 Back
BackUrinary System: Structure and Function
Study Guide - Smart Notes

Urinary System Overview
Functions of the Urinary System
The urinary system is essential for maintaining homeostasis by regulating water, solute concentrations, and removing metabolic wastes. It also plays a role in endocrine functions, blood pressure regulation, and acid-base balance.
Regulation of water and solute concentration: Maintains total water volume and solute concentration in the body.
ECF ion regulation: Controls extracellular fluid ion concentrations.
Acid-base balance: Ensures long-term acid-base balance.
Waste removal: Eliminates metabolic wastes, toxins, and drugs.
Endocrine functions: Includes renin (blood pressure regulation), erythropoietin (RBC production), and activation of vitamin D.
Gluconeogenesis: Occurs during prolonged fasting.
Organs of the Urinary System
Kidneys: Major excretory organs.
Ureters: Transport urine from kidneys to urinary bladder.
Urinary bladder: Temporary storage reservoir for urine.
Urethra: Transports urine out of the body.
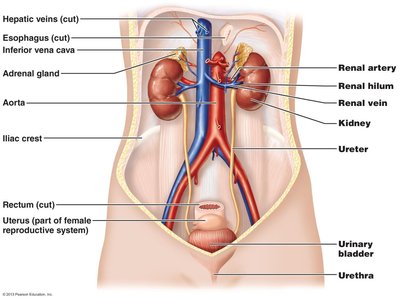
Kidney Anatomy
Location and Structure
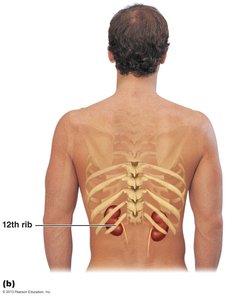
The kidneys are located between the dorsal body wall and the parietal peritoneum, in the superior lumbar region, extending from approximately T12 to L3. The right kidney is slightly lower due to the liver. Each kidney is topped by an adrenal gland and has a convex lateral surface and a concave medial surface with a renal hilum.
Renal hilum: Entry and exit point for ureters, blood vessels, lymphatics, and nerves.
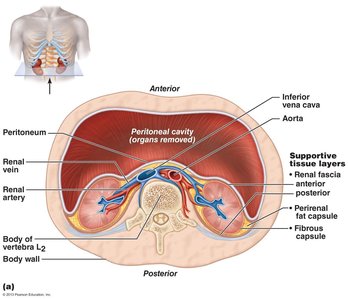
Supportive tissue layers:
Renal fascia: Dense connective tissue anchoring kidneys and adrenal glands.
Perirenal fat capsule: Cushions the kidney.
Fibrous capsule: Prevents spread of infection.
Internal Kidney Anatomy
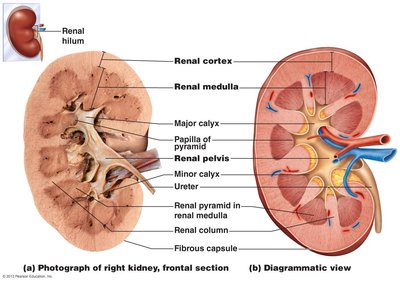
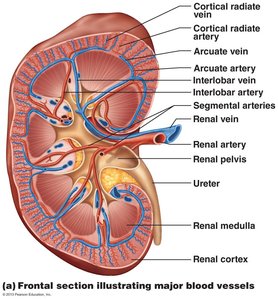
The kidney consists of three main regions: cortex, medulla, and pelvis. The cortex is the outer granular region, the medulla contains cone-shaped pyramids, and the pelvis is a funnel-shaped tube continuous with the ureter.
Renal cortex: Superficial, granular appearance.
Renal medulla: Contains medullary pyramids separated by renal columns.
Renal pelvis: Collects urine from major calyces and drains into the ureter.
Urine flow: Renal pyramid → minor calyx → major calyx → renal pelvis → ureter.
Blood and Nerve Supply of the Kidney
Renal Circulation
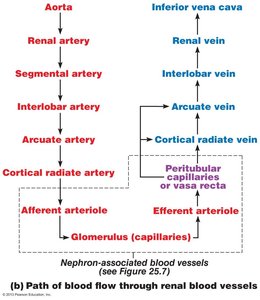
The kidneys receive about 25% of cardiac output each minute. Blood flow follows a specific path through arteries and veins, and the renal plexus provides sympathetic nerve supply.
Renal artery → segmental artery → interlobar artery → arcuate artery → cortical radiate artery → afferent arteriole → glomerulus → efferent arteriole → peritubular capillaries/vasa recta → cortical radiate vein → arcuate vein → interlobar vein → renal vein → inferior vena cava
Nephrons: The Functional Units
Structure of Nephrons
Nephrons are the blood-processing units of the kidney, responsible for urine formation. Each kidney contains over one million nephrons, which consist of a renal corpuscle and a renal tubule.
Renal corpuscle: Located in the cortex; includes the glomerulus and glomerular (Bowman's) capsule.
Renal tubule: Begins in the cortex, passes into the medulla, and returns to the cortex.
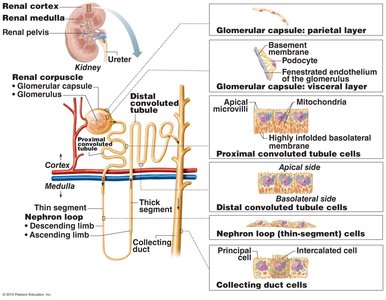
Renal Corpuscle
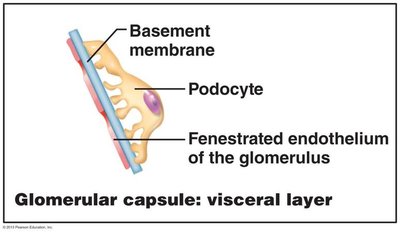
Glomerulus: Tuft of capillaries with fenestrated endothelium, allowing filtrate formation.
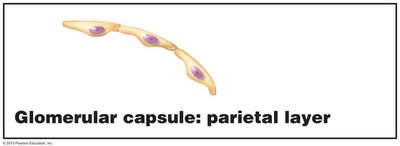
Glomerular capsule: Surrounds the glomerulus; has parietal (structural) and visceral (podocyte) layers.
Renal Tubule and Associated Cells
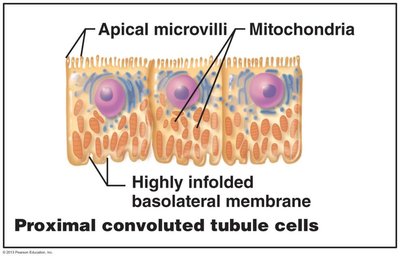
Proximal convoluted tubule (PCT): Cuboidal cells with dense microvilli for reabsorption and secretion.
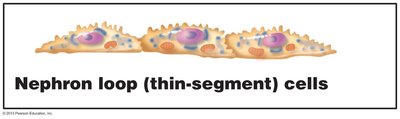
Nephron loop: U-shaped, with descending and ascending limbs; thin segment lined by simple squamous epithelium.
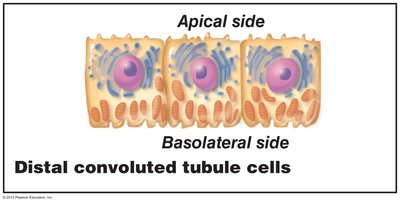
Distal convoluted tubule (DCT): Cuboidal cells with few microvilli; primarily involved in secretion.
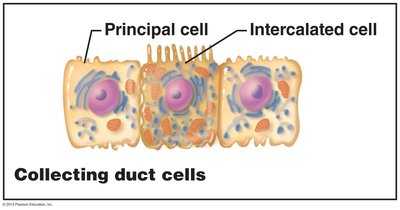
Collecting duct: Contains principal cells (water and Na+ balance) and intercalated cells (acid-base balance).
Classes of Nephrons
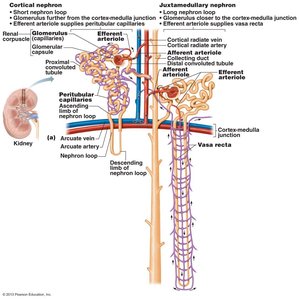
Cortical nephrons: 85% of nephrons; almost entirely in cortex.
Juxtamedullary nephrons: Long nephron loops that invade the medulla; important for concentrated urine production.
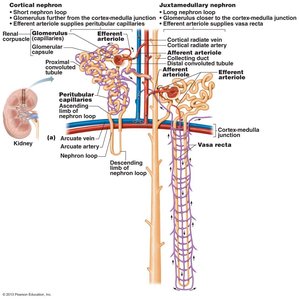
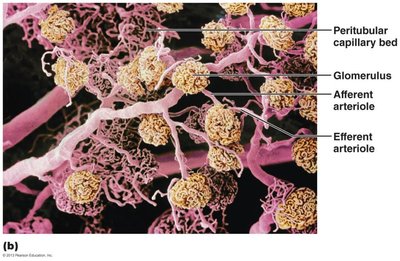
Nephron Capillary Beds
Types and Functions
Glomerulus: Specialized for filtration; fed and drained by arterioles.
Peritubular capillaries: Adapted for absorption; low-pressure, porous vessels.
Vasa recta: Long, straight vessels associated with juxtamedullary nephrons; important for concentrated urine formation.
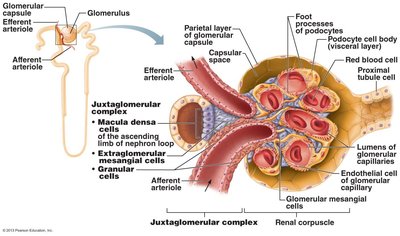
Juxtaglomerular Complex (JGC)
Structure and Function
The JGC is crucial for regulating filtrate formation and blood pressure. It consists of macula densa (chemoreceptors), granular cells (mechanoreceptors, secrete renin), and extraglomerular mesangial cells (signal transmission).
Kidney Physiology: Mechanisms of Urine Formation
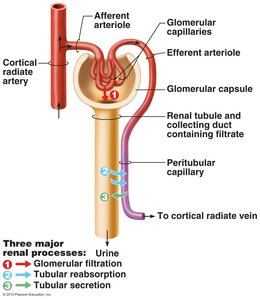
Three Major Renal Processes
Glomerular filtration: Produces cell- and protein-free filtrate.
Tubular reabsorption: Returns 99% of substances from filtrate to blood.
Tubular secretion: Moves substances from blood to filtrate.
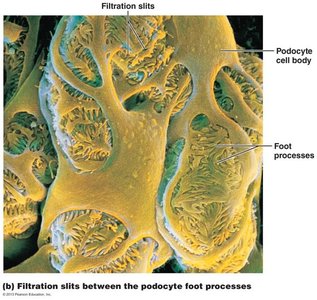
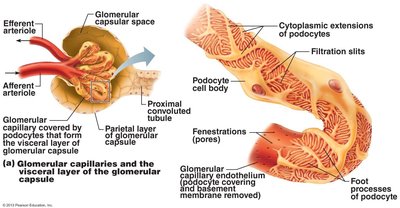
The Filtration Membrane
Three layers: Fenestrated endothelium, basement membrane, and foot processes of podocytes.
Allows passage: Water, glucose, amino acids, nitrogenous wastes; blocks cells and most proteins.
Colloid osmotic pressure: Maintains water in blood.
Glomerular Filtration: Forces and Regulation
Outward pressure: Hydrostatic pressure in glomerular capillaries (HPgc) pushes water and solutes out.
Inward pressures: Hydrostatic pressure in capsular space (HPcs) and colloid osmotic pressure in capillaries (OPgc) oppose filtration.
Net Filtration Pressure (NFP):
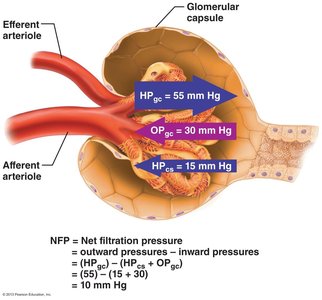
Glomerular Filtration Rate (GFR)
Definition: Total amount of filtrate formed per minute by both kidneys (120–125 ml/min).
Factors: NFP, surface area, and membrane permeability.
Regulation: Intrinsic (renal autoregulation) and extrinsic (nervous/endocrine) controls.
Urine Formation: Tubular Reabsorption and Secretion
Tubular Reabsorption
Selective process: Most tubular contents reabsorbed to blood.
Routes: Transcellular (through cells) and paracellular (between cells).
Reabsorption of Sodium and Solutes
Na+: Most abundant cation; reabsorbed by active transport.
Organic nutrients: Reabsorbed by secondary active transport with Na+.
Water: Reabsorbed by osmosis, aided by aquaporins.
Transport Maximum (Tm)
Definition: Maximum rate of transport for a substance; excess is excreted.
Example: Glucose Tm exceeded in diabetes, leading to glucose in urine.
Reabsorptive Capabilities of Tubules
PCT: Site of most reabsorption (nutrients, Na+, water, ions).
Nephron loop: Descending limb permeable to water; ascending limb permeable to solutes.
DCT and collecting duct: Reabsorption regulated by hormones (ADH, aldosterone, ANP, PTH).
Tubular Secretion
Reverse reabsorption: Substances move from blood to filtrate.
Functions: Disposal of drugs, elimination of undesirable substances, excess K+, and control of blood pH.
Regulation of Urine Concentration and Volume
Osmolality and Countercurrent Mechanisms
Osmolality: Number of solute particles per liter; kidneys maintain at ~300 mOsm.
Countercurrent multiplier: Nephron loop establishes gradient.
Countercurrent exchanger: Vasa recta maintains gradient.
Collecting Ducts and Urine Concentration
ADH: Controls water reabsorption in collecting ducts.
Formation of dilute urine: Low ADH, fewer aquaporins, urine ~100 mOsm.
Formation of concentrated urine: High ADH, more aquaporins, urine ~1200 mOsm.
Clinical Evaluation of Kidney Function
Renal Clearance
Definition: Volume of plasma cleared of a substance per minute.
Formula: Where C = clearance rate, U = urine concentration, V = urine flow rate, P = plasma concentration.
Inulin: Standard for GFR measurement.
Interpretation: C < 125 ml/min (reabsorbed), C = 0 (completely reabsorbed/not filtered), C > 125 ml/min (secreted).
Urine Transport, Storage, and Elimination
Ureters
Function: Convey urine from kidneys to bladder.
Structure: Three layers: mucosa (transitional epithelium), muscularis (smooth muscle), adventitia (fibrous connective tissue).
Urinary Bladder
Function: Temporary storage of urine.
Structure: Mucosa, detrusor muscle (three layers), fibrous adventitia.
Trigone: Triangular area outlined by ureter and urethra openings; common site for infections.
Urethra
Function: Drains urine from bladder.
Sphincters: Internal (involuntary) and external (voluntary).
Female urethra: Short (3–4 cm), anterior to vaginal opening.
Male urethra: Long (20 cm), carries urine and semen; divided into prostatic, membranous, and spongy regions.
Micturition (Urination)
Process: Requires contraction of detrusor (ANS), opening of internal sphincter (ANS), and opening of external sphincter (somatic nervous system).
Homeostatic Imbalances and Developmental Aspects
Common Disorders
Pyelitis/Pyelonephritis: Infections of renal pelvis/kidney.
Renal calculi: Kidney stones; treated with shock wave lithotripsy.
Chronic renal disease: GFR < 60 ml/min for 3 months; often caused by diabetes or hypertension.
Renal failure: GFR < 15 ml/min; treated with dialysis or transplant.
Incontinence: Loss of bladder control; stress or overflow types.
Urinary retention: Inability to expel urine; may require catheterization.
Developmental Aspects
Infants: Frequent micturition, incontinence normal.
Elderly: Kidneys shrink, nephrons decrease, GFR declines, bladder tone lost.
Physical and Chemical Characteristics of Urine
Color: Clear to deep yellow; abnormal colors indicate pathology.
Odor: Slightly aromatic; ammonia odor develops upon standing.
pH: Slightly acidic (~6); varies with diet and health.
Specific gravity: 1.001–1.035; reflects solute concentration.
Composition: 95% water, 5% solutes (urea, uric acid, creatinine, ions).
Additional info: These notes provide a comprehensive overview of the urinary system, suitable for exam preparation in an anatomy and physiology college course.
