 Back
BackThe Urinary System: Structure, Function, and Physiology
Study Guide - Smart Notes

The Urinary System
Overview of Urinary System Structures
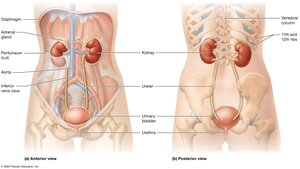
The urinary system is essential for the removal of metabolic wastes, regulation of blood composition, and maintenance of homeostasis. It consists of the kidneys, ureters, urinary bladder, and urethra, each with specialized roles in urine formation and excretion.
Kidneys: Filter blood, remove wastes, and regulate fluid and electrolyte balance.
Ureters: Muscular tubes that transport urine from the kidneys to the urinary bladder.
Urinary Bladder: Temporarily stores urine until elimination.
Urethra: Conducts urine from the bladder to the exterior of the body.
Functions of the Kidneys
The kidneys perform several vital functions that are critical for maintaining the body's internal environment.
Excretion: Removal of organic wastes from body fluids.
Elimination: Discharge of waste products via micturition (urination).
Homeostatic Regulation: Regulation of blood volume, blood pressure, plasma ion concentrations, blood pH, and conservation of nutrients.
Hormone Production: Release of erythropoietin (stimulates red blood cell production) and renin (regulates blood pressure).
Detoxification: Assists the liver in detoxifying poisons and eliminating wastes.
Nitrogenous wastes such as urea, uric acid, and creatinine are excreted in urine.
Internal Anatomy of the Kidneys
Major Regions and Structures
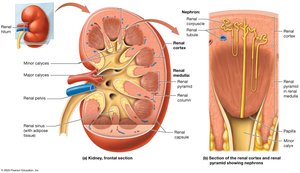
The kidney is divided into several distinct regions, each with specialized functions in filtration and urine production.
Renal Cortex: The outer region, containing the majority of nephrons (functional units of the kidney).
Renal Medulla: The inner region, organized into renal pyramids separated by renal columns.
Renal Papilla: The tip of each pyramid, projecting into a minor calyx.
Minor Calyx: Cup-shaped drain receiving urine from papillae.
Major Calyx: Formed by the convergence of minor calyces.
Renal Pelvis: Funnel-shaped chamber connecting to the ureter.
Blood Supply of the Kidneys
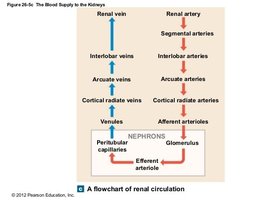
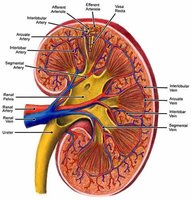
Kidneys receive a rich blood supply to facilitate filtration and reabsorption processes.
Blood enters via the renal arteries and is distributed through segmental, interlobar, arcuate, and cortical radiate arteries to the nephrons.
Venous return follows a similar path in reverse, ultimately draining into the renal vein.
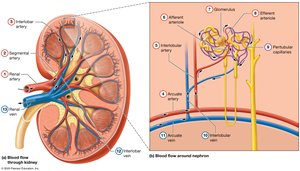
The Nephron and Collecting System
Structure of the Nephron
Each nephron is composed of a renal corpuscle and a renal tubule, which together filter blood and form urine.
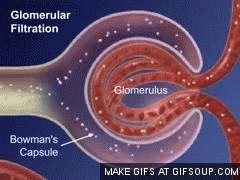
Renal Corpuscle: Includes the glomerulus (a tuft of capillaries) and the glomerular (Bowman's) capsule.
Renal Tubule: Consists of the proximal convoluted tubule (PCT), nephron loop (loop of Henle), and distal convoluted tubule (DCT).
Filtrate from the nephron drains into the collecting duct system, which carries urine to the renal pelvis.
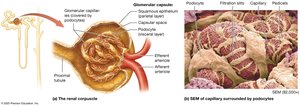
Filtration Membrane
The filtration membrane in the renal corpuscle consists of three layers:
Fenestrated endothelium: Capillary wall with pores for filtration.
Basal lamina (dense layer): Restricts passage of large proteins.
Filtration slits: Narrow gaps between podocyte foot processes (pedicels).
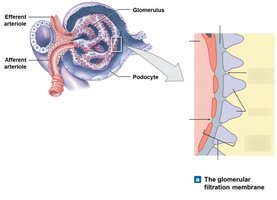
Segments of the Renal Tubule
The renal tubule is divided into distinct segments, each with specialized functions:
Proximal Convoluted Tubule (PCT): Major site of reabsorption of water, ions, and nutrients.
Nephron Loop (Loop of Henle): Descending limb reabsorbs water; ascending limb reabsorbs ions.
Distal Convoluted Tubule (DCT): Involved in selective reabsorption and secretion, regulated by hormones.
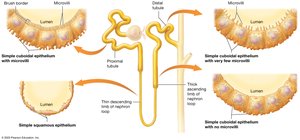
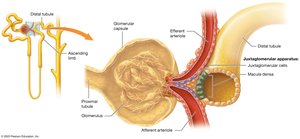
Juxtaglomerular Apparatus (JGA)
The JGA is an endocrine structure that regulates blood pressure and filtration rate.
Composed of macula densa (DCT cells) and juxtaglomerular cells (afferent arteriole smooth muscle).
Secretes erythropoietin and renin in response to changes in blood pressure or oxygen levels.
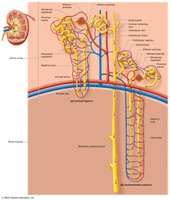
Types of Nephrons
There are two main types of nephrons, each with distinct anatomical and functional characteristics:
Cortical Nephrons: Located mostly in the cortex; short nephron loops; peritubular capillaries surround tubules.
Juxtamedullary Nephrons: Long nephron loops extend deep into the medulla; associated with vasa recta; crucial for concentrating urine.
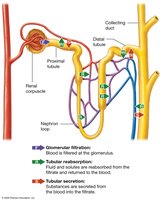
Renal Physiology: Filtration, Reabsorption, and Secretion
Three Basic Processes
Nephrons and the collecting system perform three essential physiological processes:
Glomerular Filtration: Blood pressure forces water and small solutes from the glomerulus into the capsular space, forming filtrate.
Tubular Reabsorption: Useful substances are reclaimed from the filtrate and returned to the blood.
Tubular Secretion: Additional wastes and excess ions are secreted into the tubular fluid for excretion.
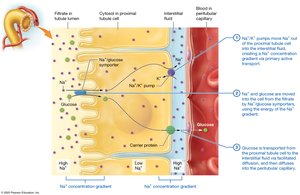
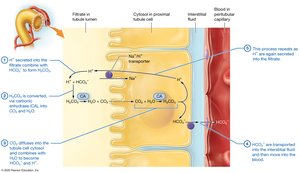
Reabsorption and Secretion in the Proximal Tubule
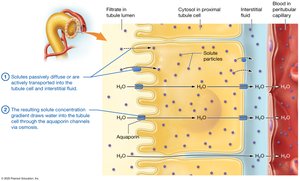
The PCT is the primary site for reabsorption of nutrients, ions, and water. It also participates in secretion of certain substances.
Reabsorbs 60-70% of filtrate volume, including nearly all glucose and amino acids.
Active and passive transport mechanisms are involved.
Some secretion of wastes and drugs occurs here.
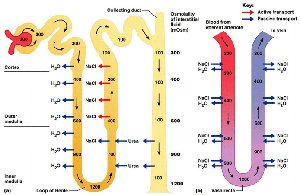
Nephron Loop (Loop of Henle)
The nephron loop establishes an osmotic gradient in the medulla, allowing for water conservation and concentration of urine.
Descending limb: Permeable to water, impermeable to solutes; water is reabsorbed by osmosis.
Ascending limb: Impermeable to water; actively transports Na+ and Cl- out of the filtrate.
Distal Convoluted Tubule (DCT) and Collecting System
The DCT and collecting ducts fine-tune urine composition through selective reabsorption and secretion, regulated by hormones such as aldosterone, parathyroid hormone (PTH), and antidiuretic hormone (ADH).
Selective reabsorption: Na+, Ca2+, and water (hormone-regulated).
Secretion: K+, H+, drugs, and toxins.
Water reabsorption: Obligatory (PCT and descending limb) and facultative (DCT and collecting duct, regulated by ADH).
Glomerular Filtration Rate (GFR) and Its Regulation
Filtration Pressures
Glomerular filtration is governed by the balance of hydrostatic and osmotic pressures across the filtration membrane.
Glomerular Hydrostatic Pressure (GHP): Blood pressure in glomerular capillaries, driving filtration (average 50 mmHg).
Capsular Hydrostatic Pressure (CHP): Opposes filtration by pushing fluid back into capillaries (average 15 mmHg).
Blood Colloid Osmotic Pressure (BCOP): Draws water back into capillaries due to plasma proteins (average 25 mmHg).
Net Filtration Pressure (NFP): The overall pressure driving filtration, calculated as:
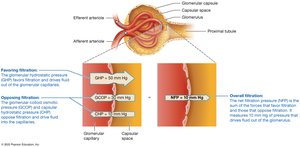
Regulation of GFR
GFR is tightly regulated by three mechanisms:
Autoregulation: Local adjustments of afferent and efferent arterioles to maintain stable GFR despite changes in blood pressure.
Hormonal Regulation: Involves the renin-angiotensin-aldosterone system (RAAS) and atrial natriuretic peptide (ANP).
Autonomic Regulation: Sympathetic nervous system can decrease GFR during stress or blood loss.
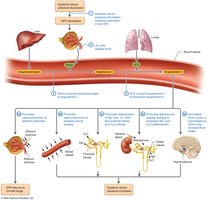
Urine Composition, Transport, and Elimination
Urine Composition and Urinalysis
Urine is a clear, sterile solution containing water, urea, creatinine, uric acid, and other dissolved ions and wastes. Its yellow color is due to the pigment urochrome, a by-product of hemoglobin breakdown.
Urine Transport, Storage, and Elimination
Urine formed in the kidneys is transported, stored, and eventually eliminated from the body through the following structures:
Ureters: Muscular tubes that propel urine to the bladder via peristalsis.
Urinary Bladder: Hollow organ that stores urine; contains rugae and a trigone region for efficient drainage.
Urethra: Conducts urine from the bladder to the exterior; shorter in females, longer and divided into regions in males.
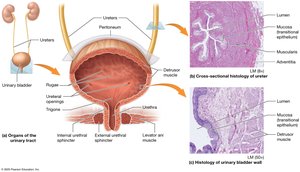
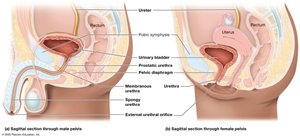
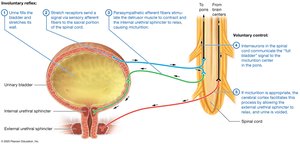
Micturition (Urination)
Micturition is the process of expelling urine from the bladder. It involves both involuntary (reflex) and voluntary control, primarily through the external urethral sphincter (skeletal muscle).
Relaxation of the external urethral sphincter allows urine to pass through the urethra and out of the body.
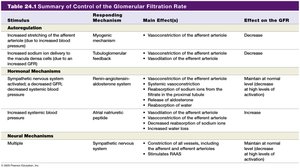
Summary Table: Control of Glomerular Filtration Rate
KStimulus | Responding Mechanism | Main Effect(s) | Effect on the GFR |
|---|---|---|---|
Increased stretching of afferent arteriole | Myogenic mechanism | Vasoconstriction of afferent arteriole | Decrease |
Decreased NaCl delivery to macula densa | Tubuloglomerular feedback | Vasodilation of afferent arteriole, vasoconstriction of efferent arteriole | Increase |
Decreased systemic blood pressure | Renin-angiotensin system | Constriction of efferent arteriole, increased Na+ and water reabsorption, release of aldosterone and ADH | Maintain or increase |
Increased systemic blood volume | Atrial natriuretic peptide | Dilation of afferent arteriole, constriction of efferent arteriole, increased water loss | Increase |
Multiple (stress, exercise) | Sympathetic nervous system | Constriction of all vessels, including afferent arteriole; stimulates RAAS | Decrease |
