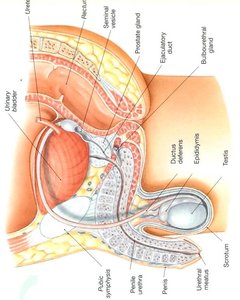
The urethra serves as a common passageway for urine and semen. It is divided into the prostatic urethra (passing through the prostate gland) and the penile urethra (running through the penis). The penis functions in urination and the introduction of sperm into the female reproductive tract. Internally, the penis contains three erectile tissues: two corpora cavernosa and one corpus spongiosum (which surrounds the urethra). Sexual arousal causes these tissues to fill with blood, resulting in an erection.
Glans penis: The enlarged distal end of the penis.
Prepuce (foreskin): The fold of skin covering the glans, often removed during circumcision.
Microscopic Anatomy and Spermatogenesis
Seminiferous Tubules and Supporting Cells
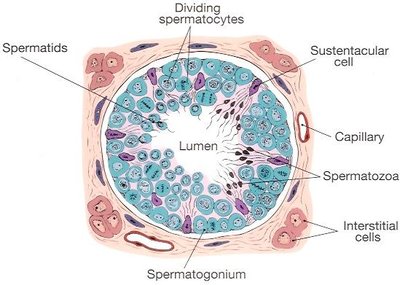
Spermatogenesis, the process of sperm production, occurs within the seminiferous tubules. The tubules are lined with several types of cells:
Spermatogonia: Stem cells located along the basement membrane; undergo mitosis to produce primary spermatocytes.
Primary and secondary spermatocytes: Undergo meiosis to reduce chromosome number.
Spermatids: Haploid cells that differentiate into mature spermatozoa.
Sertoli (sustentacular) cells: Support and nourish developing sperm; form the blood-testis barrier to protect sperm from immune attack.
Interstitial (Leydig) cells: Located between tubules; produce testosterone.
Spermatogenesis Process
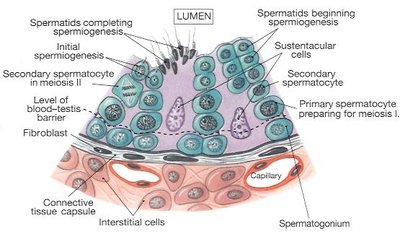
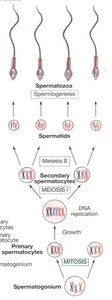
Spermatogenesis is the sequence of events in the seminiferous tubules that produces mature spermatozoa from spermatogonia. The process involves mitosis, meiosis, and spermiogenesis (final maturation).
Stages: Spermatogonia → Primary spermatocytes → Secondary spermatocytes → Spermatids → Spermatozoa
Chromosome number: Diploid (46) in spermatogonia and primary spermatocytes; haploid (23) in spermatids and spermatozoa.
About 300 million sperm are produced daily; they survive about 48 hours in the female reproductive tract.
Anatomy of Spermatozoa
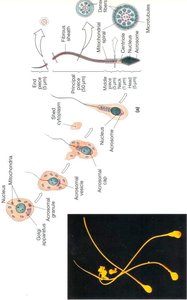
Mature sperm cells, or spermatozoa, have a specialized structure for fertilization:
Head: Contains the nucleus (genetic material) and the acrosome, which has enzymes (e.g., hyaluronidase) to penetrate the egg.
Midpiece: Packed with mitochondria to provide energy for motility.
Tail (flagellum): Propels the sperm forward.
Accessory Glands and Semen
Accessory Glands
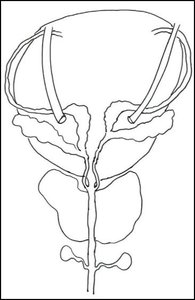
The male reproductive system includes several glands that contribute to the formation of semen:
Seminal vesicles (2): Secrete an alkaline, fructose-rich fluid (about 60% of semen volume) to nourish sperm and neutralize vaginal acidity.
Prostate gland (1): Produces an alkaline fluid (13-33% of semen volume) that enhances sperm motility and viability.
Bulbourethral (Cowper's) glands (2): Secrete a clear, lubricating mucus prior to ejaculation.
Semen
Semen is a mixture of sperm and glandular secretions. It serves as a transport medium, provides nutrients, neutralizes acidic environments, and contains antimicrobial proteins (e.g., seminalplasmin).
Average volume: 2.5 – 6 mL per ejaculation
pH: 7.35–7.50 (slightly basic)
Functions: Transport, capacitation (activation of sperm), and antimicrobial defense
Hormonal Regulation
Hormones of the Male Reproductive System
The anterior pituitary gland secretes hormones that regulate spermatogenesis and testosterone production:
FSH (Follicle Stimulating Hormone): Initiates spermatogenesis and supports sperm maturation.
ICSH (Interstitial Cell Stimulating Hormone, also known as LH): Stimulates Leydig cells to produce testosterone.
Testosterone: Controls development and maintenance of male sex organs, stimulates bone and muscle growth, and is responsible for secondary sex characteristics (e.g., increased body hair, muscle mass, and deepening of the voice).
Additional info: Anabolic steroids can suppress natural testosterone production, leading to testicular shrinkage. Androgen-binding hormone is important for proper sperm development.
