 Back
BackThe Reproductive System: Structure, Function, and Regulation
Study Guide - Smart Notes

Introduction to the Male and Female Reproductive Systems
Overview
The reproductive systems in males and females are responsible for producing gametes, secreting sex hormones, and supporting the processes of fertilization and development. The primary sex organs, or gonads, are the testes in males and the ovaries in females. These organs produce gametes (sperm and ova) and secrete hormones such as testosterone and estrogens. Accessory reproductive organs aid in the transport, nourishment, and protection of gametes.
Gonads: Primary sex organs; testes (males), ovaries (females).
Sex Hormones: Testosterone (males), estrogens (females).
Gametes: Sperm (males), ova (females); produced via meiosis.
Accessory Organs: Ducts, glands, and external genitalia that support reproductive function.
Overview of Meiosis
Chromosome Structure and Genetic Variation
Somatic cells are diploid (2n), containing 46 chromosomes (23 pairs), with one set from each parent. Homologous chromosomes carry the same genes but may have different alleles. Meiosis is the process by which gametes are produced, reducing the chromosome number by half to form haploid (1n) cells.
Homologous Chromosomes: Chromosome pairs with the same genes but possibly different alleles.
Alleles: Variants of a gene found at the same locus on homologous chromosomes.
Fertilization: Fusion of sperm and ovum to form a diploid zygote.
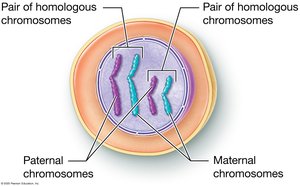
Meiosis Process
Meiosis consists of two sequential divisions: Meiosis I (reduction division) and Meiosis II (equational division). DNA replication precedes meiosis, resulting in sister chromatids joined at the centromere. Chromatin condenses into chromosomes during cell division.
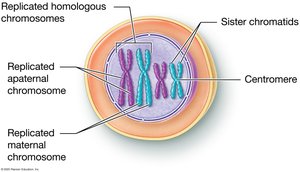
Diploid vs. Haploid Cells
Meiosis reduces the chromosome number by half, producing haploid cells. This ensures that upon fertilization, the zygote has the correct diploid number.
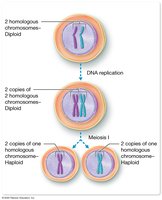
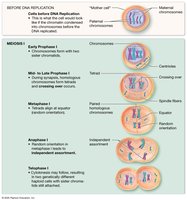
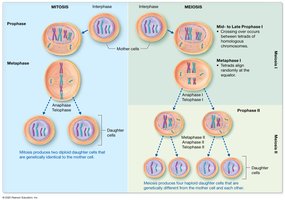
Stages of Meiosis I
Prophase I: Chromatin condenses, homologous chromosomes pair (synapsis), crossing over occurs.
Metaphase I: Homologous pairs align at the cell equator; orientation is random (independent assortment).
Anaphase I: Homologous chromosomes are separated to opposite poles.
Telophase I & Cytokinesis: Two haploid cells are formed, each with unique genetic combinations.
Stages of Meiosis II
Prophase II: Chromosomes condense again if necessary.
Metaphase II: Chromosomes align at the equator.
Anaphase II: Sister chromatids separate.
Telophase II & Cytokinesis: Four genetically unique haploid cells are produced.
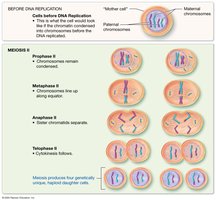
Comparison of Mitosis and Meiosis
Mitosis: Produces two genetically identical diploid cells for growth and repair.
Meiosis: Produces up to four genetically unique haploid gametes for reproduction.
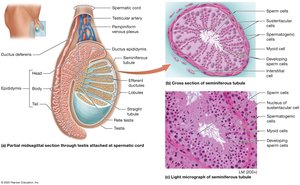
Anatomy of the Male Reproductive System
Testes
The testes are paired organs located in the scrotum, responsible for sperm production and hormone secretion. Internally, each testis contains lobules with seminiferous tubules, where spermatogenesis occurs. Interstitial cells between tubules produce testosterone.
Spermatogenic Cells: Form sperm.
Sustentacular Cells: Support and nourish developing sperm.
Interstitial Cells: Secrete testosterone.
Duct System
Epididymis: Site of sperm maturation and storage.
Ductus (Vas) Deferens: Transports sperm from epididymis to ejaculatory duct.
Ejaculatory Duct: Formed by the union of the ductus deferens and seminal vesicle duct; passes through the prostate.
Urethra: Transports urine and semen through prostatic, membranous, and spongy regions.
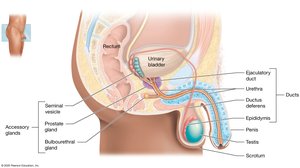
Penis
The penis is the male copulatory organ, containing erectile tissues (corpora cavernosa and corpus spongiosum) that fill with blood during erection. The glans penis is the enlarged tip, and the prepuce (foreskin) may be removed by circumcision.
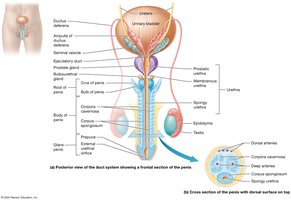
Accessory Sex Glands
Seminal Vesicles: Secrete fructose-rich fluid, prostaglandins, and coagulating proteins.
Prostate Gland: Secretes citrate, prostate-specific antigen (PSA), and antimicrobial chemicals.
Bulbourethral Glands: Secrete alkaline mucus to neutralize urine and lubricate the urethra.
Support Structures: Scrotum and Spermatic Cord
The scrotum houses the testes and regulates their temperature. The spermatic cord contains the ductus deferens, blood vessels, nerves, and the cremaster muscle, which adjusts testicular position for temperature regulation.
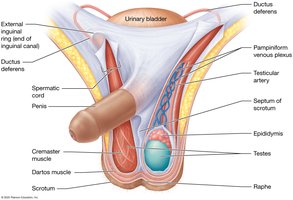
Spermatogenesis and Spermiogenesis
Spermatogenesis
Spermatogenesis is the process of sperm cell development, beginning at puberty and continuing throughout life. It occurs in the seminiferous tubules and involves mitosis, meiosis, and maturation.
Spermatogonia: Diploid stem cells that divide by mitosis.
Primary Spermatocytes: Undergo meiosis I to form secondary spermatocytes.
Secondary Spermatocytes: Undergo meiosis II to form spermatids.
Spermatids: Differentiate into mature sperm cells during spermiogenesis.
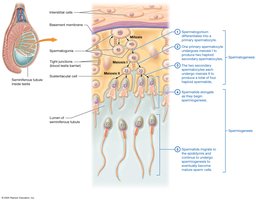
Spermiogenesis
Spermiogenesis is the maturation of spermatids into spermatozoa, involving the formation of the acrosome, flagellum, and condensation of the nucleus.
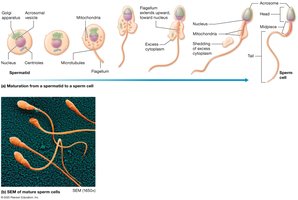
Hormonal Control of Male Reproduction
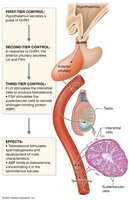
Hypothalamic-Pituitary-Gonadal (HPG) Axis
The HPG axis regulates testosterone production and spermatogenesis through a multi-tiered feedback loop involving GnRH, LH, and FSH.
GnRH: Released from the hypothalamus; stimulates anterior pituitary.
LH: Stimulates interstitial cells to produce testosterone.
FSH: Stimulates sustentacular cells to support spermatogenesis.
Inhibin: Inhibits FSH secretion.
Anatomy of the Female Reproductive System
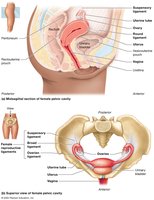
Internal Organs
The female reproductive system includes the ovaries, uterine tubes, uterus, and vagina. These organs are primarily located in the pelvic cavity and are supported by various ligaments.
Ovaries: Produce oocytes and secrete hormones (estrogens, progesterone).
Uterine Tubes (Fallopian Tubes): Transport oocytes from the ovary to the uterus.
Uterus: Site of implantation and fetal development; source of menstrual flow.
Vagina: Receives the penis during intercourse; serves as the birth canal.
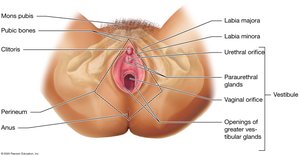
External Genitalia (Vulva)
Mons Pubis: Fatty area over the pubic symphysis.
Labia Majora and Minora: Skin folds that protect the vestibule.
Clitoris: Erectile tissue important in sexual response.
Perineum: Region between the vulva and anus.
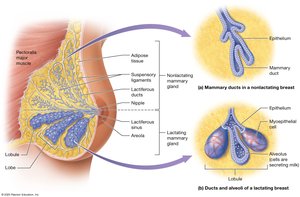
Mammary Glands
Mammary glands are modified sweat glands that produce milk. Each breast contains 15–25 lobes with lobules and alveoli for milk production, and ducts for milk transport.
Oogenesis and the Ovarian Cycle
Oogenesis
Oogenesis is the process of ovum development, beginning before birth and continuing until menopause. It involves mitosis, meiosis, and maturation, with most oocytes arrested in prophase I until puberty.
Oogonia: Stem cells that divide by mitosis before birth.
Primary Oocytes: Arrested in prophase I until puberty.
Secondary Oocyte: Released during ovulation; completes meiosis II only if fertilized.
Polar Bodies: Small cells that degenerate.
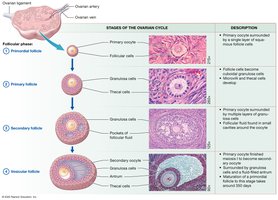
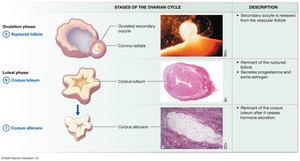
Ovarian Cycle
The ovarian cycle consists of the follicular phase (follicle growth), ovulation (release of secondary oocyte), and luteal phase (formation of corpus luteum). Hormonal regulation involves GnRH, LH, FSH, estrogens, and progesterone.
The Uterine (Menstrual) Cycle
Phases of the Uterine Cycle
Menstrual Phase (Days 1–5): Shedding of the stratum functionalis.
Proliferative Phase (Days 6–14): Regeneration of the endometrium; ends with ovulation.
Secretory Phase (Days 15–28): Endometrium prepares for implantation; if no fertilization, cycle restarts.
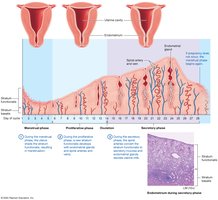
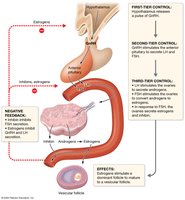
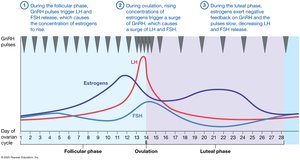
Hormonal Regulation of the Female Reproductive Cycles
Hormonal interplay between the hypothalamus, pituitary gland, and ovaries regulates both the ovarian and uterine cycles. Estrogens and progesterone provide feedback to modulate GnRH, LH, and FSH secretion.
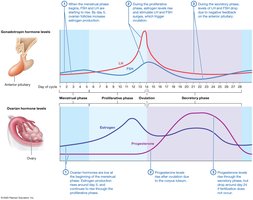
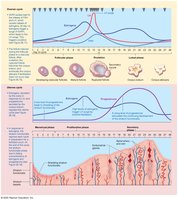
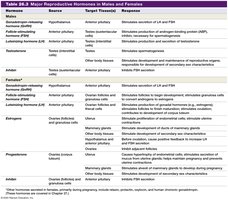
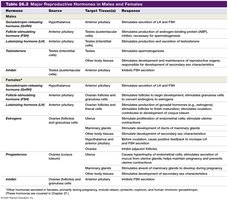
Major Reproductive Hormones in Males and Females
Hormone | Source | Target Tissue(s) | Response |
|---|---|---|---|
GnRH | Hypothalamus | Anterior pituitary | Stimulates secretion of LH and FSH |
LH | Anterior pituitary | Testes, Ovaries | Stimulates testosterone/estrogen production, ovulation |
FSH | Anterior pituitary | Testes, Ovaries | Stimulates spermatogenesis, follicle development |
Testosterone | Testes | Various | Male secondary sex characteristics, spermatogenesis |
Estrogens | Ovaries | Various | Female secondary sex characteristics, endometrial growth |
Progesterone | Ovaries | Uterus, mammary glands | Maintains endometrium, prepares for pregnancy |
Inhibin | Testes, Ovaries | Anterior pituitary | Inhibits FSH secretion |
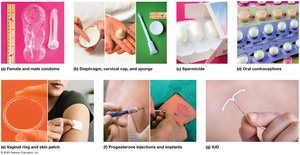
Methods of Birth Control
Temporary Methods
Behavioral: Abstinence, rhythm method, withdrawal.
Barrier: Condoms, diaphragms, cervical caps, sponges, spermicides.
Hormonal: Oral contraceptives, mini-pill, vaginal rings, skin patches, injections, implants.
Intrauterine: IUDs and IUSs.
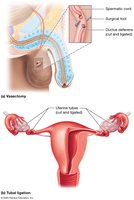
Permanant Methods (Sterilization)
Vasectomy: Male sterilization by cutting and sealing the ductus deferens.
Tubal Ligation: Female sterilization by cutting and sealing the uterine tubes.
Tubal Implants: Metal springs placed in uterine tubes to block them.
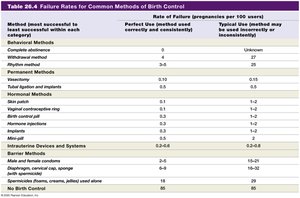
Effectiveness of Birth Control Methods
Method | Perfect Use Failure Rate (%) | Typical Use Failure Rate (%) |
|---|---|---|
Abstinence | 0 | Unknown |
Male Condom | 2 | 18 |
Oral Contraceptives | 0.3 | 9 |
IUD | 0.2-0.8 | 0.2-0.8 |
Vasectomy | 0.1 | 0.15 |
No Birth Control | 85 | 85 |
Other methods... | See table | See table |
Sexually Transmitted Infections (STIs)
Bacterial and Parasitic STIs
Chlamydia: Caused by Chlamydia trachomatis; often asymptomatic, can cause infertility.
Gonorrhea: Caused by Neisseria gonorrhoeae; symptoms include painful urination and discharge.
Syphilis: Caused by Treponema pallidum; progresses through multiple stages, can be fatal if untreated.
Trichomoniasis: Caused by Trichomonas vaginalis; may cause discharge and irritation.
Viral STIs
Genital Warts (HPV): Most common STI; some strains cause cervical cancer.
Genital Herpes: Caused by Herpes Simplex Virus Type 2; causes painful blisters, increases risk of HIV.
Cervical Cancer
Cervical cancer is often caused by HPV infection and is detected by Pap smear screening. Early detection and vaccination are key to prevention.

