 Back
BackThe Reproductive System: Structure, Function, and Gametogenesis
Study Guide - Smart Notes

The Reproductive System
Overview of the Reproductive System
The reproductive system is responsible for producing offspring and ensuring the continuation of genetic material. It consists of primary sex organs (gonads), accessory reproductive organs, and sex hormones. The male and female reproductive systems have distinct structures and functions but share the common goal of gamete production and hormone secretion.
Primary sex organs (gonads): Testes in males, ovaries in females. These produce gametes (sperm and ova) and secrete sex hormones.
Accessory reproductive organs: Ducts, glands, and external genitalia that support gamete transport and fertilization.
Sex hormones: Androgens (testosterone) in males; estrogens and progesterone in females.
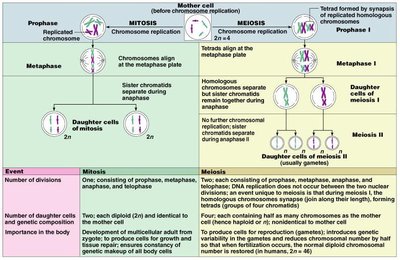
Comparison of Mitosis and Meiosis
Cell Division in Gametogenesis
Gamete formation involves specialized cell divisions. Mitosis produces genetically identical cells for growth and repair, while meiosis produces haploid gametes with genetic variation.
Event | Mitosis | Meiosis |
|---|---|---|
Number of divisions | One | Two (Meiosis I & II) |
Number of daughter cells and genetic composition | Two diploid (2n), identical to parent | Four haploid (n), genetically unique |
Role in the body | Growth, repair, asexual reproduction | Gamete production, genetic diversity |
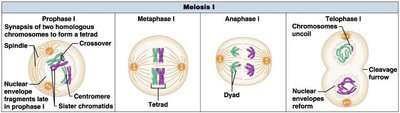
Meiosis I: Reductional Division
Meiosis I reduces the chromosome number by half, separating homologous chromosomes. Key events include synapsis, crossing over, and segregation of homologs.
Prophase I: Homologous chromosomes pair and exchange genetic material (crossing over).
Metaphase I: Tetrads align at the metaphase plate.
Anaphase I: Homologous chromosomes separate.
Telophase I: Two haploid cells form.
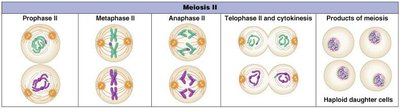
Meiosis II: Equational Division
Meiosis II resembles mitosis, separating sister chromatids to produce four haploid cells.
Prophase II: Chromosomes condense again in two cells.
Metaphase II: Chromosomes align at the metaphase plate.
Anaphase II: Sister chromatids separate.
Telophase II and Cytokinesis: Four genetically unique haploid cells result.
Male Reproductive System
Anatomy and Duct System
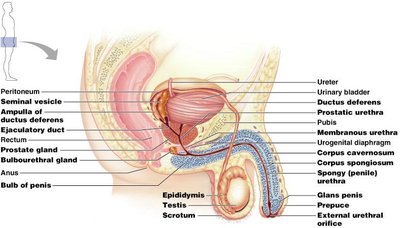
The male reproductive system includes the testes, duct system, accessory glands, and penis. The testes produce sperm, which travel through a series of ducts and are mixed with glandular secretions to form semen.
Testes: Site of sperm production and testosterone secretion.
Duct system: Epididymis, ductus deferens (vas deferens), ejaculatory duct, and urethra transport sperm.
Accessory glands: Seminal vesicles, prostate gland, and bulbourethral glands contribute fluids to semen.
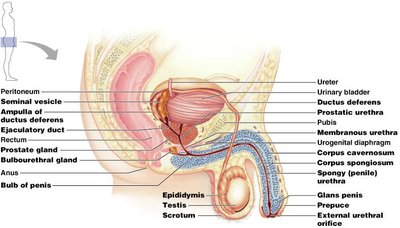
The Penis and Erectile Tissue
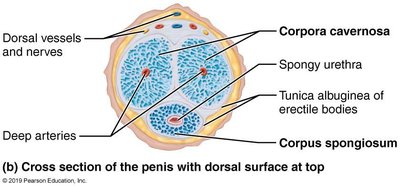
The penis contains three cylindrical bodies of erectile tissue: two corpora cavernosa and one corpus spongiosum. These tissues fill with blood during erection, facilitating copulation and sperm delivery.
Corpus spongiosum: Surrounds the urethra and forms the glans penis.
Corpora cavernosa: Paired dorsal erectile bodies.
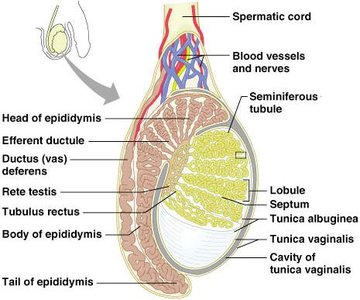
The Testes and Seminiferous Tubules
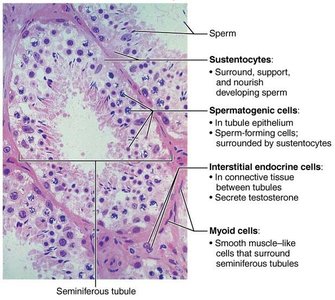
The testes are divided into lobules containing seminiferous tubules, where spermatogenesis occurs. Interstitial cells between tubules secrete testosterone.
Seminiferous tubules: Sperm production.
Interstitial (Leydig) cells: Testosterone secretion.
Epididymis, Ductus Deferens, and Ejaculatory Duct
The epididymis stores and matures sperm. During ejaculation, sperm travel through the ductus deferens, which joins the seminal vesicle duct to form the ejaculatory duct, propelling sperm into the urethra.
Epididymis: Sperm maturation and storage.
Ductus deferens: Sperm transport; site of vasectomy for birth control.
Accessory Glands and Semen
Accessory glands produce seminal fluid, which nourishes and protects sperm. Semen is a mixture of sperm and glandular secretions.
Seminal vesicles: Produce alkaline fluid with fructose and prostaglandins.
Prostate gland: Secretes milky, slightly acidic fluid with enzymes and PSA.
Bulbourethral glands: Secrete mucus to neutralize acidic urine in the urethra.
Semen: Contains nutrients, enzymes, and hormones to support sperm function.
Female Reproductive System
Female Reproductive Anatomy
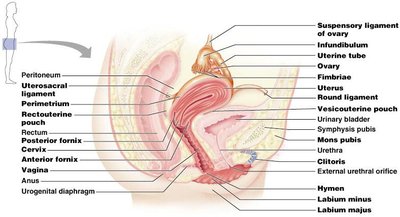
The female reproductive system includes the ovaries, uterine tubes, uterus, vagina, and external genitalia. The ovaries produce ova and secrete hormones, while the accessory ducts transport gametes and support fertilization and development.
Ovaries: Produce ova and hormones (estrogen, progesterone).
Uterine tubes (fallopian tubes): Site of fertilization; transport oocyte to uterus.
Uterus: Site of implantation and fetal development.
Vagina: Birth canal and organ of copulation.
External genitalia (vulva): Includes mons pubis, labia, clitoris, and vestibular structures.
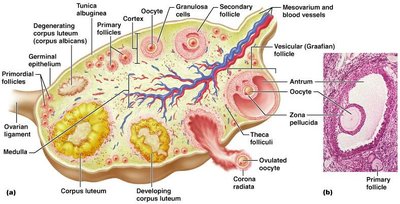
Ovarian Follicles and Ovulation
Ovarian follicles are structures within the ovary that contain developing oocytes. Follicles mature through several stages, culminating in ovulation, the release of an oocyte.
Primordial follicle: Single layer of squamous cells around oocyte.
Primary follicle: Multiple layers of granulosa cells.
Secondary follicle: Fluid-filled antrum forms.
Graafian (vesicular) follicle: Mature follicle ready for ovulation.
Corpus luteum: Remnant of follicle after ovulation; secretes hormones.
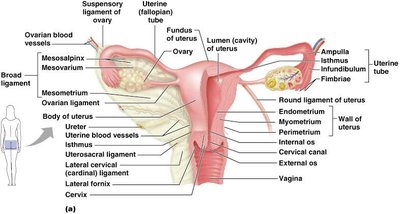
Uterine Tubes, Uterus, and Vagina
The uterine tubes capture the ovulated oocyte and are the site of fertilization. The uterus supports embryo implantation and development, while the vagina serves as the birth canal and organ of copulation.
Uterine wall layers: Perimetrium (outer), myometrium (muscle), endometrium (inner, sheds during menstruation).
Cervix: Lower part of uterus, produces mucus to regulate sperm entry.
External Genitalia and Mammary Glands
The external genitalia (vulva) protect the internal reproductive organs and include structures homologous to male genitalia. Mammary glands are modified sweat glands that produce milk for newborns.
Clitoris: Erectile tissue homologous to the penis.
Mammary glands: Consist of lobes and ducts for milk production and delivery.
Gametogenesis: Spermatogenesis and Oogenesis
Spermatogenesis
Spermatogenesis is the process of sperm production in the seminiferous tubules of the testes. It involves mitosis, meiosis, and spermiogenesis (maturation of spermatids into spermatozoa).
Spermatogonia: Stem cells that divide by mitosis.
Primary spermatocytes: Undergo meiosis I to form secondary spermatocytes.
Secondary spermatocytes: Undergo meiosis II to form spermatids.
Spermiogenesis: Spermatids mature into spermatozoa.
Oogenesis
Oogenesis is the production of female gametes (ova) in the ovaries. It begins before birth, pauses, and resumes at puberty, producing one functional ovum and polar bodies.
Oogonia: Stem cells divide by mitosis during fetal development.
Primary oocytes: Begin meiosis but arrest in prophase I until puberty.
Secondary oocyte: Completes meiosis I at ovulation; meiosis II is completed only if fertilization occurs.
Hormonal Regulation of Reproduction (EXAM!!!!)
Gonadotropins and the HPG Axis
The hypothalamic-pituitary-gonadal (HPG) axis regulates reproductive function through the release of hormones.
GnRH (gonadotropin-releasing hormone): Released by the hypothalamus; stimulates FSH and LH secretion from the anterior pituitary.
FSH (follicle-stimulating hormone): Stimulates gamete production in both sexes.
LH (luteinizing hormone): Triggers ovulation in females and testosterone production in males.
Feedback inhibition: Rising sex hormone levels inhibit GnRH, FSH, and LH release.
Ovarian and Uterine (Menstrual) Cycles
Ovarian Cycle
The ovarian cycle consists of the follicular phase (follicle growth), ovulation, and luteal phase (corpus luteum activity). Hormonal changes regulate the maturation and release of oocytes.
Follicular phase (days 1–14): Follicle growth and estrogen production.
Ovulation (day 14): Release of secondary oocyte.
Luteal phase (days 14–28): Corpus luteum secretes progesterone and estrogen.
Know how the hormones correlate with this
Uterine (Menstrual) Cycle
The uterine cycle describes cyclic changes in the endometrium in response to ovarian hormones.
Menstrual phase (days 1–5): Shedding of the functional layer of the endometrium.
Proliferative phase (days 6–14): Endometrium rebuilds under estrogen influence.
Secretory phase (days 15–28): Endometrium prepares for implantation under progesterone influence.
Both the menstrual and proliferative phases occur before ovulation, and toghether they correspond to the follicular phase of the ovarian cycle. The secretory phase corresponds in time to the lutel phase of the ovarian cycle
Know how the hormones correlate with this
Summary Table: Key Differences Between Mitosis and Meiosis
Feature | Mitosis | Meiosis |
|---|---|---|
Number of divisions | 1 | 2 |
Number of daughter cells | 2 (diploid, identical) | 4 (haploid, unique) |
Role | Growth, repair | Gamete production |
