 Back
BackThe Reproductive System: Structure, Function, and Development
Study Guide - Smart Notes

The Reproductive System
Overview and Purpose
The reproductive system is essential for the continuation of species, enabling the production of offspring through the fusion of male and female gametes. It consists of primary sex organs (gonads) and accessory structures, with distinct anatomical and functional differences between males and females.
Gonads: Testes in males, ovaries in females; produce gametes and hormones.
Gametes: Sperm (male, XY), Ova (female, XX).
Accessory Organs: Structures supporting gamete transport, fertilization, and development.
Purpose: Production of sperm and eggs, fertilization, and development of the embryo/fetus.
Anatomy of the Male Reproductive System
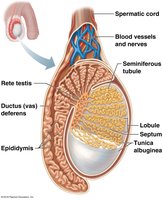
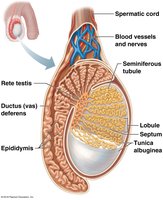
Testes
The testes are the primary male reproductive organs, responsible for sperm and testosterone production. They are located in the scrotum, outside the body, to maintain a temperature optimal for spermatogenesis.
Structure: Divided into lobules containing seminiferous tubules (site of spermatogenesis).
Interstitial Cells: Produce androgens, mainly testosterone.
Spermatic Cord: Contains blood vessels, nerves, and the ductus (vas) deferens.
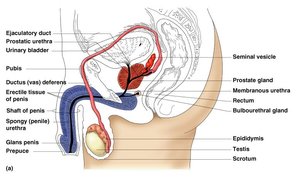
Accessory Organs
Accessory glands and external genitalia support sperm maturation, nourishment, and delivery.
Seminal Vesicles: Produce nutrient-rich fluid for sperm.
Prostate Gland: Secretes alkaline fluid to protect and activate sperm.
Bulbourethral (Cowper’s) Glands: Release mucus to neutralize urine in the urethra.
External Genitalia: Penis (sperm delivery), scrotum (testes housing).
Duct System
The duct system transports sperm from the testes to the exterior.
Epididymis: Sperm maturation and storage.
Vas Deferens: Transports sperm via peristalsis; site of vasectomy for sterilization.
Urethra: Common pathway for urine and sperm; internal sphincter prevents mixing during ejaculation.
Spermatogenesis and Spermiogenesis
Spermatogenesis is the process of sperm production, regulated by hormones. Spermiogenesis is the maturation of spermatids into sperm.
FSH: Stimulates Sertoli cells for spermatogenesis.
LH: Stimulates Leydig cells for testosterone production.
Meiosis: Reduces chromosome number to haploid (n = 23).
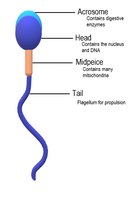
Sperm Structure: Head (nucleus, acrosome), midpiece (mitochondria), tail (motility).
Anatomy of the Female Reproductive System
Ovaries
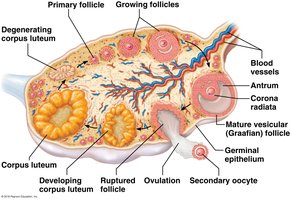
The ovaries are the primary female sex organs, producing eggs and hormones (estrogen, progesterone). They contain ovarian follicles at various stages of development.
Oocyte: Immature egg cell within follicles.
Follicle Development: Primary follicle, vesicular (Graafian) follicle, ovulation, corpus luteum.
Ligaments: Suspensory, ovarian, and broad ligaments hold ovaries in place.
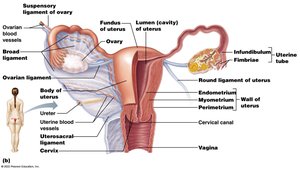
Female Duct System
The duct system includes the uterine tubes, uterus, and vagina, facilitating egg transport, fertilization, and childbirth.
Uterine (Fallopian) Tubes: Site of fertilization; fimbriae sweep egg into tube.
Uterus: Supports implantation and development; regions include body, fundus, cervix.
Vagina: Birth canal, menstrual flow exit, receives penis during intercourse.
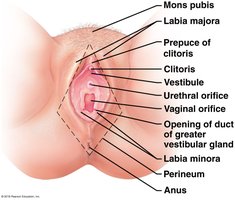
External Genitalia
The vulva encompasses the external female genital organs, including the mons pubis, labia, clitoris, and vestibular glands.
Mons Pubis: Fatty area over pubic bone.
Labia: Folds surrounding vaginal opening.
Clitoris: Highly sensitive erectile tissue.
Perineum: Area between vaginal opening and anus.
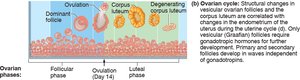
Female Reproductive Functions and Cycles
Hormonal Regulation
Estrogen and progesterone regulate the menstrual cycle and secondary sex characteristics. FSH and LH from the pituitary control ovarian hormone production.
Estrogen: Development of breasts, pubic hair, fat distribution, onset of menses.
Progesterone: Maintains pregnancy, prepares breasts for lactation.
Uterine (Menstrual) Cycle
The menstrual cycle consists of three phases, regulated by ovarian hormones.
Menstrual Phase (Days 0–4): Shedding of endometrial lining.
Proliferative Phase (Days 5–14): Regeneration and thickening of endometrium; ovulation occurs.
Secretory Phase (Days 15–28): Endometrium prepares for implantation; if no fertilization, menstruation begins.
Fertilization and Early Development
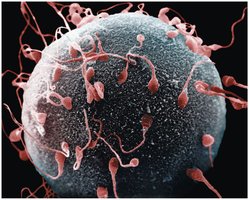
Fertilization Process
Fertilization occurs when a sperm cell fuses with an oocyte, forming a zygote. The zygote undergoes cell division and develops into an embryo and then a fetus.
Oocyte Viability: Up to 24 hours after ovulation.
Sperm Viability: Up to 48 hours after ejaculation.
Acrosomal Reaction: Sperm enzymes digest oocyte membrane for fusion.
Zygote Formation: Union of haploid gametes (n = 23) creates diploid zygote (2n = 46).
Pregnancy and Embryonic Development
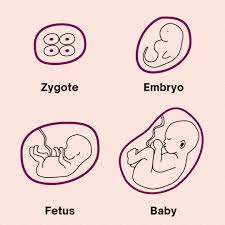
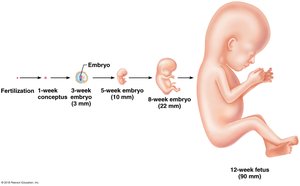
Stages of Development
Pregnancy is the period from fertilization to birth, with distinct stages of embryonic and fetal development.
Embryo: Fertilization to week 8.
Fetus: Week 9 to birth.
Gestation Period: Approximately 280 days from last menstrual period.
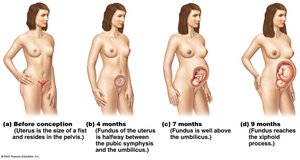
Effects of Pregnancy on the Mother
Pregnancy induces anatomical and physiological changes in the mother, affecting multiple organ systems.
Anatomical: Uterus enlargement, lumbar curvature, ligament relaxation.
Gastrointestinal: Morning sickness, heartburn, constipation.
Urinary: Increased urine production, bladder compression.
Respiratory: Congested mucosa, increased vital capacity, dyspnea.
Cardiovascular: Increased blood volume, blood pressure, varicose veins.
Childbirth
Initiation and Stages of Labor
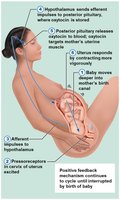
Labor is the process of expelling the infant from the uterus, initiated by hormonal changes and positive feedback mechanisms.
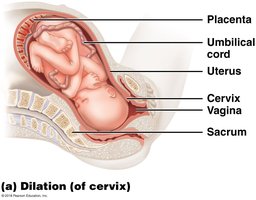
Stage 1: Dilation – Cervix dilates, contractions begin, amnion ruptures.
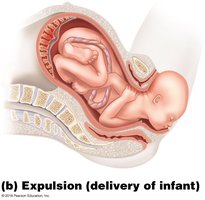
Stage 2: Expulsion – Infant passes through cervix and vagina; normal delivery is head-first.
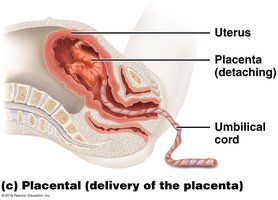
Stage 3: Placental – Delivery of placenta and fetal membranes.
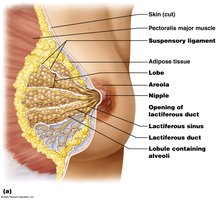
Mammary Glands and Lactation
Structure and Function
Mammary glands are modified sweat glands that produce milk to nourish newborns. They are stimulated by estrogens and progesterone during pregnancy.
Colostrum: First milk, rich in nutrients and antibodies.
Lactation: Essential for infant nutrition and immunity.
Developmental Aspects of the Reproductive System
Puberty and Menopause
Reproductive system development is regulated by genetic and hormonal factors, with distinct changes at puberty and menopause.
Puberty: Onset of reproductive function; males (testes/scrotum enlargement), females (breast development, menarche).
Menopause: Cessation of menstruation and ovarian function; symptoms include hot flashes and mood changes.

Contraception
Methods and Mechanisms
Contraception includes various methods to prevent pregnancy, each with distinct mechanisms and effectiveness.
Hormonal: Birth control pills, emergency contraceptives.
Surgical: Tubal ligation (female), vasectomy (male).
Barrier: Diaphragms, condoms.
Abstinence: Only method 100% effective.
Method | Mechanism | Effectiveness |
|---|---|---|
Birth Control Pill | Suppresses ovulation | High |
Morning-after Pill | Disrupts hormonal signals | Moderate |
Tubal Ligation | Blocks uterine tubes | High |
Vasectomy | Blocks vas deferens | High |
Condoms | Physical barrier | Moderate |
Abstinence | No intercourse | 100% |
Additional info: All content is expanded and structured for academic completeness and clarity, suitable for college-level study.
