 Back
BackThe Urinary System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Urinary System
Overview and Major Functions
The urinary system is essential for maintaining homeostasis by filtering blood, removing waste, and regulating fluid and electrolyte balance. It consists of the kidneys, ureters, urinary bladder, and urethra.
Filtration: Kidneys filter nearly 200 liters of blood daily, removing waste products such as ions, water, and toxins.
Blood Volume and Pressure Control: The kidneys regulate blood volume and pressure by secreting renin.
Water and Ion Balance: Regulation of sodium (Na+), potassium (K+), and bicarbonate (HCO3-).
pH Regulation: Excretion or reabsorption of hydrogen ions (H+) and bicarbonate.
Detoxification: Removal of free radicals and drugs.
Gluconeogenesis: Synthesis of glucose during starvation.
Red Blood Cell Production: Secretion of erythropoietin.
Vitamin D Synthesis: Conversion to active form.
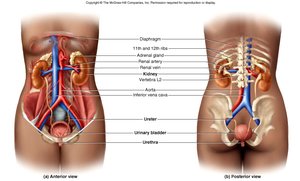
Anatomy of the Kidney
Gross Structure and Blood Flow
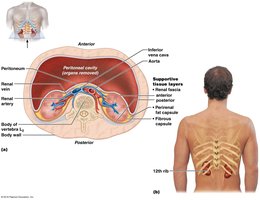
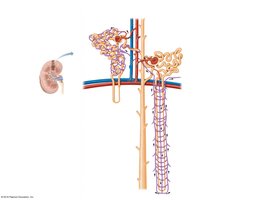
The kidneys are retroperitoneal organs located in the abdominal cavity, protected by connective tissue and adipose layers. Each kidney contains about 1.2 million nephrons, the functional units responsible for urine formation.
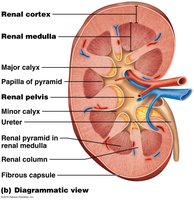
Renal Cortex: Outer region containing most nephrons.
Renal Medulla: Inner region with renal pyramids and loops of Henle.
Renal Pelvis: Funnel-shaped structure collecting urine into the ureter.
Blood Supply: Kidneys are highly vascularized, receiving about 20% of cardiac output.
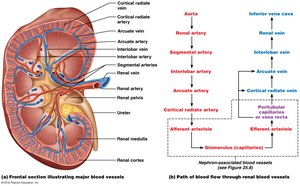
The Nephron
Types and Structure
Nephrons are the microscopic functional units of the kidney. There are two main types:
Cortical Nephrons: 85% of nephrons; located mostly in the cortex.
Juxtamedullary Nephrons: 15%; loops of Henle extend deep into the medulla, crucial for concentrating urine.
Processes of Urine Formation
Urine formation involves three main processes:
Filtration: Passive movement of fluid and solutes from blood into the nephron.
Reabsorption: Movement of substances from filtrate back into the blood (can be passive or active).
Secretion: Active transport of additional substances from blood into the nephron.
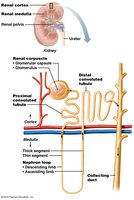
Nephron Components
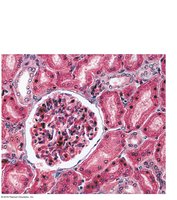
Renal Corpuscle: Includes the glomerulus (fenestrated capillary bed) and Bowman’s capsule (with podocytes forming filtration slits).
Renal Tubules: Proximal convoluted tubule (PCT), loop of Henle, distal convoluted tubule (DCT), and collecting duct.
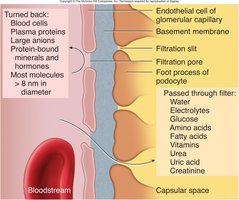
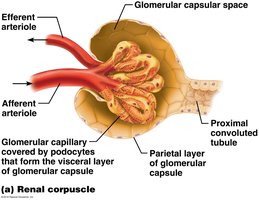
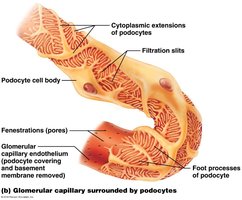
Filtration Membrane
The filtration membrane consists of three layers: fenestrated endothelium, basement membrane, and podocyte filtration slits. It allows passage of water, ions, glucose, amino acids, and small proteins, but restricts blood cells and large proteins.
Renal Tubule Functions
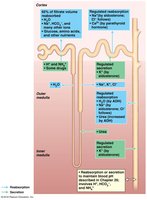
PCT: Major site of reabsorption (glucose, amino acids, vitamins, ions, water) and secretion (ions, toxins, drugs).
Loop of Henle: Reabsorption of water and ions; secretion of urea.
DCT: Reabsorption and secretion of ions; regulated by hormones (aldosterone, PTH).
Collecting Duct: Reabsorption of water (regulated by ADH), urea, and ions; secretion of ions.
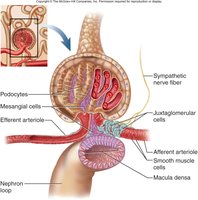
Juxtaglomerular Apparatus (JGA)
Structure and Function
The JGA is a specialized structure where the distal tubule contacts the afferent arteriole. It regulates blood pressure and filtration rate.
Granular (JG) Cells: Detect blood pressure changes and release renin when BP is low.
Macula Densa: Detects filtrate osmolarity and signals adjustments in arteriole diameter.
Mesangial Cells: Release paracrine signals to regulate glomerular filtration.
Glomerular Filtration and Net Filtration Pressure (NFP)
Filtration Forces and Calculation
Filtration in the glomerulus is driven by hydrostatic and osmotic pressures. The net filtration pressure (NFP) determines the amount of filtrate produced.
HPgc: Hydrostatic pressure in glomerular capillaries (forces fluid out).
HPcs: Hydrostatic pressure in capsular space (opposes filtration).
OPgc: Osmotic pressure of plasma proteins (draws fluid back in).
Equation:
Typical values:
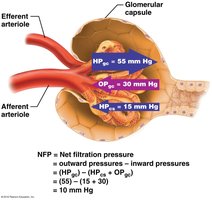
Note: Filtration stops if HPgc drops by ~15%. Blood pressure must remain high for filtration to continue.
Urine Volume and Reabsorption
Filtration Rate and Reabsorption Sites
The normal glomerular filtration rate (GFR) is about 125 ml/min (180–200 L/day), but 99% of filtrate is reabsorbed, resulting in about 1–2 L of urine excreted daily.
65% reabsorbed in PCT
15% in loop of Henle
19% in DCT and collecting duct (if ADH is present)
Regulation of Urine Production
Hormonal Control
Aldosterone: Increases Na+ and water reabsorption, K+ secretion; increases blood volume and pressure, decreases urine volume.
Renin-Angiotensin System: Low BP triggers renin release, leading to angiotensin II formation (vasoconstriction, aldosterone and ADH release, increased thirst).
ADH: Increases water reabsorption in DCT and collecting duct; increases blood volume and pressure, decreases urine volume.
Atrial Natriuretic Peptide (ANP): Inhibits ADH, aldosterone, and renin; increases urine volume, decreases blood volume and pressure.
Autoregulation and Neural Control
Autoregulation: JGA adjusts arteriole diameter to maintain stable GFR.
High BP: Afferent arteriole constricts, decreasing GFR and urine volume.
Low BP: Afferent arteriole dilates, increasing GFR and urine volume.
Sympathetic Stimulation: Constricts afferent arteriole, reducing GFR and urine volume.
Clinical Terms and Disorders
Key Terms
Diuretics: Substances that increase urine output by inhibiting water reabsorption (e.g., alcohol, caffeine, drugs).
Dialysis: Artificial filtration of blood for renal failure patients.
Micturition Reflex: Urination reflex triggered by bladder stretch receptors (~500 ml); involves voluntary and involuntary sphincters.
Diseases and Disorders
Kidney Disease: Often due to diabetes or hypertension; symptoms include high BP, edema, proteinuria; treated with BP control, diet, dialysis, or transplant.
Urinary Tract Infection (UTI): Bacterial infection, more common in females; symptoms include painful urination, fever; treated with antibiotics.
Acute Glomerulonephritis (AGN): Autoimmune inflammation of glomeruli; symptoms include proteinuria, hematuria, edema; treated with BP control, antibiotics, anti-inflammatories.
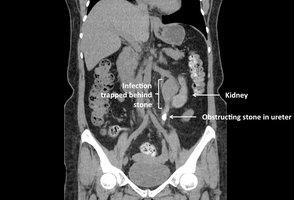
Renal Calculi (Kidney Stones): Calcium deposits causing obstruction; treated with lithotripsy.
Polycystic Kidney Disease (PKD): Genetic disorder with cyst formation, leading to kidney failure.
Abnormal Urinary Constituents
The presence of abnormal substances in urine can indicate disease:
Substance | Name of Condition | Possible Causes |
|---|---|---|
Glucose | Glycosuria | Diabetes mellitus |
Protein | Proteinuria, albuminuria | Excessive exertion, pregnancy, hypertension, heart failure, renal disease |
Ketone bodies | Ketonuria | Starvation, diabetes mellitus |
Hemoglobin | Hemoglobinuria | Transfusion reaction, hemolytic anemia, burns |
Bile pigments | Bilirubinuria | Liver disease, obstruction of bile ducts |
Erythrocytes | Hematuria | Bleeding urinary tract (trauma, stones, infection) |
Leukocytes (pus) | Pyuria | Urinary tract infection |
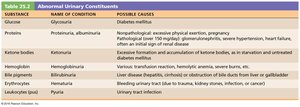
Additional info: The above table summarizes the diagnostic significance of abnormal findings in urine analysis, which is a key tool in clinical nephrology.
