 Back
BackThe Stomach: Anatomy, Histology, and Functions 22.3
Study Guide - Smart Notes

The Stomach
Gross Anatomy of the Stomach
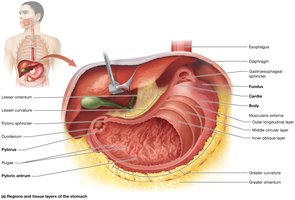
The stomach is a J-shaped organ located in the left upper quadrant of the abdomen, just inferior to the diaphragm. It serves as a major site for the mechanical and chemical breakdown of food.
Greater curvature: The convex left side of the stomach.
Lesser curvature: The concave right side.
Anatomical regions:
Cardia: Where the esophagus empties into the stomach.
Fundus: Dome-shaped top of the stomach.
Body: Largest portion.
Pyloric antrum: Inferior portion.
Pylorus: Terminal portion abutting the duodenum, containing the pyloric sphincter.
Rugae: Folds in the interior that allow expansion.

Histology of the Stomach
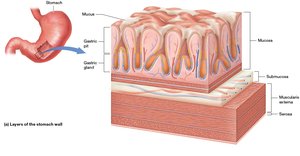
The stomach wall consists of four main tissue layers: mucosa, submucosa, muscularis externa, and serosa. The muscularis externa is unique in the stomach, containing an additional oblique layer that enables churning—motion that pummels the food into a liquid called chyme.
Mucosa: Heavily indented with gastric pits lined by columnar and goblet cells that secrete mucus.
Gastric glands: Located at the base of gastric pits, containing both endocrine and exocrine cells.
Endocrine cells secrete hormones into the bloodstream, and the exocrine cells secrete an acidic, enzyme-containing fluid called gastric juice into the lumen of the stomach.
Muscularis externa: Three layers: inner oblique, middle circular, and outer longitudinal.
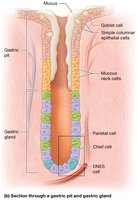
Cell Types in Gastric Glands
There are four main cell types in the gastric glands, each with distinct functions:
Mucous neck cells: Secrete acidic mucus, preventing neutralization of acid.
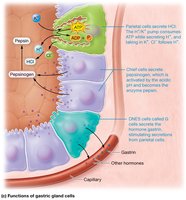
Parietal cells: Secrete hydrochloric acid (HCl), activating pepsinogen, destroying pathogens, and producing intrinsic factor for vitamin B12 absorption.
Chief cells: Secrete pepsinogen, which is activated to pepsin in acidic conditions to begin protein digestion.
Diffuse neuroendocrine system (DNES) cells: Secrete hormones such as gastrin and histamine, stimulating acid secretion; G cells are a subtype that secrete gastrin.
Functions of the Stomach
Primary Functions
The stomach performs three main functions: secretion, propulsion, and digestion. Acid secretion is a key process, regulated by neural and hormonal mechanisms.
Secretion: Release of gastric juice, including HCl, pepsinogen, and mucus.
Propulsion: Movement of food via peristalsis.
Digestion: Breakdown of proteins and other macromolecules.
Acid Secretion Mechanism
Hydrogen ions are secreted by the H+/K+ ATPase pump in parietal cells, while chloride ions follow passively. Acid secretion occurs continuously at a basal rate and is regulated in three phases:
Cephalic phase: Triggered by sight, smell, taste, or thought of food; mediated by the vagus nerve.
Gastric phase: Initiated when food enters the stomach; involves distension and presence of partially digested proteins.
Intestinal phase: Triggered by chyme entering the duodenum; brief stimulation followed by inhibition.
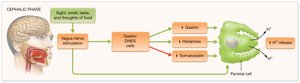
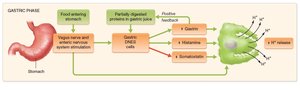
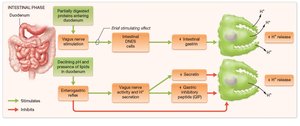
Regulation of Acid Secretion
Acid secretion is regulated by a combination of neural (vagus nerve) and hormonal (gastrin, histamine, somatostatin, secretin, GIP) signals. Positive feedback increases acid secretion until a low pH triggers negative feedback via somatostatin.
Positive feedback: Acid activates pepsin, which digests proteins, stimulating more gastrin release.
Negative feedback: Low pH triggers somatostatin, inhibiting acid secretion.
Motility and Gastric Emptying
Stomach motility enables the reception of food, churning into chyme, and controlled emptying into the duodenum. The process is regulated by neural and hormonal factors.
Receptive relaxation: Allows the stomach to fill without increasing internal pressure.
Churning: Peristaltic waves mix and propel chyme; controlled by gastric pacemaker cells.
Emptying: Liquids empty rapidly; solids must be liquefied. Rate is regulated by duodenal feedback (stretch, pH, lipid content).
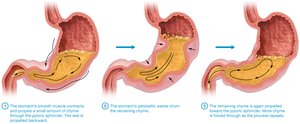
Gastroesophageal Reflux Disease (GERD)
GERD occurs when the gastroesophageal sphincter fails, allowing stomach acid to regurgitate into the esophagus. Chronic GERD can cause pain, swallowing difficulties, and increase cancer risk.
Contributing factors: Increased acid secretion, obesity, caffeine, hiatal hernia, certain medications, and Helicobacter pylori infection.
Treatments: Dietary modifications, antacids, H2 blockers, proton pump inhibitors, and antibiotics for H. pylori.
Vomiting (Emesis)
Vomiting is the expulsion of stomach contents through the mouth, often triggered by irritants, stress, or infection. It involves relaxation of stomach and intestinal smooth muscle, contraction of abdominal muscles, and coordinated neural responses.
Protective function: Expels harmful substances before absorption.
Anti-emetics: Drugs that block neurotransmitter receptors in the medulla to prevent vomiting.
Summary Table: Cell Types and Functions in Gastric Glands
Cell Type | Location | Secretion | Function |
|---|---|---|---|
Mucous neck cells | Neck of gland | Acidic mucus | Prevents neutralization of acid |
Parietal cells | Middle of gland | HCl, intrinsic factor | Acidifies stomach, activates pepsinogen, absorbs B12 |
Chief cells | Deeper in gland | Pepsinogen | Protein digestion |
DNES cells (G cells) | Bottom of gland | Gastrin, histamine | Stimulates acid secretion |
Key Equations
Hydrogen ion secretion by parietal cells:
Gastric acid feedback loop:
Negative feedback:
