 Back
BackThe Respiratory System: Structure, Function, and Clinical Aspects
Study Guide - Smart Notes

The Respiratory System
Overview and Learning Outcomes
The respiratory system is essential for gas exchange, supplying oxygen to the body and removing carbon dioxide. This system includes anatomical structures and physiological processes that ensure efficient ventilation and gas transport. Understanding its anatomy, function, and related diseases is crucial for students of anatomy and physiology.
Anatomy of the Respiratory System
Main Components
Lungs: Paired, spongy organs located in the thoracic cavity, protected by the rib cage and diaphragm.
Respiratory Tract: Series of hollow passages conducting air to and from the lungs.
Blood Vessels: Pulmonary circuit vessels facilitate gas exchange between lungs and blood.
Respiratory Muscles: Diaphragm and intercostal muscles drive ventilation.
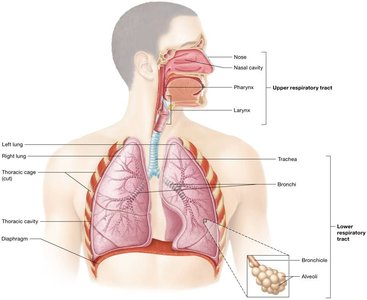
Divisions of the Respiratory Tract
Upper Respiratory Tract: Nose, nasal cavity, pharynx, and larynx.
Lower Respiratory Tract: Trachea, bronchi, bronchioles, and alveoli.
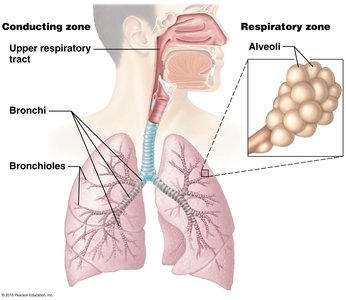
Functional Zones
Conducting Zone: Passages that conduct air into and out of the lungs (nose to terminal bronchioles).
Respiratory Zone: Sites of gas exchange (respiratory bronchioles, alveolar ducts, and alveoli).
Basic Functions of the Respiratory System
Primary Functions
Ventilation: Movement of air in and out of the lungs.
Gas Exchange: Exchange of O2 and CO2 between alveoli and blood (external respiration) and between blood and tissues (internal respiration).
Gas Transport: Movement of respiratory gases in the blood.
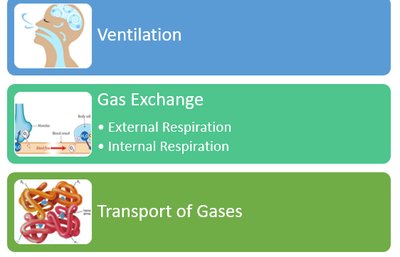
Other Functions
Speech and sound production
Olfaction (sense of smell)
Assistance in defecation, urination, and childbirth by increasing thoracic pressure

Facilitates venous and lymphatic return
Maintains acid-base balance (pH) in extracellular fluid
Synthesizes angiotensin-II, important for blood pressure regulation

Detailed Anatomy of the Respiratory System
Nose and Nasal Cavity
The nose and nasal cavity filter, warm, and humidify incoming air. The nasal cavity is lined with mucosa and contains structures such as conchae and meatuses to increase surface area and turbulence.
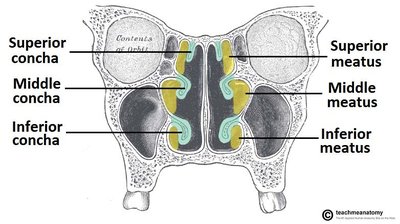
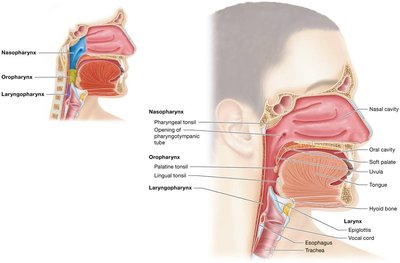
Pharynx and Larynx
The pharynx (throat) is a muscular tube that serves as a passageway for air and food. The larynx (voice box) is involved in sound production and protects the lower airways.
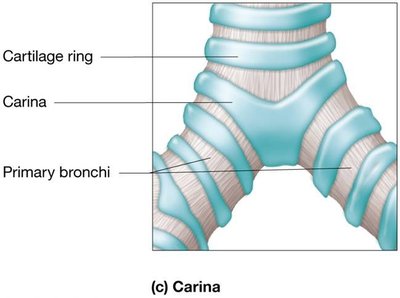
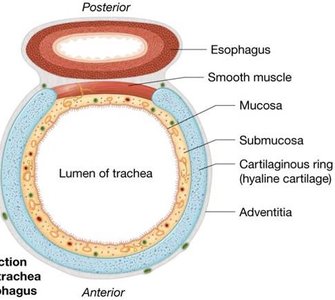
Trachea and Bronchial Tree
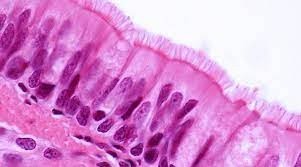
The trachea (windpipe) is supported by C-shaped cartilaginous rings and lined with ciliated pseudostratified columnar epithelium and goblet cells. The carina is a sensitive area that triggers the cough reflex if foreign material is detected.
Bronchi and Bronchioles
The bronchial tree branches into smaller bronchi and bronchioles, conducting air deeper into the lungs. Terminal bronchioles mark the end of the conducting zone.
Alveoli and Respiratory Zone
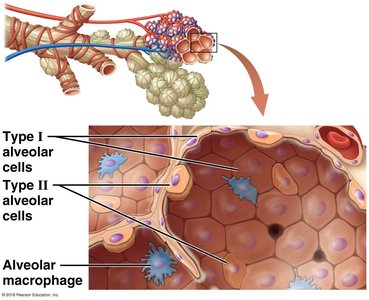
Alveoli are tiny air sacs where gas exchange occurs. They are surrounded by pulmonary capillaries and elastic fibers, and contain three main cell types:
Type I alveolar cells: Thin squamous cells for rapid gas diffusion.
Type II alveolar cells: Cuboidal cells that produce surfactant to reduce surface tension and prevent alveolar collapse.
Alveolar macrophages: Phagocytes that remove debris and pathogens.
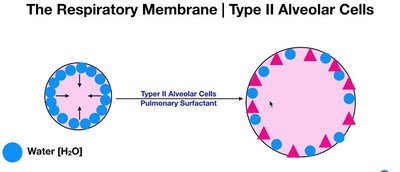
Surfactant and Alveolar Stability
Surfactant, produced by Type II alveolar cells, lowers surface tension in the alveoli, preventing collapse and making breathing easier. Deficiency in surfactant leads to conditions such as Infant Respiratory Distress Syndrome (IRDS).
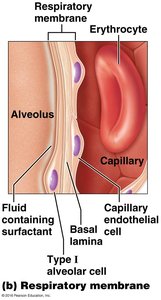
Respiratory Membrane
The respiratory membrane is the site of gas exchange and consists of the fused membranes of Type I alveolar cells and capillary endothelial cells. Its thinness and large surface area (about 75 m2) facilitate efficient diffusion of gases.
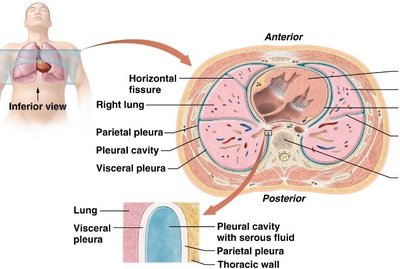
Pleural Membranes and Pleural Cavity
Structure and Function
Visceral pleura: Covers the lungs.
Parietal pleura: Lines the thoracic cavity.
Pleural cavity: Space between pleurae, filled with serous fluid to reduce friction and prevent lung collapse.
Pleural Diseases
Pleuritis: Inflammation of the pleura.
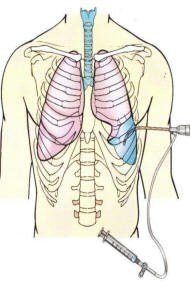
Pleural effusion: Accumulation of fluid in the pleural cavity, treated by thoracentesis.
Pulmonary Ventilation
Mechanics of Breathing
Pulmonary ventilation is driven by pressure changes in the thoracic cavity, governed by Boyle's Law:
Boyle's Law: At constant temperature and number of gas molecules, the pressure and volume of a gas are inversely related.
Atmospheric Pressure: Pressure of air outside the body (760 mmHg at sea level).
Intrapulmonary Pressure: Pressure within the alveoli; equalizes with atmospheric pressure.
Intrapleural Pressure: Pressure within the pleural cavity; always about 4 mmHg less than intrapulmonary pressure.
Pneumothorax
Pneumothorax occurs when air enters the pleural cavity, causing lung collapse. Treatment involves chest tube insertion to remove air and re-inflate the lung.
Muscles of Breathing
Inspiration: Diaphragm and external intercostals (normal); accessory muscles (forced inspiration).
Expiration: Passive at rest; abdominal and internal intercostal muscles (forced expiration).
Pulmonary Volumes and Capacities
Volume/Capacity | Definition |
|---|---|
Tidal Volume (TV) | Volume of air inhaled/exhaled during normal breathing |
Inspiratory Reserve Volume (IRV) | Additional air inhaled after normal inspiration |
Expiratory Reserve Volume (ERV) | Additional air exhaled after normal expiration |
Residual Volume (RV) | Air remaining in lungs after maximal exhalation |
Vital Capacity (VC) | Maximum air exhaled after maximal inhalation (TV + IRV + ERV) |
Total Lung Capacity (TLC) | Total volume of air in lungs after maximal inhalation (VC + RV) |
Factors Influencing Ventilation
Airway Resistance: Anything that impedes airflow, such as bronchoconstriction or inflammation.
Diseases: Asthma, COPD, and other conditions can increase resistance and reduce airflow.
Gas Exchange and Transport
Mechanisms of Gas Exchange
Occurs by diffusion across the respiratory membrane.
Efficiency depends on surface area, diffusion distance, and tissue perfusion.
Oxygen Transport
99% bound to hemoglobin (Hb) in red blood cells.
1% dissolved in plasma.
Carbon Dioxide Transport
7% dissolved in plasma
23% bound to hemoglobin
70% as bicarbonate ions in plasma
Blood pH is maintained between 7.35 and 7.45.
Diseases of the Respiratory System
Chronic Obstructive Pulmonary Disease (COPD)
Chronic Bronchitis: Inflammation and narrowing of airways, destruction of cilia, increased mucus production.
Emphysema: Destruction of alveolar walls, loss of elasticity, and impaired gas exchange.
Asthma
Characterized by bronchoconstriction, airway inflammation, and increased mucus production.
Treated with bronchodilators (β2 agonists) and anti-inflammatory steroids.
Infant Respiratory Distress Syndrome (IRDS)
Caused by insufficient surfactant production in premature infants.
Treated with surfactant administration and continuous positive airway pressure (CPAP).
Conclusion
The respiratory system is vital for life, enabling gas exchange, maintaining homeostasis, and supporting other physiological functions. Understanding its structure, function, and associated diseases is essential for students in anatomy and physiology.
