 Back
BackThe Respiratory System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Respiratory System
Overview of Respiration
The respiratory system is responsible for the exchange of gases between the atmosphere, blood, and body cells. This process is essential for cellular respiration and energy production. Respiration involves three main processes: ventilation (breathing), external respiration (gas exchange between air and blood), and internal respiration (gas exchange between blood and tissues). The system is divided into two zones: the conducting zone, which directs air to the lungs, and the respiratory zone, where gas exchange occurs.
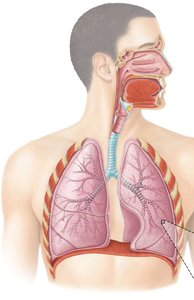
Conducting Zone
Nose and Nasal Cavity
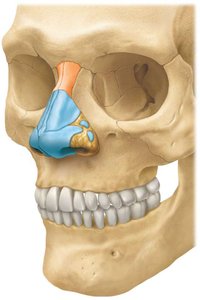
The nose is the external, visible part of the respiratory system, composed of cartilage and skin, and lined with a mucous membrane. The internal portion extends from the nasal vestibule to the pharynx and is lined with olfactory epithelium. The nose functions to warm, moisten, and filter incoming air.
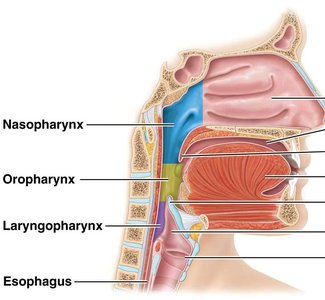
Pharynx
The pharynx is a muscular chamber that serves as a common pathway for both the respiratory and digestive tracts. It is divided into three regions:
Nasopharynx: Involved only in respiration.
Oropharynx and Laryngopharynx: Involved in both respiration and digestion.
During swallowing, the epiglottis closes the tracheal opening to prevent food from entering the airway.
Larynx
The larynx connects the laryngopharynx to the trachea and contains several cartilaginous structures, including the thyroid cartilage (Adam's apple), cricoid cartilage, and three pairs of smaller cartilages. The larynx houses the vocal cords and is essential for sound production and airway protection.
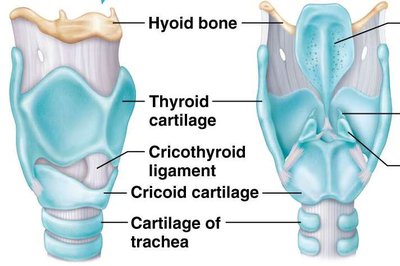
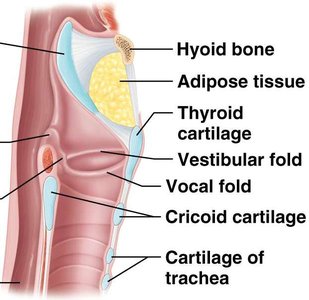
Vestibular folds (false vocal cords): Help hold breath against pressure in the thoracic cavity.
Vocal folds (true vocal cords): Vibrate to produce sound as air passes through.
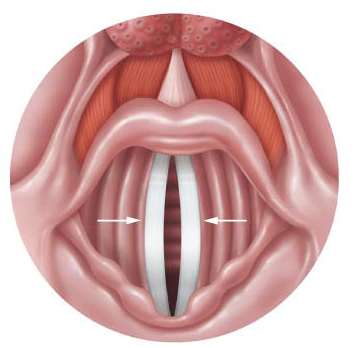
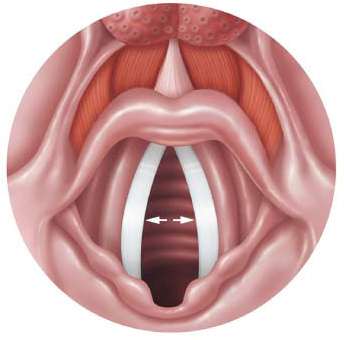
Trachea
The trachea, or windpipe, connects the larynx to the bronchi and is located anterior to the esophagus. Its wall contains 16-20 C-shaped rings of hyaline cartilage, which provide both rigidity and flexibility. The open part of the rings faces the esophagus, allowing for expansion during swallowing.
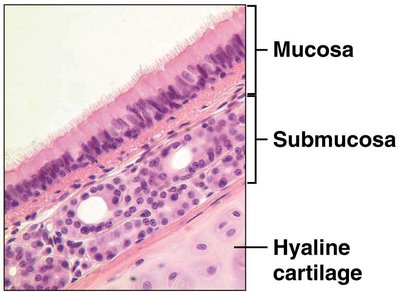
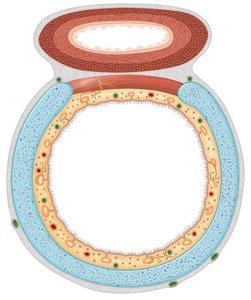
Bronchial Tree
The trachea divides into the right and left primary bronchi, each supplying a lung. The bronchi further branch into secondary (lobar) bronchi, tertiary (segmental) bronchi, and eventually into bronchioles and terminal bronchioles. As the airways branch, cartilage decreases and smooth muscle increases, and the epithelium transitions from ciliated pseudostratified to simple cuboidal.
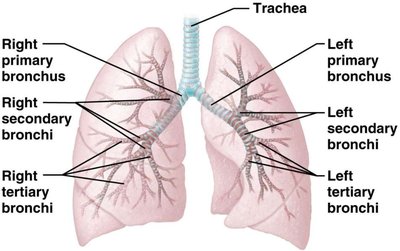
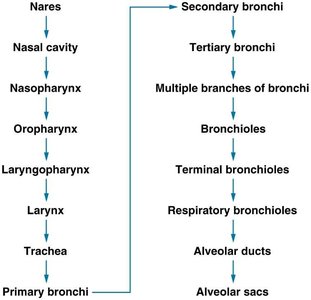
Respiratory Zone
Bronchopulmonary Segments and Alveoli
Each lung is divided into bronchopulmonary segments, each containing several lobules. Each lobule contains branches of the pulmonary and lymphatic vessels, respiratory bronchioles, alveolar ducts, alveolar sacs, and alveoli. The alveoli are the main sites of gas exchange.
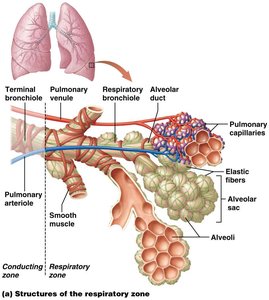
Type I alveolar cells: Numerous, responsible for gas exchange.
Type II alveolar cells: Fewer, secrete surfactant to reduce surface tension.
Alveolar macrophages: Provide immune defense.
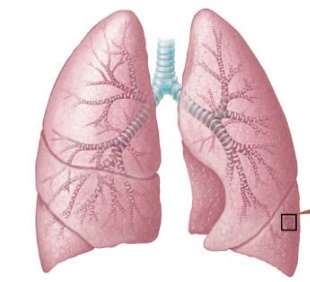
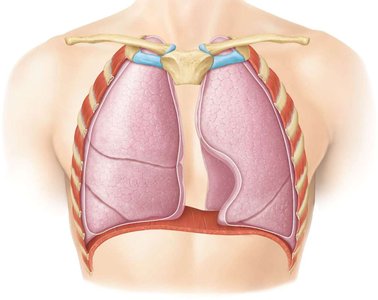
Lungs and Pleura
The lungs are paired organs located in the thoracic cavity and are enclosed by the pleural membrane. The visceral pleura covers the lungs, while the parietal pleura lines the thoracic cavity. The pleural space between these layers contains pleural fluid, which reduces friction during breathing.
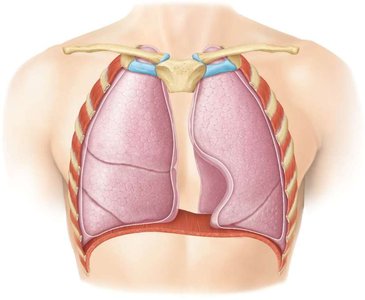
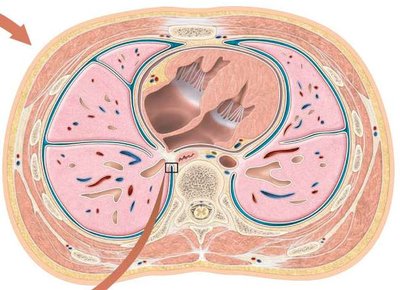
Right lung: Three lobes separated by two fissures.
Left lung: Two lobes separated by one fissure; contains a cardiac notch and is about 10% smaller than the right lung.
Pulmonary Ventilation (Breathing)
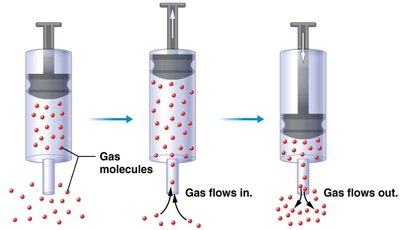
Boyle’s Law and Ventilation
Boyle’s Law states that at a constant temperature, the pressure of a gas is inversely proportional to its volume. During breathing, changes in thoracic cavity volume create pressure gradients that drive air movement:
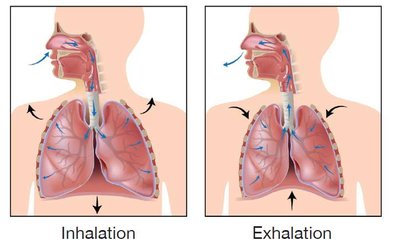
Inhalation: Thoracic volume increases, pressure decreases, air flows in.
Exhalation: Thoracic volume decreases, pressure increases, air flows out.
Air moves from areas of higher pressure to lower pressure.
Muscles of Ventilation
Normal inhalation: Diaphragm and external intercostals contract.
Forced inhalation: Sternocleidomastoids, scalenes, and pectoralis minor contract.
Normal exhalation: Relaxation of diaphragm and external intercostals.
Forced exhalation: Internal intercostals and abdominal muscles contract.
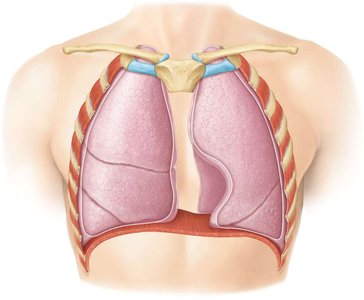
Pressure Changes During Breathing
Inhalation: Atmospheric pressure > alveolar pressure > intrapleural pressure.
Exhalation: Atmospheric pressure < alveolar pressure > intrapleural pressure.
Factors Affecting Ventilation
Intrapleural pressure: Maintains partial inflation of the lungs.
Alveolar surface tension: Surfactant prevents alveolar collapse during exhalation.
Lung compliance: The ability of the lungs to stretch and recoil.
Airway resistance: Increases as airway diameter decreases.
Lung Volumes and Capacities
Tidal volume (TV): Volume of air moved in a normal breath.
Minute volume: TV multiplied by breaths per minute.
Total lung capacity (TLC): Sum of inspiratory reserve volume (IRV), tidal volume (TV), expiratory reserve volume (ERV), and residual volume (RV).
Gas Exchange
Gas Laws
Dalton’s Law of Partial Pressures: Each gas in a mixture exerts its own pressure independently. Total atmospheric pressure is the sum of all partial pressures.
Henry’s Law: The amount of gas that dissolves in a liquid is proportional to its partial pressure and solubility.
External and Internal Respiration
External (pulmonary) respiration: O2 diffuses from alveoli to blood; CO2 diffuses from blood to alveoli.
Internal (tissue) respiration: O2 diffuses from blood to tissues; CO2 diffuses from tissues to blood.
Partial Pressures of O2 and CO2
PO2 in atmospheric air: 159 mm Hg
PCO2 in atmospheric air: 0.3 mm Hg
Gas Transport in the Blood
Oxygen Transport
1.5% of O2 is dissolved in plasma; 98.5% is bound to hemoglobin (Hb).
Each Hb molecule can bind up to 4 O2 molecules (oxyhemoglobin).
Only dissolved O2 can diffuse into tissues; O2 must bind and release from Hb rapidly.
The O2-Hb saturation curve is S-shaped due to cooperative binding. Factors such as low pH, high PCO2, and increased temperature (Bohr effect) decrease Hb's affinity for O2, promoting O2 unloading in tissues.
Carbon Dioxide Transport
7% dissolved in plasma
23% bound to Hb (carbaminohemoglobin)
70% as bicarbonate ions (HCO3-)
CO2 + H2O → H2CO3 → H+ + HCO3-
At tissues, HCO3- moves into plasma, and Cl- enters RBCs (chloride shift). In the lungs, the reaction reverses to release CO2 for exhalation.
Neural Control of Ventilation
Respiratory Centers
Clusters of neurons in the medulla oblongata and pons regulate breathing. The dorsal respiratory group (DRG) controls normal breathing, while the ventral respiratory group (VRG) is active during forceful breathing. Normal inhalation lasts about 2 seconds, and exhalation about 3 seconds.
Chemoreceptor Regulation
Central chemoreceptors in the medulla respond to increased CO2 and H+ (hypercapnia).
Peripheral chemoreceptors respond to decreased O2 (hypoxia).
Both conditions stimulate increased ventilation (hyperventilation).
